Annual State of NHSScotland Assets and Facilities Report for 2014
Report on the State of the Estate 2014
3.0 The annual cost of assets and facilities services
The revenue and lifecycle costs associated with asset ownership and use represent a considerable proportion of NHSScotland budgets. This section of the report provides a summary of the annual cost (in 2012/13) of asset ownership and facilities management services. Whilst this section provides some comparative information on annual changes, more detailed information on performance trends is described in Section 5.
3.1 Property Assets and Facilities Services - Annual Costs
There are significant annual revenue costs that are directly associated with property asset ownership including:
- Property Maintenance - regular day to day maintenance including revenue expenditure on backlog but excluding major capital expenditure on upgrading/refurbishment and backlog works)
- Energy
- PFI Facilities Management Costs (primarily Hard FM)
- Rent and Rates
- Cleaning
There are also a range of facilities management services costs that are closely associated with property asset ownership including:
- Catering
- Portering
- Laundry and linen
- Waste disposal
The annual property and facilities services costs within the scope of the SAFR are shown in the table that follows for the three years for which the SAFR has been published (excludes Special Boards and the non-hospital estate).
| Annual Property Asset and Facilities Services Expenditure (£) | ||||
|---|---|---|---|---|
| 2010/11 | 2011/12 | 2012/13 | Percentage Change 2010/11 to 2012/13 |
|
| Property Maintenance (capital and revenue costs) | 113,949,249 | 117,679,791 | 123,457,925 | 8% |
| Cleaning | 117,128,872 | 117,425,095 | 119,750,871 | 2% |
| PFI Facilities Management Costs | 101,674,478 | 106,949,026 | 117,745,007 | 16% |
| Catering | 80,866,039 | 81,039,194 | 84,888,978 | 5% |
| Energy | 72,311,800 | 89,688,057 | 104,689,012 | 45% |
| Rent | 60,303,082 | 9,028,816 | 14,649,596 | 9% |
| Rates | 46,071,140 | 50,919,886 | ||
| Portering | 47,285,685 | 47,532,728 | 48,637,007 | 3% |
| Laundry and linen | 34,164,405 | 33,566,916 | 32,120,687 | -6% |
| Waste Disposal | 10,022,261 | 10,779,203 | 11,829,875 | 18% |
| Total | 637,705,871 | 659,759,966 | 708,688,844 | 11% |
| Annual Increase | 3.5% | 7.4% | ||
Note: The above table excludes depreciation on property asset; costs associated with Community and Family Health Services, and energy costs exclude costs associated with environmental taxes and levies e.g. EU ETS Payments. Further details relating to energy costs are provided in Annex C.
It should be noted that the overall increase in costs over the three year period is heavily skewed by the large increases in Energy Costs over the period and that these increases in Energy Costs are out with the control of Boards. Also, PFI Facilities Management Costs have increased due to further schemes becoming operational over that period, including Forth Valley Royal Hospital, Midlothian Community Hospital, Victoria Hospital expansion (Fife), etc.
Previous work on SAFR has identified that these property assets and facilities services costs are primarily (but not exclusively) driven by building size (volume/area) and patient activity (as measured by consumer weeks). The change in these primary cost drivers over the last three years is shown in the table that follows. The table also shows the change in the number of hospitals in this period.
| 2010/11 | 2012/13 | Percentage Change 2010/11 to 2012/13 |
|
|---|---|---|---|
| Number of hospitals | 250 | 228 | -9% |
| Building Area used for measuring cleaning costs (sq.m) | 3,054,536 | 2,974,584 | -3% |
| Consumer weeks | 1,049,499 | 1,016,582 | -9% |
| Annual Property Asset and Facilities Services Costs | 637,705,871 | 708,688,844 | 11% |
The table shows that the 11% increase over two years in expenditure on assets and facilities has been at a time when the property assets have been decreasing in terms of both the number of hospitals and the building size (area) and reduced inpatient activity (consumer weeks). However, it should be recognised that whilst inpatient activity (as measured by consumer weeks) has reduced there has been significant increases in the number of patients treated as outpatients or on a day case basis.
Interrogation of the ISD archive files has enabled a comparison of broadly similar assets and facilities costs and metrics over the last decade as shown in the two tables below.
| Expenditure on assets & facilities services | |||
|---|---|---|---|
| 2003/4 | 2012/13 | 03/04 to 12/13 Increase | |
| Property Maintenance (capital and revenue costs) | 91,398,478 | 123,457,925 | 35% |
| Cleaning | 72,559,057 | 119,750,871 | 65% |
| PFI Facilities Management Costs | 60,225,578 | 117,745,007 | 96% |
| Catering | 71,741,569 | 84,888,978 | 18% |
| Energy | 37,186,858 | 104,689,012 | 182% |
| Rent | 53,902,008 | 65,569,482 | 22% |
| Rates | |||
| Portering | 31,175,373 | 48,637,007 | 56% |
| Laundry and linen | 30,751,874 | 32,120,687 | 4% |
| Waste Disposal | 10,242,004 | 11,829,875 | 16% |
| Total: | 459,182,799 | 708,688,844 | 54% |
| Number of hospitals | 289 | 228 | -21% |
| Area (sq.m) used for cleaning | 2,967,490 | 2,974,584 | 0.2% |
| Consumer weeks | 1,281,093 | 1,016,582 | -21% |
It should also be recognised that over the ten year period significant changes in service delivery models have taken place including:
- Property Maintenance - greater use of technology based environmental control systems in modern healthcare buildings which inherently require more sophisticated maintenance regimes.
- Cleaning - the need for more rigorous cleaning to combat HAI
- PFI Facilities Management- New hospitals have become operational during the period, PFI/PPP contracts are generally inflation linked, and some facilities have no inpatient accommodation and thus have no inpatient consumer week data, e.g. two ACAD facilities in Glasgow.
- Catering - Improved patient choice and food quality
- Rent & Rates - generally indexed linked to inflation
- Portering - development of mulit-tasking whereby porters take on roles previously undertaken by security and other staff
- Laundry and linen- efficiency measures, including move from conventional linen to fitted bedding, have counter balanced inflationary pressures resulting in a relatively small increase in the cost of this service
- Waste - major regulatory changes introduced on clinical waste combined with re-cycling initiatives.
The profile of expenditure on assets and facilities services over this ten year period is shown in the table that follows and it is interesting to note that there has been very little change in this profile over the period. The one exception being energy which, as a percentage of total expenditure has increased by 7% points although even this is relatively low given the large increases in energy costs over the decade.
| Percentage of total expenditure on assets & facilities services | |||
|---|---|---|---|
| 2003/4 | 2012/13 | Difference | |
| Property Maintenance (capital and revenue costs) | 20% | 17% | -2% |
| Cleaning | 16% | 17% | 1% |
| PFI Facilities Management Costs | 13% | 17% | 3% |
| Catering | 16% | 12% | -4% |
| Energy | 8% | 15% | 7% |
| Rent & Rates | 12% | 9% | -2% |
| Portering | 7% | 7% | 0% |
| Laundry and linen | 7% | 5% | -2% |
| Waste Disposal | 2% | 2% | -1% |
3.2 Vehicles - Annual Costs
NHSScotland's estimated annual expenditure on its vehicles assets, as indicated through NHS Board information returns, is shown in the table below.
| Annual Expenditure on Vehicle Assets | ||||
|---|---|---|---|---|
| Description | £ | % of Total | No. of Vehicles | Average per Vehicle |
| Insurance & accident costs (net cost) | £6.21m | 13.06% | 10,909 | £569 |
| Fuel costs | £13.26m | 27.89% | 10,909 | £1,216 |
| Maintenance & servicing costs - owned vehicles | £0.76m | 1.59% | 1,917 | £394 |
| Leased vehicle costs (including maintenance) | £4.44m | 9.34% | 2,101 | £2,115 |
| Hired vehicle costs | £0.43m | 0.91% | 181 | £2,396 |
| Staff car scheme lease costs (including maintenance & mileage claims) | £22.45m | 47.21% | 6,710 | £3,346 |
| Staff contribution towards private use | -£11.12m | - | 6,710 | (£1,657) |
| Total Net Costs | £36.44m | 100% | 10,909 | £3,341 |
Note: excludes capital charges and depreciation on owned fleet.
In addition to the above, many NHSScotland staff use their private vehicles for official business and claim fuel and running costs of circa £23m through expenses claims.
The Transport & Fleet Management Review is looking at ways in which improvements can be made to the efficiency and effectiveness of this fleet aimed at reducing these operational costs (see Annex E for further details).
3.3 Medical Equipment - Annual Costs
Medical equipment use requires operational (revenue) costs for associated consumables and accessories, for routine scheduled maintenance and for breakdown maintenance. The survey explored these operational costs that, together with the acquisition and installation costs, form the total cost of ownership (COO) of the equipment. Consumable and accessory costs are typically charged to individual departments and no central records will cover all these costs. In most cases maintenance costs (scheduled and unscheduled) are easier to identify. Maintenance is provided through a combination of in-house staff and external service suppliers, the later often through service contracts. Efforts are being made through robust negotiations to fix maintenance costs, in some cases for up to 10 years, to reduce the total cost of ownership of medical devices. The annual maintenance expenditures reported by Boards is shown in the table that follows.
| Description | Expenditure (£) (incl VAT) | % of Total |
|---|---|---|
| Maintenance expenditure (excluding cost of in-house teams) on: | ||
| Renal Dialysis Equipment | 529,932 | 1% |
| Cardiac Defibrillators | 195,712 | 0.4% |
| Flexible Endoscopes | 3,607,562 | 7% |
| Infusion Devices | 327,359 | 1% |
| Radiotherapy Equipment | 1,536,532 | 3% |
| Imaging Equipment | 12,382,153 | 22% |
| All other Medical Equipment | 18,159,652 | 33% |
| Lease costs (including associated maintenance etc) | 757,835 | 1% |
| Annual payments (including maintenance etc) for managed equipment services and private finance arrangements (excluding Laboratory managed services) | 2,991,420 | 5% |
| Cost of in-house teams responsible for management of medical equipment | 9,517,198 | 17% |
| All other revenue based expenditure on medical equipment | 5,446,755 | 10% |
| TOTAL ANNUAL EXPENDITURE ON MEDICAL EQUIPMENT: | £55,452,110 | 100% |
As with property assets, there is a need to balance investment between ongoing annual maintenance of medical equipment, investment in its lifecycle replacement and investment in new innovative developments that advance the cost effectiveness of health care, including the ability to provide health care in the community. These advances, some facilitated by integration with information and communication technology (ICT), offer patient benefits including improved patient care, improved quality of life for patients, care in the community, and for imaging equipment clearer sharper images with reduced radiation doses. Staff benefit from the improved equipment functionality, improved reliability, and ease of use as manufacturers respond to standards on ergonomics. As equipment life is relatively short (often less than 15 years) the level of maintenance needs to be sufficient to ensure its continued safety, availability and effectiveness within that period whilst accepting that other considerations, such as technical and clinical obsolescence, can influence the need to replace equipment earlier than planned.
3.4 IM&T - Annual Costs
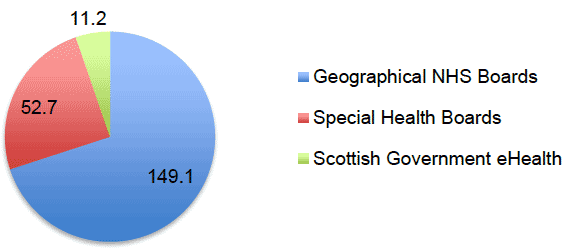
The IM&T survey identified that the overall level of expenditure by NHSScotland on IM&T in 2011/12 (the base date for the expenditure analysis), was £236.5m. Of this total, £213m was incurred on expenditure items of a revenue nature, with £23.5m incurred on capital expenditure. An analysis of the revenue expenditure is shown in the chart below.
Total Revenue Expenditure, £213m
The capital expenditure on IM&T of £23.5 million in 2011/12 is similar to that planned by Boards over the next 5 years (£26 million per annum)
The total revenue expenditure of £213m is split as follows:
- £57.5m (27%) of non-recurring expenditure by NHS Boards to support national systems and deliver eHealth strategic priorities.
- £91.5m (43%) of revenue expenditure by NHS Boards.
- £53m (25%) of revenue expenditure by Special Health Boards.
- £11m (5%) expenditure by the Scottish Government eHealth Division.
The table that follows provides a summary of the overall total revenue expenditure incurred by NHSScotland expressed as a percentage of Revenue Resource Limit (RRL) for 2011/12. By taking RRL as a proxy for NHSScotland's overall annual revenue expenditure it is possible to obtain an indicative measure of the level of overall revenue resource committed to IM&T by NHSScotland.
| Revenue Expenditure by NHS Board | RRL Percentage (%) | Revenue Expenditure by NHS Board | RRL Percentage (%) |
|---|---|---|---|
| Geographical NHS Boards | Special Health Boards | ||
| Ayrshire & Arran | 1.82 | NHS24 | 13.31 |
| Borders | 2.46 | Golden Jubilee ( NWTC) | 2.34 |
| Dumfries & Galloway | 1.92 | NHS Health Scotland | 3.00 |
| Fife | 1.57 | Healthcare Improvement Scotland | 1.73 |
| Forth Valley | 1.31 | National Education Services | 0.61 |
| Grampian | 1.48 | National Services Scotland | 7.07 |
| Greater Glasgow & Clyde | 1.81 | State Hospitals | 2.11 |
| Highland | 1.75 | Scottish Ambulance Service | 6.05 |
| Lanarkshire | 1.63 | Average: | 4.37 |
| Lothian | 1.34 | ||
| Orkney | 2.27 | ||
| Shetland | 2.41 | ||
| Tayside | 1.82 | ||
| Western Isles | 2.27 | ||
| Average: | 1.67 | ||
| Total: 2.11 | |||
Based on information from the IM&T Survey on NHSScotland expenditure for 2011/12
The table identifies that in 2011/12 the overall level of revenue expenditure on IM&T incurred by NHSScotland was 2.11% of its overall RRL. The table also shows that NHS Boards spent between 1.31% and 2.46% of their RRL on revenue IM&T expenditure, while Special NHS Boards typically spent higher percentages reflecting the different nature of the services they provide. This is particularly evident in the case of NHS24, which spent 13.31% of its RRL on revenue IM&T expenditure.
3.5 Summary of Total Annual Asset and Facilities Costs
The chart below provides an analysis of the combined total asset and facilities annual expenditure that has been described earlier. The combined expenditure of £1.013 billion is an increase of circa 6% on the expenditure reported in the 2013 SAFR.
NHSScotland's Annual Expenditure on Assets and Facilities Services (Total Expenditure 1.013 Billion)
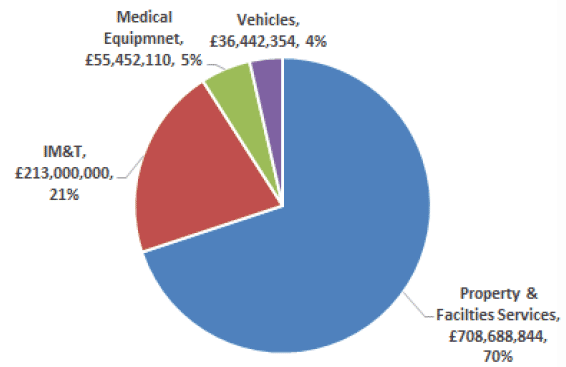
Notes: 1) Excludes capital charges and depreciation costs associated with asset ownership
2) Excludes any annual expenditure on lifecycle replacement and capital expenditure on backlog maintenance
3) Property & Facilities Service Expenditure is for the Hospital Estate only.
It should be noted that the above annual expenditure on assets excludes capital expenditure on:
- Replacement of existing assets - both major capital schemes (Board capital and NPD) and smaller schemes procured through hubco.
- Replacement of major existing assets - medical equipment, vehicles and IM&T - procured through revenue or Board capital.
- Major lifecycle maintenance/backlog such as boiler and major infrastructure and backlog replacement - procured through Board capital.
Contact
Email: Gillian McCallum