Children and young people - national neurodevelopmental specification: principles and standards of care
Seven standards for services to support children and young people who have neurodevelopmental profiles with support needs and require more support than currently available.
Introduction
The Children and Young People's Mental Health and Wellbeing Taskforce reported in 2019 and recommended that Scottish Government and Partners should: "Develop a Neurodevelopmental Service Specification for use across services in Scotland". The Children and Young People's Mental Health and Wellbeing Programme Board and the subsequent Joint Delivery Board took responsibility for developing these principles and standards of care.
The National Neurodevelopmental Specification ("the Specification") is for children and young people who have neurodevelopmental profiles with support needs and require more support than currently available. These children are often referred to Child and Adolescent Mental Health Services (CAMHS) but do not always meet the mental health criterial described in the CAMHS national service specification criteria.
The Specification complements, and sits within, the Getting It Right for Every Child approach. It reflects the principles of UNCRC, the Universal Health Visiting Pathway, and Ready to Act for Allied Health Professionals.
The Specification aims to ensure that children and families receive the supports and access to services that meet their needs at the earliest opportunity, based on the GIRFEC approach. For many children and young people, such support is likely to be community based, and should be quickly and easily accessible.
Children, young people and their families will be able to access additional support, appropriate for their neurodevelopmental needs, through universal services, such as via the named person, and community based mental health and wellbeing supports and services. Universal services should work closely with professionals working in neurodevelopmental services, relevant health and social care and education services. These professionals should be linked with CAMHS so that children and young people with both neurodevelopmental and mental health support needs can get the additional support they require.
Professionals providing support in neurodevelopmental services will support both universal and additional children and young people's services, including new and enhanced Community Mental Health and Wellbeing Supports. They should do this by providing consultation, advice and training and, where appropriate, supervision of those staff supporting children and young people who have neurodevelopmental needs. These services should be available for all children and young people who are aged 0 – 18 years, and young adults aged 18-24 (and up to age 26 for care experienced people).
Professionals providing support will also provide assessment, formulation, recommendations, and where appropriate and helpful, diagnostic assessment for those children and young people to help them understand their neurodevelopmental differences and support needs. Understanding of support needs can be enhanced by diagnosis but should not wait for diagnosis.
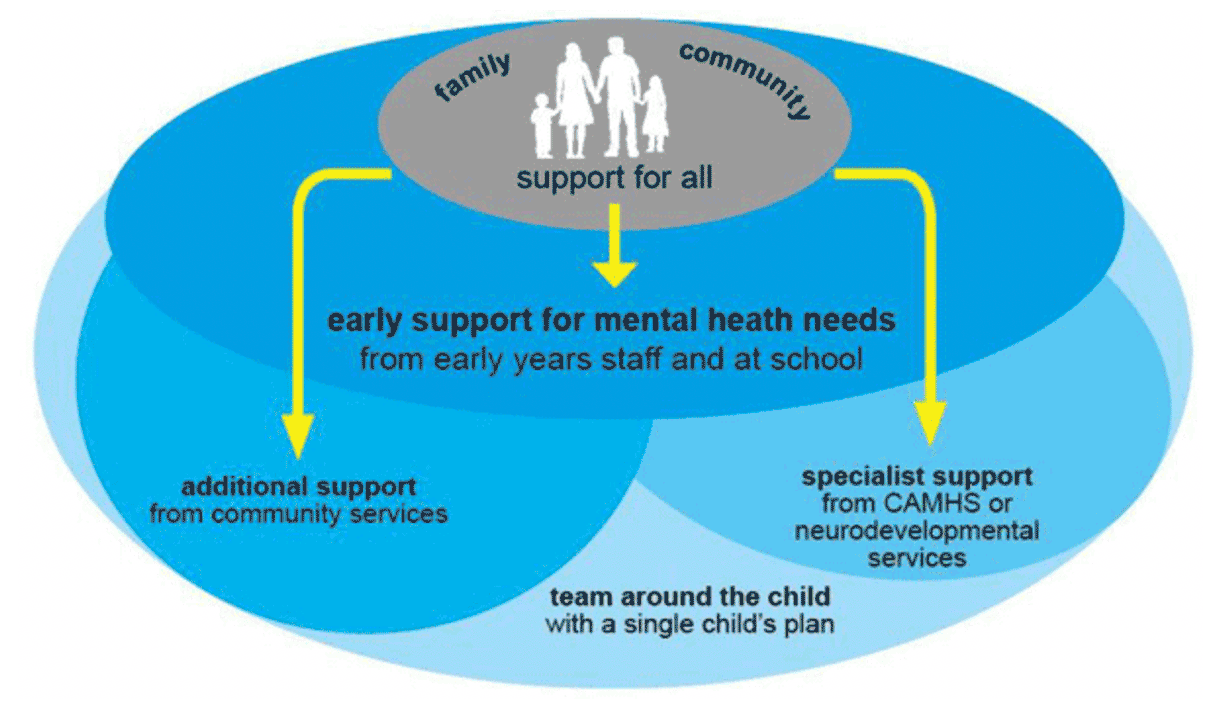
*CAMHS and / or neurodevelopmental service
The National Neurodevelopmental Specification sits along the NHS Scotland National Service Specification for Child and Adolescent Mental Health Services (CAMHS) and the same principles underpin both specifications.
Standards 1 to 7 below provide the minimum standard of care expected in neurodevelopmental services. These standards will be reviewed regularly. Appendix 1 section 6 provides further information about the delivery of the Neurodevelopmental Specification.
The following statements should be read with the preface "Neurodevelopmental Services in Scotland will":
Standard 1: High Quality Care and Support that Is Right for Me
1.1 Publish information in a clear, accessible format about who the neurodevelopmental services are for and how children, young people and their parents/carers can access them.
1.2 Offer a first appointment to all children and young people who have been identified (e.g. by a GP, a Named Person or a Children's Planning meeting) as needing a neurodevelopmental assessment. This first appointment should be as soon as possible and no later than 4 weeks from identification of need.
1.3 Provide support and personalised, meaningful signposting to the child/young person and their family/carers, with informed consent, to access other services within the children and young people's service network, in cases where families' needs are best met elsewhere.
1.4 Conduct a full initial multi-disciplinary community-based assessment, based on the information within the request for assistance, and on the child's plan where completed and available.
1.5 Assure that the member of staff undertaking the initial assessment is appropriately trained, supervised and experienced for the purpose, including identifying strengths, as well as difficulties.
Standard 2: I am fully involved In the Decisions about my Care
Getting It Right for Every Child (GIRFEC) stresses the importance of care planning and collaboration between professionals as the required standard for delivery of children's services in Scotland. All services delivering the Neurodevelopmental Specification should work to the GIRFEC principles on a multi-professional and agency basis.
2.1 Ensure that initial and continuous care planning includes everyone involved in the child or young person's care, e.g. the child/young person and their families/carers.
2.2 Ensure that a single child's or young person's plan is in place for all children and young people receiving support from all services delivering the Neurodevelopmental Specification.
2.3 Ensure the child or young person's plans: are coordinated across agencies, teams and disciplines (using the GIRFEC principles); are clearly written; identify the case holder/care coordinator; and are developed in collaboration with children/young people and families and carers (e.g. The Triangle of Care).
2.4 Provide copies of the child or young person's plan to the child or young person and their families/carers, and, with informed consent, those professionals in other agencies working with the child, young person and families/carers such as social work, schools, children's services providers and primary care (e.g. GPs).
2.5 Build on and contribute to other parts of agreed multi-agency care pathways, including health, education and social work.
2.6 Agree, through a process of shared decision making, the goals of the child, young person and family, and regularly review those interventions and progress towards the goals.
2.7 Respond as early as possible to any indications that children, young people and their families/carers may need support, based on the principle that early intervention can happen at any age.
2.8 Ensure that the rationale for formulation and diagnosis, evidence considered, and decisions made will be fully documented. This should be shared with the child/young person and family/carer in writing as appropriate. Services should consult the child/young person and family/carers on the information to be shared with other agencies e.g. that the assessment has taken place and recommendations within the child or young person's plan.
Standard 3: I will receive High Quality Assessment, Formulation and Recommendations that are right for me
Children, young people and their families may require further neurodevelopmental assessment when they present with additional support needs arising from environmental barriers to participation in daily life and differences in:
- Communication and interaction, and broad social functioning;
- Emotional regulation, and attention;
- Development and intellect;
- Co-ordination and movement.
This further assessment, formulation, recommendations and diagnosis, if appropriate and helpful, will be provided by a range of professionals delivering the Neurodevelopmental Specification (see Appendix 1 for further detail).
Standard 4: My Rights are acknowledged, Respected and Delivered
Services delivering the Neurodevelopmental Specification will take a rights-based approach. Due to the impact of inequality and discrimination on development, physical and mental health, it's important that children, young people and their families know the actions taken to ensure their rights are respected. Children's services organisations are reminded of their duties under the Equality Act 2010 and the Equality Act 2010 (Specific Duties) Regulations (Scotland) to assess the impact on persons who share a protected characteristic in the delivery of this service.
4.1 Be available to all children and young people, taking into account all protected characteristics. Where it is deemed clinically appropriate, alternative services may be established that meet the specific needs of one or more groups within a community. Such services will enhance rather than detract from the minimum standards.
4.2 Deliver the service in timely, age-appropriate, accessible, and comfortable settings, as close to home as possible, meeting the needs of children and young people.
4.3 Ensure that informed consent issues around both sharing of information within the family, with other agencies and around interventions/treatment are clearly explained and documented.
4.4 Ensure that all service developments and/or redesigns are undertaken using the best standards of engagement, including involvement and development with children, young people and their families/carers.
4.5 Provide and act upon a risk assessment for all those children/young people who did not attend/were not brought to their appointment, including implementation of local 'unseen child' protocols and standards. (NB: services delivering the Neurodevelopmental Specification should not close a case due to non-attendance/engagement without discussion with the referrer that the child/young person has not attended/was not brought. See Child Protection Guidance for Health Professionals SG 2013)
4.6 Publish clear re-engagement policies and make them available to referrers, children/young people and families/carers.
4.7 Offer creative and acceptable alternatives to face to face work where the children/young people live at a distance from staff locations e.g. the use of approved technology like Attend Anywhere, or advice to a local professional who is working with the child, young person and their family/carer. This is particularly relevant during the Covid-19 pandemic, however families who struggle to access digital services should not be disadvantaged.
Standard 5: I am fully involved in Planning and Agreeing my transitions
Transitions for children and young people are known to increase risks, particularly for the most vulnerable. The Scottish Government published the Transition Care Planning Guidance in 2018 and this describes the standards required in the planning of good transitions for young people moving to Adult Mental Services. The Principles of Transition guidance is relevant in planning and supporting all transitions for children and young people, including those who have been supported by services delivering the Neurodevelopmental Specification.
5.1 Implement the Scottish Government's Transition Care Planning Guidance. Ensure protocols are in place so that transitions between children and young people's services and other services are robust and that, wherever possible, services work together with the young person and families/carers to plan in advance for transition (this is especially critical in the transfer from children and young people's services to adult services and primary care or other services, e.g. voluntary/third sector).
5.2 Ensure that Transition Care Plans provide children and young people with continuity of care. Ensure that any risks, and any child and adult support and protection concerns, are clearly identified and documented.
Groups of children and young people who are more at risk to adversity during transitions and require robust transition plans include:
- Looked after children;
- Care leavers;
- Young people entering or leaving inpatient care;
- Young people entering or leaving prison;
- Young people in the youth justice system;
- Children and young people with learning disabilities;
- Children and young people with neurodevelopmental disorders;
- Unaccompanied asylum-seeking minors;
- Children and young people with caring responsibilities;
- Children and young people not in education, employment or training;
- Children supported under the Additional Support for Learning Act in particular taking in account the guidance of the review of the Additional Support for Learning Implementation published in June 2020;
- Young parents;
- Young people entering college or university study and, in particular, those moving health board area;
- Children and young people with risk to their mental health and/or comorbidity.
Standard 6: We fully involve Children, Young People and their Families and Carers
The Children and Young People's Mental Health and Wellbeing Model (Diagram 1) has been built on, and informed, by significant involvement of children, young people and their families/carers. In particular, but not limited to, the Audit of Rejected Referrals Report, The Youth Commission on Mental Health and the Children and Young People's Mental Health and Wellbeing Taskforce. Services delivering the Neurodevelopmental Specification will work in partnership with children, young people and their families/carers in all aspects of service design and delivery.
6.1 Provide clear and simple ways for children, young people and families/carers to provide regular feedback or to complain. This feedback should be used to improve the support offered.
6.2 Ensure independent advocacy and support services to the whole system are well signposted and children, young people and families/carers are supported to access the help available.
6.3 Seek feedback from children, young people and families/carers, and other professionals involved with the child or young person with agreement, each time they are supported, and are involved in reviewing progress, goals and outcomes.
6.4 Involve children, young people and families/carers in all decisions/plans that affect them. This includes the design, planning, delivery and review of services.
6.5 Develop leaflets, websites, social media and other communications aimed at children, young people and families/carers in partnership with them, taking into account any barriers to communication and/or accessibility.
Standard 7: I have confidence in the Staff who support Me
No public service can provide quality of care without a commitment to develop and sustain a high quality workforce. The lack of available information about workforce levels, professional mix, skill mix, activity, productivity and outcomes in many children and young people's services, especially those delivering the Neurodevelopmental Specification, was noted in both the Audit of Rejected Referrals report and the Audit Scotland report. Workforce development for services delivering the Neurodevelopmental Specification is a critical element of the delivery of high quality and consistent care across Scotland.
7.1 Provide sufficient staff resources to meet the recommended standards for:
(i) a minimum critical mass for services delivering the Neurodevelopmental Specification, taking into account specific local circumstances;
(ii) demand and capacity model for services delivering the Neurodevelopmental Specification, taking into account wider provision of children and young people's services, ensuring Fair Work standards, and quality of care standards, are met;
(iii) an assessment of neurodevelopmental needs at a local population level.
[NB: Further guidance will follow on Scottish Government's recommended capacity and workforce model for services delivering the Neurodevelopmental Specification, which will include Fair Work Standards, and the Health and Care (Staffing) Scotland Act.]
7.2 Involve, and take into account the views of, children, young people and their families/carers in recruitment and appointment of staff.
7.3 Involve children, young people and families/carers in the design, delivery and/or evaluation of staff training.
7.4 Provide opportunities for team/service away days to build team relationships, facilitate learning and service development. This should be done on a multi-professional /agency basis wherever possible.
7.5 Develop effective relationships and pathways with key local organisations to ensure the holistic needs of children, young people and families/carers are met in a timely and appropriate manner, in line with the GIRFEC National Practice Model and the child or young person's plan (where completed).
7.6 Clearly describe the roles of professionals in services delivering the Neurodevelopmental Specification, and make this information available to a range of audiences in accessible formats. Including the capacity for supporting children, young people and their families/carers, and including administration support, team meetings and supervision.
7.7 Ensure sufficient resources are available for professional, clinical and managerial supervision, including supervision regarding the arrangements for the safety of children and young people.
7.8 Provide opportunities for professionals working in services delivering the Neurodevelopmental Specification to participate in small group case discussions about case goals and outcomes, and on a multi-agency basis where possible. This should also include consultation, where appropriate.
7.9 Include children, young people and families/carers' views and experiences in professional appraisals for staff working in services that deliver the Neurodevelopment Specification, and provide systems and process to gather views appropriately, with consent for this purpose.
7.10 Ensure systems and processes are in place (IT and others) to monitor, report on, analyse and respond to: fluctuations in the local planned capacity calculations; and to report on outcomes of interventions.
7.11 Ensure staff working in services which deliver the Neurodevelopmental Specification are supported to grow and develop the necessary compassion, values and behaviours to provide person-centred, integrated care. Ensure staff are supported to enhance the quality of experience through education, training and regular continued personal and professional development that instils respect for children/young people and families/carers.
7.12 Ensure the multi-disciplinary workforce capacity, current and future, is sufficient ensuring an appropriate skill mix and scope of practice to deliver a range of recommended evidence-based interventions within the recommended delivery and capacity model.
Contact
Email: ceu@gov.scot