Chief Medical Officer's Annual Report 2014-15 Executive Summary
The Exeuctive Summary of the Chief Medical Officer's Annual Report 2014-2015
Chief Medical Officer's Annual Report 2014 - 15 Executive Summary
This is the Executive Summary of the Chief Medical Officer for Scotland’s Annual Report. You can find the full report at www.gov.scot/cmoannualreport201415.
The Added Value of Doctors in a Complex System
Current models of healthcare services are stretched and do not always suit patients, their carers or the aspirations of the workforce. High profile failures in care have emphasised the importance of good clinical leadership which is clearly linked to good patient care. Strong clinical leadership is arguably the single most effective means of preventing similar failings occurring in the future.
Realism in Health Care
Doctors generally choose less treatment for themselves than they provide for their patients.
In striving to provide relief from disability, illness and death, modern medicine may have overreached itself and is now causing hidden harm – or at best providing some care that is of lesser value.
We must deliver healthcare that focuses on true value to the patient. Waste in healthcare should be assessed not in terms of what might be thrown away, but in interventions that don’t add value for patients. This includes avoiding unwarranted variation in clinical practice and resultant outcomes.
Evidence-based guidelines developed for people with single diseases should not necessarily be extrapolated to the management of patients with multiple conditions, given the possibility that this may result in over-treatment and over-complex medication regimes.
We as clinicians have a duty to ensure that we are able to acknowledge our powerlessness at times, and ensure that a difficulty on our part in accepting the inevitable does not adversely affect the patient’s experience of death.

Sharing Decision-making and Informing Consent: People and Professionals Combining their Expertise
“The single biggest problem with communication is the illusion that it has taken place.”
George Bernard Shaw
We need to change the outdated ‘doctor knows best’ culture to one where both parties can combine their expertise and be more comfortable in sharing the power and responsibility of decision making. It requires system and organisational change to promote the required attitudes, roles and skills.
Such system change is articulated in models such as the House of Care, which provides a useful representation of the components, all of which are required, to place collaborative, relational decision making and planning at the heart of our system.
Scotland’s House of Care
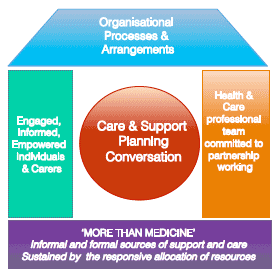
Shared decision making is not a one-way transmission of information about options and risks from the professional to their patient. It is a two-way relational process of helping people to reflect on, and express, their preferences based on their unique circumstances, expectations, beliefs and values. Simple approaches can readily be implemented within consultations to improve communication by avoiding jargon, and checking understanding, using techniques such as Teach Back.
Doctors and the Management of Clinical Risk
Managing risk in healthcare is a universal challenge for doctors and other professionals. Doctors tread a difficult path, with the expectation that they will make robust decisions balanced against criticisms of being overly paternalistic.
There is risk associated with every clinical decision, whether it is to do something, or do nothing. Beyond risk factors identified by statistical analysis there is no substitute for clinical experience. An early sign in burn out of doctors is their reduced ability to tolerate the anxiety of making risky decisions.
Good risk management is also dependent on communication of risk with other services.
Changing our Practice to Support Improvement
Scotland’s medical staff, working with all our colleagues in health and social care, continue to be at the forefront of the wide range of improvements in the safety, effectiveness and quality of care and treatment within our National Health Service.
Improvements in the quality of care are often dependent upon having the right conditions in place – positive relationships with colleagues, a learning culture and an understanding of tried and tested ways of implementing change in complex systems.
We should be focusing completely and relentlessly on what matters most to the people who look to us for care, support and treatment.
From Lucas, B & Nacer, H. (2015). The habits of an improver. Thinking about learning for improvement in health care. London: The Health Foundation. P.8.
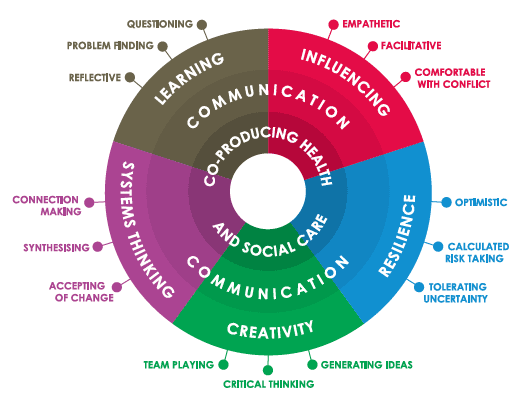
Translation of Medical Research into Routine Clinical Practice
The translation of research findings into clinical practice has transformed healthcare. It is a cornerstone of modern evidence-based medicine and of an advanced healthcare system. However, the route to translation can be challenging: high costs, scarce funds, shortages in key research infrastructure, capacity or capabilities, slow and incomplete recruitment to trials are amongst the potential barriers to the progress of translational research studies. Medical research and development can follow ill-defined and circuitous paths before being taken up into improved patient care.
I’d really welcome your opinion. If you have feedback I can be reached at:
Email: cmo@gov.scot Phone: 0131 244 2379
You can also interact with me on twitter.com/CathCalderwood1
and via my blog blogs.scotland.gov.uk/cmo/ and via at www.linkedin.com/in/catherine-calderwood-691979108.
Or complete my survey www.surveymonkey.co.uk/r/LMDCMWM
Contact
Email: Diane Dempster