Scottish Health Survey 2019 - volume 1: main report
Presents results for the Scottish Health Survey 2019, providing information on the health and factors relating to health of people living in Scotland.
This document is part of a collection
Chapter 5: Smoking
Adult self-reported current smokers
- 17% of adults smoked in 2019, the lowest level in the time series *
Men smoked a higher number of cigarettes per day on average than women in 2019.
- 13.1 mean number of cigarettes smoked per day by men
- 11.3 mean number of cigarettes smoked per day by women
Smoking prevalence in 2019 was highest among those aged 25 – 54 and lowest among those aged 75 and over.
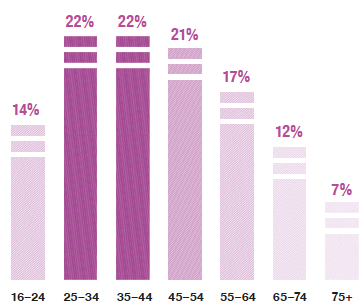
* Although not significantly different from 2018 (19%) or 2017 (18%).
The proportion of non-smokers that reported being exposed to second-hand smoke in their own or another person's home has decreased over the years.
- 25% in 2003
- 14% in 2013
- 10% in 2019
The proportion of children exposed to secondhand smoke in their own home has stabilised at 6-7% in recent years.**
- 12% in 2012
- 6% in 2019
** Note that a ban on smoking in enclosed public places was introduced in Scotland in 2006.
E-cigarette use in 2019
- 20% of all adults had ever used e-cigarettes
- 13% had previously used e-cigarettes
- 7% were current e-cigarette users
Current e-cigarette use has remained stable since 2015.
- 5% in 2014
- 7% in 2019
There has been an overall decrease in the percentage of adults that have never used e-cigarettes.
- 85% in 2014
- 80% in 2019
The highest proportion of current e-cigarette users in 2019 was among those aged 35–44 and the lowest among those aged 75 and over.
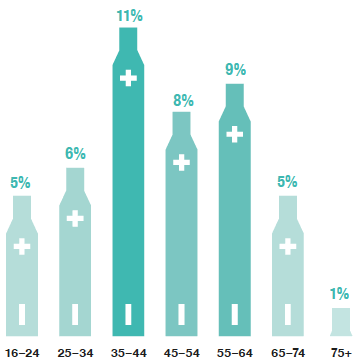
Around one in five adults self-reported as a current cigarette smoker in 2018/2019, a figure which did not vary significantly when adjusted for cotinine levels for the same period.
- 19% current cigarette smoker
- 23%cotinine-adjusted levels
In 2018/2019, more than one in five non-smokers had a detectable level of cotinine in their saliva.
- 21%
The proportion of non-smokers with detectable cotinine exposure decreased over time.***
- 85% in 2003
- 38% in 2008/2009
- 21% in 2018/2019
*** Note that a ban on smoking in enclosed public places was introduced in Scotland in 2006.
5. Smoking
5.1 Introduction
The World Health Organisation describe tobacco as 'one of the biggest public health threats the world has ever faced' with more than 7 million deaths worldwide a direct result of tobacco use and a further 1.2 million attributed to second-hand smoke exposure[1]. In Scotland, smoking was associated with around 9,360 deaths in those aged 35 and over[2] and an estimated 99,296 hospital admissions in 2018, with a smoking-attributable disease or condition the primary reason for 51,969 of these admissions[3]. Tobacco use is associated with stillbirths and infant deaths, childhood respiratory diseases, and communicable as well as non-communicable diseases in adulthood[4]. As the cause of around one in five deaths and the primary preventable cause of premature death, smoking represents the chief threat to Scotland's public health[5]. Smoking rates continue to be highest in Scotland's most deprived areas underlining smoking as a key ongoing health inequality challenge[6].
The risks associated with smoking increase the longer a person continues smoking. However, these risks can reduce substantially when a person stops, adding further weight to the importance of cessation policies, interventions and initiatives. Smoking cessation interventions, including pharmacotherapy such as nicotine replacement therapy (NRT), are among the most cost-effective health care interventions available[7].
5.1.1 Policy background
Part of the Scottish Government's National Outcomes Framework is the overall strategic objective for health: 'We are healthy and active'[8]. Scottish Health Survey (SHeS) data are used as a National Indicator to measure the proportion of adults with two or more of the following health risk behaviours: currently smoking, harmful drinking, low physical activity and obesity[9].
In 2013, the Scottish Government set out its ambition to create a 'tobacco-free generation' (defined as 'a smoking prevalence among the adult population of 5% or lower') by the year 2034[10]. The Scottish Ministerial Working Group on Tobacco Control was formed in 2015 to provide expert advice to the Scottish Government that would inform policy development, as well as monitoring existing policies and sharing best practice[11].
Raising Scotland's Tobacco-free Generation was published in June 2018[12] outlining interventions and policies that aim to ensure that when those born in 2013 reach the age of 21, they will be a 'tobacco free' generation. The actions include awareness raising campaigns, encouraging healthier behaviour in public settings, improving cessation services, regulations on smoking in prisons, the advertisement of e-cigarettes and restrictions on heated tobacco products. In addition, in 2018, the Scottish Prison Service implemented a smoking ban in prisons, accompanied by cessation support[13].
The 'quit your way' branding was established as part of Raising Scotland's Tobacco-free Generation. This wasbrought to life through the 'Quit Your Way – with our support' campaign, which under the banner of a single national identity for smoking cessation support in Scotland[14], aims to support individuals to stop smoking in a way that works for them with information on the benefits of quitting, local support services, personal quit plans and more[15].
Working with COSLA, NHS Health Scotland published Smoke-free Local Authority Implementation Guidance[16] in January 2017 which set out actions related to the themes of smoking prevention, protection and cessation. The 2015/16 NHS Local Delivery Plan (LDP) Standards and subsequent 2019 report on progress[17], while focused on delivering a universal smoking cessation offer, also includes a target of helping those living in Scotland's most deprived areas. The targeting of these areas through LDP Standards has been recognised by organisations such as Cancer Research UK as a positive approach to tackling this health inequality[18].
The Health (Tobacco, Nicotine etc. and Care) (Scotland) Act 2016[19] commenced on 1 April 2017. The Act includes provisions to regulate:
- the introduction of a minimum age of 18 for the sale of Nicotine Vapour Products (NVPs) – including electronic cigarettes
- a ban on the purchase of NVPs on behalf of an under 18 – 'proxy purchase'
- the introduction of mandatory registration for the sale of NVPs
- bans on certain forms of domestic advertising and promotion of NVPs
- the introduction of an age verification policy for sales of tobacco and NVPs by under 18s ('Challenge 25')
- a prohibition on the sale of NVPs from vending machines.
- a ban on unauthorised sales of tobacco and NVPs by under 18s
- the introduction of statutory smoke-free perimeters around buildings on NHS hospital sites.
Regulation on most of these provisions came into force in 2017. The results of a consultation on proposals to ban smoking outside hospital buildings found that the majority of respondents were in favour, with around seven in ten in support of a 15 metre no-smoking perimeter[20].
Additional legislation on smoking passed by the Scottish Parliament includes the Smoking Prohibition (Children in Motor Vehicles) (Scotland) Act 2016 which deems it an offence for an adult to smoke in cars in a public place in the presence of children[21]. While across the UK, regulations came into force on 21 May 2017 making it an offence to sell cigarettes in any pack containing less than 20 cigarettes, and ensuring all cigarettes are sold in standardised brand-neutral packs[22].
5.1.2 Reporting on smoking in the Scottish Health Survey (SHeS)
Reliable data on smoking behaviour, cessation, nicotine replacement therapy (NRT) use and exposure to second-hand smoke are vital to effective monitoring of trends relevant to the various targets in place. This chapter presents prevalence of adult cigarette smoking and e-cigarette use for 2019 as well as trends in prevalence of both. Exposure to second-hand smoke among children and adult non-smokers is also reported with and without adjustments for cotinine.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. Readers should refer to the Glossary at the end of this Volume for a detailed description of SIMD.
Supplementary tables are also available on the Scottish Government SHeS websitehttps://www.gov.scot/collections/scottish-health-survey/
5.1.3 Comparability with other UK statistics
The Health Survey for England, Health Survey for Northern Ireland and the National Survey for Wales provide estimates of smoking prevalence in the other home nations within the UK. The surveys are conducted separately and have different sampling methodologies, so smoking prevalence estimates across the surveys are only partially comparable[23]. Smoking prevalence estimates from the UK-wide Integrated Household Survey for Scotland, Wales, England and Northern Ireland have been deemed to be fully comparable[24].
5.2 Methods and Definitions
5.2.1 Methods of collecting data on smoking behaviour
Adults aged 20 and over were asked about their smoking behaviour during the face to face interview. For those aged 16 and 17, information was collected in a self-completion questionnaire offering more privacy and reducing the likelihood of concealing behaviour in front of other household members. Those aged 18 and 19 could answer the questions either face to face or via the self-completion booklet, at the interviewer's discretion.
5.2.2 Questions on smoking behaviour
Questions on smoking have been included in SHeS since 1995. Some small changes were made to the questions in 2008 and 2012. These are outlined in the relevant annual reports[25],[26].
The current questions in the survey focus on:
- current smoking status
- frequency and pattern of current smoking
- the number of cigarettes smoked by current smokers
- exposure to second-hand smoke
- past smoking behaviour, current and ex-smokers
- quit attempts and desire to give up smoking
- medical advice on giving up smoking
- NRT use (including questions on NRT that led to successful cessation)
- e-cigarette use (including as part of a quit attempt).
The self-completion questions were largely similar to those asked in the face to face interview. However, given the age of the participants completing the self-completion questionnaire, questions on past smoking behaviour, desire to give up smoking and medical advice to stop smoking were excluded.
5.2.3 Questions on e-cigarette use
SHeS has gathered information on the use of e-cigarettes among the Scottish adult population since 2014, in response to their increased availability and high profile. The questions ask whether participants have ever used an e-cigarette as well as whether they currently use an e-cigarette.
5.2.4 Definitions
Cigarette smoking status
Smoking status categories reported here are:
- current cigarette smoker
- ex-regular cigarette smoker
- never regular cigarette smoker
- never smoked cigarettes at all
Information on cigar and pipe use is collected in the survey but as prevalence is low these are not considered in the definition of current smoking.
Exposure to second-hand smoke (children)
Exposure to second-hand smoke for children is measured in two ways in the survey:
- whether there is someone who regularly smokes inside the accommodation where the child lives, and
- parents' and older children's (aged 13-15) reports of whether children are exposed to smoke at home.
Exposure to second-hand smoke (adults)
Exposure to second-hand smoke in adults is measured in two ways in the survey:
- by asking respondents to self-report where they have been exposed to second-hand smoke
- collecting saliva samples from a sub-set of the adult respondent sample asked the biological module in order to determine whether cotinine, an indicator of exposure to second-hand smoke, is detectable for non-smokers.
The approach used to calculate mean cotinine levels among non-smokers was updated for the 2019 report. The analysis of saliva samples uses equipment which can detect cotinine levels as low as 0.1 ng/mL. In previous reports, for the purpose of calculating mean levels of cotinine across the population, any sample below this limit of detection was assumed to have a level of 0.05 ng/mL. However, over time, the proportion of non-smokers with levels of cotinine below the limit has increased to the point that it was necessary to review this assumption in light of its impact on reported population levels of exposure to second-hand smoke[27].
The analysis method was therefore changed to utilise Tobit regression. This method assumes that the distribution of values below the level of detection follows the same pattern as those above the method of detection. Thus, as the mean levels of cotinine among those with a cotinine level of between 0.1 ng/mL and 12 ng/mL (the level at which someone is deemed to be a cotinine-validated smoker) fall, so too do the assumed mean levels of those with a cotinine level of below 0.1 mg/mL[27]. Because of this change in method, figures presented in Table 5.7 differ from those presented in the 2017 report.
Further details on the collection and analysis of saliva samples for cotinine can be found in the 2019 technical report[28].
5.3 Smoking
5.3.1 Cigarette smoking status, 2019, by age and sex
In 2019, 17% of adults identified as current smokers, the lowest level in the time series, though not significantly different to the proportions recorded in 2018[29] (19%) and 2017[30] (18%).
Smoking prevalence did not significantly differ by sex, with 19% of men and 16% of women identifying themselves as current smokers in 2019. However, on average, men smoked a higher number of cigarettes per day than women (13.1 mean cigarettes per day for men compared with 11.3 for women; 12.2 for all adults).
As seen in previous years[31], there were significant differences in smoking prevalence by age group in 2019. The highest proportions of self-reported current smokers were recorded among those aged 25-54 (21 - 22%) and the lowest smoking prevalence was among those aged 75 and over (7%).
The highest mean number of cigarettes smoked per day by current smokers in 2019 was among those aged 45-74 (14.6 - 15.0 cigarettes) and the lowest among those aged 16-24 (7.6 cigarettes).
In 2019, 23% of all adults identified as ex-regular smokers. There was a significant association between age and previous smoking status in 2019, which again is consistent with previous years. Among all adults, the lowest proportion of ex-regular smokers in 2019 was found among those aged 16-24 (6%) while 35 - 37% of those aged 65 and over reported having smoked regularly in the past. Table 5.1
5.3.2 Cigarette smoking status (age-standardised), 2003 to 2019, by area deprivation and sex
Adults living in more deprived areas were more likely to be current regular smokers than those in less deprived areas: prevalence in 2019 was 32% among those who lived in the most deprived quintile with step-decreases across the intermediate quintiles to 6% in the least deprived quintile. Despite overall decreases in smoking prevalence, this has been a consistent pattern since 2003 when 45% of those who lived in the most deprived areas were current regular smokers compared with 17% in the least deprived areas.
Current cigarette smoking prevalence (age-standardised) among adults aged 16+, 2003 to 2019, by area deprivation
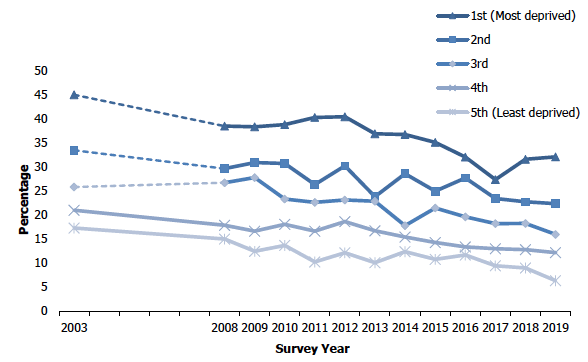
A similar overall pattern by area deprivation was recorded for the mean number of cigarettes smoked per day. In 2019, the mean number of cigarettes smoked per day among current smokers that lived in the most deprived areas (13.1 cigarettes) was higher than that among current smokers in the least deprived areas (10.2 cigarettes).
Since 2003, both smoking levels and the average number of cigarettes smoked have reduced significantly for all area deprivation quintiles. However, the gap between current smoking prevalence in the most deprived and least deprived areas increased from 18 percentage points in 2017 (27% in most deprived and 9% in least deprived) to 26 percentage points in 2019 (32% in most deprived and 6% in least deprived). Figure 5A, Table 5.2
5.3.3 Adult non-smokers' exposure to second-hand smoke, 2003 to 2019
The proportion of adult non-smokers that reported being exposed to second-hand smoke in their own or another person's home has reduced over the time series, with an overall decrease from 25% in 2003 to 10% in 2019. This pattern was evident for both men (24% in 2003 and 9% in 2019) and women (27% in 2003 and 10% in 2019).
There have been no significant variations over the time series since 2012 in the proportions of adult non-smokers that reported being exposed to second-hand smoke outside of buildings for either men or women, with proportions fluctuating between 11% and 15% for all adults since 2012.
The percentage of adult non-smokers who reported that they were not exposed to second-hand smoke in any of the places included in SHeS[32] has been relatively stable at 70% from 2012 to 2014 and then remaining in the range of 73 - 74% since 2015. Similar patterns and levels were found for men and women. Table 5.3
5.3.4 Children's exposure to second-hand smoke, 2012 to 2019
In 2019, 11% of children were living in accommodation in which someone regularly smoked indoors; a figure which was consistent for both boys and girls. There was a significant decrease between 2012 and 2015 in the proportion of children living in accommodation with someone who smoked indoors (from 19% to 12%). Since 2016, this figure has remained in the range 10 - 11%.
A small percentage of children were exposed to second-hand smoke in their own home in 2019 (6%). Over the time series, this exposure followed a similar pattern to the proportion of children living in accommodation in which anyone regularly smoked indoors. Between 2012 and 2014, 11 - 12% of children were exposed to second-hand smoke in their own home, a proportion that decreased to 6% in 2015 and that has remained in the range of 6 - 7% since. This pattern was similar among boys and girls in 2019. Figure 5B, Table 5.4
Percentage of children exposed to second-hand smoke in their own home, 2012 to 2019, by sex
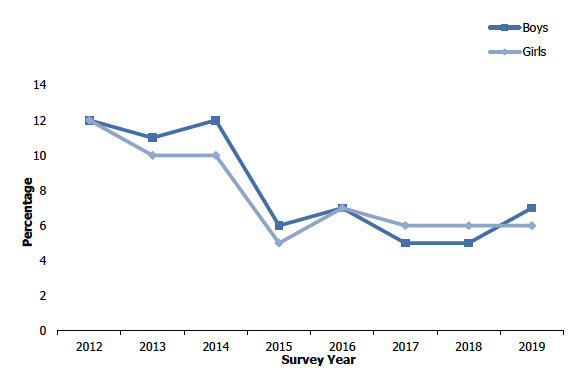
5.3.5 E-cigarette use among adults, 2014 to 2019, by age and sex
In 2019, 20% of all adults reported that they had ever used e-cigarettes: 7% reported being current users and 13% having previously used them. Four out of five adults (80%) had never used e-cigarettes.
Men and women were equally likely to be current users of e-cigarettes (7% for both men and women) in 2019. Similarly, there were no statistically significant differences in the proportion of men and women in 2019 who had used e-cigarettes in the past (14% and 12% respectively) or that reported never having used them (79% and 81% respectively).
The highest proportion of current e-cigarette users in 2019 was recorded among those aged 35-44 (11%) with the lowest proportions among those aged 75 and over (1%) and those aged 16-24 and 65-74 (both 5%). The highest proportion of former e-cigarette users was among those aged 25-34 (21%), while the lowest was among those aged 75 and over (3%).
Adult e-cigarette use - whether ever used, 2014 to 2019, by sex
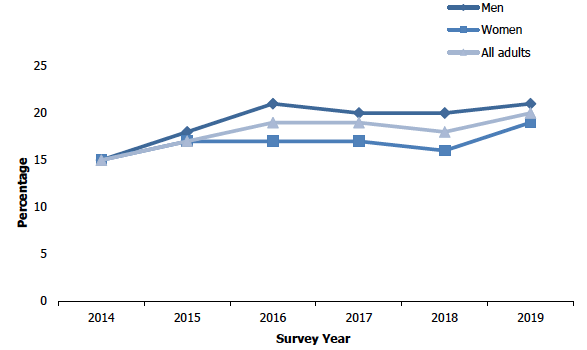
Current e-cigarette use has remained stable at 7% since 2015, having increased from 5% in 2014. There has been an overall decrease in the percentage of adults that have never used e-cigarettes from 85% in 2014 to 80% in 2019. Over the time series, the proportion of adults that reported never trying e-cigarettes has consistently been highest among those aged 75 and over (95 - 98% between 2014 and 2019). Figures 5C & 5D, Table 5.5
Current adult e-cigarette use, 2019, by age and sex
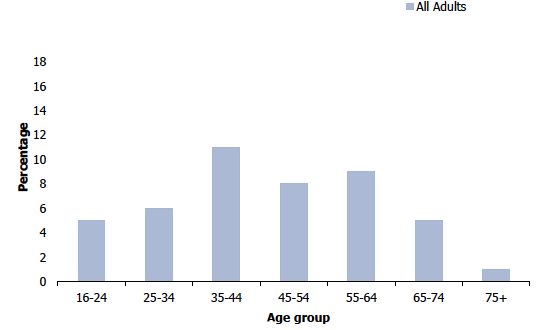
5.3.6 Smoking prevalence estimates without and with saliva cotinine adjustment, 2018/2019 combined, by age and sex
To increase the sample size available, the detailed analysis of smoking prevalence estimates without and with saliva cotinine adjustment by age and sex, used data from the 2018 and 2019 surveys combined for those with a valid cotinine measurement. Around one in five adults (19%) self-reported as a current cigarette smoker in 2018/2019, which did not differ significantly when adjusted for cotinine levels (23%). The 2018/2019 gap of four percentage points between self-reported smoking and cotinine adjusted levels for all adults was similar to those reported for 2016/2017 (five percentage points) and 2014/15 (three percentage points)[30].
There were no significant differences between men and women for either of these measures. The difference between self-reported smoking status and cotinine-adjusted smoking prevalence in 2018/2019 was four percentage points for all adults, as well as for men (20% and 24%) and women (18% and 22%).
The difference between self-reported smoking prevalence and the cotinine-adjusted smoking prevalence for adults aged 16 and over did not vary significantly with age. Figure 5E, Table 5.6
Smoking prevalence estimates without and with saliva cotinine adjustment, 2018/2019 combined, by age
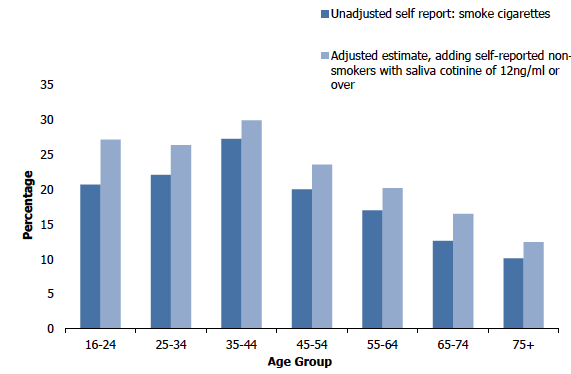
5.3.7 Self-reported, cotinine validated adult non-smokers' exposure to second-hand smoke, 2003 to 2018/2019 combined
To increase the sample size available, the analysis for self-reported cotinine validated adult non-smokers' exposure to second-hand smoke used data from 2003 alone and then subsequently combined data for two survey years at a time from 2008/2009 combined to 2018/2019 combined.
Adult non-smokers' geometric mean cotinine levels reduced significantly from 0.40 ng/ml in 2003 to 0.05 ng/ml in 2008/2009. In 2012/2013 there was a further significant decrease in the non-smokers' geometric mean cotinine levels to 0.02 ng/ml and it has remained at this level for each of the combined survey periods since, including in 2018/2019.
In 2018/2019, around one in five non-smokers (21%) had a detectable level of cotinine in their saliva. The largest drop in the proportion of non-smokers with detectable cotinine exposure was between 2003 (85%) and 2008/2009 (38%), a 47 percentage point decrease. There was a subsequent fall of 13 percentage points in 2012/2013 (to 25%) with a gradual decrease since from 26% in 2014/2015 to 21% in 2018/2019.
Across the time series, both geometric mean cotinine levels and the proportions with detectable cotinine exposure have generally been very similar for male and female non-smokers. Figure 5F, Table 5.7
Percentage of self-reported non-smokers exposed to cotinine, 2003 to 2018/2019 combined
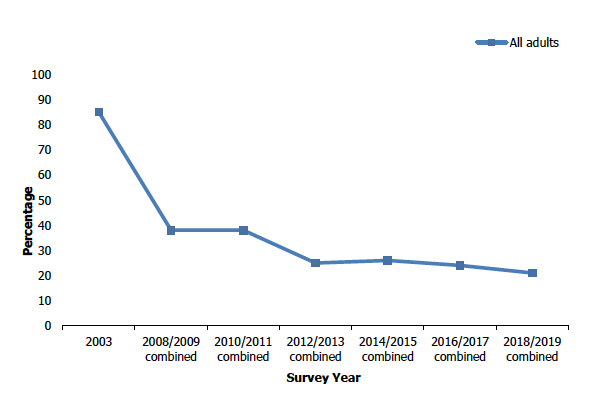
Table List
Table 5.1 Cigarette smoking status, 2019, by age and sex
Table 5.2 Cigarette smoking status (age-standardised), 2003 to 2019, by area deprivation and sex
Table 5.3 Non-smokers' exposure to second-hand smoke, 2003 to 2019
Table 5.4 Children's exposure to second-hand smoke, 2012 to 2019
Table 5.5 E-cigarette use, 2014 to 2019, by age and sex
Table 5.6 Smoking prevalence estimates without and with saliva cotinine adjustment, 2018/2019 combined, by age and sex
Table 5.7 Self-reported, cotinine validated non-smokers' exposure to second-hand smoke, 2003 to 2018/2019 combined
The tables can be found on the main report page under supporting files: https://www.gov.scot/publications/scottish-health-survey-2019-volume-1-main-report/
References and notes
1. World Health Organisation (2019) Tobacco. See: https://www.who.int/news-room/fact-sheets/detail/tobacco
2. See: https://www.scotpho.org.uk/behaviour/tobacco-use/data/smoking-attributable-deaths/
3. See: https://www.scotpho.org.uk/behaviour/tobacco-use/data/smoking-attributable-admissions/
4. World Health Organisation (2014). Tobacco and Inequities: Guidance for addressing inequities in Tobacco-related harm. Available from: http://www..who.int/en/publications/abstracts/tobacco-and-inequities.-guidance-for-addressing-inequities-in-tobacco-related-harm-2014
5. Raising Scotland's tobacco-free generation: our tobacco control action plan 2018. Edinburgh: Scottish Government, 2018. Available from: https://www.gov.scot/publications/raising-scotlands-tobacco-free-generation-tobacco-control-action-plan-2018/
6. See: http://www.healthscotland.scot/news/2018/june/welcoming-scotland-s-tobacco-control-action-plan
7. A guide to smoking cessation in Scotland. Edinburgh: NHS Scotland, 2017. Available from: http://www.healthscotland.scot/media/1097/helping-smokers-to-stop-smoking-2017.pdf
8. The National Performance Framework is described here: https://nationalperformance.gov.scot/
9. See: https://nationalperformance.gov.scot/measuring-progress/national-indicator-performance
11. See: https://www.gov.scot/groups/scottish-ministerial-working-group-on-tobacco-control/
12. Raising Scotland's tobacco-free generation: our tobacco control action plan 2018. Edinburgh: Scottish Government, 2018. Available from: https://www.gov.scot/publications/raising-scotlands-tobacco-free-generation-tobacco-control-action-plan-2018/
13. See: https://uk.changeincorporated.com/context/prison-smoking-ban-is-deemed-a-success-in-scotland
14. See: https://www.gov.scot/news/quit-smoking-your-way/
15. See: https://www.nhsinform.scot/campaigns/quit-your-way-scotland
16. Smoke-free local authority implementation guidance. Edinburgh: NHS Health Scotland, 2017. Available from: http://www.healthscotland.scot/media/1277/smoke-free-local-authority-implementation-guidance-jan2017-english.pdf
17. See: https://www.gov.scot/publications/nhsscotland-performance-against-ldp-standards/pages/introduction/
18. Caroline Smith, Sarah Hill, and Amanda Amos (2018) Stop Smoking Inequalities: A systematic review of socioeconomic inequalities in experiences of smoking cessation interventions in the UK.Cancer Research UK. Available from: https://www.cancerresearchuk.org/sites/default/files/stop_smoking_inequalities_2018.pdf
19. See http://www.legislation.gov.uk/asp/2016/14/pdfs/asp_20160014_en.pdf
20. See https://www.gov.scot/news/smoking-ban-proposals-1/
21. Smoking Prohibition (Children in Motor Vehicles) (Scotland) Act 2016. See: http://www.legislation.gov.uk/asp/2016/3/contents
23. Comparing official statistics across the UK. Government Statistical Service, 2016. Available from: https://www.statisticsauthority.gov.uk/wp-content/uploads/2016/11/Comparing-Official-Statistics-Across-the-UK.pdf
24. See: https://fingertips.phe.org.uk/documents/smoking_prevalence_comparisons_AUG2016.pdf
25. Gray L & Leyland AH (2009). Chapter 4: Smoking. In: Bromley, C., Bradshaw, P. and Given, L. (eds.) The 2008 Scottish Health Survey – Volume 1: Main Report. Edinburgh: Scottish Government. 2009. www.gov.scot/Publications/2009/09/28102003/0
26. Gray L & Leyland AH (2013). Chapter 4: Smoking. In: Rutherford, L., Hinchliffe, S. and Sharp, C. (eds.) The Scottish Health Survey 2012 – Volume 1: Main Report. Edinburgh: Scottish Government. Available from: www.gov.scot/Publications/2013/09/3684
27. Semple, S., Mueller, W., Leyland, A H., Gray, L. & Cherrie, J W. (2019). Assessing progress in protecting non-smokers from secondhand smoke. Tobacco Control. Available from: https://tobaccocontrol.bmj.com/content/28/6/692.info
28. Gray, L & Leyland, A H. (2017). Chapter 5: Smoking. In: McLean, J., Christie, S., Hinchcliffe, S. and Gray, L. (eds.) The Scottish Health Survey 2017: volume one - main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/
29. Dean, L & Mirani, K. (2018). Chapter 4: Smoking. In: McLean, J., Dean, L. and Hinchcliffe, S. (eds.) The Scottish Health Survey 2018: main report – revised 2020. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2018-volume-1-main-report/
30. Gray, L & Leyland, A H. (2017). Chapter 5: Smoking. In: McLean, J., Christie, S., Hinchcliffe, S. and Gray, L. (eds.) The Scottish Health Survey 2017: volume one - main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/
31. Dean, L & Mirani, K. (2018). Chapter 4: Smoking. In: McLean, J., Dean, L. and Hinchcliffe, S. (eds.) The Scottish Health Survey 2018: main report – revised 2020. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2018-volume-1-main-report/
32. At their own / other's home, at work, in cars / vans, outside buildings, or in public places
Contact
There is a problem
Thanks for your feedback