Financial planning for large hospital services and hosted services: guidance
Guidance on the financial aspects of delegated services provided in 'large hospitals' and the treatment of hosted services included in delegated functions.
Guidance on Financial Planning for Large Hospital Services and Hosted Services
1. Context
Integration of health and social care requires the new health and social care partnerships - Integration Authorities - to deliver the national outcomes for health and wellbeing via their strategic plans, which must incorporate the needs and priorities of their localities.
Integration authorities will be responsible for strategic planning, in partnership with the hospital sector, of those hospital services most commonly associated with the emergency care pathway, alongside primary and community health care and social care.
The objective is to create a coherent single cross-sector system for local joint strategic commissioning of health and social care services and a single process through which a shift in the balance of care can be achieved. The strategic commissioning process will involve a co-production approach through meaningful engagement with a range of stakeholders, including those who use and provide services. Integration Authorities will be required to establish a strategic planning group to prepare the strategic plan. This group will include representation of these key stakeholders.
Fundamental to this endeavour is a clear understanding of how "large hospital" services are being consumed and how that pattern of consumption and demand can be changed by whole system redesign. There are some similarities between large hospital and hosted services and the latter are also included within the scope of this guidance. As a first step it is critical that there is transparency for Partnerships and localities on how resources are being used. As a second step, there needs to be clarity about the financial impact of changes agreed through the strategic planning process.
It is recognised that this is a complex journey and the guidance is intended to provide a financial framework within which a start can be made.
2. Introduction and purpose
This guidance has been produced jointly by the Integrated Resources Advisory group and the Joint Commissioning Steering Group; it supplements sections B4.4 and C4.4 in the existing IRAG guidance (http://www.gov.scot/Topics/Health/Policy/Adult-Health-SocialCare-Integration/About-the-Bill/Working-Groups/IRAG/Guidance) and will in due course be incorporated into revised statutory financial guidance.
The purpose of the guidance is to provide advice on:
- Implementing the requirements of the Act and regulations in respect of the amounts to be set aside for those delegated services provided in "large hospitals" (see annex A for definition); and
- The treatment of hosted services included in delegated functions.
Annex A sets out the requirements of the Act and the draft regulations for the amounts to be set aside by Health Boards, for use by Integration Authorities, for services provided in "large hospitals".
3. Scope of the Guidance
The guidance covers:
a) A method for establishing the amount to be set aside for the services that are delivered in a "large hospital", as defined in the Act - i.e. showing consumption by partnership residents;
b) A method for quantifying and reporting performance for the financial consequences of planned changes in capacity as they relate to "set aside" budgets for large hospitals, which may be:
(i) steady state i.e. the strategic plan results in no changes to consumption of services in scope / is designed to avoid increases in consumption
(ii) increased consumption
(iii) decreased consumption
4. Principles and Assumptions
The guidance is based on the following:
1) The initial focus for strategic planning for hospital services will be those services associated with unplanned care set out in the regulations.
2) The resources within scope of the strategic plan will comprise:
- The totality of the budget covering health and social care pathways and services for emergency care / discharge pathways outwith the hospital setting; and
- The sum "set aside".
3) Changes will be agreed through the strategic planning process. Resource flows will only follow actual implementation of planned changes and there should be a formal framework of accountability underpinning this.
4) The Health Board hospital sector will be a key stakeholder in the development of the strategic plan.
5) Where more than one partnership exists within a Health Board area, the change programme for hospital services will have to be coherent across individual strategic plans (under S30 (3) of the Act). Consequently, there should be an overarching strategic plan for the hospital services delegated to Integration Authorities that is a consolidation of the individual partnership plans and this should be coordinated and held by the Health Board hospital sector.
6) The strategic plans produced by the Integration Authority/ies must in turn be consistent with the strategic context set by the Health Board and Local Authority. The hospital capacity and hosted services included in the strategic plan should evolve from the existing capacity and plans for those services.
7) Strategic plans will reflect locality planning in due course.
8) Hosted services are similar to hospital services i.e. the provision of a common service is managed on behalf of all partnerships, but strategic planning for the use of the service is by each partnership for their respective populations.
5. Scoping Consumption of Hospital Services: Establishing the set aside Budget
It is recommended that the consumption of hospital services by partnership populations should be determined by analysis of hospital activity and cost information.
Activity
Hospital activity is recorded on Health Board hospital patient administration systems (PAS) which are based on the individual record of each inpatient hospital episode. These can be used to analyse hospital activity by type of admission, specialty, procedure, length of stay, diagnosis etc. This data, aggregated to locality and partnership level, should be used to identify the hospital activity and capacity used by patients for each partnership:
The data can be obtained from either:
- Local Health Board information teams; or
- National Services Scotland (NSS), which produce these datasets for each partnership through the Health and Social Care Data Integration& Intelligence Project (HSCDIIP); see annex B for an overview of this work and the fields available in the datasets.
It is recommended that an average of three years of activity is used to scope partnership consumption for the first year of the strategic plan.
Cost
Attaching a £ value to activity can be achieved in a number of ways, for example:
- Blue book admission or bed day rates;
- Local Costing methodologies;
- NSS patient level costing (PLICS) available through HSCDIIP.
It is a local decision as to which method is used, however it is recommended that a consistent method is used for all partnerships in a Health Board area.
It is recommended that this approach should also be used for hosted services that are provided in hospital.
For those hosted services that are not provided in hospital, other information will be required to scope consumption. Patient level community activity datasets will allow consumption of these services to be estimated in a similar way to hospital services and in due course the HSCDIIP project will incorporate community activity datasets for all partnerships. Until that time, it is recommended that partnerships use patient level community activity data where it is available locally; where it is not available, it is recommended that partnerships use budget information from financial systems and other local information for apportioning community hosted services to partnerships for consumption purposes. It is also recommended that partnerships adopt a method proportionate to the likelihood of the hosted service being subject to re-design or where changes in demand for service are likely to vary across partnerships, in the near term.
Partnerships may wish to consider extending the consumption analysis to include other non-delegated functions as shown in figure 1, which would allow full transparency of the use of all health and social care resources by partnership populations; this is a local decision.
Figure 1: Consumption of Health and Social Care resources
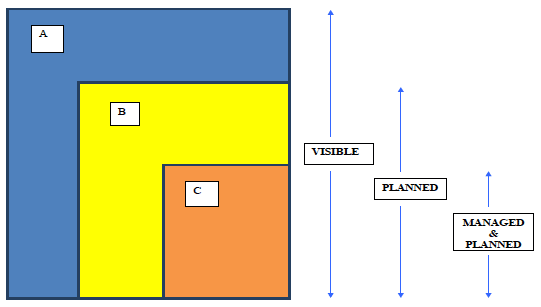
A = Non delegated health & social care resource used by the Integration Authority population. Visible to the Integration Authority but not in scope of the Strategic Plan. (Elements from A may be included in B in future).
B = Hospital resource used by the Integration Authority population for delegated "large hospital" hospital services. Within scope of the Strategic Plan with operational management by Health Board. (Elements may switch between B&C as set out in the Strategic Plan).
C= Delegated Community Health and Social Care Resource, including community hospitals. Within scope of the Strategic Plan with operational management by the Chief Officer
Fair share consumption
Under the approach recommended above, the initial consumption included in the first strategic plan will be based on historical resource consumption. In due course, decisions made by partners about the capacity required by their populations taking account of demographic change and service redesign are likely to result in the consumption included in the strategic plan moving away from that based on past performance.
Using historical consumption as a starting point inevitably builds in any existing inequity of resource use in the historic position i.e. partnerships that historically use more than their fair share of hospital capacity will have this resource consolidated into the resource in scope of their strategic plan. It is difficult to avoid this without causing immediate destabilisation. The policy is not intended to deliver total change on day one, rather it is to establish a process of transformation over the longer term starting from a good foundation. Over time, issues of equity can be considered by Health Boards and may be addressed through their subsequent allocations to partnerships.
It is recommended that partnerships use fair share information based on the National Resource Allocation Committee (NRAC) methodology available from NSS (through the HSCDIIP project) for benchmarking partnership expenditure.
6. Financial consequences of planned changes in capacity
Strategic Planning will be a cyclical process of Analyse, Plan, Do and Review and this will likely involve a two stage process for developing cases for change: from considering initial proposals to full inclusion in locality and strategic plans. This will require cost and activity information at different levels of detail, depending on whether consideration is of an outline case or a full case proposal.
Outline Cases
Chief Officers, GPs, other clinicians, strategic planning groups and other stakeholders will require a practical and easily used method to model the potential implications for the set aside resource that may follow from change, whether redesign proposals or from underlying demographic pressures. This method would allow stakeholders to produce outline cases for initial consideration that could subsequently be subject to more detailed assessment and estimates as required.
It is recommended that bed day rates are used to provide information for outline cases; it is also recommended that they are adjusted to account for cost behaviour, as costs do not vary proportionately with activity and instead tend to be either variable, stepped or fixed in nature. This can be achieved by adjusting the bed days rates to:
- Exclude indirect overheads from the bed day rates; and
- Provide a range of bed day rates to apply over a corresponding range of changes in activity-from marginal cost savings for small changes to more material savings in stepped costs for larger scale effects.
This data is available from a number of sources:
- Blue book bed day rates;
- Local Costing methodologies;
- NSS PLICS data.
The choice of which method to use is a local decision but it is recommended that a consistent method be used for all partnerships in a Health Board area.
Full Case proposals
More detailed estimates of the effect of change proposals, where indicated by positive outline cases and for the effect of underlying demographic change, will be required.
It is recommended that these are developed for each by a group comprising the hospital sector director (or similar postholder) and the Chief Officers of the Integration Authorities whose populations use the hospital services (including those with a material level of cross boundary flow). A financial plan should be developed and agreed that sets out the capacity and resource levels required for the set aside budget for each Integration Authority and for the hospital sector, for each year. This should be based on an agreed implementation plan with assumptions for:
- Activity changes based on demographic change;
- Agreed activity changes from new interventions;
- Cost behaviour;
- Hospital efficiency and productivity targets;
- An agreed schedule for timing of resource released/additional resource.
It is recommended that the approach to producing detailed financial plans based on the agreed changes should be similar to those previously used for Learning Difficulty Same As You (SAY) and other major redesign exercises.
Where there is a planned increase in consumption, the Integration Authority will need to consider how to fund the additional capacity through the Strategic Plan. Similarly, where resource is released, the Integration Authority will be able to consider how to use this resource through the Strategic Plan.
7. Reporting Performance Against Plan
Partnerships and the hospital sector will require information on their performance against the plan for hospital capacity in order to flex the strategic plan and also to take remedial action in year if necessary. This will need to be available at two levels: for each partnership; and for the overarching hospital plan.
It is recommended that the group comprising the Chief Officers and Health Board hospital sector director receive regular activity reports comparing the expected capacity set out in the strategic plan, for each integration authority, with actual capacity used.
Actual activity and expected activity will be available from NSS HSCDIIP reports or alternatively from local Health Board information teams.
8. Accountability Framework
It is recommended that there is a clear understanding of where the balance of risk lies, between each Integration Authority and the Health Board hospital sector, for delivering the strategic plan for hospital capacity. There are two main risks:
- Activity and case mix: i.e. the agreed capacity set out in the plan is not delivered or not delivered on the agreed schedule; and
- Resources: i.e. the capacity set out in the plan is delivered, but the resource required is different to that agreed.
Ultimately these risks are shared between the Integration Authorities and the Health Board hospital sector (or host organisation in the case of hosted services); however, it is recommended that the primary responsibility for delivering capacity (i.e. activity and case mix) should lie with each Integration Authority; and that for providing the capacity within agreed resources should lie with the Health Board hospital sector.
It is recommended that the process for making adjustments to the set aside resource to reflect variances in performance against the plan are agreed and clearly set out. This should explicitly deal with cases of offsetting variances between Integration Authorities. It is also recommended that in-year resource adjustments should be avoided and that changes be made through annual adjustments to the Strategic Plan. If partners consider that in-year resource adjustments should be made, it is recommended that minimum thresholds for activity variances are agreed, below which no resource adjustments will be required.
The basis of the accountability framework should be a local decision.
Contact
Email: hscintegration@gov.scot