The Scottish Health Survey 2011 - volume 2: children
Annual report of the Scottish Health Survey for 2011. Volume focussing on child health.
This document is part of a collection
5 Obesity
Linsay Gray and Alastair H Leyland
SUMMARY
- In 2011, 65.6% of children aged 2-15 had a healthy weight (BMI >5th percentile and <85th percentile), a small decrease from 70.3% in 1998.
- 31.6% of children were overweight or obese in 2011 (BMI >85th percentile), a slight increase since 1998 when the prevalence was 28.0%.
- 15.7% of children were obese (BMI >95th percentile and <98th percentile) or morbidly obese (BMI >98th percentile) in 2011, representing a small rise in prevalence from 13.0% in 1998.
- The trends over time have largely been driven by boys, with little change seen for girls in the 1998-2011 period.
- Boys were significantly less likely than girls to be a healthy weight (65.1% compared with 69.8%) and were more likely to be overweight or obese (32.7% compared with 28.0%) (2008-2011 combined).
- Healthy weight prevalence was significantly associated with age though not in a linear fashion. Prevalence was generally highest in the early years (aged 2-7) and was lowest among boys aged 10-11 (56.6%) and girls aged 12-13 (62.9%).
- Boys aged 10-11 and girls aged 12-13 had the highest prevalence of overweight or obesity (41.9% and 33.4%, respectively).
- There is a strong association between parental BMI and child BMI. Children with parents who are either a healthy weight or underweight are less likely to be overweight or obese than children of obese parents (21.0% compared with 40.1%).
- Boys in the lowest income households were more likely than those in
other household income groups to be obese (19.7% compared with 14.2% in the highest income group). There was no clear pattern by household income for girls. - Area deprivation was significantly associated with obesity. Girls and boys in the most deprived quintile were less likely to be a healthy weight and more likely to be obese than girls and boys in the least deprived areas. Children living in the 15% most deprived areas in Scotland had a significantly higher prevalence of obesity than those living elsewhere (18.7% compared with 14.5%).
5.1 INTRODUCTION
The negative health consequences experienced by overweight and obese children are wide ranging and include an increased risk of hypertension, type 2 diabetes and asthma.[1],[2] Children's mental wellbeing has also been shown to be negatively affected by overweight and obesity. The health risks of an unhealthy weight in childhood continue into adulthood and can result in an increased risk of conditions in life including cardiovascular disease.[3],[4] The SIGN guidelines for managing child healthy weight reflect the evidence about such lifecourse risks and recommend that parents should be made aware of the increased prevalence of a number of risk factors for cardiovascular disease and diabetes among obese children and adolescents.[4] Similarly, recognition of the mental health consequences for obese children is underlined by SIGN's recommendation that they should be referred for psychological assessment if they show signs of distress.
The policy significance of child healthy weight is evident by its inclusion as one of the Scottish Government's National Performance Framework (NPF) national indicators, which is being monitored via the Scottish Health Survey (SHeS). The original indicator in the 2007 NPF was:[5]
Reduce the rate of increase in the proportion of children with their Body Mass Index outwith a healthy weight
In the revised NPF, published in 2011, the indicator was changed to:[6]
Increase the proportion of healthy weight children
The revised NPF also includes a new indicator to increase the proportion of babies born with a healthy birth weight, another reflection of the increasing recognition that a long-term approach to overweight and obesity prevention is needed.
The introductions to the obesity chapters in the three previous SHeS Reports[7],[8],[9],[10] provided a detailed overview of the recent policy context in Scotland. These included:
- The Scottish Government's Healthy Eating, Active Living: An action plan to improve diet, increase physical activity and tackle obesity.[11]
- The Keep Well initiative.[12]
- The Scottish Government's Route Map for tackling obesity and the associated Obesity Route Map Action Plan, published in 2011.[13] SHeS is the measurement tool for seven of the Route Map's indicators, including the long-term goal of: fewer children in Scotland overweight or obese.[14]
- The Scottish Intercollegiate Guidelines Network (SIGN) national clinical guideline on obesity management.[4]
- The NHS Scotland HEAT[15] target established in 2008/09 to deliver 6,317 child healthy weight interventions by March 2011. 8,406 interventions were delivered during the target period.[16]
In addition, a number of policy actions targeted specifically at improving children's diets (described in Chapter 3) and physical activity levels (described in Chapter 4) are also relevant in the context of tackling obesity.
The HEAT target noted above was extended to cover the delivery of 14,910 interventions in the April 2011 to March 2014 period with a new requirement that at least 40% of such interventions should be delivered to children living in the two most deprived SIMD quintiles.[16] 5,052 interventions were delivered between April 2011 and March 2012 and an evaluation is currently underway to explore the impact of the programme.
The association between healthy weight and wellbeing noted above has also been reflected in the new National Mental Health Indicators for children and young people in Scotland.[17] The percentage of 2 to 15 year olds classified as obese or morbidly obese (Body Mass Index (BMI) at or above the 95th Centile of the 1990 UK reference data) is one of the indicators and has been included as part of the individual contextual domain as a measure of healthy living.
This chapter focuses on body mass index (BMI), derived from the direct measurements of height and weight taken in the main interview. Trends in child BMI over the 1998-2011 period are examined by age and sex. The chapter takes advantage of the combined 2008 to 2011 samples to provide more robust estimates of BMI for different age groups, and repeats the analysis of the association between parents' and children's BMI presented in the 2009 report.[9] Finally, differences by socio-demographic group are also shown.
5.2 METHODS AND DEFINITIONS OF MEASUREMENT
Full details of the protocols for carrying out the measurements are contained in Volume 3 of this report and are briefly summarised here.
5.2.1 Height
Height was measured using a portable stadiometer with a sliding head plate, a base plate and three connecting rods marked with a metric measuring scale. Participants were asked to remove shoes and socks. One measurement was taken, with the participant stretching to the maximum height and the head positioned in the Frankfort plane. The reading was recorded to the nearest even millimetre.
5.2.2 Weight
Weight was measured using Soehnle and Tanita electronic scales with a digital display. Participants were asked to remove shoes, socks and any bulky clothing. A single measurement was recorded to the nearest 100g. Participants aged under 2 years, or who were pregnant, or chairbound, or unsteady on their feet were not weighed. Participants who weighed more than 130 kg were asked for their estimated weights because the scales are inaccurate above this level. These estimated weights were included in the analysis.
In the analysis of height and weight, data from those who were considered by the interviewer to have unreliable measurements, for example those who had excessive clothing on, were excluded from the analysis.
5.2.3 Body Mass Index (BMI)
The Body Mass Index (BMI), defined as weight (kg)/height (m2), is a widely accepted measure that allows for differences in weight due to height. It has been used in each Scottish Health Survey report to date. However, BMI has some limitations.[19],[20] It does not distinguish between mass due to body fat and mass due to muscular physique. It also does not take account of the distribution of fat.
BMI was calculated for all those participants for whom a valid height and weight measurement was recorded.
BMI in children is defined in the same way as it is for adults: weight (kg)/height (m2). However, despite the relatively wide acceptance of the use of BMI as an adiposity indicator, the establishment of a specific obesity and overweight classification system for children and young people has proved to be difficult. Constant changes in body composition during growth mean that the relationship between weight-for-height and adiposity during childhood and adolescence is age-dependent, and this relationship is further complicated by ethnicity and gender.[21] Several methods have been employed to define early life overweight and obesity, including body fatness as measured by skinfold thickness,[22],[23] national BMI percentile charts,[24],[25],[26] weight-for-height indices,[27] BMI percentile cut-off points,[28] and international[29] and national[30] BMI cut-off points.
Percentile charts can be used to compare an individual child's BMI with the distribution of BMI in a reference population to see whether it corresponds with the average or whether it is unusually high or low. Since children's BMI changes as they age, the comparison needs to be age specific. For example the BMI for a child of 5 needs to be compared with a reference population with a large sample of 5 year olds rather than data for children with a wide age range.
The classifications of children's BMI used in this chapter, set out below, have been derived from BMI percentiles of the UK 1990 reference curves[25],[26] (referred to as the National BMI percentiles classification); these have been used in all the Scottish Health Surveys to date. SIGN recommends that these reference curves and thresholds should be used for population surveillance in Scotland.[31]
| Percentile cut-off | Description |
|---|---|
| At or below 5th percentile | Underweight |
| Above 5th percentile and below 85th percentile | Healthy weight |
| At or above 85th percentile and below 95th percentile | Overweight |
| At or above 95th percentile and below 98th percentile | Obese |
| At or above 98th percentile | Morbidly obese |
The 85th / 95th cut-off points are commonly accepted thresholds used to analyse overweight and obesity in children. These thresholds have previously been used to describe childhood overweight and obesity prevalence trends in the UK.[32],[33],[34],[35] The National BMI percentiles classification has been shown to be reasonably sensitive (i.e. not classifying obese children as non-obese) and specific (i.e. not classifying non-obese children as obese).[36],[37] As noted in the introduction, one of the Scottish Government's National Indicators relates to healthy weight in children, defined as neither underweight nor overweight / obese.[6] For this reason the data have been categorised to show the total proportions that are overweight, obese or morbidly obese, as well as the proportion underweight.
The use of reference curves require children's ages to be exactly matched to those in the reference population charts. This is a fairly straightforward process in clinical settings where an individual child's exact age can be compared with the look-up chart for their age. Matching exact ages to population charts in a survey dataset containing many children is somewhat less straightforward. SHeS uses a method developed by ISD Scotland that plots the exact ages of the children in the sample against the reference population data.[38]
Although children's exact age was used to calculate the BMI grouping prevalence rates (based on the interview date and the date of birth), the results are presented using grouped ages based on age at last birthday.
5.3 RESPONSE TO ANTHROPOMETRIC MEASUREMENTS, BY AGE AND SEX
The response to anthropometric measurements for children aged 2-15 in 2011 is shown in Table 5.1. Similar proportions of boys and girls had their height and weight measured. A valid measurement for height was obtained for 75% of boys and 76% of girls. The equivalent figures for weight were 76% and 75% respectively. The proportions providing valid height and weight measurements increased significantly with age for boys but not for girls. 70% of boys aged 2-6 had a valid height measurement and 72% had a valid weight measurement compared with 81% of those aged 12-15. Among girls, response to weight measurement was lowest among the oldest age group (aged 13-15) (72% compared with 76%-77% for younger girls).
A valid BMI was derived for 74% of boys and 75% of girls. Response increased significantly by age for boys, from 70% at age 2-6 to 81% at age 12-15, whereas among girls, the oldest group were the least likely to have a valid BMI measure (72%).
Table 5.1
5.4 TRENDS IN THE PREVALENCE OF CHILD HEALTHY WEIGHT, OVERWEIGHT AND OBESITY SINCE 1998
This section focuses on three measures of BMI for children aged 2-15: obese (>95th percentile); overweight or obese (>85th percentile); and within the healthy weight range (not underweight, overweight or obese; i.e. >5th percentile and <85th percentile). The previous three reports have included discussions of the proportions of children with a BMI outwith the healthy weight (i.e. underweight, overweight and obese combined).[7],[9],[10] This reflected the National Performance indicator relating to this measure.[5] However, as noted in the introduction, the new National Performance Framework child weight indicator, published in 2011, is based on healthy weight prevalence.[6] For this reason, both the prevalence of children within and outwith the healthy range are shown in Table 5.2, but the discussion below focuses on the within healthy range results. Figures for 1998 onwards are presented in Table 5.2 and Figure 5A. A more detailed analysis of the patterns by sex and age group, based on the 2008 to 2011 combined data, is presented in Section 5.5 below, and shown in Table 5.3.
As noted in the introduction, the proportion of children aged 2-15 who are obese or morbidly obese is one of the new Mental Health Indicators for children and young people in Scotland.[17] In 2011, 15.7% of children aged 2-15 were obese or morbidly obese. This represents a small rise over time in prevalence, from 13.0% when it was first measured in 1998. With the exception of 2009 and 2010, when figures stabilised or dropped slightly, most years have seen small increases. As noted in previous reports, this slight increase in obesity prevalence was largely confined to boys. For example, 13.1% of girls were obese in 1998, as were 13.7% in 2011, with fluctuations between 12.3% and 14.7% in the intervening years. In contrast, with the exception of 2009 and 2010, the proportion of boys that were obese has increased each year since 1998 when it stood at 13.0%. In 2011 17.5% of boys aged 2-15 were obese.
The overall prevalence of overweight including obesity since 1998 has followed a similar pattern to that of obesity. There was a slight increase in prevalence among all children (from 28.0% in 1998 to 31.6% in 2011), relatively little change for girls (ranging between 26.9% and 28.9%) and, despite some fluctuation between 2003 and 2009, a more pronounced increase for boys (from 27.8% in 1998 to 34.5% in 2011) in this period.
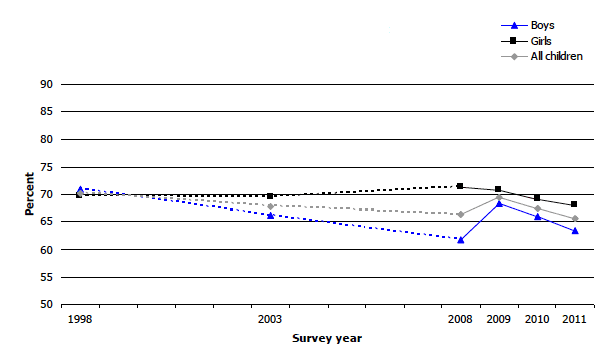
The trend data for the prevalence of healthy weight is presented in Figure 5A (note that the scale in the graph runs from 50 to 90 to increase its clarity). In line with the small increase in the prevalence of overweight including obesity outlined above, the proportion of children with a healthy weight followed a corresponding small decrease in the same period, from 70.3% in 1998 to 65.6% in 2011 (though note that at 66.4%, the 2008 figure is very similar to the 2011 figure). As is clear from Figure 5A, most of the change occurred among boys rather than girls, and there have been some notable fluctuations, particularly between 2008 and 2009 when there was a six percentage point increase in healthy weight prevalence in boys. Given the pattern since 2009, it seems likely that 2008 represented an atypical year, particularly for boys, and that the overall pattern is one of gradual decline.
Figure 5A, Table 5.2
Figure 5A
Percentage of children ages 2-15 with BMI in the healthy weight range by sex 1998, 2003, 2008, 2009, 2010 and 2011
5.5 CHILDREN'S BMI CATEGORIES, BY AGE AND SEX, 2008-2011 COMBINED
Previous SHeS reports noted that the sample size for children in individual survey years is not sufficiently large to detect statistically significant differences in BMI between some sub-groups. Now that data for the 2008-2011 period have been collected, it is possible to present more robust prevalence estimates for smaller age sub-groups based on all four years. This section examines the 2008-2011 combined prevalence figures for the three summary BMI groups discussed above (obese; overweight including obesity; and within healthy weight) as well as the proportion of underweight children, by age and sex.
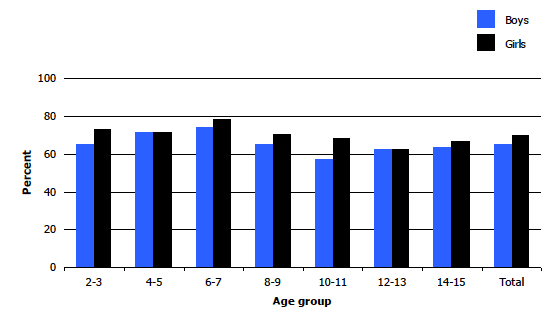
As Table 5.3 shows, in the 2008-2011 period two thirds (67.4%) of children aged 2-15 had a healthy weight. The difference between the proportion of boys (65.1%) and girls (69.8%) with a healthy weight was statistically significant. Healthy weight prevalence was also significantly associated with age, though not in a linear fashion (as Figure 5B illustrates). Prevalence of healthy weight was generally highest in the early years (ages 2-7) for both boys and girls. The patterns then depart somewhat, with a large decline among boys from 74.1% at age 6-7 to a low of 56.6% at age 10-11, followed by a small increase for those aged 12-15 (62.4%-63.0%). Among girls, there was a sharp decline between the ages of 6-7 and 8-9 (from 78.1% to 70.4%) which continued until age 12-13 (62.9%), before increasing to 66.4% at age 14-15.
Figure 5B
Prevalence of healthy weight in children aged 2-15, by age and sex, 2008-2011 combined
It is clear from Table 5.3 that the pattern in healthy weight prevalence across the age groups illustrated in Figure 5B was largely accounted for by differences in the proportion of children classified as obese or morbidly obese. For example, 5.1% of boys and 2.9% of girls aged 2-3 were morbidly obese, this increased threefold by the age of 10-11, to 15.9% in boys and 8.8% in girls. In contrast, the prevalence of underweight fluctuated in boys with no obvious pattern. Prevalence of underweight was higher among girls aged 10-13 (3.7%) than at any other age.
Three in ten children (30.4%) aged 2-15 were overweight or obese; again this was significantly higher for boys (32.7%) than for girls (28.0%). The proportions that were overweight or obese showed similar (but inverted) age-related patterns to those for children within the healthy weight range. For example, boys aged 10-11, and girls aged 12-13, had the highest overweight including obesity prevalence (41.9% and 33.4%, respectively).
Figure 5B, Table 5.3
5.6 CHILDREN'S BMI CATEGORIES, BY PARENTAL BMI CATEGORIES
The BMI status of children by parental BMI is presented in Table 5.4. This table is based on the 2008-2011 combined samples. Each year the survey included a boost sample of households in which children were interviewed but adults were not. This table is therefore based on children in the main sample where at least one of their parents was also interviewed (and had a valid BMI measurement). The data have been re-weighted so this analysis shows the pattern of association between parental and child BMI, and provides population estimates of the prevalence of child unhealthy weight in households with different parental profiles. For households with BMI measures for two parents, the measure of parental BMI was based on whichever parent's BMI was the highest.[39] If just one parent's BMI was measured this was used for this analysis.
The results presented in the 2009 report[9] showed a strong association between parental and child BMI. The 2008-2011 combined data confirmed this.
Children with a parent who was healthy weight or underweight were more likely to have a healthy weight themselves. For example, 75.7% of children with an under or healthy weight parent had a healthy weight compared with 71.4% of children with an overweight parent, and 58.7% of those with an obese parent.
Prevalence of overweight and obesity in children increased significantly in line with parental BMI. Children with an obese parent were twice as likely as those with an under or healthy weight parent to be overweight or obese (40.1% compared with 21.0%). The relative difference between the groups was even larger for the obese/morbidly obese category. The prevalence of obesity in children was three times higher for those with an obese parent than for those with an under or healthy weight parent (23.2% versus 9.4%).
All these patterns were similar for girls and boys. Despite having data from four years, the sample size is still not sufficiently large to permit this analysis to be conducted for mothers and fathers separately. Evidence from other sources suggests that maternal BMI has a stronger influence on girls' BMI than on boys', while the opposite is true for father's BMI.[40]
Table 5.4
5.7 OVERWEIGHT AND OBESITY, BY SOCIO-DEMOGRAPHIC FACTORS
Tables 5.5 to 5.7 present children's BMI status by socio-economic classification (NS-SEC of the household reference person), equivalised household income and the Scottish Index of Multiple Deprivation (SIMD) for the years 2008-2011 combined (descriptions of each of these measures are available in the Glossary at the end of this volume).
5.7.1 Socio-economic classification (NS-SEC)
Children's BMI status by NS-SEC of the household reference person is presented in Table 5.5 for all children and for boys and girls separately. There were no significant associations between NS-SEC and the prevalence of healthy weight, overweight including obese, or obesity. This confirms the findings presented in the 2009 report.[9]
Table 5.5
5.7.2 Equivalised household income
Similarly, as discussed in the 2009 report,[9] while the overall association between BMI status and household income was not significant, boys in the lowest income quintile households had a significantly higher prevalence of obesity (19.7%) than boys in other income groups (14.2%-16.4%). In contrast, no significant differences evident among girls.
Table 5.6
5.7.3 Scottish Index of Multiple Deprivation (SIMD)
Two measures of SIMD are being used throughout this report. The first - which uses quintiles - enables comparisons to be drawn between the most and least deprived 20% of areas and the three intermediate quintiles, and helps to assess the extent of any inequalities. The second contrasts the most deprived 15% of areas with the rest of Scotland (described in the tables as the "85% least deprived areas").
Of the socio-demographic factors considered, area deprivation had the strongest association with BMI status (Table 5.7 and Figure 5C). There was a significant association between deprivation (measured in quintiles) and BMI category. Patterns did not always follow a clear gradient, but children in the most deprived quintile were less likely to be a healthy weight and more likely to be obese than those in the other quintile groups. For example, 68.2%-70.0% of children in the three least deprived quintiles had a healthy weight compared with 63.3% of those in the most deprived quintile. In contrast, obesity prevalence was lowest among children in the least deprived quintile (12.1%), ranged from 14.5% to 15.2% in the next three, and was highest in the most deprived quintile, at 19.4%.
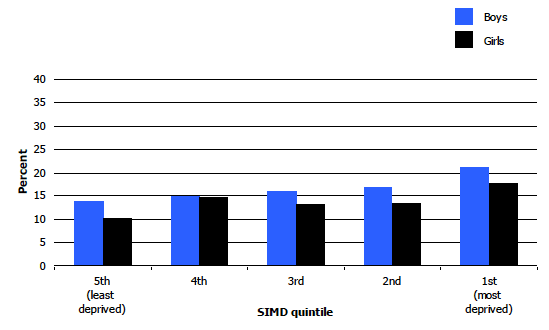
As Figure 5C illustrates, the increase in obesity prevalence by deprivation quintile among boys followed a linear pattern, increasing from 13.8% in the least deprived quintile to 21.0% in the most deprived quintile. For girls, while the pattern was not linear, prevalence was lowest for those in the least deprived quintile (10.4%) and highest in the most deprived (17.8%).The prevalence of underweight among boys and girls did not differ significantly across SIMD quintile groups.
In line with the findings for deprivation quintiles, children living in the 15% most deprived areas of Scotland had a significantly higher prevalence of obesity (18.7%) than children living elsewhere (14.5%). This pattern was evident for both boys and girls. The differences between these two deprivation groups were smaller for other BMI categories - though were in the direction expected based on the quintile analysis.
Figure 5C, Table 5.7
Figure 5C
Prevalence of obesity (including morbid obesity) in children ages 2-15, by SIMD quintile and sex, 2008-2011 combined
Throughout this chapter, differences in the prevalence of obesity have tended to stand out, both over time and between sub-groups. For example, obesity prevalence is associated with SIMD for both boys and girls, with income for boys, and is notably associated with parental BMI. These findings suggest that initiatives to increase the prevalence of healthy weight might benefit from a targeted focus on children at the upper end of the weight distribution, in combination with a whole population approach to increase healthy weight across the board.
Contact
Email: Julie Ramsay
There is a problem
Thanks for your feedback