Annual Report Of The Chief Dental Officer 2012
Inaugural Annual Report on the dental health of the Scottish population from the Chief Dental Officer, Margie Taylor.
2. Oral Health of the Population: The Facts and Key Issues
2.1 Demographics
Scotland's population currently totals 5,222,100 (http://www.gro-scotland.gov.uk/statistics/theme/population/projections/scotland/2010-based/index.html) and is spread over an area of 78,772km2, including a more urbanised central belt, remote rural areas and many islands. As the geographic area is very diverse, there are major challenges in ensuring the health needs of the population are met.
2.2 Socio-Economic Status and Social Disparity
The health experience of the population is far from evenly distributed, with some communities experiencing much poorer health and greater health risks than others. The Office of National Statistics (ONS) published life expectancy at birth figures for the UK in 2011 (www.ons.gov.uk/ons/publications/re-reference-tables.html?edition=tcm%3A77-223356). These present a stark picture of health inequalities, with 8 out of the 10 lowest-ranked life expectancy areas in the UK (total number of areas = 404) situated within Scotland. The life expectancy at birth in Glasgow City (ranked lowest at 404) was 71.6 years, compared with 85.1 in Kensington and Chelsea (London); by contrast, life expectancy in East Dunbartonshire was 79.4.
The area-based Scottish Index of Multiple Deprivation (SIMD) is commonly used as a proxy for socio-economic status at a population level and shows clearly the variance in health experience between the most deprived and most affluent areas. The causes of this variance are complex and rooted in both historical and contemporary social events that have an impact on some communities more than others. A key message shared by the Chief Medical Officer, Sir Harry Burns, talks of "the biology of deprivation", which refers to the causes of the causes and does not put ill health and inequalities solely down to our behaviours. It is a phenomenon more complex than simply the effect of poor diet and smoking, and one whereby additional, psycho-social problems prevent people from having control over their lives.
2.3 Population Projection
Figure 2.1 shows the projected change in the population age profiles for Scotland between 2010 and 2035. This indicates that by 2035 Scotland will experience a reduction in the child population and a significant increase in the number of older people, factors which will have major implications for service demand. Although many older people consider themselves to be in good health, the proportion of the population living with long-term illnesses and self-reported ill health increases sharply with age. Older people are more likely to suffer from co-morbidities and age-related frailty. These factors all have an impact on dental services, particularly the potential increase in demand for domiciliary dental care.
Figure 2.1 Projected change in the population age profiles for Scotland between 2010 and 2035
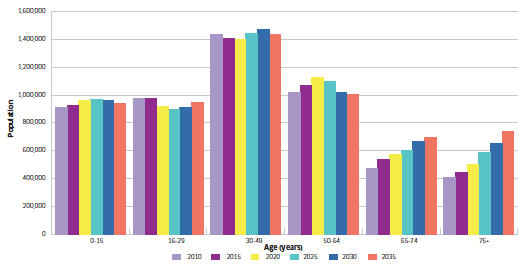
2.4 Oral Health and Oral Disease
Oral health is more than just having healthy teeth in a healthy mouth; it is integral to general health and wellbeing and is a determinant of quality of life. Good oral health enables us to eat, speak, smile, taste, chew and swallow.
On the contrary, oral disease can have detrimental effects on an individual's health and wellbeing and can impact significantly on work, school and other daily activities. Various conditions are classified as "oral disease" but the two commonest conditions are dental caries (tooth decay) and periodontal (gum) disease; the condition that is of most concern, due to its seriousness and increasing incidence, is oral cancer.
Dental caries and periodontal disease are very common and largely preventable and are therefore considered widespread public health issues. Despite significant improvements over the past 30-40 years, there remains high prevalence of dental caries.
The relationship between oral health and general health is well documented, with oral disease and non-communicable chronic disease sharing many common risk factors. Moreover, many general conditions either have oral manifestations or can affect dental treatment.
2.5 Epidemiology and Data
Epidemiology is the science concerned with the study of factors determining and influencing the frequency, distribution and control of diseases in populations. Scotland is fortunate to have some of the best health service data in the world combining high quality, consistency, national coverage and the ability to link data to allow secure, confidential patient-based analysis and follow-up.
2.6 Demographics
2.6.1 Trends in children's oral health
The National Dental Inspection Programme (NDIP) surveys are conducted each year in Scotland's schools and provide information on trends in children's oral health.
NDIP invites every Primary 1 (P1) and Primary 7 (P7) child in local authority schools to have a basic dental inspection carried out; a representative sample of these children receive a detailed dental inspection (P1 or P7 in alternate years). These inspections are a core component of the public health function of the NHS community dental service across Scotland. The main aim of the inspections is to inform parents/carers of their child's oral health and convey the degree of urgency of a dental appointment for the child. The results are also used in the planning and evaluation of local and national oral health initiatives to ensure the appropriate use of resources.
Figure 2.2 illustrates the trends of both P1 and P7 from 2003 to 2012 and shows a very encouraging picture of continual improvement in the proportion of children with no obvious decay experience.
In the school year 2011/12, the detailed inspection programme involved P1 children (www.isdscotland.org/Health-Topics/Dental-Care/Publications/2012-11-27/2012-11-27-DentalNDIP-Report.pdf?41798037291) and provided the following key results:
- 67.0% of P1 children had no obvious decay experience, compared with 42.3% in 1988.
- This was the first year that all NHS boards met the 2010 national target of 60% to have no obvious decay experience.
The 2011 NDIP Report focused on P7 children and reported that:
- 69.4% of P7 had no obvious decay experience.
- For the first time, all NHS boards achieved the 2010 national target of 60% of P7 children to have no obvious decay experience.
Figure 2.2 Trends over time in the proportion of P1 and P7 children with no obvious decay experience; 2003-2012
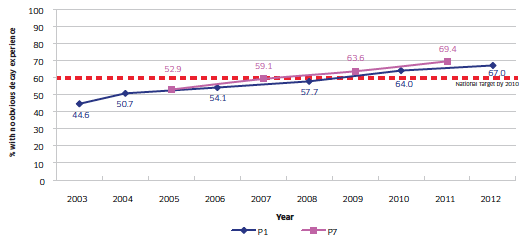
Source: NDIP reports 2003-2012
2.6 Demographics
While the results in Figure 2.2 are positive, the underlying message is that still nearly one third of children experience dental decay, which is reported as the number of decayed, missing and filled teeth. Among those children who did have decay, the number of teeth affected by obvious decay experience has decreased from 2.73 in 1988 to 1.35 in 2012. The changes over time in the mean number of decayed, missing and filled teeth are shown in Figure 2.3 and illustrate a steady improvement for both P1 and P7 children.
This mean number masks the unequal distribution of dental caries. Those with the disease have a higher burden of disease, but the average number of teeth affected by decay has also declined.
Figure 2.3 Comparison over time of the mean number of decayed, missing and filled deciduous/permanent teeth (d3mft/D3MFT) in the P1 and P7 populations and the mean number of decayed, missing and filled deciduous/permanent teeth in those children with decay (d3mft/D3MFT>0); 2005-2012
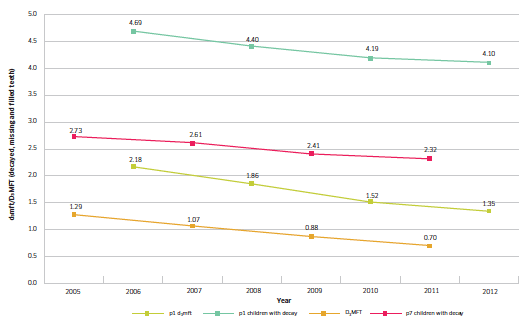
Sources: NDIP reports 2005-2012
Although the target of 60% of P1 children to have no obvious decay experience was reached at Scotland level in 2010, for the first time, all NHS boards across Scotland achieved the target in 2012.
This level of achievement across NHS boards relative to the target is illustrated in Figure 2.4.
Figure 2.4 Proportion of P1 children with no obvious decay experience by NHS board; 2012
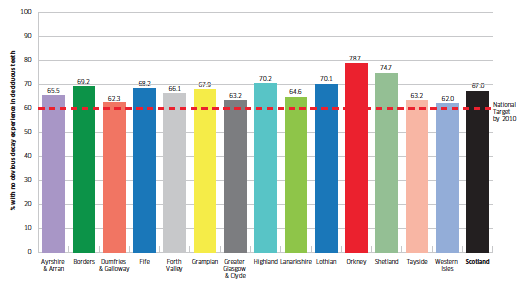
2.6.2 Trends in children's dental general anaesthesia
Dental general anaesthesia still accounts for the highest amount of inpatient and day-case hospital activity for elective surgery in children. General anaesthesia is not without risk and causes anxiety and stress to both the child and family. The procedure is a burden on resources and results in time off school (and time off work for the child's parents/carers) and remains a major public health problem, despite dental caries being a largely preventable, non-communicable disease.
The historical data for this activity have come from a variety of sources and should be interpreted with care; however, the latest figures (see Figure 2.5) for trends in dental general anaesthesia are more positive and heading in the right direction. The general picture is that there has been an overall reduction in general anaesthetics for dental extractions, which is encouraging, given the continuing investment in preventive oral health initiatives, particularly Childsmile (www.child-smile.org.uk), the national oral health programme for children.
Figure 2.5 Rates per 10,000 child population for general anaesthesia procedures for dental extractions in 0-17 year olds; 2002-2011
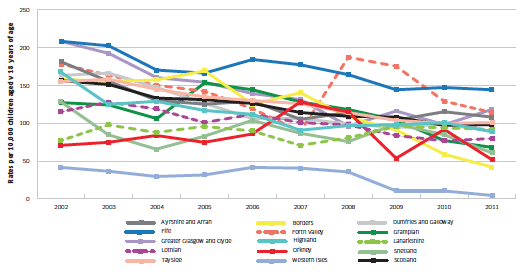
Sources: SMR01, SMR13 and local data
2.6.3 Trends in the oral health of adults
Every 10 years from 1968, Scotland took part in UK-wide Adult Dental Health Surveys (ADHS). The results of these surveys - available at Scotland level only - show a continuous improvement in dental health from the 1970s. Since 2009, Scotland has relied on data from the Scottish Health Survey (SHS).
The latest data - which enable comparisons to be made across NHS board areas - come from the combined 2008-2011 surveys. SHSs report that 89% of the adult Scottish population (here, those aged over 16) had some or all of their own natural teeth, which is just below the 2005 Dental Action Plan's target of 90% by 2010. Figure 2.6 shows the proportion of adults with no natural teeth, 19 or fewer natural teeth and 20 or more natural teeth.
Figure 2.6 Proportion of adults aged 16 and over with natural teeth by NHS board; 2008, 2009, 2010, 2011
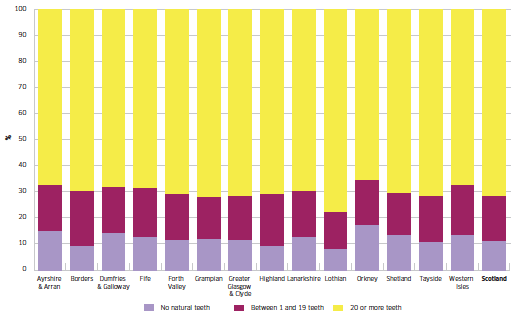
Source: www.scotland.gov.uk/Resource/0040/00402718.xls
Although people in the older population are no different in having needs that reflect the stage in life they have reached, their specific oral health needs have changed significantly over the past forty years; at one time, care of older patients focused on fitting full sets of dentures, but the most recent SHS shows that the majority of older people have retained some or all of their natural teeth. Therefore, better oral health, combined with the development of new treatments and technologies, brings a new set of challenges. The cohort of adults aged 30-40 have different needs, meanwhile: having experienced little dental treatment, they require a more preventive approach to their care and have greater expectations of their oral health maintenance.
2.6.4 Oral cancer trends
Oral cancer is a group of cancers that affect the mouth and has many definitions due to the way the anatomical sites of the mouth and the surrounding structures are clinically coded. For the purposes of this report, oral cancer has been defined as cancer of the tongue, gum, floor of the mouth, palate and other unspecified parts of the oral cavity and does not cover the lip or the wider oro-pharynx sites.
The latest figures indicate that there continues to be an increase in the incidence of oral cancer, while that of other cancers is decreasing; and while oral cancer is predominantly a disease of older people, an increase is now being seen in younger age groups. The major risk factors in the development of oral cancer are tobacco use and the excessive consumption of alcohol.
Dental teams, as part of the general health team, need to support key messages about common risk factors, encourage behaviour change and carry out opportunistic screening. The Scottish Government is working on legislation around alcohol pricing and the drink-driving level, following the introduction in 2006 of the law banning smoking in public places.
Figure 2.7 shows the 5-year summary incidence of oral cancer broken down by sex and NHS board. Incidence rates vary between NHS board areas, and oral cancer is twice as common in males compared to females.
Figure 2.7 Cancer of the oral cavity; 5-year summary of incidence by NHS board (European age-standardised incidence rates); 2006-2010
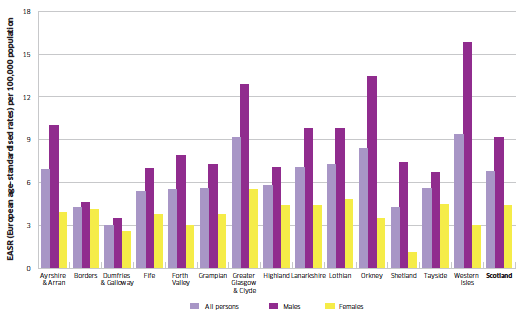
Sources: www.isdscotland.org/Health-Topics/Cancer/Cancer-Statistics/Head-and-Neck/#oral and www.isdscotland.org/Health-Topics/Cancer/Publications/2012-04-24/si_cancer_head_neck.xls
During the past 30 years there has been little improvement in the oral cancer survival rate, despite advances in medical treatment and efforts to promote early detection. Figure 2.8 illustrates the trend over the period 1983-2007 with outcomes dependent on the type, site and stage of cancer and its presentation. Women have higher survival rates than men, but the mean 5-year survival rate is approximately 50%.
Figure 2.8 Trends in 5-year survival for men, women and all persons diagnosed with oral cancer; 1983-2007
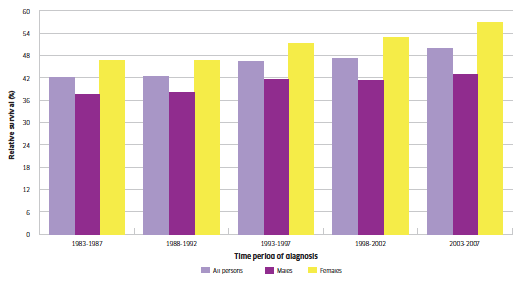
Source: www.isdscotland.org/Health-Topics/Cancer/Cancer-Statistics/Head-and-Neck/s_cancer_oral.xls?1
A well recognised association exists between oral disease and deprivation; trends suggest that the burden of disease is concentrated in more deprived populations.
Inequalities persist across socio-economic groups despite an overall improvement in oral health. A key priority is to reduce oral health inequalities while promoting oral health improvement for all.
Oral health inequalities, to a large extent, are avoidable. A reduction in inequalities will be seen when the oral health of those in more deprived areas improves at a faster rate than that of those in less deprived areas. Oral health initiatives which have a population-wide approach as well as a targeted approach will help improve oral health overall, while investing additional resources in more deprived areas will help reduce inequalities; this approach has been called "universal proportionalism" by Professor Sir Michael Marmot. There is much interest in this approach, which is being used and closely monitored within the Childsmile programme.
Focusing solely on the disadvantaged will not reduce health inequalities sufficiently. To reduce the steepness of the social gradient in health, actions must be universal, but with a scale and intensity that is proportionate to the level of disadvantage.
Fair Society, Healthy Lives
Marmot 2010
(www.instituteofhealthequity.org/projects/fair-society-healthy-lives-the-marmot-review)
The area-based Scottish Index of Multiple Deprivation (SIMD) is commonly used as a proxy for socio-economic status and identifies small-area concentrations of multiple deprivation at data zone level. The index combines seven domains to rank relative multiple deprivation across Scotland. It is useful for showing the variance in health experience between the most deprived and the least deprived quintiles (fifths) of the population.
The recently published Audit Scotland report on Health Inequalities in Scotland (www.audit-scotland.gov.uk/docs/health/2012/nr_121213_health_inequalities.pdf) found overall health has improved over the past 50 years but there are still significant differences attributable to deprivation and other factors. Despite the significant investment made and priority given by successive governments, most indicators show little reduction in health inequalities. The report recommendations included the need to (i) develop measures to assess the short-term impact of strategies which aim to improve health and reduce health inequalities in the long term, (ii) assess the impacts of policies on the population as a whole, and (iii) share learning and publish data at a local level to show progress in reducing health inequalities.
2.7.1 Inequalities in children's oral health
The 2012 NDIP figures for P1 children show a continuing improvement in oral health for children from all socio-economic backgrounds compared with the results from 2010. This is rightly seen as a success but clear inequalities still remain, with 33% of 5-year-old children having signs of obvious decay experience. The NDIP findings show the uneven distribution of caries, with a relatively small proportion of the population having a high burden of disease. However, they do also show a reduction over time in the average number of decayed teeth in children with the highest levels of disease.
The clear relationship between deprivation and dental decay can be seen in Figure 2.9, with oral health improving while inequalities persist: 81% of children in the least deprived areas have decay-free mouths, compared with just 50% in the most deprived areas.
Figure 2.9 Proportion of P1 children with no obvious decay experience in Scotland by SIMD quintile; 2008, 2010, 2012
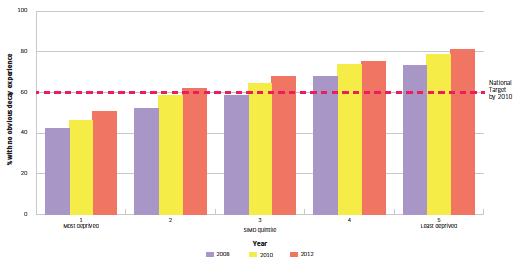
Figure 2.9 shows that proportionately more children in deprivation quintile 1 (most deprived) had still not reached the 2010 target by 2012.
Inequalities can be measured by examining absolute inequality, which is the difference in values between the least and most deprived groups. Figures for absolute inequality in children's oral health have remained constant over the past 4 years (30.9% in 2008 and 30.7% in 2012). Clearly, much still has to be done to reduce inequalities in the oral health of Scotland's children.
2.7.2 Inequalities in adults' oral health
The Scottish Health Survey is conducted annually and samples adults and children from private households across Scotland. In 2011, over 7,500 adults were surveyed and approximately 2,000 children.
The 2011 Scottish Health Survey found significant association between deprivation and the number of natural teeth present in sampled adults. The proportion of adults living in the least deprived areas who had some natural teeth was 94%, compared with 83% of those in the most deprived areas; nearly three times as many people from the most deprived backgrounds (17%) as those from the least deprived (6%) had no natural teeth (www.scotland.gov.uk/Publications/2012/09/7854/18).
Oral cancer incidence is strongly associated with deprivation and Figure 2.10 demonstrates the difference between those living in the most deprived areas and least deprived areas. Survival is lower among individuals from more deprived backgrounds and incidence is almost three times the rate of those in the least deprived quintile.
Figure 2.10 Incidence of oral cavity cancer by SIMD quintile; 2006-2010
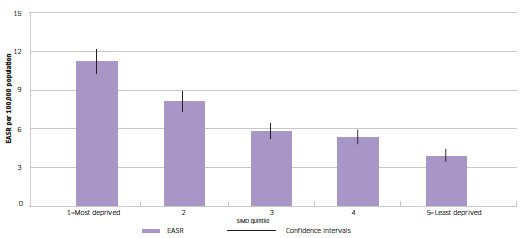
Sources: Scottish Cancer Registry, ISD (incidence); National Records of Scotland (NRS) (mortality and populations)
Data extracted September 2012
Contact
Email: Elizabeth McLear