The Scottish Health Survey 2011 - volume 2: children
Annual report of the Scottish Health Survey for 2011. Volume focussing on child health.
This document is part of a collection
1 General Health And Mental Wellbeing
Susan Reid
SUMMARY
- The general health of most children aged 0-15 was reported to be 'good' or 'very good' (95%) in 2010/2011, with no significant difference between boys and girls. 67% of boys and 68% of girls were described as having 'very good' health with 14-15 year olds the least likely to report this (55% of boys and 52% of girls).
- The proportion of children with 'bad' or 'very bad' health has remained unchanged since 1998 (1% in 2010/2011). While the proportion reporting 'very good' health as opposed to 'good' health appears to have increased. In 1998 60% of boys and girls had 'very good' health and 34% had 'good' health. The equivalent figures in 2010/2011 were 68% and 28% respectively.
- 15% of children aged 0-15 had a long-term condition in the 2008-2011 period; 9% were non-limiting, while 7% were limiting. Long-term conditions were more common in boys (17%) than girls (14%).
- Children under 4 were the least likely to have a long-term condition. Non-limiting conditions were more common than limiting ones in boys aged under 10 years, and in girls under eight.
- Conditions relating to the respiratory system were the most common long-term condition among 0-15 year olds in the 2008-2011 period (62 per 1000 children). These were followed by mental and behavioural disorders (27 per 1000), and skin complaints (20 per 1000).
- Respiratory system conditions were more common among boys than girls (71 per 1000 compared with 52 per 1000).
- There was a significant relationship between the prevalence of long-term conditions and household income with children in the lowest income quintile most likely to have a long-term condition (20% compared with 11% in the highest income quintile).
- In the 2008-2011 period 66% of children aged 13-15 had a GHQ12 score of zero while 9% had a score of four or more. These figures were not significantly different from the 2003 figures.
- Girls were more likely than boys to have a GHQ12 score of four or more (11% compared with 7%) and less likely to have a score of zero (62% compared with 70%).
- Social, emotional and behavioural problems in children aged 4-12 in 2010/2011 (measured via the Strengths and Difficulties Questionnaire (SDQ)) were more common in boys (10%) than girls (5%). 86% of children had no such problems while 7% were assessed as borderline.
- Children with abnormal total difficulties scores on the SDQ were less likely than those with a normal score to report 'very good' or 'good' general health and were also more likely to have a long-term condition.
- Children who rated their health as 'fair', 'bad' or 'very bad' had significantly increased odds of having a borderline or abnormal SDQ score compared with those who rated their health as 'good' or 'very good' (odds of 5.75 for girls and 3.95 for boys).
1.1 INTRODUCTION
This chapter covers two interrelated aspects of children's health. The first is self-assessed general health and long-term conditions. The second topic focuses on children's mental health and wellbeing. To acknowledge the interrelationship between these topics the chapter also looks at the extent to which low levels of mental wellbeing are associated with poor physical health.
As noted in the introduction to this volume, health is a key component of the Scottish Government's National Performance Framework,[1],[2] and a commitment to improving children's wellbeing and longer-term outcomes in life lies at the heart of many initiatives led by Scottish Government, local authorities and other bodies with an interest in children's lives.[3],[4] The measures reported in this chapter are therefore important indicators of progress in this area. In recent years, the overall approach to mental health in Scotland has been guided by the policy and action plan for mental health improvement published in 2009 Towards a Mentally Flourishing Scotland.[5] The Scottish Government published its new mental health strategy on 13 August 2012.[6] The strategy makes a series of commitments in respect of children and young people's mental health, including faster access to specialist services, greater attention to infant mental health and improved services for looked after children.
As discussed in the introductions to the general health and wellbeing chapters in the 2009 and 2010 Scottish Health Survey Reports,[7],[8] in 2007 NHS Health Scotland published a set of national, sustainable indicators for monitoring adult mental health.[9] A parallel set of national mental health indicators for children and young people was launched in 2011,[10] following an extensive evidence review and consultation. There are 109 indicators in the framework, some of which draw on multiple measures, structured around two levels: high level constructs relating to the state of children's mental health and wellbeing, and contextual constructs spanning five domains that influence, and are influenced by, mental health. The five domains are: individual, family, the learning environment, community and structural (such as equality, social inclusion and discrimination). The SHeS will be used to monitor the following indicators (all of which are reported in this chapter):
- Percentage of children and young people aged 15 years and under whose health in general is perceived to be good or very good.
- Percentage of children and young people aged 15 years and under who have a long-standing physical condition or disability that has troubled them for at least 12 months, or is likely to affect them for at least 12 months.
- Percentage of children and young people aged 15 years and under who have a long-standing physical condition or disability that limits their daily activities.
- Percentage of 4 to 12 year olds with a 'borderline' or 'abnormal' total difficulties score on the Strengths and Difficulties Questionnaire (SDQ).
- Percentage of 4 to 12 year olds with a 'normal' score on the pro-social scale of the Strengths and Difficulties Questionnaire (SDQ).
- Percentage of 4 to 12 year olds with a 'borderline' or 'abnormal' score on the emotional symptoms scale of the Strengths and Difficulties Questionnaire (SDQ).
- Percentage of 4 to 12 year olds with a 'borderline' or 'abnormal' score on the conduct problems scale of the Strengths and Difficulties Questionnaire (SDQ).
- Percentage of 4 to 12 year olds with a 'borderline' or 'abnormal' score on the hyperactivity/inattention scale of the Strengths and Difficulties Questionnaire (SDQ).
- Percentage of 4 to 12 year olds with a 'borderline' or 'abnormal' score on the peer relationship problems scale of the Strengths and Difficulties Questionnaire (SDQ).
In addition to these measures of children's direct experiences, the survey will also be used to report on indicators of parental wellbeing, alcohol misuse, and limiting long-term conditions, which acknowledges the important influence of parental health and wellbeing on children's outcomes. These measures will be included in future reports.
Many of the measures discussed here have been included in the survey series since children were first included in 1998 so they not only provide important contemporary data for the national mental health indicator set, but they also allow historical comparisons to be made.
1.2 SELF-ASSESSED GENERAL HEALTH
1.2.1 Introduction
This section presents data on children's general health. Parents answered questions on behalf of children aged 0-12, while those aged 13-15 were asked to rate their own health status. The answer options presented were 'very good', 'good', 'fair', 'bad' or 'very bad'.[10] This question is part of the new mental health indicators set for children. The relevant indicator is: "Percentage of children and young people aged 15 years and under whose health in general is perceived to be good or very good".
1.2.2 Trends in self-assessed general health since 1998
In 2010/2011, the general health of 95% of children aged 0-15 was reported as being either 'very good' or 'good'. This figure has been consistently high for both boys and girls, with very little variation, since it was first measured in 1998.[11] The proportions reported to be in 'bad' or 'very bad' health have also remained consistent over time, at just 1%. There has, however, been a shift in recent years in the composition of the very good/good category, with an increase in the proportion of children described as in 'very good' health (from 60% in 1998 to 67% in 2011) and a corresponding decrease in those reported to be in 'good' health (from 34% in 1998 to 29% in 2011).
Table 1.1
1.2.3 Self-assessed general health, by age and sex, 2010/2011
In 2010/2011, boys and girls had very similar perceptions of their health in general. Two thirds (67% of boys and 68% of girls) were described as having 'very good' health, while 28% of boys and 27% of girls described it as 'good'. Just 1% of children described their health in general as 'bad' or 'very bad'.
When combined, the proportion of children with 'very good' or 'good' self-assessed health did not vary by age. However, the oldest children were less likely than their younger counterparts to have 'very good' health, and were more likely than them to report being in 'good' health. For example, 55% of boys aged 14-15 had 'very good' health while the figures for younger boys ranged from 66% to 74% with no clear pattern. Among girls, 52% of those aged 14-15, and 62% of those aged 12-13 had 'very good' health, compared with 66%-76% of younger girls. This difference between the oldest age groups and those younger than them could, in part, be explained by the change in interview methods at this age (children aged 13-15 answer the questions themselves).
Table 1.1
1.3 LONG-TERM CONDITIONS
1.3.1 Introduction
All participants were asked if they had any long-term physical or mental conditions or disabilities that had affected - or were likely to affect - them for at least twelve months (as before, parents answered on behalf of children aged 0-12). Those who reported having such a condition were asked to say whether it limited their daily activities in any way. This enabled conditions to be further classified as either 'limiting' or 'non-limiting'. As the question did not specify that conditions had to be doctor-diagnosed, responses will have been subject to some distortion due to variation in individuals' perceptions. This question is part of the new mental health indicators set for children.[10] The relevant indicators are: "Percentage of children and young people aged 15 years and under who have a long-standing physical condition or disability that has troubled them for at least 12 months, or is likely to affect them for at least 12 months", and "Percentage of children and young people aged 15 years and under who have a long-standing physical condition or disability that limits their daily activities".
Questions about long-term conditions have been included since the survey began, however changes to the question wording in recent years mean that the trend data is only available from 2008. The tables are based on data from the 2008-2011 combined sample, which enables more robust figures to be presented for narrow age subgroups. The prevalence of long-term conditions is presented by age and sex, and then by three socio-economic measures: the National Statistics Socio-economic Classification (NS-SEC), household income and the Scottish Index of Multiple Deprivation (SIMD). This is the most detailed presentation of long-term conditions in children since the 2003 SHeS Report.[12]
1.3.2 Prevalence of long-term conditions, 2008-2011 combined, by age and sex
The combined data for 2008 to 2011 showed that 15% of children aged 0-15 had a long-term health condition that had either lasted, or was likely to last, for at least 12 months. This was comprised of 7% with limiting conditions and 9% with non-limiting conditions. Boys were more likely than girls to have a long-term condition, 17% and 14% respectively. Although not large, this difference between the genders was statistically significant.
As Figure 1A illustrates, the prevalence of long-term health conditions increased with age for both boys and girls, most notably up to the age of nine. It then stabilised somewhat among boys but fluctuated more for girls. The figures for all children presented in Table 1.2 help illustrate the general pattern. The prevalence of long-term conditions doubled between the ages of 0-1 and 4-5 (from 7% to 14%), and then ranged from 16% to 20% among the older age groups. Non-limiting conditions were more common than limiting ones in boys aged under 10 years, and in girls under eight, after which the figures were broadly similar for both types of long-term condition.
Figure 1A, Table 1.2
Figure 1A
Prevalence of long-term conditions in children ages 0-15, by age and sex, 2008-2011 combined
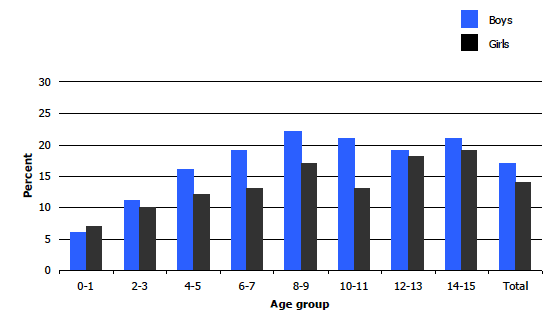
1.3.3 Rates of long-term conditions, 2008-2011 combined, by age and sex
Long-term conditions were classified using the International Classification of Diseases (ICD-10) coding schema.[13] Conditions were first coded by broad category and then aggregated into groups based on ICD-10 chapters. The classification of conditions was based solely on participants' definitions and self-reported symptoms. As a result the classification might not always correspond with a doctor's diagnosis. As the prevalence for some of the conditions is very low, figures are presented in rates per 1000 children.
The most common long-term conditions for children aged 0-15 in the 2008 to 2011 period related to the respiratory system (62 per 1000) (Table 1.3). These were followed by mental and behavioural disorders (27 per 1000), and skin complaints (20 per 1000).
The overall pattern for types of conditions was generally similar for boys and girls, but there were some minor differences. Although respiratory system conditions were the most common for both boys and girls, rates were higher in boys than girls (71 versus 52 per 1000). Rates of mental and behavioural disorders were also higher in boys than girls (38 versus 15 per 1000). Mental and behavioural disorders were the second most common condition for boys, and were joint third most common for girls, alongside digestive conditions and musculoskeletal conditions. Rates for skin conditions were similar for boys and girls (at 20 and 19 per 1000, respectively).
Variation by age was dependent on condition type. For some, such as respiratory system conditions and mental and behaviour disorders, rates increased with age. In contrast, prevalence of conditions of blood and related organs and conditions of the heart and circulatory system did not vary by age group while prevalence of musculoskeletal conditions varied by age but with no clear pattern.
Table 1.3
1.3.4 Long-term conditions by socio-demographic characteristics
Tables 1.4 to 1.6 present the prevalence of long-term conditions by socio-economic classification (NS-SEC of the household reference person), equivalised household income and the Scottish Index of Multiple Deprivation (descriptions of each of these measures are available in the Glossary at the end of this volume). The figures presented are based on the 2008 to 2011 surveys combined.
Socio-economic classification (NS-SEC)
Overall, the proportion of children with limiting or non-limiting long-term conditions was not significantly associated with NS-SEC. However, when restricted to just those with limiting conditions, there was a significant association, though absolute differences were small in percentage point terms. The prevalence of limiting conditions increased from 5% among children living in managerial, professional and intermediate households to 8% among those in semi-routine and routine households.
Table 1.4
Equivalised household income
As Table 1.5 and Figure 1B illustrate, as household income decreased, the prevalence of long-term conditions increased significantly from 11% of children in the highest income quintile households to 20% for those in the lowest quintile. As was the case with NS-SEC, differences were particularly marked in relation to limiting long-term conditions with prevalence increasing from 4% to 10% across the income quintiles. This pattern was the same for both girls and boys.
Table 1.5
Figure1B
Prevalence of long-term conditions in children aged 0-15, by equivalised household income quintile, 2008-2011 combined
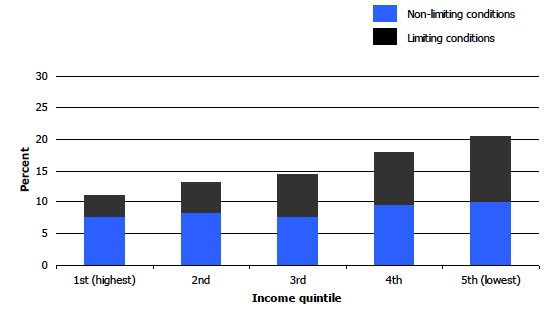
Scottish Index of Multiple Deprivation (SIMD)
Two measures of SIMD are being used throughout this report. The first, which uses quintiles, enables comparisons to be drawn between the most and least deprived 20% of areas and the intermediate quintiles. The second contrasts the 15% most deprived areas with the rest of Scotland (described in the tables as the "85% least deprived areas").
A similar, but somewhat less steep, gradient was evident in relation to the association between SIMD quintiles and long-term conditions. The prevalence of long-term conditions increased in line with level of deprivation, from 12% in the least deprived quintile to 18% in the most. The pattern was evident for both boys and girls. Once again, the difference was largely driven by variations in the prevalence of limiting, rather than non-limiting, conditions. The proportion of children in the most deprived quintile with limiting conditions was double that in the least deprived quintile (10% versus 5%).
Differences between children in the most deprived 15% of areas and those in the rest of Scotland were small but, due to the relatively large sample size, were statistically significant. Overall, 18% of children living in the 15% most deprived areas in Scotland had a long-term condition compared with 15% of those living elsewhere. The equivalent figures for limiting conditions were 10% and 6%, respectively.
Table 1.6
1.4 MENTAL HEALTH AND WELLBEING
1.4.1 Introduction
Wellbeing in children aged 13-15 has been measured via the GHQ12[14] since children were first included in SHeS in 1998. However, a recent investigation of the apparently large change in GHQ12 scores between 1998 and 2003 revealed an error in the labelling of the answer scale for one of the items in the 1998 survey. This resulted in a much higher prevalence of depression than would be expected. As a consequence the trend discussion in this section is limited to the 2003 - 2011 period.
GHQ12 is a widely used standard measure of mental distress and psychological ill-health consisting of 12 self-completion questions on concentration abilities, sleeping patterns, self-esteem, stress, despair, depression, and confidence in the previous few weeks. Children completed the questionnaire themselves. Responses to the GHQ12 items were scored, with one point given each time a particular feeling or type of behaviour was reported to have been experienced 'more than usual' or 'much more than usual' over the past few weeks. These scores are combined to create an overall score of between zero and twelve. A score of four or more (referred to as a 'high' GHQ12 score) has been used here to indicate the presence of a possible psychiatric disorder. GHQ12 measures deviations from people's usual functioning in the previous few weeks. It cannot, therefore, be used to detect chronic conditions. As the number of children aged 13-15 in the sample is fairly small, the most recent figures presented here are based on the 2008-2011 combined samples.
The social, emotional and behavioural development of children aged 4-12 has been measured via the Strengths and Difficulties Questionnaire (SDQ)[15] since 2003. The SDQ is a brief behavioural screening questionnaire designed for use with the 3-16 age group. The SDQ was completed by a parent on behalf of all children aged 4-12.
The SDQ comprises 25 questions covering themes such as consideration, hyperactivity, malaise, mood, sociability, obedience, anxiety, and unhappiness. It is used to measure five aspects of children's development: emotional symptoms, conduct problems, hyperactivity/inattention, peer relationship problems and pro-social behaviour.
A score was calculated for each of the five aspects, as well as an overall 'total difficulties' score which was generated by summing the scores from all the domains except pro-social behaviour. The total difficulties score ranged from zero to forty with a higher score indicating greater evidence of difficulties. There are established thresholds indicating 'normal' (score of 13 or less), 'borderline' (14-16) or 'abnormal' scores (17 or above).
The total and individual SDQ domain scores all feature in the new mental health indicators set for children.[10] The indicators are the percentage of children with normal scores for the pro-social domain, and the percentages with abnormal/borderline scores in the other four domains and overall. All these figures are reported in the tables, although much of the discussion in this section focuses on the total difficulties score. It looks at patterns by age and sex, compares scores in 2003, 2008/2009 and 2010/11, and looks at scores by socio-economic factors, and by general health and long-term conditions. Finally, factors associated with borderline or abnormal total difficulties scores are also presented.
1.4.2 Trends in GHQ12 scores since 2003
GHQ12 scores were broadly similar in 2003 and the 2008-2011 period. For example, in 2003 69% of children aged 13-15 had a score of zero, as did 66% in 2008-2011. The respective figures for boys were 72% and 70%, while the figures for girls were 66% and 62%. There was no significant change in the proportion of children with a score of four or more (indicative of a possible disorder) between 2003 and 2008-2011 (8% and 9%, respectively). As noted above, the composite GHQ12 scores in 1998 cannot be compared over time. However, the results for the 11 individual scale items that are directly comparable were very similar at all three time points (data not shown).
Table 1.7
1.4.3 GHQ12 scores, 2008-2011 combined, by age and sex
GHQ12 scores were significantly associated with both age and sex in 2008-2011, with psychological distress more common in girls than boys, and in older rather than younger teenagers. Boys were more likely than girls to have a score of zero (70% versus 62%), and were less likely to have a score of four or more (7% versus 11%). The difference between boys and girls appeared after the age of 13. For example, the proportion of girls with a score of zero declined from 74% at age 13, to 57% at age 14 and 54% at age 15. The corresponding figures for boys showed a smaller steadier decline, from 75% to 70% and 65% across the three ages. The pattern with regards scores of four or more was similar, with girls aged 14 and 15 more than twice as likely as girls aged 13 to have a GHQ12 score of four or more (14%, 14% and 6% respectively). For boys, the difference occurred later: 6% of those aged 13 or 14 had a score of four or more compared with 11% at age 15.
Table 1.7
1.4.4 Trends in SDQ scores since 2003
There has been little change over time in the SDQ score of children aged 4-12. In 2003, 9% of children had an abnormal total difficulties score as did 8% in 2008/2009 and 2010/2011. A further 8% had borderline scores in 2003, and the figures for 2008/2009 (6%) and 2010/2011 (7%) were not significantly different from this. The figures for scores in the normal range were 83% in 2003 and 86% in the two most recent periods. Mean SDQ score have also been very similar over time: 8.2 in 2003 and 8.0 in both 2008/2009 and 2010/2011.
Although there appear to be small differences in the SDQ scores for girls between 2003 and the later periods, these were not statistically significant. Scores for boys have remained very stable across time.
Table 1.8
1.4.5 SDQ scores by age and sex, 2010/2011
Looking now in more detail at the 2010/2011 results, boys were more likely than girls to have SDQ scores indicative of problem behaviour or low wellbeing. For example, boys were twice as likely as girls to have an abnormal SDQ score (10% versus 5%). The mean score for boys was also significantly higher than for girls (8.6 versus 7.3).
Table 1.8
Significant differences between boys and girls were seen in the proportion who had abnormal scores in three of the five domains measured in the SDQ: peer problems (13% and 8%, respectively), hyperactivity (15% and 9%), and pro-social behaviour (3% and 1%).
The proportion of children with normal, borderline or abnormal total SDQ scores did not vary significantly by age. However, significant differences were present for the emotional symptoms scores, where the prevalence of problem scores increased with age. For example, 4% of boys aged 4-5 had an abnormal emotional symptoms score compared with 11% of those aged 10-12. The corresponding figures for girls were 5% and 11%, respectively.
Table 1.9
1.4.6 SDQ scores by general health and long-term conditions, 2008-2011 combined
Table 1.10 and Figures 1C and 1D use data from the 2008-2011 combined samples to present the prevalence of 'very good' or 'good' general health, and long-term conditions, among children with normal, borderline and abnormal SDQ scores. As illustrated in Table 1.3, mental and behavioural disorders were the second most common type of long-term condition for children so the SDQ, which is a direct measure of such conditions, should overlap with the long-term conditions measure.[16] This analysis makes it possible to assess the burden of limiting conditions and poor health experienced by children with behavioural or emotional difficulties.
Children with an abnormal total difficulties SDQ score were least likely to report 'very good' or 'good' general health and most likely to have a long-term health condition. Among children with a normal total difficulties SDQ score, 97% reported a very good/good level of general health, compared with 89% of those with borderline scores, and 83% of children with abnormal scores. This variation was largely explained by a difference in the proportions describing their health as 'very good' (this was 73% among those with a normal score and 46% for those with an abnormal score). 11%-16% of children with borderline or abnormal scores had 'fair' or 'bad' health compared with just 3% of those with normal scores.
A similar pattern was seen in relation to the prevalence of long-term conditions with a three-fold increase in prevalence between children with normal and abnormal scores (from 14% to 44%). The difference was even greater for limiting conditions: children with abnormal total difficulties scores were nearly six times as likely as those with normal scores to have a limiting long-term condition (29% versus 5%).
The same overall patterns were evident for both boys and girls. Although boys with an abnormal total difficulties score were more likely than girls with such a score to have a long-term condition (48% and 35%, respectively), the sample size for girls with abnormal scores was quite small so this is not a very precise estimate of the difference between groups.
Table 1.10
Figure 1C
Prevalence of very good/good general health and long-term conditions in boys ages 4-12, by SDQ total difficulties scores, 2008-2011 combined
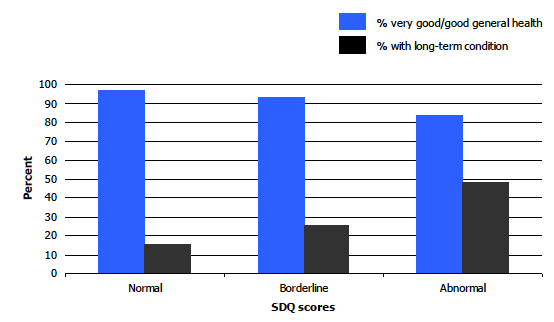
Figure 1D
Prevalence of very good.good general health and long-term conditions in girls ages 4-12, by SDQ total difficulties scores, 2008-2011 combined
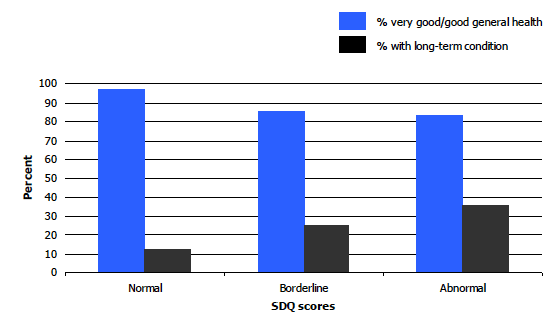
1.4.7 Factors associated with borderline or abnormal total difficulties scores on the SDQ
Using the 2008-2011 combined data, multivariate logistic regression was used to examine the independent effect of a range of socio-demographic factors associated with having a borderline (14-16) or abnormal (17-40) total difficulties score on the SDQ. Separate models were run for boys and girls with significant factors discussed below.
The odds ratios of having a borderline or abnormal total difficulties score are presented in Table 1.11. Boys and girls with a total score of 14 or above were classified as having a borderline/ abnormal score. In these analyses, the odds of a reference category (shown in the table with a value of 1) are compared with that of the other categories for each of the individual factors. In this example, an odds ratio of greater than 1 indicates that the group in question has higher odds of having a borderline/ abnormal total difficulties score than the chosen reference category, and an odds ratio of less than 1 mean they have lower odds. By simultaneously controlling for a number of factors, the independent effect each factor has on the variable of interest can be established. For more information about logistic regression models and how to interpret their results see the glossary at the end of this volume.
Self-assessed health was significantly associated with having a borderline or abnormal total difficulties score on the SDQ for both boys and girls. Compared with those who rated their health as 'good' or 'very good', those who rated their health 'fair', 'bad' or 'very bad' had significantly increased odds of having a borderline or abnormal score (odds ratio of 5.75 for girls and 3.95 for boys).
For boys, the other factors that were associated with having a borderline or abnormal SDQ score were area level deprivation (SIMD) and how physically active they were.
Boys living in the most deprived areas of Scotland (1st SIMD quintile) had significantly higher odds of having a borderline or abnormal total difficulties score than those living in the least deprived areas (odds ratio of 2.42). Compared with those meeting the physical activity guidelines, boys who had low activity levels had significantly higher odds of having borderline or abnormal total difficulties score (odds ratio of 2.17).
In addition to self-assessed health, the other factors that were significantly associated with girls having borderline or abnormal total difficulties scores on the SDQ were NS-SEC, household income and household composition.
Girls living in semi-routine and routine occupation households had increased odds (1.87) of having a borderline or abnormal total difficulties score compared with those living in managerial and professional households. Household income was also significantly related to SDQ scores for girls, with those living in the lowest household income quintile having significantly higher odds of a borderline/abnormal score compared with those in the highest income quintile (odds ratio of 3.41).
Finally, when compared with girls that lived in a one child household, those living in two children households (aged 0 to 15) had decreased odds of having a borderline or abnormal total difficulties score (odds ratio of 0.61).
Table 1.11
Contact
Email: Julie Ramsay
There is a problem
Thanks for your feedback