Scottish Health Survey 2019 - volume 1: main report
Presents results for the Scottish Health Survey 2019, providing information on the health and factors relating to health of people living in Scotland.
This document is part of a collection
Chapter 4: Alcohol
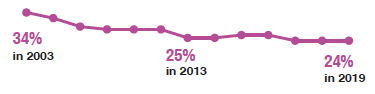
Following a significant decrease in prevalence of hazardous or harmful drinking between 2003 and 2013, prevalence for all adults has remained relatively stable.
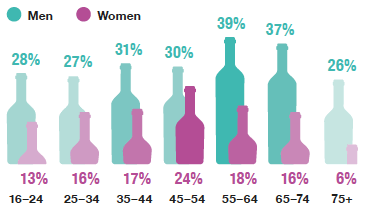
The highest prevalence of hazardous or harmful drinking for men was among those aged 55–64 and for women among those aged 45–54.
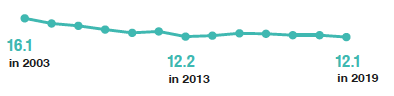
The mean number of units of alcohol consumed per week by adults has decreased over the time series to its lowest so far in 2019*.
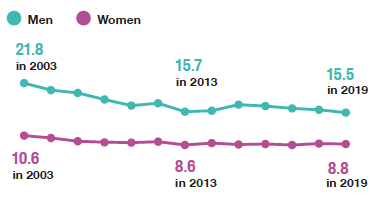
Since 2003, the mean number of units consumed per week among both men and women has decreased, with the 2019 mean the lowest in the time series for men.
* Although not significantly different from 2018.
In 2019, the highest proportion of adult nondrinkers was in the most deprived areas and the lowest was in the least deprived areas.
In 2019, prevalence of hazardous, harmful or possibly dependent drinking behaviour (AUDIT scores of 8 or more) was higher for men than for women.
- 17% All adults
- 23% Men
- 11% Women
Among all children in 2017/2019 combined:
17% were living with at least one parent who exhibited hazardous, harmful drinking behaviour or had a possible alcohol dependence (AUDIT score of 8 or more)
2% were living with at least one parent who exhibited harmful drinking behaviour or who had a possible alcohol dependence (AUDIT score of 16 or more)
83% did not live in a household with a parent who exhibited hazardous, harmful drinking behaviour or who had a possible alcohol dependence
4 Alcohol
4.1 introduction
Harmful alcohol consumption has been recognised as a major, long-lasting public health challenge in Scotland. Harmful drinking carries with it a risk of physical and mental health problems, as well as social and economic losses to individuals and society[1]. Excessive alcohol consumption at a chronic level results in increased risk of high blood pressure, chronic liver disease and cirrhosis, pancreatitis, some types of cancer, mental ill-health and accidents[2]. Recent evidence has also established links between harmful drinking and the incidence of infectious diseases such as tuberculosis and HIV/AIDS[3].
According to the most recent World Health Organisation (WHO) data (2016), harmful alcohol use is the seventh leading risk factor for premature death and disability and the highest risk factor among the population of 15-49 year olds worldwide[4], with 3 million deaths (5.3% of all deaths) worldwide the result of the harmful use of alcohol in 2016. Death and disability caused by alcohol consumption can occur relatively early in life with 13.5% of the total deaths among those aged 20-39 being alcohol-attributable as well as 7.2% of all premature deaths (among those aged 69 years and younger). The leading contributors to alcohol-attributable deaths were digestive diseases (21.3%), unintentional injuries (20.9%) and cardiovascular diseases and diabetes (19%)[5].
In 2019, 9.9 litres (L) of pure alcohol were sold per adult in Scotland (same as in 2018), equivalent to 19.1 units per adult per week, representing enough alcohol for every adult to substantially (by 36%) exceed the low risk weekly drinking guideline (14 units); 23% of off-trade alcohol sold was on promotion in 2019, a decrease from 55% in 2011. The 9.9 litres of pure alcohol per adult represents a 3% decrease from 2017 (10.2 litres) and is the lowest level seen since in Scotland since 1994. As in 2018, the volume of alcohol sold in Scotland in 2019 was 9% higher than in England & Wales which is the smallest difference since 2004[6].
In 2018, alcohol mortality in Scotland increased by 1% compared with the previous year, with 1,136 alcohol-specific deaths in 2018, up from 1,120 in 2017. This represents an average of 22 deaths per week, and it is still more than three times the number of alcohol-specific deaths in the early 1980s. The number of alcohol-specific deaths was more than twice as high among men than women in 2018 in Scotland[7]. In 2018/19, alcohol-related problems resulted in 35,685 stays in general acute hospitals and while the rate has declined over the past 10 years (at its lowest in 2018/19 – 668.8 per 100,000 population), it was still over four times higher in 2018/19 than in 1981/82[8].
Alcohol-related morbidity and mortality are not evenly distributed throughout the population and the burden is greatest among those living in the most deprived areas[9],[10]. The rate of alcohol-specific mortality among those aged 45-74 years in Scotland's most deprived areas in 2018 was 5 times higher than in the least deprived areas (93.1 compared with 18.6 per 100,000 population). Since it was first measured in 1997, the largest gap in alcohol-specific mortality rates between those living in the most and least deprived areas of Scotland was recorded in 2002 (184.7 per 100,000). Since then, this gap has fluctuated between 72.8 and 167.4 per 100,000, with 2018 (74.5 per 100.000) the third lowest gap in this time series[11]. Alcohol-related admissions to general hospitals are also linked to deprivation with seven times as many stays (per 100,000 population) with at least one alcohol-related admission from the most deprived areas compared to the least deprived areas in 2018/19. In the psychiatric setting the difference was more pronounced. In 2018/19, the stay rates in the most deprived areas of Scotland were 13 times higher than those in the least deprived areas (154 compared to 12 per 100,000 population)[12].
Harmful alcohol use carries considerable economic costs; in 2010 the Scottish Government estimated that the excessive consumption of alcohol in Scotland costs £3.6 billion a year, equivalent to £900 per adult[13]. This was estimated to include £267 million to the NHS, £209 million to social care services and £727 million to the justice system.
4.1.1. Policy background
Being 'healthy and active' is recognised as one of the National Outcomes underpinning the Scottish Government's revised National Performance Framework to improve the wellbeing and quality of life of people in Scotland[14]. Tackling harmful alcohol use is integral to ensuring that people in Scotland are healthy and to reducing social inequalities. The government's commitment to addressing harmful alcohol consumption is evidenced by the inclusion of a National Performance Framework National Indicator to 'reduce the proportion of people with multiple health risk behaviours'[15].
The UK Chief Medical Officers (CMOs) published new guidelines on alcohol consumption in January 2016, advising both men and women that it is safest not to regularly consume more than 14 units of alcohol per week. This represented a reduction in the low risk guidelines for men. Advice was also included to spread the amount drunk over a number of days and limit the amount consumed in a single session[16].
Following the Alcohol (Minimum Pricing) (Scotland) Act 2012 the Scottish Government introduced a statutory minimum price of 50 pence for a unit of alcohol, below which it cannot be sold. This was considered to provide a proportionate response to tackling harmful alcohol use whilst providing a reasonable balance between public health and social benefits and intervention in the market. It is estimated that twenty years after implementation of the policy, when it is considered to have reached full effectiveness, there would be around 120 fewer alcohol-related deaths per annum and around 2,000 fewer hospital admissions per annum[17].
Before Minimum Unit Pricing (MUP)[18] was introduced in Scotland on 1 May 2018, it was possible to exceed the low risk guidelines for alcohol (14 units per week) for around £2.50; whereas, with the 50 pence minimum unit price, that figure rose to at least £7[19]. In 2019, alcohol sold in the UK was 75% more affordable than it was in 1987[20].
The impact of Minimum Unit Pricing is subject to a comprehensive evaluation undertaken by Public Health Scotland over five years with a final report due in 2023. The evaluation has four outcome areas: implementation and compliance; alcohol market; consumption; and health and social harms. Some reports in these outcomes have been published[21].
One of the reports, which was published on 10 June 2020, was a statistical analysis of 12 months off-trade alcohol sales following the introduction of Minimum Unit Pricing. This showed that the introduction of Minimum Unit Pricing in Scotland was associated with a net reduction in per adult off-trade alcohol sales of between 4% and 5% in Scotland in the 12 months following the implementation of MUP[22]. Another report published in May 2020 concluded that the available evidence so far strongly suggests Minimum Unit Pricing has reduced alcohol consumption in Scotland[23].
It is too early to assess the impact of this reduced consumption on alcohol harms as this will take longer to feed through.
The annual Monitoring and Evaluating Scotland's Alcohol Strategy (MESAS) Report includes headline statistics for high-level indicators relevant to Scotland's alcohol strategy Alcohol Framework 2018: Preventing Harm[24]. The most recent report was published in June 2020[25]. The Alcohol Framework 2018 endorses the WHO Safer initiative of five evidence-based strategies that WHO recommends governments should prioritise to tackle alcohol alcohol-related harm[26]. It continues to take an evidence-based approach to tackling the three central themes of Scotland's 2009 alcohol strategy; reducing consumption; positive attitudes, positive choices and supporting families and communities. The key actions for the next few years are to:
- Put the voices of young people at the heart of developing preventative measures on alcohol
- Reduce alcohol consumption through affordability and sales and review the Minimum Unit Price of 50 pence two years after implementation
- Keep the licensing system under review to ensure it can deliver for public health
- Consult on marketing restrictions to protect children and young people from alcohol marketing
- Press the UK Government to improve measures to protect children and young people from exposure to alcohol marketing
- Improve the programme of substance use education in schools
- Continue to raise awareness of the UK CMO guidelines and the harmful effects of alcohol
- Review evidence on alcohol brief interventions to ensure they are being carried out in the most effective manner.
4.1.2. Measuring alcohol consumption in surveys
The alcohol consumption estimates discussed in this chapter are based on self-reported data collected during the survey interview. It is, however, important to note that surveys consistently obtain lower consumption estimates than those implied by alcohol sales or tax revenue data. This discrepancy can largely be explained by participants' under-reporting of consumption, due in part to a lack of accounting for atypical/special occasion drinking[27], and there is also some evidence that survey non-responders are more likely than responders to engage in hazardous alcohol use among other risky health behaviours[28],[29],[30] . The most recently available annual estimates of alcohol sales in Scotland show that 9.9 litres (19.1 units per adult per week) of pure alcohol per person aged 16 years and over were sold in 2019 (the equivalent figure for England and Wales in 2019 was 9.1 litres (17.5 units per adult per week)[31].
While self-reported survey estimates of consumption are typically lower than estimates based on sales data, surveys provide valuable information about the social patterning of individuals' alcohol consumption. Findings from the Scottish Health Survey (SHeS) are used in the MESAS evaluation of the Alcohol Framework and in the modelling of estimated impact of minimum unit pricing on consumption patterns across different groups in society.
4.1.3. Reporting on alcohol consumption in the Scottish Health Survey (SHeS)
Key trends and breakdowns for weekly and daily alcohol consumption are updated and presented in this chapter. For weekly consumption, categories are based on the revised guidelines; hence all weekly consumption category figures for men, going back to 2003, have been revised. Figures for mean consumption are presented for drinkers only. Problem drinking including levels of alcohol dependency and high risk alcohol use, as measured by the Alcohol Use Disorders Identification Test (AUDIT), are also presented as well as figures for children living with a parent with medium or high levels of alcohol problems.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on alcohol consumption are also published on the Scottish Government SHeS website https://www.gov.scot/collections/scottish-health-survey/
4.1.4 Comparability with other UK statistics
The Health Surveys for England and Northern Ireland and the National Survey for Wales all provide estimates for alcohol consumption. A report published by the Government Statistical Service in 2016 advised that alcohol estimates across the UK were 'not comparable' at that time[32]. While questions are similar in each of the surveys, questions on alcohol consumption were delivered through self-completion in the Welsh Health Survey prior to 2015/16, complicating comparisons. These questions are now included in the National Survey for Wales which is delivered face-to-face; the same mode of collection as SHeS. However, categorisation of drinkers and non-drinkers is also inconsistent across the surveys and further differences exist in the way some alcoholic drinks are categorised. On these bases, no attempt is made to compare alcohol estimates from SHeS to those from other surveys.
4.2. Methods
Questions about drinking alcohol have been included in SHeS since its inception in 1995. Questions are asked either face-to-face via the interviewer or included in the self-completion questionnaire if they are deemed too sensitive for a face-to-face interview (e.g. if being interviewed with a parent). All those aged 16-17 years are asked about their consumption via the self-completion, as are some of those aged 18-19 years, at the interviewers' discretion. The way in which alcohol consumption is estimated in the survey was changed significantly in 2008. A detailed discussion of those revisions can be found in the chapter on alcohol consumption in the 2008 report[33].
In 2019, the SHeS questionnaire covered the following aspects of alcohol consumption:
- usual weekly consumption
- daily consumption on the heaviest drinking day in the previous week
- problem drinking
Weekly consumption
Participants (aged 16 years and over) were asked preliminary questions to determine whether they drank alcohol at all. For those who reported that they drank, these were followed by further questions on how often during the past 12 months they had drunk each of six different types of alcoholic drink:
- normal strength beer, lager, stout, cider and shandy
- strong beer, lager, stout and cider
- spirits and liqueurs
- sherry and martini
- wine
- alcoholic soft drinks (alcopops)
From these questions, the average number of days per week the participant had drunk each type of drink was estimated. A follow-up question asked how much of each drink type they had usually drunk on each occasion. These data were converted into units of alcohol (see Section 4.2.2) and multiplied by the amount they said they usually drank on any one day[34].
Daily consumption
Participants were asked about drinking in the week preceding the interview, with actual consumption on the heaviest drinking day in that week then examined in more detail[35]. Details on the amounts consumed for each of the six types of drink listed in the weekly consumption section above were collected and converted into units of alcohol consumed.
Problem drinking
Since 2012 the AUDIT questionnaire has been used to assess problem drinking. AUDIT is widely considered to be the best screening tool for detecting problematic alcohol use. It comprises ten indicators of problem drinking: three indicators of consumption, four of use of alcohol considered harmful to oneself or others, and three of physical dependency on alcohol. Given the potentially sensitive nature of these questions, they were administered in self-completion format for all participants.
4.2.2. Calculating alcohol consumption in SHeS
The guidelines on lower risk drinking are expressed in terms of units of alcohol consumed. As discussed above, detailed information on both the volume of alcohol drunk in a typical week and on the heaviest drinking day in the week preceding the survey was collected from participants. The volumes reported were not validated. In the UK, a standard unit of alcohol is 10 millilitres or around 8 grams of ethanol. In this chapter, alcohol consumption is reported in terms of units of alcohol.
Questions on the quantity of wine drunk were revised in 2008. Since then, participants reporting drinking any wine have been asked what size of glass they drank from: large (250ml), medium (175ml) and small (125ml). In addition, to help participants make more accurate judgements they are also shown a showcard depicting glasses with 125ml, 175ml and 250ml of liquid. Participants also had the option of specifying the quantity of wine drunk in bottles or fractions of a bottle; with a bottle treated as the equivalent of six small (125ml) glasses.
There are numerous challenges associated with calculating units at a population level, not least of which are the variability of alcohol strengths and the fact that these have changed over time. Table 4A below outlines how the volumes of alcohol reported in the survey were converted into units (the 2008 report provides full information about how this process has changed over time)[36].Those who drank bottled or canned beer, lager, stout or cider were asked in detail about what they drank, and this information was used to estimate the amount in pints.
4.2.3. Age-standardised estimates for weekly alcohol consumption
The area deprivation data presented for weekly alcohol consumption are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this volume for a detailed description of SIMD and age-standardisation.
| Type of drink | Volume reported | Unit conversion factor |
|---|---|---|
| Normal strength beer, lager, stout, cider, shandy (less than 6% ABV) | Half pint | 1.0 |
| Can or bottle | Amount in pints multiplied by 2.5 | |
| Small can (size unknown) |
1.5 | |
| Large can / bottle (size unknown) |
2.0 | |
| Strong beer, lager, stout, cider, shandy (6% ABV or more) | Half pint | 2.0 |
| Can or bottle | Amount in pints multiplied by 4 | |
| Small can (size unknown) |
2.0 | |
| Large can / bottle (size unknown) |
3.0 | |
| Wine (including champagne and prosecco) | 250ml glass | 3.0 |
| 175ml glass | 2.0 | |
| 125ml glass | 1.5 | |
| 750ml bottle | 1.5 x 6 | |
| Sherry, vermouth and other fortified wines | Glass | 1.0 |
| Spirits | Glass (single measure) | 1.0 |
| Alcopops | Small can or bottle | 1.5 |
| Large (700ml) bottle | 3.5 |
4.2.4. Definitions
The UK CMO alcohol guidelines consist of three recommendations:
- A weekly guideline on regular drinking;
- Advice on single episodes of drinking; and
- A guideline on pregnancy and drinking.
According to the weekly guideline, adults are safest not to regularly drink more than 14 units per week, to keep health risks from drinking alcohol to a low level. If you do drink as much as 14 units a week, it is best to spread this evenly over three days or more. On a single episode of drinking, advice is to limit the total amount drunk on any occasion, drink more slowly, drink with food and alternate with water. The guideline on drinking and pregnancy, or planning a pregnancy, advises that the safest approach is not to drink alcohol at all[37].
Consumption of more than three units (women) or four units (men) on a single day is also reported in this chapter. This allows comparison with previous SHeS reports although these daily amounts of alcohol are no longer included in the most recent guidance from the UK Chief Medical Officers. Consumption of double this amount (six units for women and eight for men) is also reported.
Alcohol Use Disorders Identification Test (AUDIT) scale
The AUDIT questionnaire was primarily designed to screen for levels of alcohol dependency or high-risk use. In line with the WHO guidelines on using the tool, responses to each of the ten AUDIT questions were assigned values of between 0 and 4[38]. Scores for the ten questions were summed to form a scale, from 0 to 40, of alcohol use.
The WHO guidelines[39] for interpreting AUDIT scale scores are as follows:
| Score | Category description |
|---|---|
| 0 to 7 | low-risk drinking behaviour, or abstinence |
| 8 to 15 | medium level of alcohol problems, with increased risk of developing alcohol-related health or social problems (sometimes described as hazardous drinking behaviour) |
| 16-19 | high level of alcohol problems, for which counselling is recommended (harmful drinking behaviour) |
| 20 or above | warrants further investigation for possible alcohol dependence. |
4.3 Alcohol
4.3.1. Estimated usual weekly alcohol consumption level, 2003 to 2019
Following a significant decrease in prevalence of hazardous or harmful drinking levels for all adults from 34% in 2003 to 25% in 2013, levels have remained between 24% and 26% since then (24% in 2019). The prevalence of hazardous or harmful drinking levels has been around twice as high for men than for women across the time series (32% for men and 16% for women in 2019).
A corresponding increase in the proportion of non-drinkers was recorded between 2003 and 2013 when prevalence among all adults rose from 11% to 16%. Since 2013, the prevalence of non-drinking among all adults has remained between 16% and 17% (17% in 2019).
There were small differences between men and women in the prevalence of non-drinking across the time series. Among men, following a rise from 8% in 2003 to 14% in 2014, levels have since remained relatively stable fluctuating between 13% and 15% (15% in 2019). Prevalence of non-drinking among women rose from 13% in 2003 to 20% in 2013 and has remained in the range of 18 - 19% since (18% in 2019).
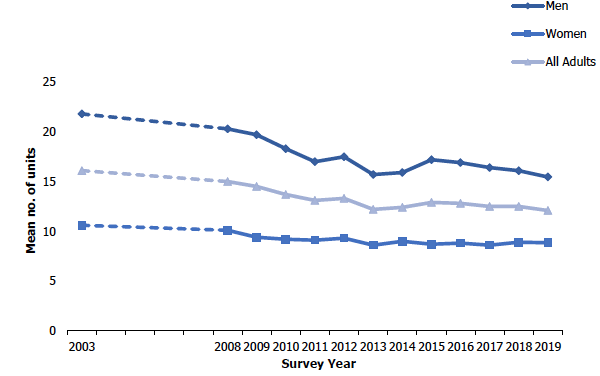
There has been an overall decrease over time in the mean number of units of alcohol consumed per week by all adult drinkers from 16.1 units in 2003 to 12.1 units in 2019, the lowest recorded across the time series. Although the means have consistently been higher for men than for women, trends across the time series are similar for both sexes: the mean number of units consumed per week has decreased from 21.8 units for men and 10.6 units for women in 2003 to 15.5 units and 8.8 units respectively in 2019. Figure 4A, Table 4.1
Mean number of units of alcohol consumed per week among adults, 2003- 2019, by sex
4.3.2. Estimated usual weekly alcohol consumption level, 2019, by age and sex
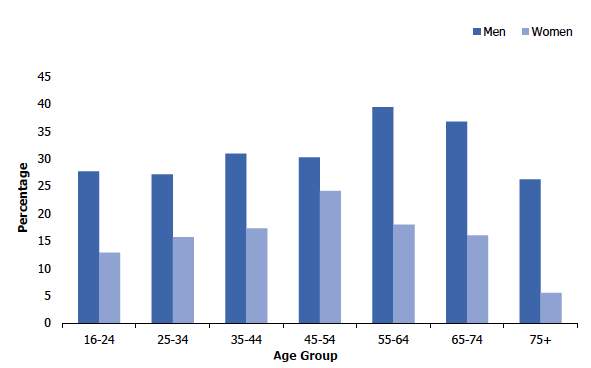
The prevalence of hazardous or harmful drinking for all adults was 24% in 2019, with men twice as likely to report hazardous or harmful drinking levels than women (32% and 16% respectively). The prevalence of hazardous or harmful drinking also differed by age, increasing from 20% among those aged 16-24 to 26 - 28% among those aged 45-74 before falling to the lowest proportion among adults aged 75 and over (14%).
As shown in Figure 4B, patterns of hazardous or harmful drinking levels by age were found to differ for men and women. Among men, the younger and oldest age groups recorded the lowest prevalence of hazardous or harmful drinking: 27- 28% among those aged 16-34, and 26% among those aged 75 and over and prevalence was highest among men aged 55-74 (37 - 39%). Among women, prevalence of hazardous or harmful drinking levels was lowest among those aged 75 and over (6%) and those aged 16-24 (13%) and peaked among those aged 45-54 (24%).
Adult hazardous/harmful drinking, 2019, by age and sex
The mean number of units of alcohol consumed per week by all adult drinkers was 12.1 units with men likely to consume more than women (15.5 units compared with 8.8 units per week respectively).
The mean number of units of alcohol consumed per week was lowest among adults aged 75 and over (8.2 units) and highest among those aged 55-64 (14.1 units). However, different patterns by age were found for men and women. Among men, the mean number of units of alcohol consumed per week was highest for those aged 55 to 64 (19.3 units) and lowest for those aged 25-34 (12.1 units). Among women, those aged 45-54 reported the highest mean number of units consumed per week (11.9 units) while those aged 75 and over reported the lowest (4.8 units).
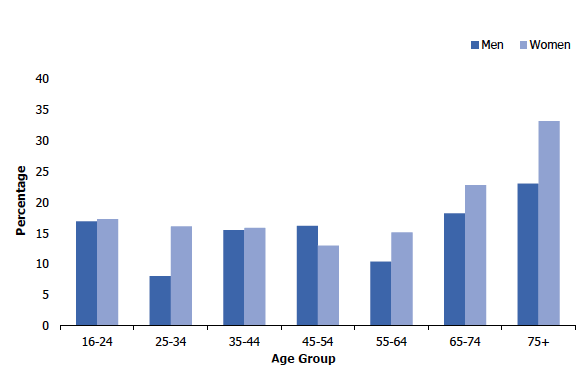
The prevalence of non-drinking among all adults was 17% in 2019, with variations by both age and sex (see Figure 4C). Prevalence of non-drinking was higher among women (18%) than among men (15%) and it was higher among all adults aged 65 and over (21% of those aged 65-74 and 29% of those aged 75 and over) than among those in younger age groups (prevalence ranged from 12% to 17% in those aged between 16 and 64). Figures 4B & 4C, Table 4.2
Adult non-drinkers, 2019, by age and sex
4.3.3. Estimated usual weekly alcohol consumption level (age-standardised), 2019, by area deprivation and sex
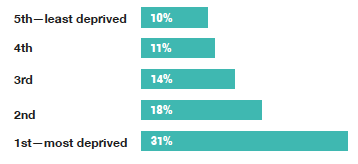
In line with results from previous years[40], the estimated levels of weekly alcohol consumption differed by area deprivation in 2019. Among all adults, the prevalence of hazardous or harmful drinking levels was highest among those living in the least deprived areas (30%) and lowest among those living in the most deprived areas (17%). Similar patterns were found for men and women.
Non-drinkers and hazardous/harmful drinkers, 2019, age-standardised and by area of deprivation
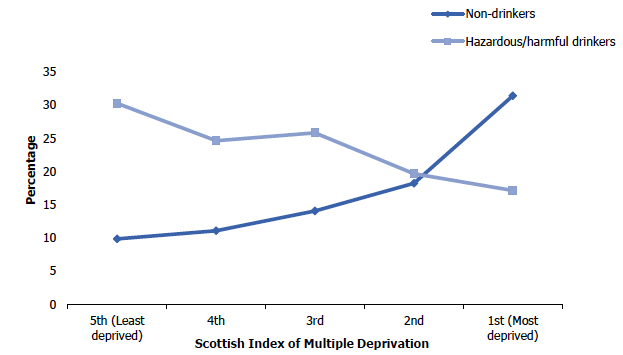
There continued to be a significant association between area deprivation and non-drinking prevalence in 2019, with the highest proportion of non-drinkers in the most deprived areas (31%) and lowest proportion in the least deprived areas (10%). Again, similar patterns were recorded for men and women.
The mean number of units of alcohol consumed per week for all drinkers did vary by area of deprivation in 2019 but with no clear pattern. For men drinking at a hazardous or harmful level, the consumption pattern observed in 2018was also evident in 2019, with a higher mean number of alcohol units per week recorded among men living in the most deprived areas (40.1 units) than among men living in the other areas (28.9 - 31.9 units). These differences were not statistically significant. This pattern was not evident for women drinking at a hazardous or harmful level. Figure 4D, Table 4.3
4.3.4. AUDIT scores, 2019, by age and sex
Using the AUDIT score to determine alcohol dependency or high-risk use, 83% of all adults were abstinent or drinking in a way that conferred low risk in 2019, an equal proportion to that reported for 2016/2017 combined. Women were more likely than men to be abstinent or drinking in a way that conferred low risk (89% compared to 77% respectively).
The prevalence of hazardous, harmful or possibly dependent drinking behaviour (AUDIT scores of 8 or more) in 2019 among all adults was 17% but was higher for men than for women (23% compared with 11%).
Hazardous drinking behaviour (AUDIT scores of 8-15) and harmful or possibly dependent drinking behaviour (AUDIT scores of 16 or more) also differed by sex. Among men, 20% reported hazardous drinking behaviour and 3% harmful or possibly dependent drinking behaviour while among women, these figures were 9% and 1% respectively.
Among all adults in 2019, the prevalence of hazardous drinking behaviour decreased with age from 21% among those aged 16-24 to 3% among those aged 75 and over. Similar patterns were found for men and women.
Harmful or possibly dependent drinking (AUDIT scores of 16 or more) also decreased with age from 5% among those aged 16-24 to 1% or less among those aged 55 and over. Patterns by age differed for men and women. For men, the prevalence of harmful or possibly dependent drinking ranged between 3% and 6% among those aged 16-64 before dropping to 1% or less for those aged 65 and over. For women the prevalence dropped from 5% among those aged 16-24 to between less than 1% and 2% for all other age groups.
AUDIT scores for all adults, 2019, by age
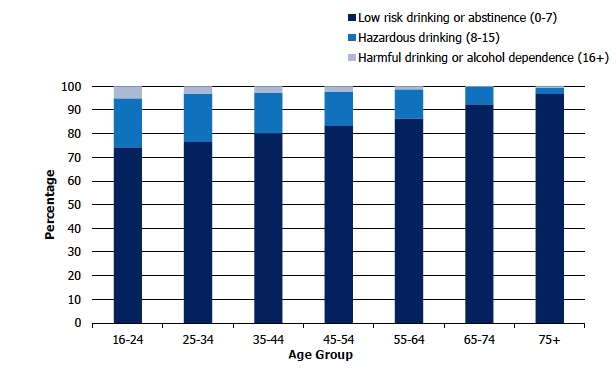
The prevalence of abstinence or low risk drinking showed a corresponding increase with age, from 74% of those aged 16-24 to 97% of those aged 75 and over. Patterns by age differed for men and women. For men, the prevalence of abstinence or low risk drinking was lowest among those aged 25-44 (71%) while for women it was lowest among those aged 16-24 (75%). Figure 4E, Table 4.4
4.3.5. AUDIT scores (age-standardised), 2019, by area deprivation and sex
There was no clear association between area deprivation and the prevalence of hazardous, harmful or possibly dependent drinking behaviour among all adults or by sex. However, although not statistically significant, the proportion of men who reported harmful or possibly dependent drinking behaviour (AUDIT scores of 16 or more) was higher among those who lived in the most deprived areas than the proportions in the less deprived areas (7% compared with 2-3% in the other areas). A lower proportion of men in the most deprived areas reported low risk drinking or abstinence (70% compared with 75 - 82% in other less deprived areas). Table 4.5
4.3.6. Children living with a parent with an AUDIT score of 8+ and 16+, 2017/2019 combined, by age and sex
To increase the sample size available, the detailed analysis of children living with parents with an AUDIT score of 8 or more and 16 or more, by age and sex used data from the 2017 and 2019 surveys combined.
Among all children in 2017/2019 combined, the majority (83%) were not living in a household with a parent exhibiting hazardous drinking behaviour or with a possible alcohol dependence (AUDIT scores of 0-7). Just under a fifth of children (17%) were living with at least one parent in their household who exhibited hazardous, harmful drinking behaviour or had a possible alcohol dependence (AUDIT score of 8 or more). Two per cent lived with at least one parent in their household who was drinking at a harmful level or who had possible alcohol dependence (AUDIT score of 16 or more). There were no significant differences by age or sex of the child in the proportion of children who had at least one parent who exhibited hazardous or harmful drinking behaviour or with a possible alcohol dependence. Table 4.6
Table List
Table 4.1 Estimated usual weekly alcohol consumption level, 2003 to 2019
Table 4.2 Estimated usual weekly alcohol consumption level, 2019, by age and sex
Table 4.3 Estimated usual weekly alcohol consumption level (age-standardised), 2019, by area deprivation and sex
Table 4.4 AUDIT scores, 2019, by age and sex
Table 4.5 AUDIT scores (age-standardised), 2019, by area deprivation and sex
Table 4.6 Children living with a parent with an AUDIT score of 8+ and 16+, 2017/2019 combined, by age and sex
The tables can be found on the main report page under supporting files: https://www.gov.scot/publications/scottish-health-survey-2019-volume-1-main-report/
References and notes
1. World Health Organization (2018) Alcohol Fact Sheet. Available from: www.who.int/news-room/fact-sheets/detail/alcohol
2. Mathers C, Stevens G and Mascarenhas M (2009). Global health risks: mortality and burden of disease attributable to selected major risks. Geneva: World Health Organization. Available from: www.who.int/healthinfo/global_burden_disease/GlobalHealthRisks_report_full.pdf
3. World Health Organization (2018) Alcohol Fact Sheet. Available from: www.who.int/news-room/fact-sheets/detail/alcohol
4. Griswold MG, Fullman N, Hawley C, Arian N, Zimsen SR, Tymeson HD, Venkateswaran V, Tapp AD, Forouzanfar MH, Salama, JS, Abate KH (2018). Alcohol use and burden for 195 countries and territories, 1990-2016: a systematic analysis for the Global Burden of Disease Study for 2016. The Lancet, 392(10152), 1015-1035.
5. World Health Organisation (2018) Global Status Report on Alcohol and Health. Available from: http://www.who.int/substance_abuse/publications/global_alcohol_report/gsr_2018/en/
6. NHS Health Scotland (2020) Monitoring and evaluating Scotland's Alcohol Strategy (MESAS) Available from: http://www.healthscotland.scot/media/3103/mesas-monitoring-report-2020.pdf
8. Alcohol-Related Hospital Statistics Scotland 2018/19, Edinburgh: NHS National Services Scotland, Information Services Division, 2019. Available from: https://www.isdscotland.org/Health-Topics/Drugs-and-Alcohol-Misuse/Publications/2019-11-19/2019-11-19-ARHS-Report.pdf
9. Beeston C, Robinson M, Craig N and Graham L (2011). Monitoring and Evaluating Scotland's Alcohol Strategy. Setting the Scene: Theory of change and baseline picture. Edinburgh: NHS Health Scotland. Available from: www.healthscotland.com/uploads/documents/15580-MESASsettingTheSceneReport.pdf
10. Katikireddi SV, Whitley E, Lewsey J, Gray L and Leyland AH (2017). Socioeconomic status as an
effect modifier of alcohol consumption and harm: analysis of linked cohort data. Lancet Public
Health; 2: 267–76.
11. Long-term monitoring of health inequalities: January 2020 report. Annual update of the long- term monitoring of health inequalities headline indicators. Available from: https://www.gov.scot/binaries/content/documents/govscot/publications/statistics/2020/01/long-term-monitoring-health-inequalities-january-2020-report/documents/long-term-monitoring-health-inequalities-january-2020-report/long-term-monitoring-health-inequalities-january-2020-report/govscot%3Adocument/long-term-monitoring-health-inequalities-january-2020-report.pdf
12. Alcohol-Related Hospital Statistics Scotland 2018/19, Edinburgh: NHS National Services Scotland, Information Services Division (2019). [online]. Available from: https://www.isdscotland.org/Health-Topics/Drugs-and-Alcohol-Misuse/Publications/2019-11-19/2019-11-19-ARHS-Report.pdf
13. The Societal Cost of Alcohol Misuse in Scotland for 2007, Edinburgh: Scottish Government, 2010. Available from: https://www.webarchive.org.uk/wayback/archive/20170701074158/http://www.gov.scot/Publications/2009/12/29122804/21
14. Further information on Scotland Performs can be found at: http://nationalperformance.gov.scot/
15. See: https://nationalperformance.gov.scot/measuring-progress/national-indicator-performance
16. See: www.gov.scot/Topics/Health/Services/Alcohol/safer-drinking
17. Angus C, Holmes J, Pryce R, Meier P and Brennan A (2016). Model-based appraisal of the comparative impact of Minimum Unit Pricing and taxation policies in Scotland: An adaptation of the Sheffield Alcohol Policy model version 3. Sheffield: University of Sheffield. Available from: www.sheffield.ac.uk/polopoly_fs/1.565373!/file/Scotland_report_2016.pdf
18. Alcohol (Minimum Pricing) (Scotland) Act 2012. See: www.legislation.gov.uk/asp/2012/4/contents/enacted
19. See: www.gov.scot/Topics/Health/Services/Alcohol/minimum-pricing
20. NHS Health Scotland (2020) Monitoring and evaluating Scotland's Alcohol Strategy (MESAS) Available from: http://www.healthscotland.scot/media/3103/mesas-monitoring-report-2020.pdf
21. See: http://www.healthscotland.scot/health-topics/alcohol/evaluation-of-minimum-unit-pricing-mup
22. Robinson, M, Mackay, D, Giles, L, Lewsey, J and Beeston, C. (2020). Evaluating the impact of Minimum Unit Pricing (MUP) on sales-based alcohol consumption in Scotland: controlled interrupted time series analyses. Public Health Scotland. Available from: http://www.healthscotland.scot/publications/evaluating-the-impact-of-minimum-unit-pricing-mup-on-sales-based-alcohol-consumption-in-scotland-controlled-interrupted-time-series-analyses
23. Institute of Alcohol Studies. (2020). Minimum Unit Pricing in Scotland: what we know so far about its effects on consumption and health harms. Available from: http://www.ias.org.uk/uploads/pdf/IAS%20reports/sb27052020.pdf
24. Scottish Government. (2018). Alcohol Framework 2018: Preventing Harm. Available from: https://www.gov.scot/binaries/content/documents/govscot/publications/strategy-plan/2018/11/alcohol-framework-2018-preventing-harm-next-steps-changing-relationship-alcohol/documents/alcohol-framework-2018-preventing-harm-next-steps-changing-relationship-alcohol/alcohol-framework-2018-preventing-harm-next-steps-changing-relationship-alcohol/govscot%3Adocument/00543214.pdf
25. HS Health Scotland (2020) Monitoring and evaluating Scotland's Alcohol Strategy (MESAS) Available from: http://www.healthscotland.scot/media/3103/mesas-monitoring-report-2020.pdf
26. World Health Organization (2018) SAFER initiative. Available from: https://www.who.int/substance_abuse/safer/launch/en/
27. Bellis MA, Hughes K, Jones L, Morloe M, Nichols J, McCoy E, Webster J and Sumnall H (2015). Holidays, celebrations, and commiserations: measuring drinking during feasting and fasting to improve national and individual estimates of alcohol consumption. BMC Med; 13(1): 113. Available from: https://bmcmedicine.biomedcentral.com/articles/10.1186/s12916-015-0337-0
28. Torvik FA, Rognmo K and Tambs K (2012). Alcohol use and mental distress as predictors of non-response in a general population health survey: the HUNT study. Social Psychiatry and Psychiatric Epidemiology; 47(5):805-816. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3328681/
29. Gorman E, Leyland AH, McCartney G, White IR, Katikireddi SV, Rutherford L, Graham L and Gray L (2014). Assessing the representativeness of population-sampled health surveys through linkage to administrative data on alcohol-related outcomes. American Journal of Epidemiology; 180(9): 941-8. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4207717/
30. Gorman E, Leyland AH, McCartney G, Katikireddi SV, Rutherford L, Graham L, Robinson M and Gray L (2017). Adjustment for survey non-representativeness using record-linkage: refined
estimates of alcohol consumption by deprivation in Scotland. Addiction; 112(7): 1270-1280. Available from: https://onlinelibrary.wiley.com/doi/abs/10.1111/add.13797
31. NHS Health Scotland (2020) Monitoring and evaluating Scotland's Alcohol Strategy (MESAS) Available from: http://www.healthscotland.scot/media/3103/mesas-monitoring-report-2020.pdf
32. Comparing official statistics across the UK. Government Statistical Service, 2016. Available from: https://www.statisticsauthority.gov.uk/wp-content/uploads/2016/11/Comparing-Official-Statistics-Across-the-UK.pdf
33. Reid S (2009). Chapter 3: Alcohol consumption. In: Bromley C, Bradshaw P and Given L. (eds.) The 2008 Scottish Health Survey – Volume 1: Main Report. Edinburgh: Scottish Government. 2009. Available from: www.gov.scot/Publications/2009/09/28102003/31
34. For participants aged 16 and 17, details on alcohol consumption were collected as part of a special smoking and drinking self-completion questionnaire. Some aged 18 and 19 also completed the self-completion if the interviewer felt it was appropriate. For all other adult participants, the information was collected as part of the face-to-face interview. The method of estimating consumption follows that originally developed for use in the General Household Survey and is also used in the Health Survey for England. For six types of alcoholic drink (normal strength beer/lager/cider/shandy, strong beer/lager/cider, spirits/liqueurs, fortified wines, wine, and alcoholic soft drinks), participants were asked about how often they had drunk each one in the past twelve months, and how much they had usually drunk on any one day. The amount given to the latter question was converted into units of alcohol, with a unit equal to half a pint of normal strength beer/lager/cider/alcoholic soft drink, a single measure of spirits, one glass of wine, or one small glass of fortified wine. A half pint of strong beer/lager/cider was equal to 1.5 units. The number of units was then multiplied by the frequency to give an estimate of weekly consumption of each type of drink. The frequency multipliers were:
| Drinking frequency | Multiplying factor |
|---|---|
| Almost every day | 7.0 |
| 5 or 6 times a week | 5.5 |
| 3 or 4 times a week | 3.5 |
| Once or twice a week | 1.5 |
| Once or twice a month | 0.375 |
| One every couple months | 0.115 |
| Once or twice a year | 0.029 |
The separate consumption figures for each type of drink were rounded to two decimal places and then added together to give an overall weekly consumption figure.
35. Participants were first asked if they had drunk alcohol in the past seven days. If they had, they were asked on how many days and, if on more than one, whether they had drunk the same amount on each day or more on one day than others. If they had drunk more on one day than others, they were asked how much they drank on that day. If they had drunk the same on several days, they were asked how much they drank on the most recent of those days. If they had drunk on only one day, they were asked how much they had drunk on that day.
36. See: https://www.gov.scot/publications/scottish-health-survey-2008/pages/29/
37. See: https://www.drinkaware.co.uk/alcohol-facts/alcoholic-drinks-units/latest-uk-alcohol-unit-guidance/
38. AUDIT questionnaire
| Questions | 0 | 1 | 2 | 3 | 4 |
|---|---|---|---|---|---|
| 1. How often do you have a drink containing alcohol? | Never | Monthly or less | 2-4 times a month | 2-3 times a week | 4 or more times a week |
| 2. How many drinks containing alcohol do you have on a typical day when you are drinking? | 1 or 2 | 3 or 4 | 5 or 6 | 7 to 9 | 10 or more |
| 3. How often do you have six or more drinks on one occasion? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 4. How often during the last year have you found that you were not able to stop drinking once you had started? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 5. How often during the last year have you failed to do what was normally expected of you because of drinking? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 6. How often during the last year have you needed a first drink in the morning to get yourself going after a heavy drinking session? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 7. How often during the last year have you had a feeling of guilt or remorse after drinking? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 8. How often during the last year have you been unable to remember what happened the night before because of your drinking? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
| 9. Have you or someone else been injured because of your drinking? | No | Yes, but not in the last year | Yes, during the last year | ||
| 10. Has a relative, friend, doctor, or other health care worker been concerned about your drinking last year? | No | Yes, but not in the last year | Yes, during the last year |
39. Babor, T.F., Higgins-Biddle, J.C., Saunders, J.B. and Monteiro, M.G (2001). AUDIT – The Alcohol Use Disorders Identification Test – Guidelines for Use in Primary Care, Second Edition. Geneva: World Health Organization.
40. Vosnaki, K (2018). Chapter 3: Alcohol. In: McLean, J, Dean, L and Hinchcliffe, S. (eds.) The Scottish Health Survey 2018 – Volume 1: Main Report. Edinburgh: Scottish Government. 2020. Available from: https://www.gov.scot/publications/scottish-health-survey-2018-volume-1-main-report/
Contact
There is a problem
Thanks for your feedback