Annual Report of the Chief Medical Officer 2013 - Medical Leadership in Scotland
The Annual Report of the Chief Medical Officer 2013 - Medical Leadership in Scotland.
Chapter 2: Health Protection and Health Improvement
NHS Resilience
NHS Boards continue to improve their resilience planning to cope with major disruptions to their services from such incidents as environmental hazards and public health outbreaks e.g. severe weather and pandemic flu. With the publication of the Preparing for Emergencies guidance in 2013 a NHS Scotland exercise - 'Exercise Safe Hands' was held to support Boards in preparing for and being ready in the event of a major incident. This was the first time a national exercise with all Boards had been organised and provided key lessons to improve existing arrangements and response across Scotland. The Scottish Government Health and Social Care Directorates NHS Scotland Resilience Unit has also worked in partnership with Boards in continuing to provide a safe and effective health service.
2013 also saw changes to Scotland's multi agency resilience structures. Three Regional Resilience Partnerships (RRPs) replaced the eight Strategic Coordinating Groups. A number of Local Resilience Partnerships have been set up to support each RRP and health boards play a key role within these new structures.
Creating a New Food Body
In June 2012, the Scottish Ministers agreed to create a new food safety and standards body in Scotland, which would take over the functions currently carried out by the UK-wide Food Standards Agency (FSA) in Scotland. The FSA in Scotland is responsible for food safety and hygiene, labelling and nutrition. Legislation is required to create the new food body and the Scottish Government are working towards introducing a Bill to the Scottish Parliament in spring 2014.
To take this commitment forward, in February 2013 the Scottish Government launched A Healthier Scotland: Consultation on Creating a New Food Body, and held several stakeholder events to seek views on the roles, responsibilities and functions of the new food body. The responses to the consultation were independently analysed and showed that the majority of respondents supported a new food body and there was broad support for widening its scope beyond the functions currently carried out by the Food Standards Agency. At the same time, the Food Standards Agency ran the Consultation on New Proposed Enabling Primary Food and Feed Legislation Provisions which focused on seeking views on giving the body new enforcement sanctions, power to detain food which contravenes food law in relation to food standards or labelling and establishing a statutory basis for a food hygiene information scheme.
Additionally, in June 2013, an independent Expert Advisory Group led by Professor Jim Scudamore and commissioned by the Minister for Public Health, published a report on the lessons learned from the horsemeat food fraud incident. The Scottish Government and the Food Standards Agency published a joint response to the report and many of the report's recommendations will be taken forward by the new food body and the following will be contained in the Bill:
- Statutory power to seize and detain food which does not comply with food information law (eg mislabelled food);
- Statutory offence of failure to report breaches of food information law;
- Statutory scheme to be introduced, by regulation, for the mandatory display by food businesses of inspection outcomes;
- New administrative sanctions so that offences will be dealt with more quickly and at less cost than prosecution.
More information can be found on the Scottish Government's Creating a New Food Body website: http://www.scotland.gov.uk/Topics/Health/Healthy-Living/Food-Health/NewFoodBody.
Drinking Water Quality
The Drinking Water Quality Regulator for Scotland (DWQR) closely regulates the activities of Scottish Water (SW) on the quality of drinking water that they provide to 97% of the population of Scotland who are connected to the public water supply. In 2013, 154,755 tests were carried out on samples collected from consumers' taps and 99.89% of these complied with the standards, demonstrating the continued improvement in drinking water quality since SW was formed in 2002.
At the end of 2013, the standard for lead in drinking water was reduced from 25 to 10 micrograms per litre. SW currently manages compliance with this standard by either dosing a chemical which prevents the uptake of lead from any lead pipework which is still in the distribution system or by replacing that part of the lead pipe which is in SW ownership with a different material and informing the building owner that they have done this, offering advice about what they can do to protect themselves from high levels of lead. Such advice includes for example how they could replace their section of any lead pipe which is in their ownership and/or to run the tap for a short while to prevent any lead that may have built up in the pipe while the water has been standing in it. The DWQR is of the view that it is timely to review Scotland's policy for lead in drinking water and explore opportunities for reducing exposure to lead by working with stakeholders to identify areas where policy can be aligned. A working group was set up in the autumn of 2013, is run by the DWQR and has representatives from SW, Scottish Government health and housing and Health Protection Scotland on it.
Private water supplies (PWS) are drinking water supplies which are not the responsibility of SW but of their owners and users. The standards relating to PWS are enforced by local authorities and the DWQR supervises this enforcement. There are around 20,000 PWS in Scotland, 2,500 of which are what are called Type A supplies which supply 50 or more people or 10 cubic metres of water or more, and any PWS which is used in a commercial or public activity. The remaining 17,500 PWS are termed Type B which are the smaller, domestic supplies. In 2013, 40,620 tests were carried out on samples taken from Type A PWS, with 94.5% of these complying with the standards. The smaller Type B PWS, which are sampled less frequently, had 14,521 tests undertaken, of which 88.8% met the required standards. The main concern is that E.coli, which can cause illness, were detected in 13.6% of Type A supplies in 2013 and that this number of failures appears to be fairly static.
The DWQR had been concerned about the degree of compliance that PWS have with the standards, particularly with E.coli. Compliance had not improved despite new regulations having been brought into force in 2006 and the introduction of a financial grant to help PWS owners and users to improve their water supply. So in 2012, the DWQR organised a workshop for local authorities and health professionals to look at the issues to see what could be done and discuss the need for a multiagency strategy to deliver improvement. The strategy and action plan were developed during 2013 and contains three main elements. One element relates to how the legal system can be improved, another relates to improving communications, for example with owners and users about the health risks of being on a PWS and what they can do to protect themselves and the third element relates to improving technical guidance available to councils to help them when considering PWS issues. The Strategy also includes the actions contained in the VTEC Action Plan that was published by the Scottish Government in November 2013, as the two documents are very closely linked in terms of PWS. Progress with the actions in the strategy will be monitored by a Steering group consisting of representatives from all stakeholders involved in the strategy's development.
Health and Justice
The delivery of healthcare in criminal justice settings offers an opportunity for people in the community who find services hardest to reach, to benefit from support even of the briefest nature. This contributes to reduced health inequalities, which remain a major problem in Scotland, and has the potential to reduce re-offending. However, it remains the case that key determinants of health are poverty, housing and access to welfare or employment opportunities, along with social aspects of rehabilitation. Without addressing them, risk factor and health improvement intervention will have limited impact and this applies equally to police custody and prisons.
It has been estimated that around 54% of the 200,000 detainees passing through police custody in Scotland per annum are assessed as having alcohol and drug problems and a significant number present with mental health issues, both during contact in relation to crime, and also in interaction with the police service in a variety of non-criminal incidents; 68% had medical, mental health or substance misuse issues (Thematic Inspection of Custody Arrangements in Scotland HMICS 2014). Approximately 20,000 of the detainees are subsequently transferred, via the court system, into prison and thereby to health boards' healthcare services.
A study of Scottish prisons in 2007 indicated that nearly three quarters (73%) of prisoners have an alcohol problem, with almost two in five (36%) of those likely to be alcohol dependent. Nearly half (45%) reported being under the influence of alcohol at the time of their offence. 77% of prisoners tested positive for illegal drugs on reception to prison (33% for opiates) and 39% of prisoners reported being under the influence of drugs at the time of their offence. 74% of prisoners smoke compared with 26% of men and 23% of women in the general population. Nearly one in five of those in prison (19%) are estimated to be Hepatitis C positive and although data on mental health are scarce, prescribing indicators suggest significant numbers on treatment for depression and psychosis - 14% of prisoners were reported as having a psychiatric history. Severe dental decay in male prisoners was three times that of the general population (29% compared to 10%) whilst for women prisoners it was 14 times greater (42% compared with 3%).[1]
A Scottish study on the mortality of those who had been imprisoned in Scotland found that men were over three times more likely to die (3.3) than the general population and women over seven (7.6) times more likely to die, with risks elevated even after accounting for deprivation (2.3 and 5.7 respectively). The risk was greatest straight after release from detention, as prisoners return to the poor circumstances, poverty of opportunity and hope that they left. [2]
Coordinated action is required to address the health needs of those in police custody and the criminal justice system.
Police Custody
The NHS and Police Scotland have a joint responsibility to address the health and wellbeing of communities. Through joint working, the short period of detention can provide an opportunity to undertake healthcare interventions, as well as link people to community services on release, which otherwise would not happen e.g. services supported by Alcohol and Drug Partnerships. This can help to change the approach from an episodic reactive service to one that includes proactive and health promoting elements, which complement existing public services aimed at reducing inequalities, and reducing re-offending.
Actions include:
- Service redesign to improve efficiency and effectiveness and incorporate health improvement services;
- improvement of mental health and addiction services to people in custody, linking with relevant services in the community;
- improvement of the responsiveness and appropriateness of services to vulnerable children, particularly those who have been or are at risk of being abused;
- development of sustainable and safe approaches with partner agencies to deal with people who are drunk and incapable in the community;
- agreement of joint approaches for dealing with alcohol and violence, including gender based violence e.g. highlighting the impact on the police and NHS to Licensing Boards .
Prisons
The National Prisoner Healthcare Network has several work streams with a service focus in areas such as through care, mental health and addictions. Additionally, prisons are adopting a 'whole prison' approach to health improvement, working collaboratively with health boards and other partner organisations on the following issues:
- Reduced use of tobacco, and harmful use of alcohol and illicit drugs;
- improved mental wellbeing;
- increased uptake of healthy eating and reduce obesity;
- encouragement of better oral health;
- increased safer sex and better relationships;
- reduced transmission of blood borne viruses;
- increased physical activity;
- improved parenting;
- management and prevention of long term conditions.
A great deal of health improvement work is already being undertaken within Scotland's prisons and the next steps involve working with health and justice community partners to improve through care opportunities for offenders in the wider community.
Vaccine Preventable Disease
Extension of the immunisation programmes
A number of significant extensions to the immunisation programme were implemented in 2013. These include:
- Extending the seasonal flu programme to all children aged 2-3 years, and commencing pilot programmes for primary school children;
- changing the scheduling of Meningococcal C vaccine, including introducing vaccination for adolescents;
- offering Rotavirus vaccination to all young infants;
- introducing Herpes Zoster (shingles) vaccine for all those aged 70 years as a routine programme, and for those aged 79 years as part of a phased catch-up.
These developments mean that over 2 million vaccines are now offered every year to protect the population of Scotland. The programme is delivered by colleagues in Scottish Government working closely with Health Protection Scotland, NHS Boards and primary care. Immense benefits are already being seen. For example, the introduction of rotavirus vaccine in July 2013 has resulted in dramatically fewer infants having the dehydrating and debilitating symptoms of rotavirus gastroenteritis.
Measles
In 2013, there were 51 cases of laboratory confirmed measles and 3 probable cases, a number well in excess of the maximum of 5 cases a year required for accreditation by the WHO as having eliminated measles. The majority of these cases were in small clusters among partially and un-immunised patients with no evidence of transmission to the wider community. Most cases were seen in the first half of the year coinciding with a large, widespread measles outbreak in England and Wales. A risk assessment by Health Protection Scotland in 2013 identified young people caught up in the controversy generated by the Wakefield Paper to be at increased risk of measles transmission. NHS boards now routinely offer vaccine to under-immunised individuals at the teenage DTP vaccine booster appointment and there was a targeted catch-up campaign for those aged 10-17 in the summer of 2013.
Influenza
October 2013 saw the first stage of an extension of the seasonal influenza vaccination programme which offered a live intranasal vaccine (Fluenz) to all children age 2-17. The magnitude of the change necessitated a staged introduction to avoid an inadvertent impact on the rest of the Scottish Immunisation Programme (SIP). The first year involved the routine offer of Fluenz to all children aged 2 or 3 and piloting of the offer of vaccine to primary school age children. The offer was well accepted by parents as evidenced by uptake of 50.6% and 67.2% respectively. There was no evidence of any adverse impact on the rest of the SIP with seasonal flu vaccine uptake in those over the age of 65 above the WHO target of 75% for the seventh consecutive season (77%) and increased to 60.6% in those in clinical risk groups under the age of 65. Whilst the last two seasons have resulted in less burden on general practice in terms of clinical illness presentation there has been an increase in the number of severe cases requiring ITU management (125 in 2012/13 compared to 17 in 2011/12).
Pertussis
In 2012 and 2013 Scotland, like the rest of the UK, experienced a large national outbreak of pertussis. Young infants are also the group most likely to suffer complications and even death. A temporary programme to protect these infants by offering vaccine to pregnant women began in October 2012. Whilst the overall incidence of pertussis remained high in 2013, there was a dramatic decrease in the number of cases in infants. The over 85% reduction in incidence of lab confirmed cases of pertussis among infants is an indication of the immunisation programmes effectiveness in reducing disease in those most susceptible to severe infection, complications and death. The challenge now is to retain the high uptake rates among pregnant women.
Tuberculosis
Tuberculosis (TB) is a major global health problem which the World Health Organisation has ranked as the second leading cause of death from an infectious disease worldwide, after the human immunodeficiency virus (HIV). The Scottish Government is committed to eliminating TB as a public health problem in Scotland by 2050 - in line with WHO targets.
In 2013 there were 393 reported cases of TB in Scotland, an incidence of 7.4 per 100,000. This represents a continued decrease in numbers and incidence of TB cases reported since 2010, in contrast to the UK as a whole where rates are stable. However, accepted indicators suggest that recent transmission may be ongoing and increasing in Scotland; the rate of tuberculosis among children under five years of age increased from 1.4 per 100,000 population in 2012 to 3.4 in 2013, and, the child to adult notification ratio also increased, from 0.14 in 2012 to 0.30 in 2013.
The number and proportion of cases known to be born in the UK increased by five percentage points in 2013 but those born outside of the UK still accounted for more than half of all TB cases notified in Scotland (51.3%). The rate of tuberculosis among those born out with the UK decreased to 51.8 cases per 100,000 population from 60.6 cases per 100,000 per population in 2012. The rate of tuberculosis among those born in the UK increased to 3.6 cases per 100,000 population in 2013 from 3.3 cases per 100,000 population in 2012. The rate of tuberculosis amongst non-UK born individuals was approximately 14 times higher than the rate in the UK born population (51.8 versus 3.6 cases per 100,000 population).
For the first time since enhanced surveillance began in 2000, treatment outcomes of TB cases first notified in 2012 were increased when compared with 2011 (85.3% compared with 78.8%) and exceeded the ECDC target of 85%. In addition the number of deaths and the case fatality rate decreased to the lowest levels since surveillance began in 2000 (32 deaths, 8.4% CFR). However, delayed diagnosis and drug resistance present a challenge to on going improvement in these indicators: in 2013 17.5% (50/286) of tuberculosis cases had been symptomatic for longer than six months at notification which was higher than in 2012 (36/298; 12.1%); and although drug resistance rates remained within the recommended range, there was an increase in the number and proportion of cases resistant to any first line drug (20 cases, 8.4%) and an increase in the number and proportion of multi-drug resistant cases (4 cases, 1.7%).
Historically, the most commonly reported risk factor in Scotland is alcohol misuse and this may contribute to many of the challenges with respect to incidence, diagnostic delay, treatment completion and case fatality in Scotland. In 2013, risk factors were identified for 86 cases (24.9%), of whom five cases had more than one known risk factor. The main risk factors identified include immunosuppression (25 cases; 7.2%), alcohol misuse (20 cases; 5.8%), working in healthcare (19 cases; 5.5%), being a refugee (16 cases; 4.6%).
This summary is based on the Enhanced Surveillance of Mycobacterial Infections (ESMI) in Scotland: 2014 tuberculosis annual report for Scotland, the full report is available at: http://www.hps.scot.nhs.uk/documents/ewr/pdf2014/1438.pdf
In November 2013, Scottish Government published its first annual report on TB since the launch of the TB Action Plan for Scotland in 2011. Key recommendations are:
- To eliminate, by 2050, TB as a public health problem (WHO target of incidence <1 per million population = less than 5 cases per year);
- to use a monitoring framework to measure progress towards this goal;
- to establish case finding for latent TB among new entrants and migrants from high incidence countries;
- to establish new approaches to case finding for active TB among vulnerable groups, e.g. those with high alcohol intake, by linking with existing services in the community;
- to improve data quality through the development of electronic surveillance of TB;
- to establish a national multidisciplinary TB network to take these actions forward.
Legionnaires' Disease
The annual incidence rate of Legionnaires' disease in Scotland was 19.6 cases per million in 2012 and 9.6 cases per million in 2013. Twelve cases of Legionnaires' disease were notified to NHS Greater Glasgow and Clyde (NHS GGC) between June and September 2013. A multi-agency Outbreak Control Team (OCT) chaired by NHS GGC was convened to manage the incident. The conclusion of the OCT was that there was a cluster of cases of LD which were linked in time and place and probably as a result of exposure to a single environmental source. However, the exact source could not be elucidated although cases were associated with exposure in the Renfrew area.
In the period August to September 2013, six confirmed and one probable case of Legionnaires' disease caused by Legionella longbeachae were reported in NHS Lothian and NHS Tayside. The six confirmed cases were severely unwell and all required treatment in intensive care units, including ventilation. All cases survived. The majority of cases were keen gardeners and had exposure to growing media, soils and water in the garden during their incubation period. Prior to this cluster, eleven sporadic cases of Legionnaires' disease caused by L. longbeachae infection had been reported to Health Protection Scotland, in the period 2008-2012. Due to cases being identified in two NHS boards, the investigation was co-ordinated by HPS and a report published at : http://www.documents.hps.scot.nhs.uk/respiratory/legionella/legionella-outbreak-report-2014.pdf
Blood Borne Viruses and Sexually Transmissible Infections
Hepatitis C Virus Infection
2013 saw a considerable number of people, infected with HCV genotype 1, treated with first generation protease inhibitors administered in combination with pegylated interferon and ribavirin. The total number of individuals started on HCV antiviral therapy - around 1,000 - was similar to those observed in 2011 and 2012. Randomised controlled trial data, demonstrating the high effectiveness, safety and ease of administration of newly developed, direct acting HCV antiviral therapies, were published in 2013. Accordingly, the HCV treatment landscape is about to change dramatically. It is anticipated that by 2015, several different interferon free antiviral therapies will be available. These are likely to be cost-effective but costly. The hepatitis C challenges ahead will be the identification of HCV infected individuals, particularly those with advancing disease, and the accessing of funds to pay for the therapies.
Recognising these imminent benefits and challenges, the Minister for Public Health established a Hepatitis C Treatment and Therapies Group to generate a set of principles around the diagnosis and treatment of hepatitis C in this new therapeutic era; these principles, to be aligned with Scotland's healthcare quality strategy, will be developed in 2014 and will inform future policy in this area.
Chlamydia
In 2013, just over 17,000 diagnoses of genital chlamydia infection were made - the lowest number since 2005 and a reduction of around 800 from that observed in the previous year. While there is no dispute that this infection causes pelvic inflammatory disease, ectopic pregnancy and infertility, increasing evidence indicates that the frequency of these events is lower than previously thought. Accordingly, the Scottish Government, in the context of a review on chlamydia screening policy, commissioned a study to assess the cost-effectiveness of such screening. This work, to be completed in 2014, will inform decision making around such policies.
Syphilis
Two outbreaks of infectious syphilis among young heterosexual men and women in Scotland were observed in 2012/13. These were confined to individuals in Lanarkshire and Tayside, with 9 and 15 being diagnosed in 2013, respectively. Most were aged under 25 and some were aged under 18. Both health boards responded by setting up youth clinics to provide testing opportunities and increase awareness of the problem. Leaflets, postcards, posters and Facebook adverts were used to increase awareness of syphilis among the general public. In Lanarkshire presentations were delivered to pupils in schools. These interventions, together with partner notification initiatives, appear to have controlled the problem.
These two syphilis outbreaks highlight the fact that casual unprotected sexual intercourse among young men and women remains a major public health challenge in Scotland.
Gastrointestinal and Zoonotic Infections
Campylobacter data linkage
Campylobacter is the most commonly reported bacterial cause of infectious intestinal disease in Scotland, with 6163 laboratory confirmed cases reported in 2013. Studies have estimated that for every case reported by national surveillance, 9.3 occur in the community, applying this ascertainment value, the true number of cases may be in the region of 55,800 per year. A data linkage project is currently underway to achieve a greater understanding of the burden of Campylobacter infection. This work has linked laboratory confirmed cases for the past five years to the SMR01 hospitalisation data. This will enable national estimates of the number of cases requiring hospitalisation, the duration of hospitalisation and the identification of factors that may increase the risk of hospitalisation. A small proportion of cases may develop sequelae post-Campylobacter infection, the most important of which is Guillain-Barré Syndrome (GBS), a demyelinating disorder resulting in acute neuromuscular paralysis. This project will also enable estimates of sequelae to be determined as well as some of the risk factors associated with developing sequelae.
Norovirus
While those infected with norovirus (NV) usually experience a mild, short lived clinical illness its public health importance relates to its highly infectious nature, causing outbreaks especially in semi-closed settings such as hospitals, care homes, schools and hotels, resulting in social and economic disruption. The number of laboratory reports of NV varies considerably year by year, with some years experiencing particularly high NV seasons. In 2013, laboratory reports declined by 34% compared to 2012, from 2920 to 1915. This decline was also evident in the number of general outbreaks of NV which fell by 25% from 329 in 2012 to 245 in 2013.
Hepatitis E
In recent years the public health importance of hepatitis E virus (HEV) has become established as a newly emerging zoonotic pathogen; the major animal reservoir is believed to be domestic pigs. In Scotland laboratory reports of HEV have increased dramatically over the past five years, from three in 2009 to 95 in 2013. In 2013, 65% of reports were from males, with 73% of cases in males aged 50 years and over. Health Protection Scotland has recently established a working group with a range of stakeholders to investigate this increase in more detail and to ascertain the extent to which this sudden rise is due to improved ascertainment and how much is a genuine increase in incidence. This information will help in identifying the most important vehicles of transmission and will inform the development of strategies for interventions to stop the upward trend, and ultimately reduce the burden of HEV infection. Much remains to be understood about the epidemiology, risk factors for infection and vehicles of transmission of this emerging disease.
Salmonella
In 2013, laboratory reports of Salmonella increased by 12%. However much of this increase was due to two notable outbreaks - one involving 25 confirmed cases of Salmonella Hofit associated with a school, the other involving 30 cases of Salmonella Mikawasima associated with a national outbreak also affecting people in England & Wales. A case control study found that eating chicken outside the home was associated with illness.
VTEC/E.coli O157
In 2013, a total of 167 culture positive cases were notified to HPS, a further three cases were identified by serodiagnosis of antibodies to E. coli O157 alone. The total of 167 culture positive cases represented a decrease of 67 (29%) compared to 234 cases notified in 2012. The total for 2013 was the lowest for the last five years, and was substantially below the annual average for that period (221 cases per annum). Of the 170 culture or serum positive cases in 2013, 23 (14%) were reported by local investigators to be part of outbreaks. One of these cases was part of a Great Britian-wide outbreak that was associated with watercress. Three were part of outbreaks that originated from locations in other parts of the UK. The majority of cases in 2013 were therefore apparently sporadic cases, as has historically been the case in Scotland. The 19 cases linked to outbreaks in Scotland were part of three separate incidents. Thirty-one (19%) of the 167 culture positive cases in 2013 were believed to have acquired their infection outwith the UK.
In November 2013, the Scottish Government published the VTEC/E. coli O157 Action Plan for Scotland, 2013-2017, which was compiled by the multi-disciplinary VTEC/E. coli O157 Action Group, co-ordinated on Scottish Government's behalf by HPS. The Action Plan uses a systematic framework to describe the pathways of transmission of VTEC from animal source to human case, and recommends where new control measures might be effective, and where new methods of monitoring compliance and evaluating effectiveness are required. The Action Group will continue to meet to provide feedback for Scottish Government on the progress of various agencies across Scotland in implementing these reforms.
A full copy of the VTEC/E. coli O157 Action Plan can be downloaded from: http://www.scotland.gov.ukaa36d850-e821-40cc-838a-7cf302895367.
Lyme borreliosis
In May 2013, Health Protection Scotland and the National Lyme Testing Laboratory convened an interdisciplinary symposium over two days in Inverness to establish and take forward a strategy for lyme borreliosis (Lyme Disease) in Scotland. Participants included patient representatives, primary and secondary care clinicians, human and animal health epidemiologists and ecologists, social scientists, policy makers, rural stakeholder groups and colleagues from England and Wales. A range of presentations and workshops yielded a commitment to work collaboratively around the production and implementation of a Lyme Disease strategy for Scotland, drawing together skills and experience from a diverse range of experts. Knowledge exchange will be the core of the strategy, with an emphasis on collaboration to provide the best available information to enable prevention, early recognition, and treatment of Lyme borreliosis. The strategy will be co-ordinated by Health Protection Scotland.
Rabies
Guidance on prophylaxis and management in humans in Scotland
This guidance, originally issued in 2010, was updated in July 2013 and offers clear, easy to follow advice on pre and post-exposure immunisation as well as administration and financial arrangements. Although primarily intended for use across NHSScotland, it has been well received and used by colleagues throughout the UK. The guidance is not intended to advise on clinical case management or animal handling, except where the latter affects the management of potential human exposure.
Updates in the 2013 guidance include:
- Changes to the supply of human rabies immunoglobulin (HRIG);
- new table on pre-exposure prophylaxis for travellers;
- changes to the Pets Travel Scheme;
- new link to the updated Green Book Chapter on rabies (https://www.gov.uk/government/publications/rabies-the-green-book-chapter-27).
The guidance is available at: http://www.hps.scot.nhs.uk/giz/guidelinedetail.aspx?id=46619
Healthcare Associated Infections and Antimicrobial Resistance
Healthcare associated infections (HAI) are increasingly caused by multidrug resistant organisms and represent a continuing threat to patient safety and healthcare delivery. HAI place a significant financial burden on NHSScotland with HAI originating in acute care estimated to cost the NHS in Scotland £137 million annually.
Health Protection Scotland and NHS Boards work closely with the Scottish Patient Safety Programme which aims to improve safety and reliability of healthcare. Key programme areas that can reduce HAI and antimicrobial resistance include leadership walk-rounds, Peripheral Venous Catheter (PVC) bundle, Ventilator Associated Pneumonia (VAP) and Catheter Related Blood Stream Infection (CR-BSI) prevention packages, the surgical checklist; hand hygiene and safety walk rounds.
Staphylococcus aureus bacteraemia
During 2013, a total of 1,584 cases of Staphylococcus aureus bacteraemia including meticillin resistant S. aureus (MRSA) were reported. This represented an annual incidence of S. aureus bacteraemia of 31.1 per 100 000 Acute Occupied Bed Days. Neither the number of bacteraemias nor the incidence was significantly different from 2012. The majority of bacteraemias in 2013 were due to methicillin sensitive S. aureus (MSSA) (1,430 bacteraemias, 90.3%).
In 2013, the Health Protection Scotland S. aureus bacteraemia surveillance team undertook a pilot linkage study using S. aureus bacteraemia case records which were linked to records of hospital admissions and deaths. This proved that the linkage was feasible, enabling further epidemiological analyses of risk markers and clinical outcomes. The methodology of the pilot study will be developed for further epidemiological work.
Additionally, NHS boards and HPS are jointly undertaking an enhanced surveillance programme of S.aureus bacteraemia patients. This will lead to a better understanding of clinical risks for S.aureus bacteraemias and allow NHS boards to share learning in the management of S. aureus bacteraemias.
A Key Performance Indicator (KPI) for compliance with Clinical Risk Assessment (CRA)-based MRSA screening was introduced in April 2013. The compliance reported during 2013/14 was 78%, below the Scottish Government Health and Social Care Directorate (SGHSCD) target of 90%. In the clinical setting, CRA-based screening performs favourably compared to universal screening as the percentage of colonised patients identified is equivalent (assuming 66% compliance with universal nasal screening as reported in English hospitals). This is important as the added benefits of pre-emptive isolation and significantly lower cost of CRA mean it remains a clinically and cost-effective policy.
Surgical site infection (SSI)
The incidence of SSI following hip arthroplasty and caesarean section surgery did not change significantly between 2012 and 2013. As part of ongoing work to assess and improve Post Discharge Surveillance for caesarean section procedures within NHSScotland a number of initiatives were introduced within the last year by HPS. This will help inform and improve practice within NHSScotland to ensure that PDS methods currently used adequately capture the patient population and that data presented in the public domain are accurate thus ensuring comparability between NHS boards.
Figure 1: Incidence of SSI following caesarean section procedures in Scotland (inpatient and PDS to day 10), 2009 to 2013
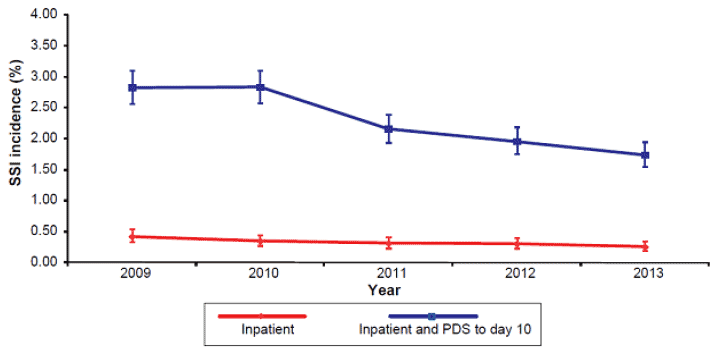
Figure 2: Incidence of SSI following hip arthroplasty procedures in Scotland (inpatient and readmission to day 30), 2009 to 2013
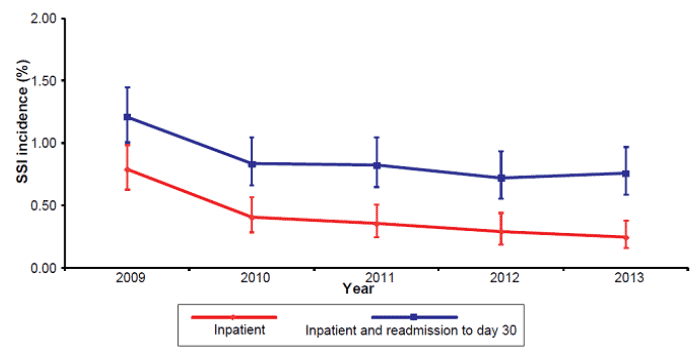
Intensive care unit HAI surveillance
During 2013, 3.0% of patients staying in ICU for more than 2 days developed a HAI. The incidence of blood stream infection, central venous catheter related infection and pneumonia remained similar to rates reported in 2012.
Escherichia coli
In Scotland, Escherichia coli (E. coli) is the most common pathogen implicated in bacteraemia in community and healthcare settings. During 2013, there were 4,321 cases of E. coli bacteraemia in Scotland compared to 3,924 in 2012. The incidence increased from 66.6 per 100,000 persons in 2009 to 81.3 per 100,000 persons in 2013. A pilot study has been undertaken in 2013 to allow us to begin to describe the epidemiology of E. coli infection and elucidate which interventions are likely to be most effective.
The recent increase in burden of disease caused by E. coli bacteraemia does not seem to have been driven by resistant strains as decreases in resistance to key antimicrobials have been observed in this period. This includes an overall decreasing trend in resistance to the cephalosporins antimicrobial class from 10-14% in 2008 to 6-8% in 2012, and in extended spectrum beta-lactamases (ESBL) producers among E. coli (from 7.2% in 2008 to 6.6% in 2012). Resistance to gentamicin remained at 9% in E. coli in 2010-2012 despite increasing use of this agent.
Clostridium difficile infection (CDI)
In patients aged ≥65 years there was a statistically significant decrease in the CDI annual incidence rate of 8.7% between 2012 and 2013 (34.5 vs. 37.8 per 100,000 total bed days). The annual incidence rate in patients aged 15-64 years was unchanged compared to 2012 (35.0 per 100,000 acute occupied bed days). Compared to 2012, the prevalence of ribotype 078 has decreased though this type remains the predominant one in Scotland. Previously epidemic ribotypes 001, 027 and 106 remain at low levels in Scotland. HPS has been involved with linking outcome data (including morbidity and mortality) to CDI case data to develop a more detailed picture of the epidemiology and impact of CDI on patient health, and to inform interventions to further reduce the burden of CDI in Scotland.
Figure 3: Annual CDI incidence rates in patients aged ≥65 and 15-64 years* in Scotland per 100 000 bed days (2007 to 2013)
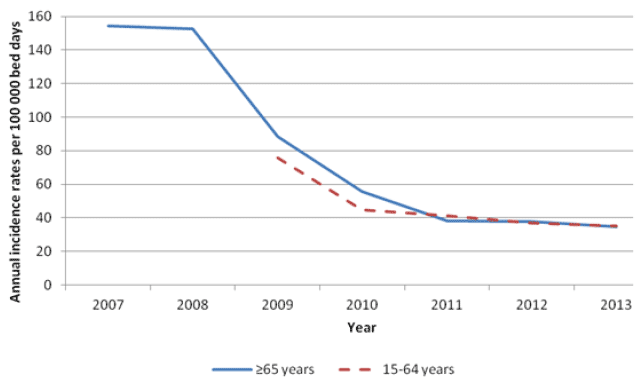
*surveillance in 15-64 years age group began in April 2009
Outbreaks
In 2013, a total of 49 health-care associated outbreaks were reported to HPS of which: seven were of the highest category Hospital Infection Incident Assessment Tool (HIIAT) red, 30 were HIIAT amber and nine were HIIAT green. Three outbreaks were not HIIAT assessed as they arose in care homes or were awaiting laboratory confirmation which was subsequently not confirmed.
Figure 4 shows the infection types that arose in healthcare related outbreaks reported during 2013. The most commonly reported outbreaks involved gastrointestinal and respiratory infections. The most common organism causing gastrointestinal outbreaks was norovirus (n=11) and for respiratory outbreaks was influenza (n=7). The majority of these outbreaks occurred in Care of the Elderly wards.
Figure 4: Types of infections in HAI outbreaks (number of events) reported to HPS during 2013
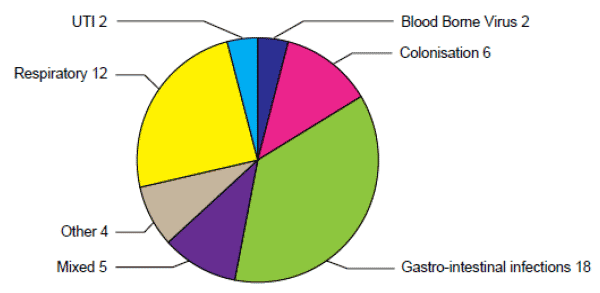
Carbapenemase producing Enterobacteriaceae
Multidrug resistance among Gram-negative organisms continues to be a major threat to public health and patient safety. In particular, the emergence of carbapenemase producing bacteria is concerning as this leaves few options to treat severe infections. In 2013, a total of 22 carbapenemase producers were reported to HPS from the Antimicrobial Resistance and Healthcare Associated Infection (AMRHAI) Reference Laboratory at Public Health England (PHE), bringing the total number of reports in Scotland to 101 since 2003. In a summary report from PHE, it was estimated that confirmed carbapenemase producers from Scotland accounted for 3.2 % of all UK carbapenemase producers in this period.
Controlling Antimicrobial Resistance in Scotland (CARS)
In September 2013 the Department of Health and Department for Environment, Food and Rural Affairs published a UK-wide five year antimicrobial resistance strategy (agreed between the governments of the four UK nations and involving human and animal health agencies). This strategy is aimed at slowing the development and spread of antimicrobial resistance and will be co-ordinated across the UK. In Scotland, the Scottish Management of Antimicrobial Resistance Action Plan (ScotMARAP) has been refreshed and an overarching Controlling Antimicrobial Resistance in Scotland (CARS) group has been established to ensure that all areas of the strategy are implemented. Prevention of infection in healthcare is essential to reduce cross-transmission of resistant organisms and reduce the need for antibiotics.
Summary
The continuing plateau in the incidence of key HAIs, and the emerging threat from AMR, indicates the need for changes in strategy to ensure we have no harm from preventable infection in Scotland. HPS will support boards to ensure intelligence gathered during 2013 will be translated into clinical practice and that interventions are informed by the evidence base. The integration of health and social care in Scotland will bring new challenges in the monitoring, and infection prevention and control of infections associated with healthcare. Strategies to contain AMR will become a real focus for work in the coming year and an integrated approach between this and the prevention of HAI in all care settings will be essential to ensure the safety of patients and the public and our continued ability to treat common infections.
Travel & International Health
Health Protection Scotland is responsible for surveillance of travel-related infectious disease imported in Scotland and also works to protect the health of travellers from Scotland by provision of appropriate health advice to professionals and members of the public.
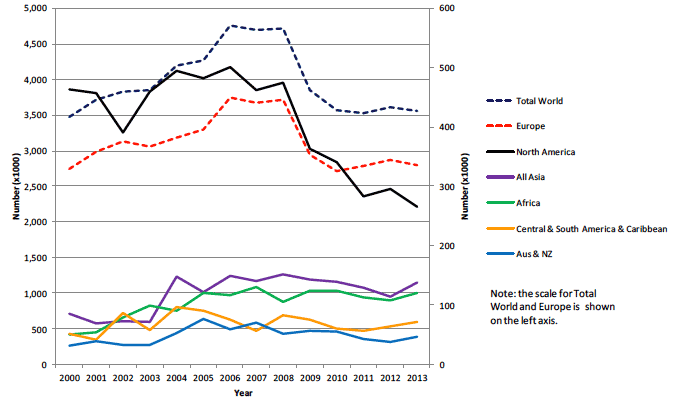
In 2013, there were approximately 3.6 million journeys abroad from Scotland, representing 6% of total journeys from the UK. Europe (78%) was the most visited destination followed by North America (7%), Asia (4%), Africa (3%), Central, South America and the Caribbean (2%) and Australia and New Zealand (1%) (Figure 5)
Figure 5: Travellers from Scotland (Source: Office for National Statistics, Travel Trends)
Imported infection
Those infections which are reported to HPS as imported are included in the annual totals of travel-related infection.
In 2013, 159 episodes of schistosomiasis were reported, making this the infection most frequently reported as being travel-related. It is advised that travellers who bathe in fresh water in endemic countries are tested for infection on their return home. School visits to countries where Schistosoma sp. and other pathogens are endemic are now common place and HPS has developed guidance specifically for this group of travellers. (HPS. Travel Health Guidance for Schools. Available at: http://www.fitfortravel.nhs.uk/media/405657/travel%20health%20guidance%20for%20schools%20feb%202013.pdf).
Non-viral gastrointestinal infections were among the most frequently reported as being travel-related, the most common being Giardia sp (43) followed by Escherichia coliO157 (31) andShigella sp. (29). It is likely that the true figure for traveller's diarrhoea is greater than that reported. Thirteen reports of enteric fever comprised 10 reports of typhoid and 3 of paratyphoid. Vibrio infections were less common, with five reports of Vibrio parahaemolyticus and one of V. cholerae. Imported viral hepatitides were infrequently seen, with a total of three reports of Hepatitis A and two reports of Hepatitis E. (HPS Weekly Report 22 January 2014 Volume 48 No. 2014/03 ISSN 1753-4224 (Online) Available at: http://www.hps.scot.nhs.uk/documents/ewr/pdf2014/1403.pdf)
Fifty-nine reports of malaria were made in Scotland in 2013, 3.9% of the UK total of 1,501. This is an increase of 9% since 2012 (54), the same percentage increase as for the UK as a whole. Of the Scottish total, 40 were identified as P. falciparum and 15 were P. vivax. P. ovale (3) and P. malariae (1) comprised the remainder. Eighty-three percent of these infections were acquired in Africa. One death from P. falciparum malaria acquired in West Africa was reported in Scotland in 2013.
Enhanced surveillance is now carried out for all malaria diagnosed in Scotland, and the quality of data is much improved with travel history available for all reports made in 2013. Further information is available at (HPS Weekly Report 6 August 2014 Volume 48 No. 2014/31 ISSN 1753-4224 (Online) http://www.hps.scot.nhs.uk/documents/ewr/pdf2014/1431.pdf)
Of the other vector-borne infections reported in 2013, dengue virus (31) was most common. There were two reports of chikungunya virus. Both of these infections are widespread in tropical and sub-tropical climates, and are increasingly found in those parts of the temperate zone that can support the viruses' mosquito vectors. Two reports of Leishmania sp, which is transmitted by sandfly bites in temperate and tropical zones, were made in 2013.
HPS maintains two websites carrying up to date evidence-based travel health advice. TRAVAX (http://www.travax.nhs.uk) is available to health care professionals in Scotland and elsewhere and has detailed information on vaccination and risk of infections such as dengue fever and malaria. Outbreaks are published on TRAVAX to highlight increased risk for travellers, as are advice and recommendations to help reduce the risk. Fitfortravel is aimed at the general public and is available at: www.fitfortravel.nhs.uk.
Global Health Threats
As in previous years, the international occurrence of infectious diseases of global importance such as influenza, measles and poliomyelitis was monitored and responded to by HPS in 2013.
Middle East respiratory syndrome coronavirus (MERS-CoV), formerly novel coronavirus, was of particular concern having become established in the Arabian Peninsula during 2013, with imported cases appearing in other geographic regions, including Europe, throughout the year.
In preparation for the 2014 XX Commonwealth Games in Glasgow, during 2013 HPS increased activity around surveillance and emergency planning to ensure Scotland can predict and respond to established and emerging global health threats, particularly those posed by infectious diseases. The legacy of this for health protection will be invaluable and long-lasting.[3]
Tobacco
Tobacco remains the primary preventable cause of ill health and premature death. Each year in Scotland, it is associated with over 13,000 deaths (around a quarter of all deaths in Scotland every year) and 56,000 hospital admissions. Annual costs to Scotland's health service associated with tobacco-related illness are estimated to exceed £300m and may be higher than £500m.
Reducing the number of people who take up smoking, supporting those who do smoke to quit and protecting people from second-hand smoke have long been clear public health priorities for the Scottish Government.
On 27 March 2013 our latest Tobacco Control Strategy, Creating a Tobacco-free Generation, was launched. This reaffirmed our vision for a tobacco-free Scotland and set a world-leading target to achieve this by 2034. This will mean that a child born in 2013 will become an adult in a Scotland, which is largely devoid of tobacco-use with all the health, social and economic benefits that entails.
This is a challenging target. Achieving it will require a determined effort to support people to choose not to smoke. Our strategy sets out a package of measures to move us along this journey over the next five years.
It is therefore disappointing to see that national smoking rates have stalled since around 2011 and concerning to see a slight rise in our 20% most deprived areas. Scotland's most deprived areas not only have the highest smoking rates but also the greatest incidence of disease and lowest life expectancy - these facts are not unconnected.
To help address the inequalities that tobacco contributes to, Boards are working towards a new HEAT target for 2014/15 which is focussed on our most deprived areas (NHSScotland to deliver universal smoking cessation services to achieve at least 12,003 successful quits, at three months post quit, in the 40% most deprived within-board SIMD areas (60% for Island health boards) over the two years ending March 2016). It is vital that we ensure services are best placed to support smokers to make the decision to quit and to sustain that quit. NHS Health Scotland have recently completed a review of cessation services across Scotland and the Scottish Government will work with Boards to consider what additional steps need now to be taken to achieve the new target.
Scottish Government continues to build an environment that supports people, particularly our young, to choose not to take up smoking. Scottish Ministers have led the way in the UK on the commitment to introduce standardised packaging of tobacco products. We are now working with the UK Government and devolved administrations in Northern Ireland and Wales to introduce this policy.
Looking forward, we are facing emerging challenges with the appearance of new alternatives to smoking. In recent years there has been a significant increase in availability and take up of electronic cigarettes, also known as Electronic Nicotine Delivery Systems (ENDS). Currently there is much debate amongst public health experts about the potential benefits and possible harms of these products, as the evidence base continues to grow. It is widely acknowledged that ENDS are likely to be less harmful than tobacco and could potentially assist smokers to quit tobacco use. However, there is a growing consensus that they should be regulated in a way that protects against any activity that could promote take up amongst non-smokers, particularly young people. The Scottish Government is actively considering what action needs to be taken in Scotland to deal with the public health issues associated with electronic cigarettes.
Alcohol
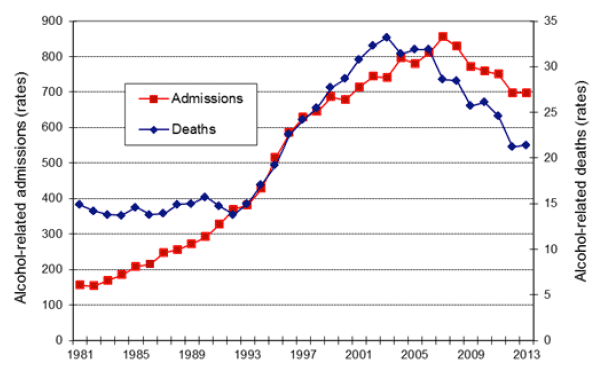
Scotland's relationship with alcohol is rarely far from the national headlines. While we have seen some improvements in alcohol-related hospital admissions and deaths in very recent years, our nation remains light years away from the low numbers of 1980, after which the affordability and availability of alcohol soared. Today, we are living with the consequences, including the fact alcohol-related deaths increased again, by 2%, in 2013. Given the established link between affordability and alcohol-related harm, the increase in deaths may be linked to the improving economic environment in Scotland.
Figure 6: Alcohol Hospitalisations and Deaths in Scotland 1981-2013
The Scottish Government's comprehensive Alcohol Framework contains over 40 measures, many of which have been implemented successfully. For example, in the year ending March 2014 Scotland's NHS Boards carried out 104,356 Alcohol Brief Interventions, far exceeding the HEAT Standard of 61,081. Boards are to be greatly commended on this achievement, which needs to be sustained in future years.
One crucial measure, Minimum Unit Pricing (MUP), has not been implemented as yet, due to the ongoing legal challenge by parts of the alcohol industry. There are many others within the industry who endorse the measure, and it continues to enjoy public support. The Scottish Government remains absolutely committed to continuing to pursue the policy goal of Minimum Unit Pricing - it is the most equitable approach to tackling the serious health problems arising from easy access to cheap, strong alcohol.
Health Promoting Health Service
An NHS Scotland which places health improvement at its core is a strongly held Scottish Government ambition and is beginning to be realised in hospital settings. The Health Promoting Health Service (HPHS) concept ("every health care contact is a health improvement opportunity") was launched in 2008 with the publication of CEL 14 (2008) http://www.sehd.scot.nhs.uk/mels/CEL2008_14.pdf. The concept is simple. It is founded on the belief that many of the 150,000 plus NHS Scotland staff have the right skills and knowledge to not only treat illness, but also to promote health and wellbeing. We need to use as much of that capacity as possible to ensure that, over time, health improvement becomes as much the mainstream business of NHS Scotland as health care delivery. Health promotion in acute care settings offers a significant opportunity to improve health and given the proportionately greater use of acute services by patients from deprived communities - to reduce inequalities. The 2008 CEL tasked Boards with implementing specific health promoting actions on smoking, alcohol problems, breast feeding, food and health and health at work. In 2012 an update was issued http://www.sehd.scot.nhs.uk/mels/CEL2012_01.pdf, building on progress made over the preceding 3 or 4 years, and again tasked Chief Executives, Directors of Public Health and Medical Directors with implementing specific health improvement actions in hospitals. A further three actions in the areas of sexual health, physical activity and active travel were added to the five in the original CEL.
An NHS Scotland which promotes healthier choices amongst its patients, visitors and staff has been increasingly evident in the last year. There has been a rise in the number of patients referred to smoking cessation support, and a substantial increase in the number of conversations taking place between patients and health professionals on the benefits of physical activity, in both preventing and mitigating a wide range of clinical conditions. Improvements in the hospital environment are also clear, with healthier food choices on offer to staff, patients and visitors and increased efforts to eradicate smoking on hospital premises.
NHS Scotland's own retail brand (the Aroma Brand) developed by Health Facilities Scotland (HFS), is presently operating in a number of Boards across Scotland. It provides a high street retail offer to staff and visitors and conforms to the Healthyliving award criteria to provide healthier food choices for staff, visitors and patients. Aroma outlets also provide the opportunity to maximise income generation direct to the NHS from retail and other income generating opportunities, which can be used to improve patient experience and safeguard jobs. The brand has been very successful in reducing subsidy and providing substantial profit back into patient care.
All of the progress with HPHS has been the result of a concerted effort by NHS Boards (with the help of Health Scotland) to successfully embed preventative action into every day routine practice. A Ministerial Group chaired by the Minister for Public Health has been established, and each NHS Board now has a non-executive director acting as a Champion for the HPHS concept.
However, although substantial progress has been made, much remains to be done. To date clinical leadership - in particular from the medical profession has been limited. The importance of clinical involvement in this agenda should not be underestimated. All clinical groups - doctors, nurses, AHPs and pharmacists have crucial a role to play in promoting healthy behaviours. The myth that this takes up too much time during a clinical encounter needs to be debunked. It takes a matter of minutes to ask about smoking, alcohol consumption and levels of physical activity and then signpost patients to sources of further advice and support. The non-executive Champions have been tasked with helping to map existing referral pathways in hospitals for this kind of patient follow-on support, so that clinical staff (particularly doctors) can be reassured that these conversations and onward referrals will not place an undue burden on their time.
Once the onward referral pathways work has been completed, the Ministerial Group will help to promote awareness widely, particularly within the clinical community. The Group is also giving thought to the next iteration of the Health Promoting Health Service, building on progress to date.
Organ Donation in Scotland
There have been dramatic changes in the field of transplantation over the last 25 years. In patients with terminal heart, liver or lung failure, transplantation currently offers the only option for survival, and renal transplantation is now established as the optimum treatment for irreversible kidney failure. Yet, tragically, around 50 people in Scotland die each year because donated organs are not available.
The donation and transplantation of organs programme operates on a co-ordinated and collaborative basis across the UK. The fact that the UK (and Scotland within the UK), had one of the worst records for organ donation in Western Europe prompted the setting up of the UK Organ Donation Taskforce in 2006. Its first report, Organs for Transplants was published in 2008 www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_082122 and contained 14 recommendations for action, all of which were accepted by all four UK health administrations. The Taskforce was convinced that if all 14 recommendations were implemented in full, a 50% increase in organ donation was achievable across the UK within 5 years. The Scottish Transplant Group, which provides expert advice to Ministers on matters relating to organ donation and transplantation, was tasked with implementing the recommendations in Scotland.
Key actions included:
- Strengthening the network of donor transplant co-ordinators (now called Specialist Nurses for Organ Donation) and centralising their employment within the UK Organ Donation Organisation, NHS Blood and Transplant;
- Appointing a Clinical Lead for Organ Donation, usually an intensive care consultant, in every ICU;
- The establishment of a Donation Committee in each NHS Board to monitor donation activity;
- Regular Scotland-wide high profile media and advertising campaigns;
- CMO Guidance on Legal Issues relevant to Donation following Circulatory Death. www.sehd.scot.nhs.uk/cmo/CMO(2010)11.pdf
Between April 2009 and March 2013, organ donation numbers in Scotland rose by 74.1% and the transplant waiting list dropped. 41% of the Scottish population were on the NHS Organ Donor Register - the highest percentage of all the UK countries, with the UK average being 31%.
In spite of this improvement, the Scottish Transplant Group considered that more could be done, and in July 2013 the Scottish Government published A Donation and Transplantation Plan for Scotland 2013-2020 www.sehd.scot.nhs.uk/cmo/CMO(2012)08.pdf. This sets out the ways in which donation and transplantation in Scotland can be further improved and builds on the very good progress made under the auspices of the Organ Donation Taskforce. The plan was developed as a companion piece to the over-arching Strategy Taking Organ Transplantation to 2020 http://www.nhsbt.nhs.uk/to2020/the-strategy/strategy/ developed by the four UK countries and NHS Blood and Transplant.
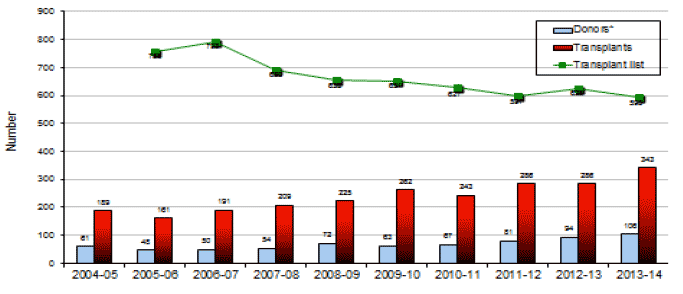
One year into the delivery of the Plan we have seen continued good progress. From the baseline year of 2007-08 we now have a 96% rise in organ donation numbers and a 63% increase in solid organ transplants, along with a fall in the transplant waiting list.
Figure 7: Deceased donors, transplants and transplant waiting list, Scotland.
Organ donation and transplantation is complex and multi-faceted and no single thing can revolutionize donation rates. Our plan sets out twenty one recommendations across the organ donation pathway and commits us to meet certain targets by 2020:
- Overall deceased donation rates will increase from 17.9 per million population in 2012/13 to 26 per million population;
- Overall transplantation rates in Scotland from deceased donors will increase from 65.8 to 74 per million population;
- Family authorisation rates in donation after circulatory death will increase from around 50% to 80%;
- Family authorisation rates in donation after brainstem death will increase from around 78% to 85%.
All solid organ transplant services, with the exception of adult renal transplantation, are nationally commissioned by National Services Division (NSD). An initial impact assessment undertaken by NSD has suggested that implementation of the UK and Scotland strategies is likely to increase solid-organ transplantation levels in Scotland by 48% from 344 in 2012/13 to around 510 transplants in 2019/20, with increases in the number of transplants using organs from both deceased and living donors. This significant level of growth in transplantation will need careful planning in order to ensure that transplant services continue to meet the needs of all of their patients.[4]
Contact
Email: Mark Johnstone