Attend Anywhere / Near Me video consulting service evaluation 2019-2020: report
This report presents the findings of an external evaluation of the Attend Anywhere / Near Me video consultations service used across health and care services in Scotland
1. Background and aims
1.1 About the evaluation
This evaluation was conducted during Aug 2019-March 2020 by a research team based within the Interdisciplinary Research in Health Sciences (IRIHS) unit at the University of Oxford. It was commissioned by the Scottish Government to deliver policy and practice-focused outputs which can shape and direct future investment decisions, programme management and national support activities for remote video consultations across Scotland. In particular, the evaluation sought to provide evidence to support the spread and scale-up of video-based access to health & social care services.
The evaluation focused on the implementation and scaling up of Attend Anywhere, which is a bespoke video call system that has been purpose-built for the health sector. It works via an internet browser and can be used on a computer, mobile and tablet device using the internet browsers Google Chrome, Microsoft Edge or Apple Safari. Attend Anywhere is more than a technology; it is a framework to introduce and support remote video consultations at scale.
An initial national licence for the Attend Anywhere system was procured on behalf of the Scottish Government in October 2016. Following the outcomes of initial pilot work, a further two-year national contract, with an option for a third year, was established in October 2017, in order to provide local health and social care organisations across Scotland with access to the system free of charge.
Financial investments had also gone into developing and expanding the service model during 2018/2019, including the NHS 'Near Me' projects in NHS Highland (developing video consultations to patients at home or local clinics) and the 'scale-up challenge' to support implementation across a number of participating health boards [3].
Uptake and use of Attend Anywhere has steadily grown following the launch of this scaling up programme, and by the time of writing this report (early 2020), all 14 territorial Health Boards and the Golden Jubilee National Hospital were enrolled. In addition, services have been established across a wide range of Health and Social Care Partnerships[2] (HSCP) and Third Sector organisations (see Appendix A).
This evaluation applied a mixed-methods (qualitative and quantitative) approach to provide a deeper understanding of outcome achievements in relation to the uptake and use of Attend Anywhere, review its current and potential for service improvement, and identify barriers and facilitators that have a bearing on the continued expansion of the video consultation services.
The main aims were as follows:
a. To assess Attend Anywhere's progress and achievements in relation to the use and outcomes of Attend Anywhere.
b. To develop an understanding of the implementation experience of Attend Anywhere to date.
c. To make recommendations relevant to any future scaling-up, spread and sustainability of Attend Anywhere and similar digital services.
1.2 A brief history of Attend Anywhere in Scotland
There has been a long established strategic intent to use video for remote consulting, and this has been consistently advocated through Scotland's eHealth Strategy [4,5] and Scotland's Digital Health & Care Strategy [6]. It has been viewed as a means to improve citizens' access to health and care services and, ultimately, to improve their health outcomes.
In 2014, the Scottish Government established the Technology Enabled Care (TEC) Programme, which included a series of workstreams to drive the widespread adoption of technology to support self-management, access to care and remote management within health and social care. The Scotland-wide programme was set up to respond to the need for service transformation in the context of rising demand for health and social care. Through central funding, the programme aims to drive deployment at a local level alongside national infrastructure and support work, and to place Scotland at the forefront of innovative approaches to technology enabled care.
In the context of Scotland's unique geography, video consulting was seen as enabling the pooling of expertise and provision across the country to ensure a better patient experience that reached those in the farthest corners of the country. The TEC programme's video-consulting (VC) workstream focused on the roll out of video consultations across Scotland. This initially involved a range of pilot studies using different video consulting technologies, including Cisco Jabber and Polycom devices, to improve communication between health and social care organisations.
In 2015, the TEC team became aware of Attend Anywhere, which has evolved in collaboration with Australian governments, universities and public hospitals over many years to support business-as-usual video call access to public health services by patients. The Attend Anywhere organisation was founded in Melbourne, Australia in 1998. It operates on a not-for-profit basis, selling licences to healthcare organisations, constituting user accounts that allow the creation and management of 'virtual waiting areas'. Each clinician or staff member within a service has their own clinic account and can use the same waiting area. The licence cost will vary depending on the number of waiting areas used by the health organisations.
Attend Anywhere uses internet browser-based video technology that can be accessed by a member of the public using their own device, be it a laptop, tablet or mobile phone. It has been designed to match the consulting workflow.
Attend Anywhere consists of three main components:
a. A service and operations layer - this includes professional assistance and advice from a team of experts, providing recommended ways of introducing and running video consultations within existing workflows and a supporting resource centre (e.g. guidance, implementation protocols, template patient leaflets).
b. A management layer - software platform design to help implement the Attend Anywhere model within healthcare settings. This includes a web-based management console to allow the care provider to see when the patient has arrived in the virtual waiting area, and to manage video appointments through existing processes and systems. Staff can create/manage the waiting areas, control access to them and view detailed reports about adoption and use.
c. A video technology layer - open-source video technology called WebRTC video technology, which is integrated with the software platform in a way that meets security and privacy requirements
One of the defining features of the Attend Anywhere model for video consulting is the 'inbound' (or ' person-centric') workflow, which seeks to emulate the ways in which patients physically attend their appointments. For example, a single button on a website (or consistent weblink address on an appointment letter) offers a consistent channel or 'front door' for patients to access a 'virtual waiting room' (potentially managed by a receptionist), before being joined virtually by the clinician. This is illustrated in the diagram below.[3]
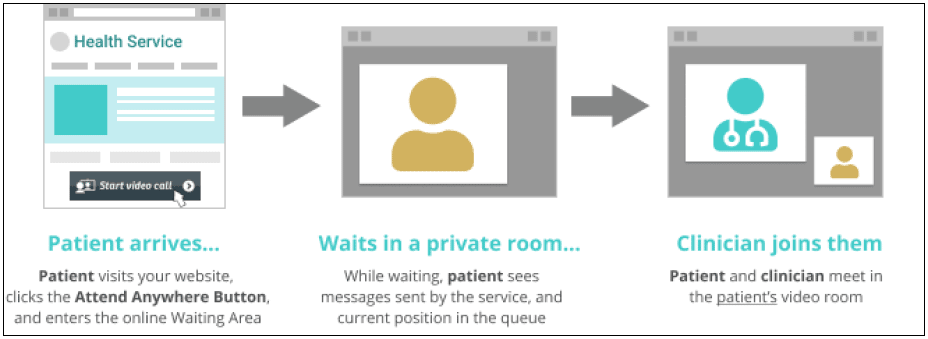
This contrasts with other mainstream video consulting tools that might be described as providing an 'outbound' workflow; in that, the video call is configured around a specific meeting slot which people are invited to join via a unique internet (URL) link, at a particular time:
"[Conventional] video conferencing is outbound, provider-centric, simple workflows. The purpose is to get the person into the slot as quickly as possible. Whereas healthcare isn't like that. Healthcare involves inbound patient-centric workflows. They are complex." (#53, CEO and founder, Attend Anywhere)
An initial licence for Attend Anywhere was procured by the Scottish Government for Scotland in October 2016 and formally launched by the Cabinet Secretary for Health and Sport in December 2016 for initial piloting. This started with a one year 'pathfinder' programme to assess a range of factors including technical feasibility, usability and demand for the video consulting system. Access to the platform was provided free of charge to Health Boards, Health and Social Care Partnerships and Third Sector organisations.
NHS Highland was one of the early adopter sites, where a clinician-manager (a pharmacist by training) with a strong interest in quality improvement thought that a video link might be used to solve the problem of patchy provision of specialist pharmacy services.
"Our problem was in remote parts we can't recruit skilled professionals such as GPs or pharmacists. The question I started with was could we do medication reviews, polypharmacy reviews that kind of thing, via video link?" (#1 Debbie, clinician-manager)
Debbie gained two quality improvement fellowships (one funded by a charity and one by the Scottish Government); she travelled to the USA to see video consulting models in action, and developed her skills in quality improvement and co-design. The pilot pharmacy project, which used Attend Anywhere, was successful in demonstrating improved access to pharmacists and greater convenience for patients in rural areas, and Debbie could see that the model had much wider potential.
"I invited the CEO of NHS Highland to see what we'd done. She was so impressed that she gave me a secondment to develop a video outpatient service. She wanted me to extend what I'd done for pharmacy to cover medical appointments too." (#1 Debbie, clinician-manager)
In January 2018, funding was provided to NHS Highland to establish video clinics in Caithness (in the far north of Scotland). Following approval by NHS Highland of the business case to fund the ongoing service, an additional award was made in July 2018 to support the one-off costs to extend the service across Highland.
Debbie worked with others to undertake detailed service redesign work in some remote areas. A strong, patient-centred branding was seen as important.
"History is as important as geography. [Remote region in NHS Highland] had felt rather low priority. Historically NHS Highland had not engaged much with this particular community. There's a vocal public campaign group; it was set up a few years ago after they shut one of the hospitals, that campaign group is still active. They feel that they're the forgotten community. I said to Debbie, let's take a co-design approach; build some bridges. Debbie is very personable. People like her, even though she works for the [NHS Highland] board. We had to avoid this being framed as "you're gonna cut our services and give us the VC instead". We had to sell it carefully: "use VC to prevent a 6-hour round trip to Inverness". So we held a public meeting, doing a joint presentation and hearing feedback. It's what they called an ideation workshop - it's a bit of a fancy focus group - we did process mapping. We got them to add steps, take away steps." (#50 Pauline, clinician-manager)
Debbie and Pauline's efforts to establish both a central 'hub' (at their base in Raigmore Hospital, Inverness) and 'spoke' centres across NHS Highland from which patients could connect to the service, gradually created a network effect. In other words, because more and more sites were being established, that increased the opportunities for further development.
"If Debbie's set up an NHS Near Me in a new place, we follow her." (#15 Moragh, respiratory consultant providing a remote clinic)
As the national infrastructure grew, local staff considered which remote services were a priority for them. An important driver here, both nationally and locally, was cost. In the Western Isles, for example, a systematic analysis of the budget spent on travel costs revealed a large pot of funding that could potentially be redeployed to support remote services. This issue is discussed further in the section on organisational issues, below.
A final contributor to what one interviewee called a "confluence of drivers" for developing the Attend Anywhere service was positive feedback from patients.
"I thought we'd discover it was as good as face to face and better than nothing. What we actually discovered was patients preferred it. There was a strong patient voice saying it was much better. That changed my thinking." (#1 Debbie, Clinician-manager, Highlands)
Largely because of media coverage, and also via word of mouth from others who had used the service, patients had begun to contact the hospital asking whether they could have their consultation by video.
Interest in Attend Anywhere grew nationally through TEC team outreach activity with Health Boards, taken on and driven locally by clinical champions. In NHS Grampian, for example, Attend Anywhere was introduced in 2017 within the Gastroenterology clinic, led by a consultant looking to improve on the current VC consulting system.
"We had been doing video clinics for a long long time. I had been doing video clinics since 2009, but we used to use the meeting room structure. So patients had to go into a GP surgery or local hospital and then sit in a waiting room, waiting for me to connect from clinic and not knowing if I was running late or what was happening…. And then, coincidentally, I was speaking at the event that Attend Anywhere was launched at, and so we got talking and it was what we were waiting for". (#67, Kevin, consultant gastroenterologist)
Based on the success of the funded Highland programme, as well as the other unfunded developments, the Attend Anywhere Scale-Up challenge was launched in November 2018. The TEC Programme provided scale-up funding totalling £1.6 million, in which Health Boards and HSCPs were provided with up to £150K for programmes of work related to the introduction and scale-up of Attend Anywhere for remote consultations. By mid-2019, uptake and use of Attend Anywhere had expanded across all 14 territorial board areas and the Golden Jubilee National Hospital, as well as a wide range of Health and Social Care Partnerships and Third Sector organisations.
The ways in which service teams use Attend Anywhere to connect with patients and service users varies across settings and specialties, and are summarised under three different models of use:
- Hub-home, in which the clinician connects from the clinic to patient at home (or other locations on personal devices),
- Dyadic hub-spoke, in which the clinician in a specialist 'hub' centre connects to patient in remote 'spoke' health or care site without additional staff member present (e.g. in an unstaffed kiosk)
- Triadic hub-spoke, in which the clinician in a specialist 'hub' centre connects to patient in remote 'spoke' health or care site with an additional staff member (nurse, GP, healthcare support worker (HSW)) present.
These three models were used to support remote consulting of patients within a single Health Board, and for consultations across Health Boards, including the provision of services from mainland hospitals to patients living in the islands, and services provided by the Golden Jubilee National Hospital.
Whilst local evaluations provided valuable information about the uptake and potential benefits of this new service model, it was decided that an independent and comprehensive evaluation was needed to review progress and produce recommendations for the scale-up, spread and sustainability of Attend Anywhere (and similar digital services) going forward.
1.3 Structure of the report
This report presents the key findings and lessons on the uptake and use of Attend Anywhere across health and social care in Scotland. The remaining sections in this report are structured around three main parts:
- The methods, including sampling strategy, data collection and analysis.
- The findings, on the factors influencing adoption, use and scale-up.
- The discussion, focusing on the programme achievement, outcomes and recommendations for future scale-up.
As noted above, the term 'Near Me' is a branding developed by NHS Highland to describe their video consulting services established using Attend Anywhere. Some boards have also adopted the Near Me service name, but have been encouraged to ensure staff members are aware (for training and navigation purposes) that the underlying technology continues to be delivered by Attend Anywhere. For this reason both the terms 'Attend Anywhere' and 'Near Me' are used by interviewees. We use both terms in this report. Some staff outside Highlands thought that Near Me was a different technology. Some staff who talked about Attend Anywhere were actually referring to other video technology (e.g. Cisco Jabber).
Contact
Email: socialresearch@gov.scot
There is a problem
Thanks for your feedback