Introduction
Aim, vision and making it happen
Transforming Outpatient Services is aimed at supporting NHS Boards and local partnerships to move care closer to home and enable more people to receive the right care, from the right person, at the right time, in the right place.
It supports teams working together with patients and the public to understand and diagnose system issues, design and innovate and use continuous improvement to deliver high-quality, person-centred care and best value for money.
Healthcare teams, working with patients and public representatives, have developed Towards Our 2020 Vision a picture of how the services that we currently call outpatient services will need to change for patients and staff as we move towards 2020. (See page 17) (Towards Our 2020 Vision is available in poster format from QuEST.)
Now all NHS Boards working with partners are beginning to take the strategic actions necessary to create the contextual, cultural and leadership conditions to enable staff, practitioners and patients to achieve their 2020 vision. Some Boards have already formalised outpatient transformation as a strategic priority. In other Boards specialties, or teams are undertaking improvement led by enthusiastic service managers, or clinicians who may or may not have been given support and resource.
Four NHS Boards have been commissioned (2012-14) to use three different improvement methodologies: invention and innovation through technology; benchmarking to improve utilisation of appointment resources and clinic space; and rapidly testing changes and contributing to change packages that help spread reliable improvements.
This year (2013-14), Chief Executives of all NHS Boards agreed to support rapid adoption and spread of five evidence based, high impact change concepts. Getting patients on the right pathway through transforming Community Allied Health Professional MSK services is one of these. (See page 18 for the Transforming Outpatient Services Driver Diagram.)
Are we making the right changes?
Scotland's AHP MSK services deal with high volume demand, currently 400,000+ referrals annually. It is estimated that: 20-30% of all GP consultations have an MSK component; 10 million work days are lost annually and people with an MSK condition make up 22% of those receiving incapacity benefit.
MSK conditions have significant consequences for the individual, but also significant impact on a wider socio-economical scale. The volume of referrals to orthopaedics is also high, with duplication across general practice, orthopaedic and AHP services, providing opportunities for integrated pathways, new innovative teamworking and a reduction in the variation in patient experience.
It has been estimated that between 10% to 40% of new orthopaedic referrals do not require a surgical opinion and of patients on a waiting list, between 5% and 15% do not want or need surgery. It has therefore been considered important that General Practitioners (GPs), orthopaedic services and AHP services work in unison to ensure that referrals are appropriately reviewed to ascertain which patients require acute hospital referral and those patients who could benefit from rapid access to more locally based community services. The success of this approach requires
a collaborative approach between primary, secondary and community care and adherence to recognised referral criteria.
The aim of getting patients on the right pathway through transforming Community Allied Health Professional (AHP) MSK services, is to improve the patient's pathway of care; the patient's experience; reduce whole journey waiting time; and reduce the number of unwarranted outpatient clinic attendances. This will enable people with MSK problems across Scotland to have easy access to a self-management resource and early appropriate advice and, if necessary, assessment by an efficient AHP service to get them started on the right pathway for their treatment first time.
Rapid Access to AHP MSK Services (4 weeks) has been included as a priority in the 2020 Local Delivery Plans.
What is the purpose of the change package?
The change package describes in detail the steps needed and how to plan for, adopt, implement and monitor effectiveness of AHP musculoskeletal pathways. It includes evidence base, resources, information and contacts for teams to use and also provides information and resources to enable planning for spread.
The package is the result of webex and face-to-face learning sessions and workshops (from April 2013 to March 2014) involving people who have day-to-day responsibility for the provision of MSK services and close collaboration with the Allied Health Professional National Musculoskeletal (AHP MSK) service redesign group; the AHP MSK leads group; and colleagues in NHS Special Boards.
The usefulness of this change package has been tested. However, we aim for it to be a live document that incorporates new findings and examples from research and experience as knowledge develops.
Any feedback is very welcome. Please contact:
gillian.borthwick@scotland.gsi.gov.uk
senga.cree@lanarkshire.scot.nhs.uk
How do we use the change package?
- Familiarise yourself with the change package, sustainability guidance, resources and experiential learning from other Boards
- Form a multidisciplinary project team with enough autonomy to implement change: ensure public and senior management buy-in
- Assess readiness and understand current state: apply the principles of improvement methodologies (e.g. DCAQ, process map)
- Identify changes you will make: consider the factors that first need to be addressed to help build sustainable change
- Implement your changes: apply the principles of improvement methodologies (e.g. PDSA cycles)
- Maintain your improvement: evaluate, sustain, modify (as required) and spread
Spread and sustainability
The concept of Getting patients on the right pathway through transforming Community Allied Health Professional MSK services has moved beyond the innovation phase. Prototype services and systems have been tested in a range of Boards, and sites and some spread has taken place. This has enabled us to amass evidence and information about creating the right conditions including leadership for change, intended and unintended consequences, costs and benefits and factors affecting reliability. This change package will guide teams through the decision to adopt and implementation phases. Sustainability although depicted as the final stage of the framework below should be planned for from the very early stages.
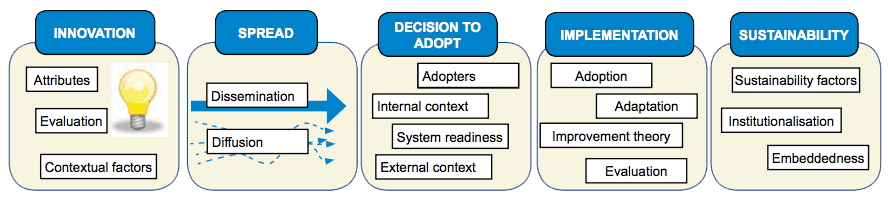
(Health Improvement Scotland Spread and Sustainability Framework)
Allied Health Professionals Musculoskeletal Pathway Redesign - Drivers
| What drivers will support achieving the aim? |
Suggested local measures of success |
| Patient Access Model |
Getting patients on the right pathway:
- NHS Inform used consistently by all points of contact with patients as a self-management platform
- GP decision support tool - pointing patients to self-management and telephone triage as appropriate
- Introduce the national self-referral model through a single point of access
- Implement MSK telephone triage model
|
- % webpage hits, app downloads
- % referral - self, telephone triage (non-clinical, clinical), orthopaedic into AHP MSK services
- Patient views of service
|
| Efficient AHP IT and Referral Management |
- Boards have centralised AHP MSK administration processes - with focus on efficient capacity utilisation
- Efficient referral management - electronic referrals, clinic booking, diaries and patient tracking
- Efficient booking and optimal utilisation - patient opt in and patient reminder systems
|
- MSK hub implemented
- % referrals and tracking process fully electronic
- Capacity utilisation - slot fill %
- % NP and RP DNA rate
- Patient opt in and Patient Reminder System
|
| Sustainable AHP-led Clinical Pathways |
- Implementation of the Clinical AHP MSK Standards Framework
- Embed, evidence-based, person-centred pathways - from self-referral or GP through AHP services to orthopaedic surgical opinion when required
- Timely assessment and getting patients onto the right pathway
- Utilise patient reported outcome measures
|
Embedded clinical pathways for all body parts
Total demand and pathway flows by body part:
- % patients self-managing after non-clinical triage
- % patients discharged after clinical telephone triage
- % patients seen in general AHP MSK services
- % patients seen by ESP AHP staff
- % patients seen by orthopaedic consultancy
- Source of referrals into orthopaedics - % from AHP and GPs etc.
- % patients waiting under 4 weeks
|
Allied Health Professionals Musculoskeletal Pathway Redesign - Drivers (continued)
| What drivers will support achieving the aim? |
Suggested local measures of success |
| Efficient Exit Route Solutions |
Service links and partnerships into associated services to ensure ease of flow from a patient perspective. To include:
- Mental health
- Rheumatology
- Leasure services
- Chronic pain
- Employability
|
- Number and % patients referred to exit routes listed
|
| Low Back MRI Protocol |
Consistent use of national protocol for appropriate referral for low back MRI |
- MRI referral rates per population
- % reduction low back MRI
|
| Accurate Data and Reporting |
Implementation of 'MSK Data Set Standards' through ISD data warehouse |
- All Boards by December 2014
|
| Change Concept |
Change Package |
Essential Resources |
| Getting patients on the right pathway through transforming Community Allied Health Professional (AHP) MSK services. Outcome and Measures: (National Transforming Outpatient Services programme measures) Increasing trend in direct access to appropriate MSK clinician in the most appropriate setting Reduce traditional consultant led 'NEW' outpatient clinic appointments by 5% by 2016 Rationale:
- 10% to 40% of new orthopaedic referrals don't need surgical opinion and of patients on a waiting list, between 5% and 15% do not want/need surgery, hence it is important that General Practitioners (GPs), orthopaedic services and AHP services work in unison to ensure that referrals are appropriately reviewed to ascertain which patients require acute hospital referral and those patients who could benefit from rapid access to more locally based community services.
- People with MSK problems across Scotland will have easy access to a self-management resource and early appropriate advice and if necessary, assessment by an efficient AHP service to get them started on the right pathway for their treatment first time.
- Patient Focus - 'If I have a muscle or joint problem that is interfering with my life or my work I want to
be able to access information about how I can help myself. If I need any assessment or intervention,
I want this to happen in a timely manner and be
by the most appropriate person.'
|
Programme Infrastructure Communication, Engagement and Leadership
- Form multidisciplinary AHP MSK pathway implementation project team
- Engage specialty teams
- Ensure IT support/engagement - (patient information systems and electronic data transfer)
- Engage senior management colleagues
- Engage public and local communities
- Identify and engage a group of champion GPs to support ongoing development and dissemination of information
- Develop communication plan (include stakeholder engagement)
- Identify and agree key benefits and messages (patient experience, quality, clinic utilisation, waiting times, financial etc.)
- Scope and review current best practice, evidence base
- Implementation of publicity campaign (pre and post-implementation of re-designed service)
- Review/assess patient and service user views on re-designed MSK pathway
- Develop spread strategy and plan
- Engage with and provide local leadership support via the National MSK Programme Board, AHP MSK Leads Group and the National Transforming Outpatient Services Delivery Group
- Encourage and practice systems thinking and collaboration across boundaries
- Plan and deliver education interventions prior to implementation to support the dissemination of the AHP MSK pathways to primary, community and secondary care clinicians
- Development and delivery of staff training package to support smooth implementation of redesigned administrative systems and processes
- Identify and agree evaluation process and core Data set to enable ongoing and timeous evaluation (include: patient outcomes, clinical satisfaction, patient and service user views on MSK pathways and MSK minimum data standards)
|
|
| Evidence:
|
Assess readiness, capture, communicate and enable the appropriate response to current state resource status and anticipated resource implications/requirements following AHP MSK Pathway implementation
- Undertake DCAQ to understand the demand and capacity along entire MSK pathways (AHP and Orthopaedic)
- Undertake DCAQ for anticipated MSK referrals directly to AHP services and to understand resulting impact on Orthopaedic services
- Identify skill mix requirements for the delivery of all the components of the redesigned MSK pathway
- Multidisciplinary redesign of traditional pathways of work (linking as appropriate with nationally developed models) to create AHP capacity (self-management, telephone triage) and minimise unnecessary duplication and utilising third sector and leisure services
- Release and create sufficient AHP capacity to deliver redesigned AHP MSK services (new and return)
- Ensure appropriate resource transfer to enable the delivery of high quality AHP MSK pathway services
- Necessary appropriate clinic capacity templated and available for booking (new and return)
- Resources in place (staff, facilities etc.). Appropriate resource transfer to support increased community demand and activity
- Develop and implement robust processes for management of waiting lists (new and return)
- Training, education and support for AHP to ensure skills for service provision
- Training, education and support referring clinicians (intra/inter Board) as appropriate
- Implement and sustain Allied Health Professional MSK 4 week target
|
|
| |
HIGH IMPACT AREAS
Patient access model
- Provide patient information in primary, community and acute settings about the local referral process, what to expect (include information to the patient about his/her rights and responsibilities)
- Develop and provide condition appropriate evidence- based information to clients
- Develop reliable mechanism to direct patients towards self-management resources via NHS Inform
- Ensure NHS Inform used consistently by all points of contact with patients as a self-management platform
- Introduce the national self-referral model through a single point of access
- Develop/utilise integrated web management platform to support personal responsibility
- Ensure accessibility to and enable use of GP Decision Support Tool - pointing patients to self-management and telephone triage as appropriate
- Ensure reliable electronic communication mechanism/ a process in place to allow direct communication between the AHP and GPs
- Implement MSK telephone triage models - consider non clinician call handler protocol driven triage and clinician triage models
|
|
| |
Efficient Referral Management
Information systems and processes
- Ensure reliable electronic mechanisms/functionality in place to ensure that referrals for direct access to community AHP MSK services are sent direct to the relevant departments
- IT systems to support referral directly from self-referral and primary care to AHP services (Referral Management System)
- Electronic referral management as standard (electronic referral, diaries, patient tracking)
- Robust mechanism in place to ensure equitable and reliable access and data transfer for inter-disciplinary and inter-Board referrals
- Boards have centralised AHP MSK administration processes - with focus on waiting list management and efficient capacity utilisation
- Ensure mechanism in place to ensure effective electronic vetting of referrals
- Efficient Booking processes and optimal utilisation - Patient opt in and Patient Reminder Systems (PRS)
- Identify and implement a process to ensure that direct listing of patients when their condition is deemed to be clinically appropriate
- Ensure information systems appropriately track and record patient journey times from referral to first contact, with particular reference to MSK data standards
- Consider provision of electronic 'Advice only'/'Clinical Dialogue' referrals back to referring clinician
- A system and functionality should be in place to return treatment and outcome reports back to the relevant referrer
|
|
| |
Implementation of sustainable AHP-led Clinical pathways:
Enable and ensure reliable implementation of Musculoskeletal (MSK) Pathway Framework - (National Minimum Standard)
Pre-referral considerations:
- Standard A: Screen for Serious Pathology Indicators (Red Flags) Serious pathology indicator/red flags to be agreed and evidence of dissemination to all members of the musculoskeletal team documented
- Standard B: Consistent Advice from All Contact Points Utilising NHS Inform Resources NHS Inform resources to be made available to all members of the musculoskeletal team and evidence of dissemination documented. Service User Information and related resources to be available to all members of the musculoskeletal team on common musculoskeletal conditions
- Standard C: Medication/Analgesia as Appropriate Consistent advice on the use of medications in acute and chronic musculoskeletal conditions to be made available to all members of the musculoskeletal team, including the use of the World Health Organization analgesic ladder
- Standard D: Appropriate Investigations If indicated, appropriate diagnostic tests should be carried out prior to any referral being made
- Standard E: Equal Opportunities to Access Musculoskeletal Pathways via Self or Healthcare Professional Referral AHP services should provide evidence that they are working towards self-referral, where appropriate
|
|
| |
Post-referral considerations:
- Standard F: NHS Board Working to Current National Waiting Time Targets AHP services provide evidence that they are working to National Waiting Time targets
- Standard G: AHP Services Will Provide Timely Clinical Consultation AHP services provide one-to-one clinical consultation within an appropriate timeframe which may not necessarily be face-to-face
- Standard H: Management Plan Discussed and Agreed as per Pathways NHS Boards to clearly define referral pathways from primary to tertiary care for common musculoskeletal conditions, e.g. low back pain, knees. AHP services to provide evidence of patient-centred goal setting
- Standard I: Clinical Supervision Framework with Case Review Policy AHP services have a clearly defined and documented supervision and case review policy/standard operating procedure with evidence of use
- Standard J: Musculoskeletal (MSK) Service Access to Investigations as Appropriate AHP Advanced Practitioners/Extended Scope Practitioners will have a documented clinical governance infrastructure, competencies and standard operating procedures in place to allow independent requesting of appropriate investigations
- Standard K: Process for Onward Referral from Musculoskeletal (MSK) services to Other Clinical Specialties AHP services have documented process for onward referral, when and where appropriate
|
|
| |
Implementation of sustainable AHP-led Clinical pathways:
- Implement interdisciplinary evidence based, MSK person-centred pathways
- Fully implement, deliver and monitor delivery of minimum standards framework
- Develop reliable mechanisms to ensure availability of relevant pathway information for referrers (including AHP GPs and consultants), including criteria for referral and roles and responsibilities
- Clear, unambiguous and easily accessible referral protocols in place
- Mechanism for AHP to order and review investigations
- Initial telephone assessment and advice where appropriate
Direct access to diagnostics
- Develop and implement agreed multi disciplinary MSK MRI referral protocol(s)
Efficient and Integrated Exit Route Service Solutions:
Boards will develop partnerships and service links to promote straightforward flow from a patient perspective to include:
- Mental health
- Chronic pain
- Rheumatology
- Employability
- Leisure services
|
Examples of NHS Board MSK Clinical pathways:
MRI Investigation protocols:
Mental Health / Chronic Pain:
Working Health services:
NHS Board examples of best practice:
|
| |
Monitor MSK minimum data standards to ensure and enable consistency of quality and access
Measure the quality of the AHP MSK Service by ensuring that appropriate MSK minimum data standards are available, captured electronically and reported nationally for the following purposes.
| What |
Quality Aim |
Measurement |
By Whom |
| MSK Waiting Times |
Timely and Equitable |
Capturing variation in adjusted waiting times per Health Board, profession and body region reported nationally and quarterly |
All MSK Service and ISD |
| MSK Key Performance Indicators - (outcome measures) |
Effective |
No. of returns to work.
EQ5D start and end score variations.
No of reported Onward referrals to leisure facilities. No of patient with no improvement? |
ISD phase 2 of MSK waiting times |
| Demand, Capacity, Activity and Queuing |
Efficiency |
No. of services using DCAQ tool |
Boards should identify leads locally to have responsibility for DCAQ analysis and actions |
| Customer Satisfaction |
Person Centred |
To be confirmed |
To be agreed locally |
| Risk register |
Patient Safety |
IT systems Clinical risk register |
Initially locally with number of reported high risk incidents nationally? |
| Electronic record and Tracking |
Safety and Governance |
risk register |
Initially locally |
|
|
| |
Review demand and capacity management on an ongoing basis
- Assess the effectiveness of population health interventions, self-management and telephone consultation in creating AHP quality and capacity
- Assess the effectiveness referrals to community physiotherapy MSK compared with a provisional orthopaedic specialist appointments without prior physiotherapy
- Identify any increase in GP referral to community physiotherapy and compare against the total workload to Orthopaedic services across MSK pathways
- Review the impact on outpatient services, i.e. requests for new outpatient (Quality and governance measures to be known and applied)
- Ongoing evaluation to be undertaken between AHP/ GP/ESP services and Orthopaedic services to ensure appropriate referrals are made to permit optimisation of the service: monitor referral trends for both direct access and consultant-led referral clinics and also monitor variation patterns between Clinicians. This will highlight the aspects that will require to be addressed by units providing this service
- Patient experience feedback will be collected on an ongoing basis
|
|
| |
Ongoing communication and review
- Ongoing engagement between community, primary and secondary care MSK services
- Ongoing review of patient outcomes
- Ongoing review of clinical satisfaction
- Implement post-implementation publicity campaign
- Review/assess patient and service user views on MSK pathways
- Share learning with other teams and Boards
|
Local media (press & radio)
Signs/posters/leaflets/stickers
GP surgeries
Patient letters
NHS Community Post-implementation publicity suggestions:
- Number of appointment opportunities that have been created for patients and the equivalent cost, or cost of missed appointments
- Examples of health benefits for patients of being treated on time
- The responsibilities of the patient in achieving all of the above
|
