Attend Anywhere / Near Me video consulting service evaluation 2019-2020: report
This report presents the findings of an external evaluation of the Attend Anywhere / Near Me video consultations service used across health and care services in Scotland
2. Methods
2.1 Locations and sampling
Between August 2019 and March 2020, we collected a range of data comprising ethnographic field notes, interviews, documents and direct observation of technologies (computers, screens, peripherals) and the rooms and spaces they were used in. We purposefully selected a sub-sample of Health Boards for qualitative data collection, in order to analyse data within the organisational context. These were selected to explore variations in geography (urban and rural, islands), clinical context, regional (NHS territorial health boards) and adoption progress. The selection was guided by initial scoping interviews with local project leads at each health board. The geographical areas covered by the NHS Health Boards are shown in Figure 2 below.
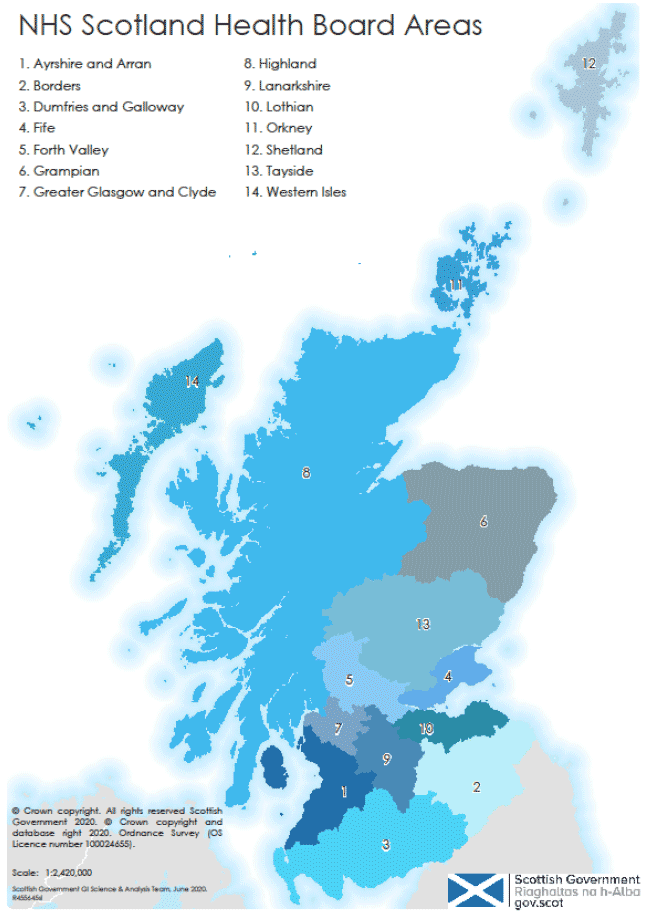
To collect these data, we (JW and TG) undertook a total of 6 visits to Scotland, along with phone and video calls. A total of 11 sites were visited in person (see Table 1).
Table 1: Sites visited during fieldwork
Health Board: Site
NHS Forth Valley:
Falkirk Community Hospital
NHS Highland:
Raigmore Hospital, Inverness
Portree Hospital, Skye
New Craigs Hospital, Inverness - mental health
NHS Grampian:
Aberdeen Royal Infirmary
Woodend Hospital, Aberdeen
NHS Great Glasgow and Clyde:
Glasgow Royal Infirmary
NHS Orkney:
Balfour Hospital, Kirkwall
Dounby Surgery, Orkney
NHS Western Isles:
Uist and Barra Hospital, Benbecula, Western Isles
Western Isles Hospital, Stornoway
We conducted remote interviews with staff and patients who were based at 17 additional sites (see Table 2).
Table 2: Sites for remote interviews
Health Board: Site
NHS Grampian:
2 GP Practices in Aberdeenshire
Rape Crisis Grampian
NHS Greater Glasgow and Clyde:
Hospice in Paisley
Inverclyde Royal Hospital
NHS Highland:
Bedford Hospital, Fort William
Caithness Hospital
GP practice in Fort William
GP practice in Wick
Maternity services in Argyll & Bute
NHS Forth Valley:
Clackmannanshire Community Health Care Centre
Forth Valley Royal Hospital
National Waiting Times Centre:
Golden Jubilee National Hospital
NHS Lothian:
St John's Hospital
NHS Orkney:
GP Practice in Rousay
NHS Western Isles:
2 GP practices, Isle of Lewis
In addition, we met with representatives from Scottish Government, NHS Scotland, industry (Attend Anywhere), the national VC Support team and other national level organisations relevant to the use of video consultations.
In total, we conducted 140 interviews and observed eight remote consultations. These are summarised in Table 3.
| Stakeholder groups | Interviews |
|---|---|
| Doctors | 29 |
| GPs (9) | |
| Consultants (18) | |
| Dual accredited (2) | |
| Nurses | 18 |
| Allied health professions | 22 |
| Physiotherapists (7) | |
| Dietitians (4) | |
| Counsellors (3) | |
| Speech and Language Therapists (3) | |
| Psychologists (2) | |
| Pharmacists (2) | |
| Occupational Therapist (1) | |
| Health support worker | 2 |
| Third sector support worker | 1 |
| Clinician-managers | 4 |
| Non-clinical managers | 14 |
| Admin / support | 8 |
| EHealth/IT staff | 9 |
| Patients | 16 |
| Relatives/carers | 5 |
| National level stakeholders | 12 |
| Total | 140 |
2.2 How we did the interviews
Participants for interviews were identified in one of three ways: direct contact (e.g. clinicians or managers who had been recommended to us by the Scottish Government or who were listed as having a strategic role in video consulting nationally or locally); indirect contact ('snowballing' from an interviewee by asking them to recommend someone else); and social media (via a Twitter call using the key word Attend Anywhere and NHS Near Me). All interviewees gave informed consent either in writing or on tape.
Most people were interviewed individually but some chose to be interviewed in pairs (e.g. consultant plus specialist nurse) or (in three cases) a group of up to five (Macmillan nurses, Colorectal Surgery team and an administrative support team). Staff interviews were conversational in format, with the staff member identifying the key issues they wished to speak about. A prompt list of key topics was used where needed.
The 140 interviews covered 139 interviewees; one person was interviewed twice because they had used Attend Anywhere both as a staff member and as a patient. Of the 140 interviews, 120 were audiotaped with consent; contemporaneous notes were written or typed during all interviews. Interviews lasted from 15 to 45 minutes. Tapes were not fully transcribed (partly for resource reasons and partly to avoid loss of overview, since salient issues were often captured succinctly by making field notes) but we returned to the audiotape to obtain a verbatim record where needed. Six consultations were audiotaped with patient and clinician consent.
Ethical Approval
The study received NHS Research Ethics Committee (REC) approval in June 2019 (ref 19/LO/0550) and NHS Research Scotland Permissions Coordinating Centre (NRSPCC) approval in October 2019, with subsequent local approvals obtained from Research and Development (R&D) departments within each health board.
2.3 Data analysis
Data were pseudonymised by giving each interviewee a different name (gender and ethnically matched). A spreadsheet of real names and pseudonyms was kept on an encrypted hard drive.
Data was managed and stored confidentially and securely at the University of Oxford. We paid strict attention to the General Data Protection Regulations (GDPR) and followed data management and data security policies at the University of Oxford, which can be supplied on request.
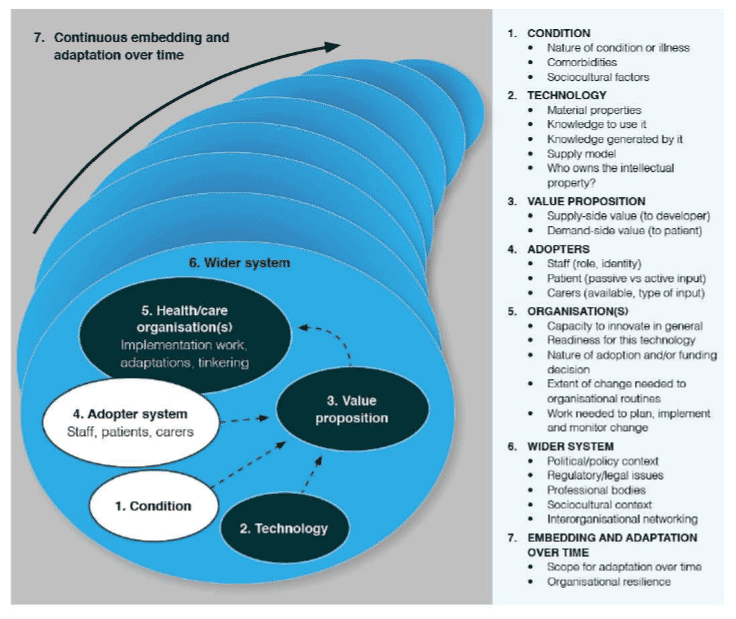
Field notes and typewritten interview notes (along with selected audio transcripts) were organised into an Excel spreadsheet using the 'framework' method, in which each row represents an interviewee (or document) and each column represents a different thematic category. Sections of text are copied and pasted into categories, which were taken from the NASSS framework [1] (specifically, the sub-domains on the right of Figure 3 below). NASSS is a multi-level theoretical model which helps predict and evaluate the success of technology-supported health or social care programmes.
We then considered each thematic category in turn, along with the interactions and interdependencies between these categories. We produced a provisional draft of our findings, broadly structured around the NASSS framework domains, which was circulated to all interviewees and stakeholders who had requested to see it. We amended the draft to correct factual errors. Where people (rarely) disagreed with our interpretation of our findings, we have included their perspective as well as our own.
Contact
Email: socialresearch@gov.scot
There is a problem
Thanks for your feedback