Scottish Health Survey 2019 - volume 1: main report
Presents results for the Scottish Health Survey 2019, providing information on the health and factors relating to health of people living in Scotland.
This document is part of a collection
Chapter 1: General Health, CVD and Diabetes
Among all adults in 2019:
- 72% described their general health as 'good' or 'very good'
- 9% described their general health as 'bad' or 'very bad'
Self-assessed 'good' or 'very good' general health in all adults has reduced since 2009.

A greater proportion of men described their general health as 'good' or 'very good' in 2019.
- 74% Men
- 70% Woman
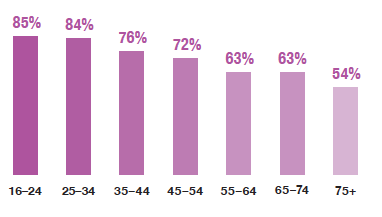
The proportion of adults who assessed their general health to be 'good' or 'very good' in 2019 decreased with age.
Among all children in 2019:
- 95% described their general health as 'good' or 'very good'
- 1% described their general health as 'bad' or 'very bad'
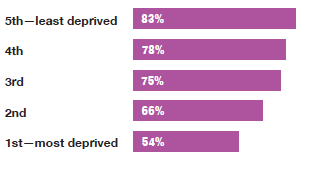
The age-standardised proportion of adults who self-assessed their general health as 'good' or 'very good' once again varied by area deprivation in 2019.
Around half of adults reported living with (limiting or non-limiting) long-term conditions.
- 47%
The proportion of adults with long-term conditions increased with age.
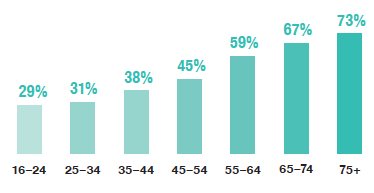
Higher proportions of men than women had:
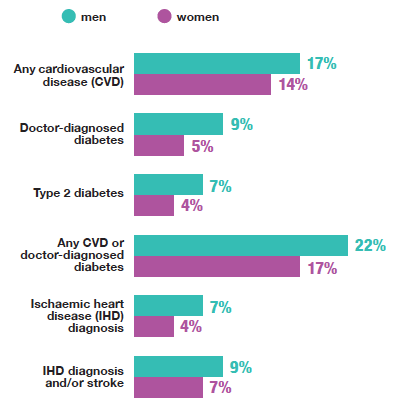
There was no variation by gender in the prevalence of Type 1 diabetes or stoke in 2019.
- 1% prevalence of Type 1 diabetes among all adults
- 3% prevalence of stroke among all adults
The proportion of adults with hypertension* has stabilised in recent years:
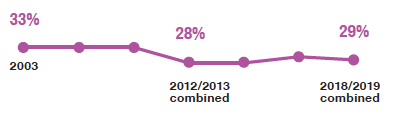
A higher proportion of men had hypertension than women in 2018/2019 combined.*
- Men 31%
- Woman 26%
* Nurse equivalent calibrated estimates
In 2019, over half of adults reported having ever attended CPR training.
- 56% CPR training
Adults who had ever attended CPR training, reported doing so as: **
In 2019, a fifth of all adults reported attending any CPR training (original or refresher) within the past two years.
- 21%
In 2019, the proportion of adults who reported attending any CPR training (original or refresher) within the past two years generally decreased with age.
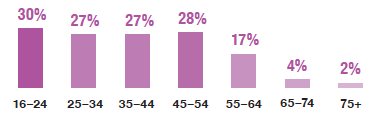
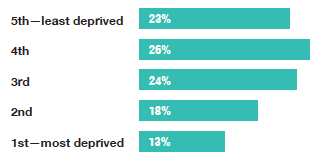
Those living in the most deprived areas were less likely to have attended any CPR training in the past two years than those in the remaining quintiles.
** Combined figures may diff er from individual categories due to rounding.
1 General Health, CVD And Diabetes
1.1 Introduction
Population measures of self-reported health are evidenced to be good predictors of mortality, morbidity or use of health care[1]. They can reflect subjective experiences of both diagnosed and undiagnosed illnesses both physical and mental, and their severity, which more objective measures for the whole population may overlook.
In addition to the impact on individuals, the prevalence of long-term conditions places considerable and unsustainable strain on healthcare provision[2]. Further challenges are presented by the persistent inequalities in health outcomes and the ageing population. Significant disparities in life expectancy, which can differ by more than 20 years between the most and least deprived areas in Scotland, continue to be evident by levels of deprivation[3]. In addition, older people are more likely to have at least one long-term condition and often multiple conditions, which coupled with a general increase in life expectancy, means that more people are living in ill-health for longer[4]. In the context of an ageing population, where a 75% increase in the proportion of those aged 75 and over between 2004 and 2031 is expected[5], this remains a critical health matter for Scotland.
Cardiovascular disease (CVD) is a general term describing diseases of the heart and blood vessels whereby blood flow to the heart, brain or body is restricted. Its main components are ischaemic heart disease (IHD, or coronary heart disease) and stroke, both of which are well-established clinical priorities for the NHS in Scotland[6],[7]. Since 2009, there has been a steady downward trend in incidence and deaths from coronary heart disease and stroke in Scotland. Between 2009 and 2018 the mortality rate for coronary heart disease decreased by 32% and the rate at which new cases of coronary heart disease occur has fallen by 19% in the last ten years although it has remained steady over the last four years. However, in the last five years the rate of decline in coronary heart disease has slowed and since 2016 death rates from heart attacks have increased by a small amount[8]. In the last decade overall incidence for cerebrovascular disease (of which stroke is the most common) has decreased by 12% and the mortality rate has decreased by 34%[9]. Coronary heart disease (CHD) continues to be one of the leading causes of death in Scotland with 6,615 deaths in 2018 where it was the underlying cause[10]. Stroke also remains one of the biggest killers in Scotland and the leading cause of disability[11].
Diabetes, the most common metabolic disorder, is a growing health challenge for Scotland. The prevalence of people registered with Type 1 diabetes increased from 27,464 in 2008 to 32,828 in 2018, which reflects better survival and the rising incidence in children. The number of people registered with Type 2 diabetes increased from 190,772 in 2008 to 267,615 in 2018 which could relate to several factors, including: demographic change - diabetes is more prevalent in older people, so the increasing number of older people each year increases the prevalence of diabetes - better survival, and possibly better detection[12].
Cardiac arrest is when the heart suddenly stops pumping blood round the body. Cardiopulmonary Resuscitation (CPR) keeps blood circulating until attempts are made to restart the heart when someone has a cardiac arrest. Every year around 3,500 Scottish people experience a cardiac arrest and attempted resuscitation in the community with 1 in 10 currently surviving to hospital discharge compared to 1 in 20 when the Scotland's Out-of-Hospital Cardiac Arrest (OHCA) Strategy (see below) was released in 2015[13], although in some European countries there have been almost 1 in 4 survival rates[14]. Early recognition of a cardiac arrest and administration of CPR is one of the key elements that contribute to better survival rates. Prompt bystander CPR can increase the likelihood of survival by 2 or 3 times[15].
1.1.1 Policy background
The Scottish Government recognises the importance of working towards sustainable healthcare provision, particularly in the context
of the changing Scottish demographic, notably an ageing population and increasing numbers of people living with long-term conditions and multi-morbidity. The strategic policy focus on promoting and improving general health and wellbeing, supporting people living with long term illnesses/conditions and equipping more people in CPR is set out in four over-arching strategies.
The National Clinical Strategy[16], published in 2016, is a high level vision for how health and social care services need to and should change over a 15 year period while the Health and Social Care Delivery Plan[17] presents a programme that is focused on prevention, early intervention and support for self-management. The aim is to enable those living in Scotland to live longer, healthier lives with the highest standard of care, be this at home or in a homely setting.
Practising Realistic Medicine[18], publishedin 2018, outlined ways to support the translation of the principles of the previous report(Realising Realistic Medicine[19]) from theory through to patient-centred, practical application. In addition to encouraging a personalised approach to individual patient care and tackling sustainability of NHS service provision, the report examines the ways in which the principles of realistic medicine can be applied to positively influence the social determinants of health such as childhood experiences, social support, access to health services and more.
Underpinning these strategies, Public Health Priorities for Scotland[20]sets out six public health priorities, aimed at improving the health of Scotland and increasing healthy life expectancy including, amongst others, a range of initiatives geared towards a Scotland where people eat well, have a healthy weight and are physically active.
These priorities, along with the Scottish Government's long-term condition strategies (the over-arching Action Plan[21] published in 2009 and the separate heart disease[22], stroke[23] and diabetes[24] improvement plans published in 2014) support Scotland's Public Health Priorities[25] and the National Performance Framework National Outcome that 'we are healthy and active[26].
A number of the National Indicators are linked to reducing cardiovascular disease risk factors, most notably smoking as part of the health risk behaviours indicator, but also physical activity and maintaining healthy weight[27],[28]. In addition to being a risk factor for cardiovascular disease, living with overweight or obesity is also the primary risk factor for the development of Type 2 diabetes[29].
Increased likelihood of survival following a cardiac arrest is supported by Scotland's Out-of-Hospital Cardiac Arrest (OHCA) Strategy. Launchedin March 2015[30], the overarching aim is for Scotland to become an international leader in OHCA outcomes by 2020. This is underpinned by two high level aims:
- To increase survival rates after an OHCA in order to save 1,000 additional lives by 2020.
- To equip an additional 500,000 people in Scotland with CPR skills by 2020.
1.1.2 Reporting on general health, CVD, diabetes and CPR training in the Scottish Health Survey (SHeS)
In this chapter trends in self-assessed general health for adults and children are presented. Prevalence of self-reported long-term conditions in adults is reported for 2019 and trends for self-reported CVD conditions and diabetes prevalence in adults are presented as well as for 2019. Blood pressure level trends and detection and treatment of hypertension for 2016-19 combined are presented. Prevalence of CPR training (including refresher training) and the length of time since CPR training was last attended are also reported for 2019.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on general health and CVD are also published on the Scottish Government SHeS website https://www.gov.scot/collections/scottish-health-survey/
1.2 Methods and Definitions
1.2.1 Methods
Self-assessed general health
Each year, participants who are aged 13 and over are asked to rate their health in general with answer options ranging from 'very good' to 'very bad'. For children under the age of 13 the question is answered by the parent or guardian completing the interview on their behalf.
CVD conditions and diabetes
Participants were asked whether they had ever suffered from any of the following conditions: diabetes, angina, heart attack, stroke, heart murmur, irregular heart rhythm, or 'other heart trouble'. If they responded affirmatively to any of these conditions, participants were asked whether they had ever been told they had the condition by a doctor and whether they had experienced the conditions in the previous 12 months. For the purposes of the analysis presented in this chapter, participants were only classified as having a particular condition if they reported that the diagnosis had been confirmed by a doctor.
It is important to note that no attempt was made to verify these self-reported diagnoses objectively. It is therefore possible that some misclassification may have occurred because some participants may not have remembered (or not remembered correctly, or not known about) diagnoses made by their doctor.
Blood pressure
Blood pressure was measured as part of the biological module[31], using the Omron HEM device. This equipment has been used on SHeS since 2003. Prior to 2012, blood pressure was collected in a follow-up interview conducted by survey nurses. The nurse interview was discontinued in 2012, and since then specially trained interviewers have been collecting some of the less complex measures and samples previously collected by nurses, as part of the biological module. The equipment and protocol for taking blood pressure readings did not change. A validation study was carried out to assess the impact of the switch from nurse to interviewer administration[32].
As a result, unadjusted measurements collected by interviewers are used within the report for more recent periods (2012/2013, 2014/2015, 2016/2017 and 2018/2019), with calibrated estimates (nurse equivalent) being used to show longer-term trends.
Three blood pressure readings were taken from consenting participants at one minute intervals using an appropriately sized cuff and on the right arm where possible. Participants were in a seated position and readings were taken after a five minute rest. Systolic and diastolic pressures and pulse measurements were displayed on the Omron for each measure. As in previous years, pregnant participants were excluded.
Since the size of the cuff used when taking blood pressure readings is an important factor in ensuring that accurate measurements are obtained three different sizes of cuff were available for use. Full details of the protocol used to take blood pressure readings in the survey are available on request from ScotCen.
The blood pressure measures used in this chapter are the means of the second and third measurements obtained for those for whom three readings were successfully obtained. Analyses exclude results from participants who had eaten, drunk alcohol, smoked or exercised in the 30 minutes before the measurement was taken.
CPR training
Participants were asked whether they had ever had any type of training in CPR or learned CPR either through instructor led sessions or self-instruction using DVD/online instruction. Those who reported they had CPR training were asked to provide details of the time interval since the first training, whether they had attended refresher training and the type of CPR training.
1.2.2 Definitions
Any CVD condition
Participants were classified as having 'any CVD' if they reported ever having any of the following conditions confirmed by a doctor: angina, heart attack, stroke, heart murmur, abnormal heart rhythm, or 'other heart trouble'[33].
Diabetes
Participants were classified as having diabetes if they reported a confirmed doctor diagnosis. Women whose diabetes occurred only during pregnancy were excluded from the classification. In 2018, a new question was introduced asking participants to report if they had been told they had Type 1 or Type 2 diabetes. Prior to 2018 no distinction was made between Type 1 and Type 2 diabetes in the interview.
Any CVD condition or diabetes
A summary measure of the above conditions is presented in the tables as 'any CVD condition or diabetes'.
Ischaemic heart disease (IHD)
Participants were classified as having IHD if they reported ever having angina or a heart attack confirmed by a doctor. All tables refer to ever having had the condition.
Stroke
Participants were classified as having a stroke if they reported ever having had a stroke confirmed by a doctor.
IHD or stroke
A summary measure of the above conditions is presented in the tables as 'IHD or stroke'.
Blood pressure levels classification
In accordance with guidelines on hypertension management[34] the threshold of 140/90mmHg is used to define hypertension in SheS.
Adult participants were classified into one of four groups listed below on the basis of their systolic (SBP) and diastolic (DBP) readings and their current use of anti-hypertensive medications. For the purpose of this report, the term 'hypertensive' is applied to those in the last three categories.
| Normotensive untreated | SBP below 140mmHg and DBP below 90mmHg, not currently taking medication specifically prescribed to treat high blood pressure |
|---|---|
| Hypertensive controlled | SBP below 140mmHg and DBP below 90mmHg, currently taking medication specifically prescribed to treat high their blood pressure |
| Hypertensive uncontrolled | SBP at least 140mmHg or DBP at least 90mmHg, currently taking medication specifically prescribed to treat their high blood pressure |
| Hypertensive untreated | SBP at least 140mmHg or DBP at least 90mmHg, not currently taking a drug specifically prescribed to treat their high blood pressure |
Detection, treatment and control of hypertension
In addition to the objective definition of hypertension described above, participants were defined as having self-reported doctor-diagnosed hypertension if they stated during the interview that they had been told by a doctor or nurse that they had high blood pressure.
Hypertension detection was estimated by examining the proportion of those with survey defined hypertension (SBP at least 140mmHg or DBP at least 90 mmHg or on treatment for hypertension) reporting doctor-diagnosed hypertension. Treatment rates were estimated by examining the proportion of all those defined as having survey-defined hypertension who were on treatment at the time of the survey. The control of hypertension among those on treatment for hypertension at the time of the survey was estimated by calculating the proportion with blood pressure below 140/90mmHg.
When interpreting results it should be borne in mind that although three blood pressure readings were taken, these were all on a single occasion. Clinical diagnoses of hypertension are based on sustained levels of high blood pressure rather than a single measurement.
1.3 General Health, Cvd & Diabetes
1.3.1 Self-assessed general health, adults and children, 2008 to 2019
Self-assessed 'good' or 'very good' general health in all adults has reduced from a high of 77% in 2009 to a low of 71% in 2018 and was 72% in 2019. This pattern has been similar for men and women over the time series. Self-assessed 'bad' or 'very bad' general health has remained within the range of 7-9% since 2008 (9% in 2019) for all adults. Similar patterns have been observed for men and women over the time series.
The majority of children continued to self-assess their general health to be 'good' or 'very good' in 2019 (95%). Only 1% of children self-assessed their general health to be 'bad' or 'very bad'. These levels are consistent with those recorded since 2008 (94-96% 'good' / 'very good' and 0-1% 'bad' / 'very bad'). In 2019, there was no significant difference between the proportions of boys (94%) and girls (95%) that self-assessed their general health to be 'good' or 'very good'. Table 1.1
1.3.2 Adult self-assessed general health, 2019, by age and sex
In 2019, just over seven in ten adults (72%) described their general health as 'good' or 'very good', while just under one in ten (9%) described it as 'bad' or 'very bad'. A greater proportion of men than women described their general health as 'good' or 'very good' (74% compared with 70% respectively).
The proportion of adults who assessed their general health to be 'good' or 'very good' decreased with age, from 85% among those aged 16-24 to 54% among those aged 75 and over. A reversal of this pattern was seen in the proportion that self-assessed their general health to be 'bad' or 'very bad'; increasing from 4% among those aged 16-24 to 17% of those aged 75 and over. Consistent with previous survey years, the same general patterns were evident for men and women, although women aged 16-24 were less likely to report that their health was 'good' or 'very good' than men in the same age group (80% compared with 89% respectively). Figure 1A, Table 1.2
Percentage of adults (aged 16 and over) with 'good' or 'very good' self-reported general health, 2019, by age and sex
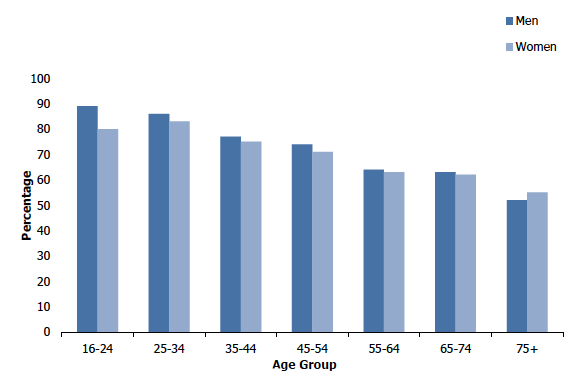
1.3.3 Adult self-assessed general health (age-standardised), 2019, by area deprivation and sex
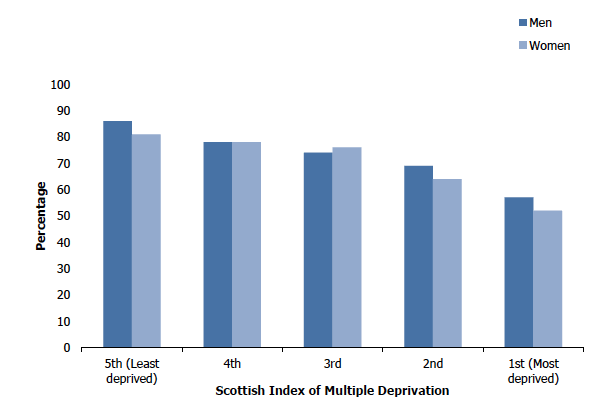
The age-standardised proportion of adults who self-assessed their general health as 'good' or 'very good' was highest (83%) for those living in the least deprived quintile and lowest (54%) for those living in the most deprived quintile. The reverse was evident for the proportion of adults who self-assessed their general health as 'bad' or 'very bad'; this was highest (20%) for those living in the most deprived quintile and lowest (4-5%) for those who lived in the two least deprived quintiles. This pattern was similar for men and women. Figure 1B, Table 1.3
Adult (aged 16 and over) self-assessed general health (age-standardised), 2019, by area deprivation and sex
1.3.4 Prevalence of long-term conditions in adults, 2019, by age and sex
Around half (47%) of adults reported living with (limiting or non-limiting) long-term conditions. The proportion of adults living with long-term conditions increased with age. Approximately three in ten (29%) of those aged 16-24 lived with long-term conditions, while more than seven in ten (73%) of those aged 75 and over lived with long-term conditions. This pattern was similar for men and women.
The majority of those with long-term conditions lived with a limiting condition. Over a third (35%) of adults lived with limiting long-term conditions with women more likely than men to do so (37% compared to 32% respectively).
The proportion of adults living with limiting long-term conditions also increased with age. Just over a fifth (22%) of those aged 16-24 lived with limiting long-term conditions, compared with almost three-fifths (58%) of those aged 75 and over. This pattern was similar for men and women. Figure 1C, Table 1.4
Percentage of adults (aged 16 and over) with long-term conditions, 2019, by age and sex
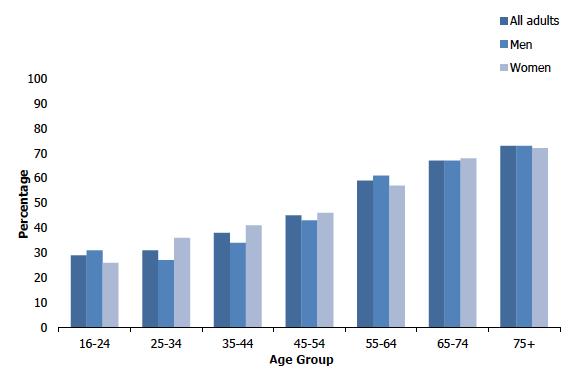
1.3.5 Trends in CVD and diabetes prevalence (age-standardised) since 2003, by area deprivation and sex
Any CVD
The extent of inequalities in age-standardised CVD prevalence by area deprivation has varied since 2003. However, since 2003, prevalence of CVD has been highest among those living in the most deprived quintile and lowest among those living in the least deprived quintile. In 2019, prevalence of CVD among those living in the most deprived quintile was 20% and between 12-16% for those living in the four other quintiles. The pattern by area deprivation was not significantly different for men and women.
Doctor-diagnosed diabetes
The prevalence of age-standardised doctor-diagnosed diabetes in 2019 was higher among those living in the most deprived quintile (10%) compared with those living in the least deprived quintile (4%). This pattern was evident for both women and men and has been consistent across previous survey years.
Ischaemic Heart Disease (IHD)
As in previous years, the prevalence of self-reported age-standardised IHD varied by area deprivation in 2019. At least twice as many adults living in the most deprived quintile reported an IHD diagnosis (10%) than those living in the least deprived quintile (4%). A similar pattern was found for men (12% compared with 6%) and for women (8% compared with 3%) in 2019. This pattern has been consistent across previous survey years.
Stroke
Stroke prevalence, for all adults and by sex, has been relatively stable
since 2008. Health inequalities by area deprivation, however, have varied in previous survey years. In 2019, there was a significant difference in stroke prevalence between the most deprived (5%) and least deprived areas (2%). A similar pattern was found among men and women.
IHD or stroke
Twice as many adults living in the most deprived areas reported an IHD or stroke diagnosis (13%) than those living in the least deprived areas (6%). This pattern has been relatively consistent across previous survey years. There was no significant difference in the pattern of IHD or stroke prevalence by deprivation for men and women in 2019. Table 1.5
1.3.6 CVD and diabetes, 2019, by age and sex
Any CVD
In 2019, 15% of adults reported having any CVD, though a higher proportion of men (17%) reported having any CVD compared with women (14%).
Having any CVD was significantly associated with age. In 2019, 4% of those aged 16-24 reported having any CVD which increased exponentially with age to 44% of those aged 75 and over. The same pattern was found for both men and women. A higher proportion of men than women reported having any CVD across all age groups.
Doctor-diagnosed diabetes
In 2019, 7% of adults reported having doctor-diagnosed diabetes; this was primarily Type 2 (6% reported Type 2 and 1% reported Type 1). There was a significant difference in prevalence of doctor-diagnosed diabetes between men (9%) and women (5%).
The prevalence of doctor-diagnosed diabetes in 2019 generally rose with age (from 1-3% among those aged 16-44 to 6-15% among those aged 45 and over). There was a significant difference in the pattern by age for men and women, driven by differences in the younger adult age groups. For women, prevalence of doctor-diagnosed diabetes rose in a clear gradient from less than 1% in women aged 16-24 to 13% among women aged 75 and over whereas for men prevalence began to increase by age only for those aged 45 and over.
Type 1 diabetes
The prevalence of Type 1 diabetes amongst all men and women was the same in 2019 (both 1%).
Type 2 diabetes
A larger proportion of men had Type 2 diabetes in 2019 than women (7% of men compared with 4% of women). Prevalence of Type 2 diabetes increased with age, from <1% for all adults aged 16-24 to 14% among those aged 75 and over. Similar patterns by age were found for men and women.
Any CVD or diabetes
A fifth of adults reported having any CVD or doctor-diagnosed diabetes in 2019, figures were slightly higher for men (22%) and lower for women (17%). Prevalence was also associated with age, ranging from 6% among those aged 16-24 to 51% of those aged 75 and over.
The pattern by age was similar for men and women, though a higher proportion of men in each age group reported having any CVD or doctor-diagnosed diabetes.
IHD
In 2019, the proportion of adults reporting an IHD diagnosis was 5%, equal to that in 2017[35] and 2018[36]. A greater proportion of men reported an IHD diagnosis (7% of men compared with 4% of women).
The proportion reporting an IHD diagnosis increased with age, from <1% among those aged 16-24 to 23% among those aged 75 and over. The increase in prevalence by age was steeper for men than for women.
Stroke
The prevalence of stroke for all adults in 2019 was 3%, the same rate for men and women. Stroke prevalence increased by age (from <1% for those aged 16-44 to 11% among those aged 75 and over). The pattern by age was similar for men and women.
IHD or stroke
The prevalence of an IHD diagnosis and / or stroke among all adults was 8% in 2019. Prevalence was higher among men (9%) than women (7%).
Prevalence of an IHD diagnosis and / or stroke increased steadily with age, from 1% or less among those aged 16-44 to 31% among those aged 75 and over. Prevalence increased with age for both men and women. Table 1.6
1.3.7 Blood pressure level, 2003 to 2018/2019 combined
To increase the sample size available, the detailed analysis of blood pressure trends since 2003 used sets of two-years of combined data from 2008/2009. Using the nurse-equivalent calibrated estimates, the combined data from 2018 and 2019 showed that 29% of adults aged 16 and over had hypertension. The nurse-equivalent calibrated estimates for all adults have remained at a similar level since 2012/2013 (28%) following a significant decrease from 33% in 2010/2011. Similar patterns were found for men and women. Since 2012/2013, the nurse-equivalent calibrated estimates for women have ranged from 26-29% and 28-32% for men.
A higher proportion of men had hypertension than women in 2018/2019 (31% compared with 26% respectively). Table 1.7
1.3.8 Detection and treatment of hypertension, 2016-2019 combined, by age and sex
To increase the sample size available, the detailed analysis of detection and treatment of hypertension, by age and sex, used data from the 2016, 2017, 2018 and 2019 surveys combined. The hypertension detection rate is the proportion of adults aged 16 and over with survey-defined hypertension who also reported doctor-diagnosed hypertension. In 2016-2019 combined, the hypertension detection level among all adults with survey-defined hypertension was 59%, the same rate for 2014-2017 combined[37].
In 2016-2019, the hypertension detection level increased significantly by age group, from 19% among adults aged 16-24 to 73% among adults aged 75 and over. A similar pattern was found for men and women.
In 2016-2019 combined, 24% of adults with survey-defined hypertension had normal blood pressure under medication (hypertension treated and controlled), while 21% of adults with survey defined hypertension were still having high blood pressure readings under medication (hypertension treated, but not controlled). Figures did not differ significantly between men and women or by age. Table 1.8
1.3.9 Adult prevalence of CPR training, length of time since original training and whether attended refresher, 2019, by age and sex
In 2019, over half of all adults (56%) reported having ever attended CPR training with no significant difference between men and women. The proportion of adults attending CPR training varied significantly by age with the highest attendance rates among those aged 45-54 (66%) and the lowest among those aged 75 and over (29%). Patterns by age were also similar for men and women.
Among those that had ever had CPR training, over three-quarters (77%) had their original training four years ago or more[38]. The likelihood of the original CPR training being four years ago or more increased with age: 95% of those aged 75 and over attended their original CPR training four years ago or more, compared with 46% of those aged 16-24. A reversal in this trend was evident for those who attended their original CPR training within the last 12 months. Among those aged 16-24, 19% had attended their first CPR training within the last 12 months compared with 1% of those aged 75 and over. Similar patterns by age were found for men and women.
Of those who had ever attended CPR training, 45% also reported attending refresher training. The proportion of adults that had attended refresher training varied by age (41-55% among those aged 16-64, compared with 27% of those 65 and over).
Among adults who had any CPR training (original or refresher), more than a third (37%) had the training within the past two years with younger adults more likely to do so than older adults. The highest proportion of any CPR training within the past two years was found among the youngest age group (aged 16-24) at 51%; the lowest (7%) was found among the oldest age group (aged 75 and over).
In 2019, a fifth (21%) of all adults reported attending any CPR training (original or refresher) within the past two years; the highest level was among the youngest age group (30%) and the lowest was among the oldest group (2%). Table 1.9
1.3.10 Adult prevalence of CPR training, length of time since original training and whether attended refresher (age-standardised), 2019, by area deprivation and sex
In 2019, the age-standardised prevalence of having ever attended CPR training was significantly associated with area deprivation. The attendance level was lowest among those living in the most deprived quintile at 43% compared with 62% of those living in the least deprived quintile. The pattern by deprivation was similar for men and women.
The length of time since original CPR training or attendance at refresher training did not differ significantly by area deprivation in 2019.
Whether any CPR training had been attended within the last two years was lowest for those living in the more deprived quintiles (29% in the 1st and 2nd most deprived quintiles compared to 34-40% in the remaining quintiles).
Of all adults, the proportion reporting having attended any CPR training (original or refresher) within the last two years also differed by deprivation with those living in the 1st and 2nd most deprived areas less likely to have done so than those in the remaining quintiles (13-18% compared with 23-26% respectively).
Patterns by deprivation did not differ between men and women. Table 1.10
1.3.11 Type of CPR training last attended, 2019, by age and sex
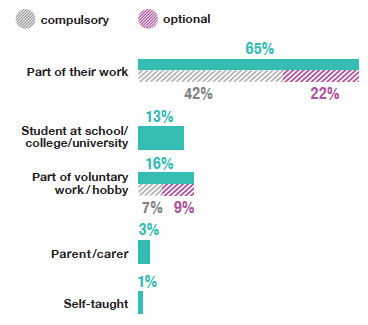
In 2019, of the adults who had ever attended CPR training, almost two-thirds (65%) last attended CPR training as part of their work; either as a compulsory part of their work (42%) or they had opted to take the training as part of their work (22%). A further 13% of adults last attended CPR training whilst they were a student as part of school / college / university work. For 7%, CPR training was a compulsory part of voluntary work or a hobby and a further 9% opted to attend CPR training as part of voluntary work or a hobby. In addition, 3% of adults last attended CPR training because they were a parent or carer. Finally, 1% of those that had attended CPR training taught themselves from a book, the internet or another self-learning tool.
Those aged 16-24 were less likely than those in older age groups to have attended CPR training as a compulsory part of their work (22% among those aged 16-24 compared with 39-49% among those aged 25 and over). Those aged 16-24 were also less likely than older age groups to have opted to do CPR training as part of their work (6% compared with 19-29% among those aged 25 and over). For those aged 25 and over, attending CPR training as a compulsory part of their work was the most common reason for last attending CPR training, followed by opting to attend as part of their work. These patterns were similar for men and women.
Over half (51%) of those aged 16-24, last attended CPR training whilst they were a student as part of school / college / university work (compared with 1-19% of other age groups). This pattern was evident for men and women. Table 1.11
Table List
Table 1.1 Self-assessed general health, adults and children, 2008 to 2019
Table 1.2 Adult self-assessed general health, 2019, by age and sex
Table 1.3 Adult self-assessed general health (age-standardised), 2019, by area deprivation and sex
Table 1.4 Prevalence of long-term conditions in adults, 2019, by age and sex
Table 1.5 Trends in CVD and diabetes prevalence (age-standardised) since 2003, by area deprivation and sex
Table 1.6 CVD and diabetes, 2019, by age and sex
Table 1.7 Blood pressure level, adults, 2003 to 2018/2019 combined
Table 1.8 Detection and treatment of hypertension, 2016-2019 combined, by age and sex
Table 1.9 Adult prevalence of CPR training, length of time since original training and whether attended refresher, 2019, by age and sex
Table 1.10 Adult prevalence of CPR training, length of time since original training and whether attended refresher (age-standardised), 2019, by area deprivation and sex
Table 1.11 Type of CPR training last attended, 2019, by age and sex
The tables can be found on the main report page under supporting files: https://www.gov.scot/publications/scottish-health-survey-2019-volume-1-main-report/
References and notes
1. Vaillant, N and Wolff, FC (2012). On the reliability of self-reported health: Evidence from Albanian Data. Journal of Epidemiology and Global Health; 2(2): 83-98.
2. The Scottish Government (2018). Public Health Priorities for Scotland. [Online] Available from:https://www.gov.scot/binaries/content/documents/govscot/publications/corporate-report/2018/06/scotlands-public-health-priorities/documents/00536757-pdf/00536757-pdf/govscot%3Adocument/00536757.pdf
3. COSLA and the Scottish Government (2020). The reform programme: why reform is important. [Online] Available from: https://publichealthreform.scot/the-reform-programme/why-reform-is-important
4. World Health Organization (2018). Mental Health: strengthening our response. [Online] Available from: https://www.who.int/news-room/fact-sheets/detail/mental-health-strengthening-our-response
5. The Scottish Executive. (2007). All Our Futures: Planning for a Scotland with an Ageing Population. [Online]. Available from:
http://www.laterlifetraining.co.uk/wp-content/uploads/2011/12/AllOurFutures_Vol3_ScottExec.pdf
6. Heart Disease Improvement Plan. Edinburgh: Scottish Government, (2014). Available from: https://www.gov.scot/publications/protecting-scotland-renewing-scotland-governments-programme-scotland-2020-2021/
7. Stroke Improvement Plan, Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/publications/stroke-improvement-plan/
8. Information Services Division (2020). Scottish Heart Disease Statistics. Available from: https://beta.isdscotland.org/find-publications-and-data/conditions-and-diseases/heart-disease-and-blood-vessels/heart-disease-statistics/
9. Information Services Division (2020). Scottish Stroke Statistics. [Online]. Available from:
https://beta.isdscotland.org/media/3311/2020-01-28-stroke-report.pdf
10. Information Services Division (2020). Scottish Heart Disease Statistics. Available from: https://beta.isdscotland.org/find-publications-and-data/conditions-and-diseases/heart-disease-and-blood-vessels/heart-disease-statistics/
11. National Records of Scotland (2018). Vital Events Reference Tables 2018. [Online]. Available from: https://www.nrscotland.gov.uk/statistics-and-data/statistics/statistics-by-theme/vital-events/general-publications/vital-events-reference-tables/2018/section-6-death-causes
12. Scottish Diabetes Data Group, NHS Scotland (2018). Scottish Diabetes Survey 2018. [Online] Available from: https://www.diabetesinscotland.org.uk/wp-content/uploads/2019/12/Scottish-Diabetes-Survey-2018.pdf
13. The Scottish Government. (2020). Scottish Out-of Hospital Caridac Arrest data linkage
project: 2018-2019 results. [Online] Available at: https://www.gov.scot/publications/scottish-out-hospital-cardiac-arrest-data-linkage-project-2018-19-results/
14. The Scottish Government. (2015). Out-of-hospital cardiac arrest: a strategy for Scotland. [Online]. Available from: https://www.gov.scot/binaries/content/documents/govscot/publications/strategy-plan/2015/03/out-hospital-cardiac-arrest-strategy-scotland/documents/out-hospital-cardiac-arrest-strategy-scotland/out-hospital-cardiac-arrest-strategy-scotland/govscot%3Adocument/00474154.pdf
15. The Scottish Government. (2015). Out-of-hospital cardiac arrest: a strategy for Scotland. [Online]. Available from: https://www.gov.scot/binaries/content/documents/govscot/publications/strategy-plan/2015/03/out-hospital-cardiac-arrest-strategy-scotland/documents/out-hospital-cardiac-arrest-strategy-scotland/out-hospital-cardiac-arrest-strategy-scotland/govscot%3Adocument/00474154.pdf
16. A National Clinical Strategy for Scotland, Edinburgh: Scottish Government, 2016. Available from: https://www.gov.scot/publications/national-clinical-strategy-scotland/
17. Health and social care delivery plan: progress report. Edinburgh: Scottish Government, 2019. Available from: https://www.gov.scot/publications/health-social-care-delivery-plan-progress-report/
18. Practising Realistic Medicine, Edinburgh, Scottish Government, 2018.Available from:https://www.gov.scot/publications/practising-realistic-medicine/
19. Realising Realistic Medicine, Edinburgh: Scottish Government, 2017. Available from: https://www2.gov.scot/Resource/0051/00514513.pdf
20. Public Health Priorities for Scotland, Edinburgh: Scottish Government/COSLA, 2018. Available from: https://www.gov.scot/publications/scotlands-public-health-priorities/pages/9/
21. Improving the Health and Wellbeing of People with Long Term Conditions in Scotland: A National Action Plan (2009). Edinburgh: Scottish Government. Available from: https://www.sehd.scot.nhs.uk/mels/CEL2009_23.pdf
22. Heart Disease Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/Publications/2014/08/5434/0
23. Stroke Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/Publications/2014/08/9114/0
24. Diabetes Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: www.gov.scot/Publications/2014/11/6742
25. The Scottish Government. (2018). Scotland's public health priorities. [Online] Available from: https://www.gov.scot/publications/scotlands-public-health-priorities/pages/4/
26. The Scottish Government. Health. [Online]. Available from: https://nationalperformance.gov.scot/national-outcomes/health
27. A Healthier Future: Scotland's Diet and Healthy Weight Delivery Plan (2018) Edinburgh: Scottish Government, 2018. Available from: https://www.gov.scot/publications/healthier-future-scotlands-diet-healthy-weight-delivery-plan/
28. A more active Scotland: Scotland's Physical Activity Delivery Plan. Edinburgh: Scottish Government. 2018. Available from: http://www.gov.scot/Resource/0053/00537494.pdf
29. Hauner H (2010). Obesity and diabetes. in Holt RIG, Cockram CS, Flyvbjerg A et al (ed.) Textbook of diabetes. 4th edition.
30. Out of Hospital Cardiac Arrest: A Strategy for Scotland (2015). Edinburgh: Scottish Government. Available from: http://www.gov.scot/Resource/0047/00474154.pdf
31. For a detailed description of the biological module see Volume 2 of this report
33. Diabetes and high blood pressure are not included in the definition of 'any CVD condition' as they are risk factors for CVD.
34. Ramsay, L.E., Williams, B., Johnston, G.D., MacGregor, G.A., Poston, L., Potter, J.F., Poulter, N.R. and Russel, G. (1999). Guidelines for management of hypertension: report of the Third Working Party of the British Hypertension Society, 1999. Journal of Human Hypertension. 13:569-592.
35. Feng, Q. (2017). Chapter 2: General Health, Long Term Conditions and Cardiovascular Diseases. McLean, J., Dean, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/6/
36. Wilson, V. (2018). Chapter 2: General Health, Cardiovascular Diseases and Caring. McLean, J. Dean, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from:
https://www.gov.scot/publications/scottish-health-survey-2018-volume-1-main-report/
37. Feng, Q. (2017). Chapter 2: General Health, Long Term Conditions and Cardiovascular Diseases. McLean, J., Christie, S., Hinchliffe, S.(eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/6/
38. A change in the time periods for the CPR training questions was introduced in 2019 in order to enable measurement of the number of people trained since the Out of Hospital Strategy was published, Therefore, the data is not comparable with that collected in 2017.
Contact
There is a problem
Thanks for your feedback