Practising Realistic Medicine: summary
This document gives a brief summary of the Chief Medical Officer's third annual report, Practising Realistic Medicine.
Summary
In this web summary of Practising Realistic Medicine, we bring out some of the key points from the main report. To read the full report please go to http://www.gov.scot/ISBN/9781788514279. Practising Realistic Medicine will help to embed Realistic Medicine and allow the spread of good practice which we have seen throughout Scotland. Realistic Medicine supports all healthcare professionals to be empowered to practise in a collaborative way with those they care for.
Building Our Personalised Approach To Care With People Across Scotland
We have considered the results from the Our Voice Citizens’ Panel to further understand public opinion on shared decision making. The results show that while 92% of people said they would feel comfortable asking their doctor about their treatment and care options, only 67% had actually spoken to their doctor about them. When asked to expand on their answers, a number of people commented that the attitude of their doctor had an impact on their inclination to ask questions. This would suggest that taking the time to listen and have a truly shared conversation is invaluable. We will explore further how we can improve shared decision making by conducting a Citizens’ Jury on this topic later in 2018.
Changing Our Style To Shared Decision Making
Effective communication skills lead to improved patient safety, symptom resolution and improvements in functional and psychological status. People often want to be more involved in decisions about their care but they may not know what questions to ask. Question prompt sheets can be helpful in this context. Choosing Wisely UK devised 5 Questions to help prompt better conversations between clinicians and patients. These questions are being used in some NHS Boards already and we plan to evaluate how effective they are. We will also distribute the 5 Questions in the form of flashcards via our Realistic Medicine Leads (Figure 1).
Changing the way we practise will take conviction from clinicians as well as skills to facilitate the change. The MAGIC programme, supported by the Health Foundation, demonstrated that “skills trump tools and attitudes trump skills.”
We should also ensure that we share decisions about how we best deliver services and work creatively to improve the way we provide care. This is at the heart of health literacy and of the new action plan Making it Easier, a health literacy action plan for Scotland for 2017-2025.
Figure 1: Asking the Right Questions Matters

Understanding And Managing Medico-Legal Risk
Clinicians often worry about the risks of being criticised if they do not offer every possible treatment. Realistic Medicine is not about failing to offer treatments. It’s about ensuring decisions are made in partnership with people, helping them to make the choices about their treatment and care that are best for them as individuals. The Scottish Public Services Ombudsman report found that inadequate consent was the most common recurring issue in complaints and has provided guidance on how obtaining consent can be improved. The General Medical Council is currently reviewing their consent guidance following the UK Supreme Court Ruling Montgomery v Lanarkshire Health Board in 2015. This ruling puts the patient ‘in the driving seat’ and encourages people to explore risk as it is relevant to them, rather than how their healthcare professional’s view the risks. This, of course, is what Realistic Medicine is all about.
Valuing Our Workforce
Our workforce is undoubtedly the most valuable asset we have in health and social care. It is important to re-emphasise this and to be clear that we value the contribution and the commitment of all health and social care staff and the challenging work they do every day. Given what we have learnt from investigations such as the Francis Report we know that an engaged workforce is vital to ensure patient safety. NHSScotland is making efforts to improve the experience of those working in the NHS using iMatter. Integral to the model is the ability of individuals and teams to shape the action which is taken in response to the feedback.
These are challenging times for all staff and we need to work on ways to help improve their experience. Changes have already been made in Scotland to try to improve the working conditions of doctors in training: for example, by abolishing doctors in training working for more than seven days or shifts in a row in any working pattern, and by developing the Professional Compliance Analysis Tool ( PCAT), a supportive improvement tool to promote safe and healthy working patterns.
Working in Scotland’s NHS can be extremely rewarding if the environment and leadership is good; it is vital that we ensure that all staff are empowered and invested in remaining within our NHS workforce, as well as encouraging others to join it and removing behaviours which have a negative effect. We are funding the development of leaders who will continue to support the practice of Realistic Medicine across Scotland.
Tackling Unwarranted Variation, Harm And Waste To Provide Value Based Healthcare
Tackling unwarranted variation is essential to improving the health gain and outcomes derived from healthcare across Scotland. The first step to achieving this is discovering where variation exists, understanding the basis for this variation and facilitating discussions to address this variation when it is wasteful or harmful. In order to achieve this we need to make data more accessible and understandable. In 2018, we will publish a publicly accessible Atlas of Healthcare Variation and launch a training and improvement programme with the goal of achieving high quality Value Based Healthcare in Scotland.
Realising Knowledge For A Realistic Era
Using relevant scientific evidence alongside clinical judgement and our patients’ preferences and values will facilitate realistic evidence based practice. Stewart Mercer stated “Achieving the aims of Realistic Medicine will require robust evidence not only on what works, but also for whom does it work, under what circumstances, and what interventions can be implemented and scaled up.” We will introduce researchers within the Realistic Medicine policy team to lead a programme of work examining the clinical, social and economic impact of Realistic Medicine as it progresses and developing further evidence to inform future approaches.
It is important that information about managing our health is available in a user-friendly way for anyone who wishes to access it. Library and Information Services across the NHS, local authorities, health and care practitioners and the voluntary sector have a key role to play in making this information more accessible to the public; this could include ensuring that staff are aware of health literacy, or supporting people to self-manage their conditions through the use of library and information services.
A Realistic Approach To Population Health
Health is more than just an absence of illness: it’s a resource that enables us to live lives we have reason to value. To realise this for the Scottish population, we need to think broadly about the factors that shape our health. Health inequalities are an element of unwarranted variation which have a variety of contributing factors (Figure 2).
It is accepted that traditional health and care services alone cannot tackle all the factors that influence good population health; complex causal factors require complex interventions. There are many inspiring stories of communities acting together to tackle some of these issues. In a project in two GP surgeries in Parkhead Glasgow, welfare rights advisors worked in clinical settings and were able to provide advice and support on benefits, debt, housing, pension and employment issues. They delivered £850,000 worth of unclaimed benefit entitlement to 165 people and helped identify and manage £156,000 worth of debt.
Figure 2: Social determinants of health

Health Of The Nation
Good quality data is a key factor in delivering appropriate services and instigating public health measures to improve the health of the Scottish population. The Scottish Burden of Disease project has produced new estimates for the overall burden of disease in Scotland that combine figures on deaths with estimates of the numbers of people living with illness.
Have a look at Section 2 of the annual report to see a snapshot of the topics covered in our overview of the Health of the Nation - from rates of mortality, diabetes and drug-related deaths to dramatic improvements in children’s oral health and the impact of the HPV vaccine in reducing inequalities in cervical cancer rates.
Asking the Right Questions Matters
To help ensure you have all the information you need to make the right decisions about your care, please ask your doctor or nurse:
Is this test, treatment or procedure really needed?
What are the potential benefits and risks?
What are the possible side effects?
Are there simpler, safer or alternative treatment options?
What would happen if I did nothing?
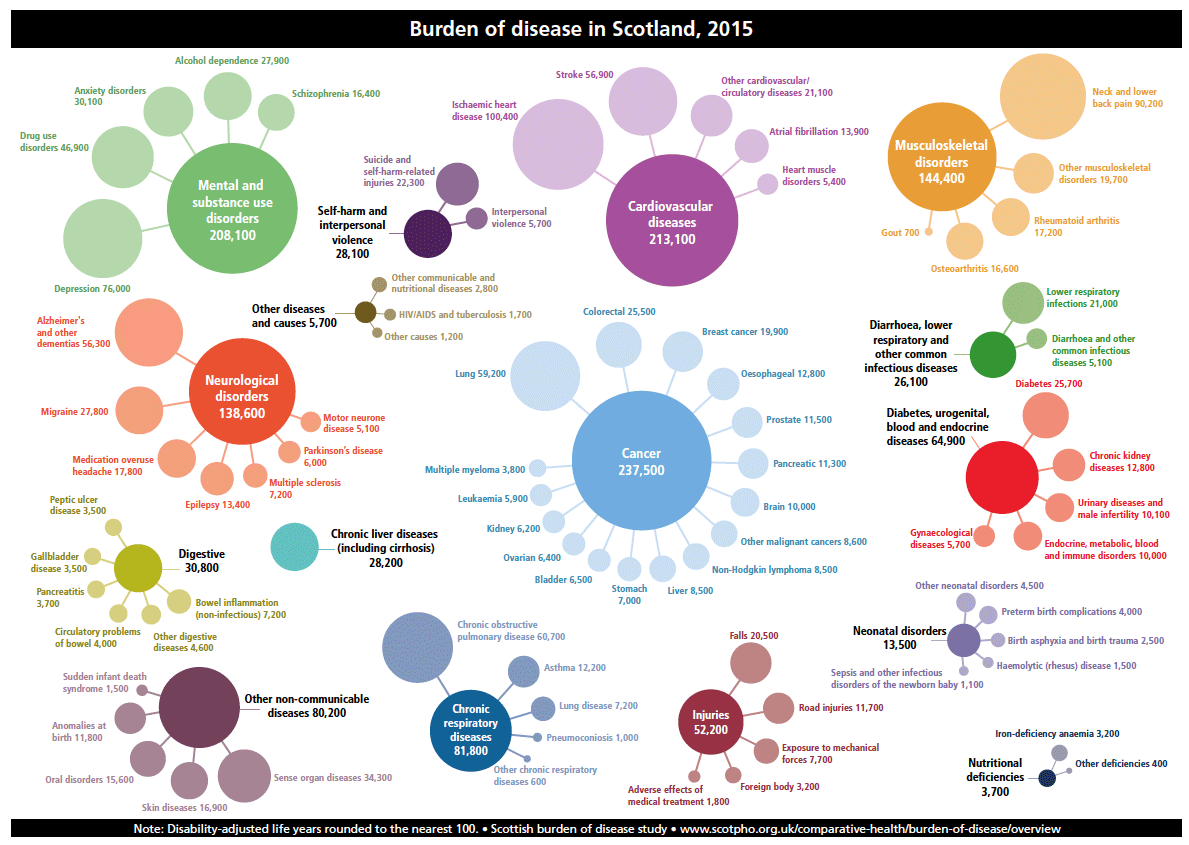
Figure 3: This infographic from the Scottish Burden of Disease study illustrates what conditions we are living with, and dying from, in Scotland. The size of each “bubble” is proportionate to the rate of death and disability caused by that condition. You can view the image in more detail at: http://www.scotpho.org.uk/media/1450/sbod2015-bubbles.pdf