Perinatal and Infant Mental Health Programme Board 2020-2021: delivery plan
Perinatal and Infant Mental Health Programme Board's Delivery Plan for 2020 to 2021.
Introduction
from Chair of Perinatal and Infant Mental Health (PNIMH) Programme Board
As Chair of the PNIMH programme board, I am delighted to present the delivery plans for perinatal mental health and infant mental health for 2020-21. In this introduction I want to briefly summarise progress and highlight successes; outline the rationale behind two delivery plans, and pay attention to the current context in which we are operating.
In March 2019, the Perinatal and Infant Mental Health Programme Board was launched by the First Minister to oversee, provide strategic leadership and have overall management of the delivery of improved perinatal and infant mental health services. This includes establishing improved provision at national, regional and local level in line with the recommendations in the Perinatal and Infant Mental Health Managed Clinical Network 'Delivering Effective Services' report published in March 2019. The Programme Board is a strategic delivery board reporting directly to the Minister for Mental Health, via the Mental Health Delivery Board and links closely to the Delivery Board for the Best Start maternity programme and the Children and Young People's Mental Health Programme Board. This commitment is supported by £50 million of investment in perinatal and infant mental health services over the next 4 years. The Board met six times in 2019-20.
One of the most important developments in 2019 was the expansion of the remit of the PNIMH programme board to include the planning and development of all Infant Mental Health (IMH) services (pre-conception to 3 years) to meet the wider needs of families experiencing significant adversity, including infant developmental difficulties, parental substance misuse, domestic abuse and trauma (Programme for Government 2019-20). The Infant Mental Health Implementation and Advisory Group was convened by Dr Anne McFadyen to provide clinical advice and support to inform the development of mental health care for infants from conception to 3 years of age, and oversee the testing and implementation of evidence-based and innovative models for the delivery of these infant mental health services. Its role is to advise and make recommendations to the Programme Board, as services develop, about best use of wider investment and best practice models. The group have developed a first delivery plan for 2020-21 presented in this document.
This broader policy responsibility moved the focus for the Programme Board from IMH only where it interfaced with perinatal issues and services, to a broader remit and scope for all IMH and the IMH delivery plan reflects this. So whilst the perinatal delivery plan still includes some aspects of IMH where they relate to perinatal care, the IMH delivery plan stands on its own. However, we are thoughtful to ensure that these are not seen as two entirely separate plans, hence they are presented together here.
Where we are now: the 1st PNIMH Programme Board Delivery Plan 2019-20
The PNIMH delivery plan for 2019/20 https://www.gov.scot/publications/perinatal-infant-mental-health-programme-boad-delivery-plan-2019-20/ set out plans to sustain and develop perinatal and infant mental health services.
The delivery plan focused on 3 key areas for perinatal and infant mental health: More Capacity, More Staff, and More Voices. Developing infant mental health networks and services was a fourth central component of the 2019-20 plan. Our initial aims were to support:
- the voice of women with lived experience to influence and improve services
- access to third sector support services
- the strengthening the workforce
- access to and the expert role of Mother and Baby Unit (MBUs)
- enhancing specialist community provision particularly in the North of Scotland
- establishing infant mental health services
- a range of educational initiatives for the whole workforce and training more specialist staff.
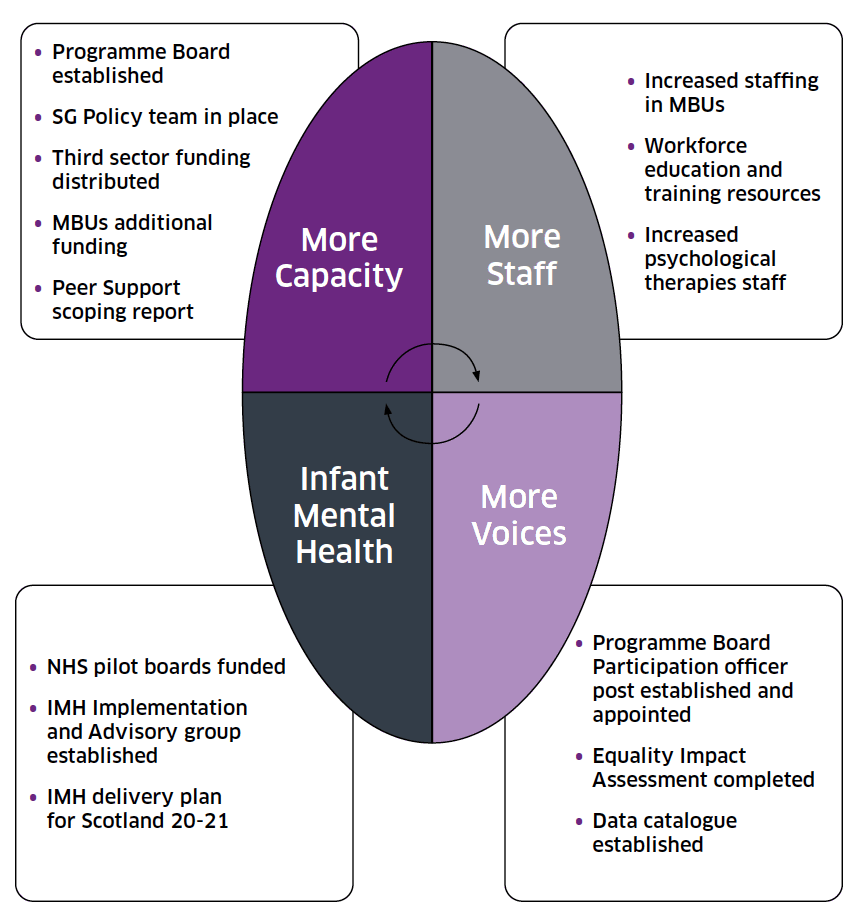
Key actions delivered in 2019-20
- £1 million of funding was made available in the financial year (2019/2020) to support the initial delivery plan and lay the foundations to develop future services.
- The funding distributed in 2019/2020 included:
- £225,000 to support existing third sector counselling and befriending services as well as develop new services to support those 11,000 women who might benefit from additional support in their community.
- Over £80,000 to develop a model for Community Services in the North of Scotland. This will inform the development of a model that can be adapted and rolled out across Scotland in subsequent financial years.
- £150,000 to increase specialist staffing levels at the two Mother and Baby Units (MBUs). This will provide capacity for the units to further develop as Centres of Expertise and improve national pathways into care and discharge planning for women who require inpatient care.
- Over £80,000 to develop a model and pilot of 2 areas on infant mental health provision to meet the wider need across families experiencing significant adversity.
- Funding to Maternal Mental Health Scotland to ensure that the views of people with lived experience are listened to and influence the decisions of the Programme Board, Health Boards and Integrated Joint Boards.
- Over £160,000 to NES to fund additional psychology trainee places and perinatal workforce training
- Over £100,000 to NSS to provide programme management for the Programme Board
- The Programme Board established a dedicated group on infant mental health to identify the key actions to take to develop an integrated infant mental health service across Scotland.
- Lived experience will be core to developing services that are fit for purpose and suit local context. The Programme Board has supported recruitment of a Participation Officer. Their main role is to engage with women and families who have used services, or have felt they would have benefitted from more support with their mental health around pregnancy and as a new parent, to gather evidence to support service development.
Finally, turning to the current context of June 2020 and Covid-19. At the start of the pandemic, the Programme Board, MCN and Scottish Government met and decided that wherever possible delivering on the 2019-20 action plan would continue. It is testament to everyone's commitment that a number of the actions have been successfully progressed or completed. The response to Covid-19 also led to some innovative developments. In the area of PNIMH which we aim to capitalise on in 2020-21. These included the Covid-19 Rapid Response Hub that produced high quality evidence based information and guidance around PNIMH and the implications of Covid-19; the priority rollout of the 'Near Me' on line patient consultation platform in partnership with Healthcare Improvement Scotland; and making available the online Solihull training resource free via the Parent Club website. Whilst the responses to Covid-19 are changing rapidly, I continue to be aware that all health and social care providers remain rightly focused on responding to Covid-19 and remobilising services, and developing new services may not be high on the agenda or feasible at the moment. This delivery plan and associated timescales will be sensitive to the priorities of the evolving context and the continuing need to respond to Covid-19 and will be subject to regular review and consultation.
As we emerge from this time, all the evidence suggests that a renewed focus on perinatal and infant mental health will be even more important. The recent reports of the impact of the pandemic on mental health in general and the predicted consequences of isolation on families that we are beginning to see, including domestic violence and child protection issues, are of real concern. That is why this should be seen as an opportunity to develop and invest in line with the clear evidence base showing the economic, social and population health benefits of a prevention approach. This is the opportunity to build on the impetus from the 2019 delivery plan and make long term sustainable changes.
Hugh Masters
Chair of PNIMH Programme Board
June 2020
Contact
Email: PIMH@gov.scot