Scottish Health Survey 2019 - volume 1: main report
Presents results for the Scottish Health Survey 2019, providing information on the health and factors relating to health of people living in Scotland.
This document is part of a collection
Chapter 3: Dental Health
In 2019, the majority of adults in Scotland had some natural teeth while a small proportion had no natural teeth.
- 7% no natural teeth
- 93% some natural teeth
More than three quarters of adults, 78%, had 20 or more natural teeth.
Natural teeth prevalence reduced with age from almost all adults aged 16–54 having some natural teeth to 71% of those aged 75 and over.
- 16-24 - 100%
- 25-34 - 100%
- 35-44 - 99%
- 45-54 - 97%
- 55-64 - 93%
- 65-74 - 82%
- 75+ - 71%
In 2019, most adults in Scotland reported having no issues with their mouth, teeth or dentures.
- 9% any issues reported
- 91% no issues reported
The most common issues adults had with their mouth, teeth or dentures were:
- 6% eating food
- 4% smiling, laughing and showing teeth without embarrassment
- 2% speaking clearly
- 1% emotional stability, such as becoming more easily upset than usual
- <1% affecting their enjoyment of the company of other people
In 2019, adults who had any issues with their mouth, teeth or dentures had lower mental wellbeing (mean WEMWBS score) than those who had no such issues.
- any issues 44.6
- no issues 50.3
3 Dental Health
3.1 Introduction
In most industrialised countries between 60-90% of school children and the vast majority of adults have tooth decay[1]. The most common types of oral disease are tooth decay and gum disease. As tooth decay is so widespread and is largely preventable, it is considered a public health issue. It is now widely recognised that a healthy mouth has a significant impact on physical health as well as on other aspects of day-to-day life including engaging with others socially and as a result, may have wider socio-economic consequences[2].
Oral cancer is the oral condition of greatest concern due to its seriousness and increasing incidence[3]. Head and neck cancer, of which oral cancer and oropharyngeal cancer are types, account for around 3% of total cases of cancer in the UK[4]. Around 530 people are diagnosed with oral cancer per year in Scotland; this is twice the rate found in England and Wales[5]. Major risk factors for oral cancer include tobacco use, excessive alcohol consumption[6] and low fruit and vegetable intake[7] and as a result, incidence is higher in men and older age groups[8].
Child and adult dental registration rates have continued to grow in recent years; 96% of the Scottish population was registered with a dentist as at 30 September 2019 with rates similar among children and adults (94% and 96%, respectively). Around 7 in 10 patients registered with an NHS dentist had visited their dentist in the previous 2 years with children more likely to have done so than adults (84% and 65% respectively)[9].
The cost of provision of General Dental Services and Public Dental Service increased between 2017/18 and 2018/19 by 3%[10], reflecting the increase in demand, an ageing population and the increase in people retaining their teeth[11]. Further improvements to oral health are evidenced by the findings of the Detailed Inspection Programme of Primary 7 children in 2019 which found that 80% of P7 children had no obvious signs of tooth decay in their permanent teeth; a significant increase from 53% in 2005[12].
While overall progress has been made, inequalities by age and deprivation remain. It is estimated that one in five residents of Scotland aged 75 or over are not registered with an NHS dentist[13]. In addition, as of September 2019, 72% of adults in the least deprived areas in Scotland had visited an NHS dentist in the last two years compared to 61% in the most deprived areas (89% and 79% amongst children)[14]. Also 88% of P7 children living in the least deprived areas had no obvious tooth decay experience compared to only 70% of P7 children living in the most deprived areas[15].
3.1.1 Policy background
Protecting Scotland's Future: The Government's Programme for Scotland 2020-21[16] reaffirms the government's commitment to accelerate the reform programme for NHS dental services and introduce a new model of preventive oral health care for adult patients. Patients will receive a comprehensive assessment of their oral health, including gums, tooth decay and soft tissues, and along with lifestyle risk factors such as smoking and alcohol, will receive an appropriate treatment plan. The intervention could be either preventive, self‑care or restorative.
These commitments continue to pursue the general objectives set out in the Oral Health Improvement Plan[17], which was published in January 2018 following extensive consultation with professionals and the public. The plan recognises the link between oral health and other public health problems, such as poor diet as well as smoking and alcohol consumption. It sets out strategies to improve the oral health of the population and to provide high quality NHS dental services under a new model of care that was reflective of the NHS dental service before COVID-19 and for the adult population. The plan proposed a move away from restorative dentistry to a preventative mode, with recognition of the impact that poor oral health can have on overall quality of life, as well as health behaviours and health status.
The Oral Health Improvement plan has several aims including:
- Developing a preventative model for oral healthcare
- Reducing oral health inequalities
- Meeting the needs of an ageing population
- Providing more services on the high street
- Improving information for patients
- Increasing quality assurance and improvement
- Developing and enhancing the dental workforce
The New Model of Care was developed during 2019 through a collaborative approach between government and a range of dental interests, including academic and clinical. The main focus of this activity was to develop the preventive policy, centred around the Oral Health Assessment, which provides for an assessment of general oral health alongside wider health risks such as smoking and alcohol. The NHS offer for restorative dentistry was taking an early look at the general framework around which the new system would deliver packages of treatment, as required for each individual patient.
The COVID-19 pandemic has meant that the preparation of the New Model of Care was paused as the government focused on the public health issue. Further development of the New Model of Care will be considered to reflect the requirements of the NHS dental service in the longer term to ensure that preventive care is at the centre of the NHS dentistry.
Prevention
Childsmile[18] is a preventative programme that encourages tooth brushing and fluoride varnish application in nursery and primary school age children while also aiming to reduce inequalities in dental health and access to dental services. This programme also distributes toothpaste and brushes for home use and involves dental practices providing preventative care for children such as supervised brushing in nurseries for 3-4 year olds. The Oral Health Improvement Plan aims to ensure that good habits learned through Childsmile are maintained throughout childhood and into adulthood. This aim is further supported by a preventative care programme for adults with personalised care plans based on the degree of risk of developing oral cancer, gum disease and decay due to lifestyle factors such as diet, alcohol consumption and smoking status.
Reducing oral health inequalities
Despite encouraging progress in overall levels of dental health, higher levels of decay are still recorded amongst children living in the most deprived communities in Scotland compared with those in the least deprived[19]. The Oral Health Improvement Plan will ensure that community-level interventions form a significant part of the overall approach to addressing health inequalities as a means to engage 'hard-to-reach' groups. Further, the plan will ensure that practitioners working in deprived areas have appropriate payments and allowances to reflect the needs of their patients. This will encourage dental practices to continue to provide care to patients in areas of greatest oral health need, such as those with a high degree of deprivation.
Meeting the needs of an ageing population
Over the next ten years the number of people over 75 is projected to increase by 25%[20]. The increasingly ageing population, combined with more adults retaining some or all of their natural teeth, is likely to mean there will be a significant increase in people requiring domiciliary dental care, either in their own home or in residential care. The Oral Health Improvement Plan aims to provide a greater system of care for those in care homes. In addition to the arrangements implemented to facilitate dental services in care homes, there are plans to extend this to people who are cared for in their own homes[21].
Providing more services on the high street
This aim is to ensure that patients are treated in the appropriate setting i.e. within Hospital Dental Services (HDS) or by General Dental Practitioners (GDPs). This involves obtaining adequate data on primary-secondary care pathways as well as ensuring that GDPs are trained and accredited to deliver a wide range of treatments such as some oral surgeries and intravenous sedations.
Improving information for patients
By way of recognition that the public do not consider themselves to have enough information about oral services available from the NHS and the associated costs, action is being taken to ensure that this information is made available and that it is streamlined across all GDPs. This includes the engagement of groups including those not currently attending check-ups, living in deprived areas and/or engaging in risk related behaviours (smoking, drinking heavily etc.).
Quality assurance and improvement
The aim is to enhance and improve service delivery, scrutiny and quality assurance in NHS dental care through a number of actions including introducing a Director of Dentistry in each Health Board area to drive national policy and provide assurance at a local level and developing a single database for quality improvement information for NHS Boards. Much of this work will build on Building a comprehensive approach to reviewing the quality of care: Supporting the delivery of sustainable high-quality services which established the need to develop a new framework in dentistry that will improve care within practices, NHS Boards and nationally[22].
Workforce
The NHS dental practitioner workforce has increased significantly over the past ten years, with a 12% increase from 3,227 dentists in 2010 to 3,603 in 2018[23]. The plan sets out the need for the workforce to continuously develop and adapt with an emphasis on working within a healthcare setting which promotes prevention, and which needs to adapt to the increased demands as a result of an increase in the older population people.
3.1.2 Reporting on dental health in the Scottish Health Survey (SHeS)
This chapter presents findings on the prevalence of natural teeth in the Scottish population in 2019 by age and sex. Additionally, the impacts of issues with the mouth, teeth or dentures on daily life and mental health are reported.
Supplementary tables are also available on the Scottish Government SHeS website https://www.gov.scot/collections/scottish-health-survey/
3.2 Methods and Definitions
Adults aged 16 and over are asked questions on dental health annually and on dental health services and actions taken to improve dental health biennially. This report presents data for 2019 only, however, it is important to be aware when referring to data in previous reports that several changes were made to the questions on dental health prior to 2008. More information about the changes made in 2008 is provided in the 2008 and subsequent reports[24]
3.3 Dental Health
3.3.1 Number of natural teeth/no natural teeth (adults), 2019, by age and sex
In 2019, the vast majority (93%) of adults in Scotland had at least some natural teeth whilst 7% had none. More than three in four adults (78%) had 20 or more natural teeth.
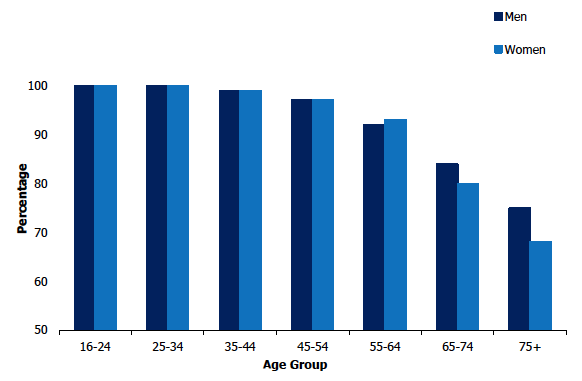
As noted in previous SHeS reports, natural teeth prevalence was significantly associated with age. Almost all adults (97-100%) aged 16-54 reported having at least some natural teeth, prevalence then decreased by age group to 71% among those aged 75 and over.
There was no significant difference in natural teeth prevalence by sex with similar patterns by age for both sexes. Figure 3A, Table 3.1
Percentage of adults with any natural teeth, 2019, by age and sex
3.3.2 Issues with mouth, teeth or dentures, 2019, by age and sex
In 2019, most adults (91%) in Scotland reported having no issues with their mouth, teeth or dentures whilst 9% reported having issues.
Prevalence of having issues with mouth, teeth or dentures did not vary significantly with age.
The most common issue reported with mouth, teeth and dentures was eating food: 6% of adults in Scotland had this issue. The second most common was issues with smiling, laughing and showing teeth without embarrassment (4%) followed by issues with speaking clearly (2%) and then issues with emotional stability, such as becoming more easily upset than usual (1%). Less than 1% of adults reported that having issues with their mouth, teeth or dentures affected their enjoyment of the company of other people.
Sex was not a significant determinant of issues with mouth, teeth or dentures among adults of any age. Table 3.2
3.3.3 Adult WEMWBS mean score (age-standardised), 2019, by issues with mouth, teeth or dentures, and sex
In 2019, adults who had any issues with their mouth, teeth or dentures had lower mental wellbeing than those who had no such issues as measured by age-standardised mean WEMWBS scores (44.6 compared with 50.3 respectively). As shown in Figure 3B, this was the case for both men and women.
Adult WEMWBS mean score (age-standardised), 2019, by issues with mouth, teeth or dentures, and sex
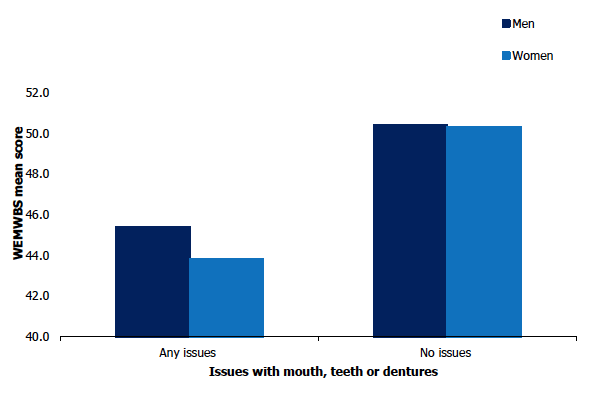
Although not statistically significant, having issues with mouth, teeth or dentures appeared to have had a greater negative impact on the mental wellbeing of women than men; the WEMWBS mean score for women with any issues with their mouth, teeth or dentures was 43.8 compared with 45.4 for men. Figure 3B, Table 3.3
Table List
Table 3.1 Number of natural teeth/no natural teeth (adults), 2019, by age and sex
Table 3.2 Issues with mouth, teeth or dentures, 2019, by age and sex
Table 3.3 Adult WEMWBS mean score (age-standardised), 2019, by issues with mouth, teeth or dentures and sex
The tables can be found on the main report page under supporting files: https://www.gov.scot/publications/scottish-health-survey-2019-volume-1-main-report/
References and Notes
1. World Health Organisation (2012). What is the burden of oral disease? [Online]. Available from: https://www.who.int/oral_health/disease_burden/global/en/
2. Oral Health Improvement Plan. Edinburgh: Scottish Government. 2018. Available from: https://www.gov.scot/publications/oral-health-improvement-plan/
3. Annual Report of the Chief Dental Officer 2012 – A picture of Scotland's Oral Health. Edinburgh: Scottish Government, 2013. Available from: https://www.gov.scot/publications/annual-report-chief-dental-officer-2012/
4. Cancer Research UK (2015). Head and neck cancers incidence statistics. [Online]. Available from: https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/head-and-neck-cancers/incidence
5. Scottish Dental. Mouth (Oral) cancer. [Online]. Available from: https://www.scottishdental.org/library-dental-topics/mouth-oral-cancer/
6. Cancer Research UK (2018). Mouth and oropharyngeal cancer: risks and causes. [Online]. Available from: https://www.cancerresearchuk.org/about-cancer/mouth-cancer/risks-causes
7. Scottish Dental. Mouth (Oral) cancer. [Online]. Available from: https://www.scottishdental.org/library-dental-topics/mouth-oral-cancer/
8. Cancer Research UK (2019). Head and neck cancers incidence statistics. [Online]. Available from: https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/head-and-neck-cancers/incidence
9. Public Health Scotland. Dental Statistics – registration and participation. [Online]. Available from: https://beta.isdscotland.org/find-publications-and-data/health-services/primary-care/dental-statistics-registration-and-participation/
10. Information and Statistics Division (2019). Primary Care Dentistry in Scotland: Annual Report 2018/19. [Online]. Available from: https://www.shsc.scot/media/61224/2019-11-26-sdpb-report.pdf
11. Oral Health Improvement Plan. Edinburgh: Scottish Government. 2018. Available from: https://www.gov.scot/publications/oral-health-improvement-plan/
12. ISD (2019). Scotland National Dental Inspection Programme. [Online]. Available from: https://www.isdscotland.org/Health-Topics/Dental-Care/Publications/2019-10-22/2019-10-22-NDIP-Report.pdf
13. Oral Health Improvement Plan. Edinburgh: Scottish Government. 2018. Available from: https://www.gov.scot/publications/oral-health-improvement-plan/
14. Public Health Scotland. Dental Statistics – registration and participation. [Online]. Available from: https://beta.isdscotland.org/find-publications-and-data/health-services/primary-care/dental-statistics-registration-and-participation/
15. ISD Scotland National Dental Inspection Programme (2019). Available from: https://www.isdscotland.org/Health-Topics/Dental-Care/Publications/2019-10-22/2019-10-22-NDIP-Report.pdf
16. Protecting Scotland, Renewing Scotland: The Government's Programme for Scotland 2020-2021, p. 72 [Online]. Available from: https://www.gov.scot/publications/protecting-scotland-renewing-scotland-governments-programme-scotland-2020-2021/
17. Oral Health Improvement Plan. Edinburgh: Scottish Government. 2018. Available from: https://www.gov.scot/publications/oral-health-improvement-plan/
18. See: http://www.child-smile.org.uk/
19. ISD (2019). Scotland National Dental Inspection Programme. [Online]. Available from: https://www.isdscotland.org/Health-Topics/Dental-Care/Publications/2019-10-22/2019-10-22-NDIP-Report.pdf
20. National Records of Scotland. Population Projections for Scottish Areas (2018-based). [Online]. Available from: https://www.nrscotland.gov.uk/statistics-and-data/statistics/statistics-by-theme/population/population-projections/sub-national-population-projections/2018-based/
21. Scottish Government. Primary care services. [Online]. Available from: https://www.gov.scot/policies/primary-care-services/dentistry-and-oral-health/
22. Healthcare Improvement Scotland - Building a comprehensive approach to reviewing the quality of care: Supporting delivery of sustainable high quality services (2016). Available from: http://www.healthcareimprovementscotland.org/our_work/governance_and_assurance/quality_of_care_approach/design_panel_final_report.aspx
23. ISD (2018). Scotland NHS Dental Workforce Statistics. General Dental Service, Public Dental Service and Hospital Dentists. [Online]. Available from: https://www.gov.scot/publications/scottish-health-survey-2008/
Contact
There is a problem
Thanks for your feedback