Healthcare quality strategy for NHSScotland
Information about how we are going to deliver the highest quality healthcare services to people in Scotland.
4. Our Response
The Aim
The ultimate aim of our Quality Strategy is to deliver the highest quailty healthcare services to people in Scotland, and through this to ensure that NHSScotland is recognised by the people of Scotland as amongst the best in the world.
'...the quality of healthcare services delivered by NHSScotland is
recognised by the people of Scotland as amongst the best in the world.'
This aim will be achieved by working from the bottom up, and will build on:
- A single and shared understanding and definition of what we mean by high quality healthcare;
- Scotland's reputation for professionalism, clinical excellence and leadership - for example, pioneering the use of quality guidelines through SIGN, Best Practice Statements, knowledge exchange and leading in the development of the use of clinical data;
- The early success of the Scottish Patient Safety Programme which has marked Scotland as a world leader in developing a national patient safety programme;
- Increasing value being placed on the quality of the experiences of the people who use healthcare services;
- The opportunity for strong leadership and delivery which our integrated NHS system provides;
'...mutually beneficial partnerships with their families
and carers and those delivering healthcare services.'
- A whole system anticipatory approach to delaying or preventing, and slowing the progression and impact of, ill-health;
- Cross-system quality improvement led by engaged clinicians working collaboratively across disciplines for example in Managed Clinical Networks;
- Staff ownership and enthusiasm for improving quality and safety;
- Public sector partnership working;
- High quality partners in the independent and voluntary sectors;
- Patients' motivation to be involved in mutually beneficial partnerships with their families and carers and those delivering healthcare services;
- Scotland's focus on collaboration and professional values;
- The range of existing national and local initiatives and programmes already in place; and
- A focus on each individual's wider needs, to achieve the best possible outcomes, by working with them to help them manage their own health.
We will need action at all levels if we are to succeed. We will need a clear line of sight from national strategies through to individual behaviours. In order to achieve this, our approach will be designed to be:
- Patient-based: reflecting the uniqueness of the individual, their experience of their health, illness and healthcare, and enabling them to share in decision- making about their care, to manage their own health, and illness though support and access to advice and information for them, their families and carers;
- Staff-based: enabling people working in and with NHSScotland to use their skills, further improving staff experience, staff engagement, building capacity, providing support and making the right thing the easiest thing to do;
- Systems-based: simplifying the policy/delivery landscape, aligning and re-enforcing our shared priorities, and providing the appropriate balance between performance management and continuous improvement; and
- Partnership-based: NHSScotland working with public and third sector partners, staff, independent contractors, patients and carers.
The Quality Ambitions
In order to be recognised as having world-leading healthcare services, we need to set out a clear set of ambitions with related measurable and achievable objectives (interventions) on which we can report progress.
Better Health, Better Care was based on the Institute of Medicine's six dimensions of quality. These six dimensions will remain central to our approach to systems-based healthcare quality improvement:
- Person-centred : providing care that is responsive to individual personal preferences, needs and values and assuring that patient values guide all clinical decisions;
- Safe : avoiding injuries to patients from healthcare that is intended to help them;
- Effective : providing services based on scientific knowledge;
- Efficient : avoiding waste, including waste of equipment, supplies, ideas, and energy;
- Equitable : providing care that does not vary in quality because of personal characteristics such as gender, ethnicity, geographic location or socio-economic status; and
- Timely : reducing waits and sometimes harmful delays for both those who receive care and those who give care.
We have a clear and shared vision for high quality healthcare services in Scotland which is derived from what people have told us they want and need:
- Caring and compassionate staff and services;
- Clear communication and explanation about conditions and treatment;
- Effective collaboration between clinicians, patients and others;
- A clean and safe care environment;
- Continuity of care; and
- Clinical excellence.
By focusing on what really matters to people, and through our approach to systems-based healthcare improvement based on the Institute of Medicine's six dimensions of quality, we will raise the quality of healthcare from the current high standards to world-leading by concentrating our priority action on achieving the following ambitions.
'...By focusing on what really matters to people...
we will raise the quality of healthcare from the current high
standards to world-leading... '
The Quality Ambitions |
|---|
Mutually beneficial partnerships between patients, their families and those delivering healthcare services which respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making. There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate, clean and safe environment will be provided for the delivery of healthcare services at all times. The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit, and wasteful or harmful variation will be eradicated. |
Our Commitment to Equality
NHSScotland is committed to understanding the needs of different communities, eliminating discrimination, reducing inequality, protecting human rights and building good relations by breaking down barriers that may be preventing people from accessing the care and services that they need, as well as meeting the legal duties in relation to age, race, disability and gender. It aims to address inequalities by recognising and valuing diversity, promoting a person-centred approach and involving people in the design and delivery of healthcare.
'...recognising and valuing diversity...'
There are strong linkages between some of the key actions required and being taken forward to address health inequalities in Scotland, and proposed drivers of our quality strategy. In particular the person-centred and clinical effective drivers (specifically through long-term conditions) have the potential to address the health problems of many of those who carry a disproportionate burden of ill-health in our communities. Each of the aligned and integrated national programmes, intiatives and interventions pursued in support of achieving the three Quality Ambitions will require to be fully assessed in terms of their impact on equalities through a Health Inequalities Impact Assessment ( HIIA), which includes mandatory Equalities Impact Assessment ( EQIA). Through this we will ensure that the Quality Strategy optimises its impact on reducing inequality across Scotland.
The Improvement Interventions
Person-centred
'...every patient encounter as an opportunity to improve health.'
We have a number of programmes and pilots in operation at present which are aimed at putting people at the centre of care and at supporting the development of relationships between NHSScotland staff, patients and carers which result in shared decision-making, better experiences and outcomes for patients and carers, and greater job satisfaction for staff. For example, there is the Patient Experience Programme (Better Together) (currently focusing on inpatients, general practice and long-term conditions), the S elf Management Strategy, Keep Well and Well North, Living and Dying Well, the Delivering Patient-centred Care Programme underpinned by ' Curam', the carer information strategies, Scotland Cares and the other work streams underway to develop further the caring and enabling aspects of the Nursing, Midwifery and Allied Health Professions. There is also the work to enhance the performance of NHSScotland as a Health Promoting Health Service, using every patient encounter as an opportunity to improve health.
'...this and other work will be brought together more coherently,
visibly and consistently and integrated with new developments...'
This strategy sets out how this and other work will be brought together more coherently, visibly and consistently and integrated with new developments such as the work on supporting 'relationship-based care', and shared decision making tools (for which there is strong evidence of improved patient choice, better experience and lower utilisation of expensive interventions). We will also ensure that our investment in our capital infrastructure provides the appropriate environment to support high quality healthcare experience and outcomes.
We will implement a generic and appropriate approach for measuring individual patients own assessments of the quality of the outcome of their healthcare episode, whether in primary, secondary or emergency care, so that a patient-based measure of health outcomes and experience can also be used to drive improvement in the quality of healthcare services.
In order to capture patients' assessment of their relationship with the healthcare professional supporting them, in such a way that it can be used to inform improvement, a measurement technique known as the Consultation and Relational Empathy ( CARE) measure has been developed in Scotland. The CARE measure has been well validated with doctors, both with GPs in primary care and consultants in secondary care. We will pursue the introduction of the use of the CARE measure in all clinical appraisals and with other healthcare professionals. We will be able to use these measures to highlight action needed to ensure equity in terms of health outcomes and experience. Other tools to support staff, patients and carers in achieving the mutually beneficial partnerships we want will be developed, where appropriate, including outcomes approaches such as Talking Points.
Our initial improvement interventions will be:
- Implementation of the new Self-Management Strategy
- Implementation of the Patient Rights (Scotland) Bill in 2011;
- Action in response to the first results of the Better Together Patient Experience surveys;
- Collection of appropriate data to measure patient reported outcomes ( PROMS);
- Shared decision-making defined, supported and measured;
- Implementation of the CARE approach in primary and community care;
- Building on the principles of the Quality and Outcomes Framework ( QOF) to maximise quality in the other contractor areas;
- Enhanced management of falls, pressure area prevention and nutrition;
- Improve resources to support better health literacy;
- Develop evidenced interventions to support improved person-centredness;
- Develop a programme of action to ensure that peoples' equality needs are gathered, shared and responded to across health services by Summer 2011; and
- Introduce interventions to improve staff experience.
Making It Real - Lothian Community Nursing and long-term conditions |
|---|
Before Patient/person - Older people with chronic obstructive pulmonary disease at home and having difficulty in identifying signs and how to manage their symptoms. Often housebound. Staff - aware that these older people need access to specialist nurses. Actions Touch screen technology is installed in the homes of people with chronic obstructive pulmonary disease. After Patient/person - Older people have found the equipment easy to use and feel supported in self management of their condition. Staff - The nurses assess and coach people, monitor trends, refer when appropriate and enourage self management. System - Technology enables vital sign collection and prompts. Enables video conferencing connecting people to specialist nurses who monitor their care remotely. |
Safe
The Scottish Patient Safety Programme is now making a significant impact across the NHS in Scotland. It represents an ambitious effort to make substantial safety improvements for the benefit of patients across a health system, and has gained significant ownership and buy-in from NHS staff. It aims to implement a set of key evidence-based interventions uniformly across all acute hospitals in Scotland, and to deliver significant reductions in premature mortality and in adverse events. We will roll out the successful focus on patient safety into a range of other care environments, and will develop appropriate approaches to improving safety in primary care and in mental health involving the contribution of both patients and staff.
'We will roll out the successful focus on patient
safety into a range of other care environments...'
NHSScotland's eHealth Strategy launched in June 2008 is focused on using information to improve quality. Good progress is being made in developing information technology and improving the business processes necessary to ensure that we get benefit from our investment in eHealth. The aim is to build a 'virtual patient record' that will contribute towards safety, continuity of care and collaborative decision making. With additional investment planned for 2010/11, key eHealth contributions to better quality care will include:
- Development of the Emergency Care Summary ( ECS) and the Emergency Palliative Care Summary to enable, for example, their use in planned care as well as emergency care and extend as the Electronic Care Summary;
- Implementation of the 'clinical portal' programme to enable better sharing of patient information;
- Continued development of the 'patient portal' to allow patients access to information about their health; and
- Work on ways to bring clinical data to frontline staff.
Finally, we will ensure that the Scottish Patient Safety Programme, combined with our comprehensive HAI agenda, delivers change on the ground, so frontline staff can deliver a higher level of service to patients.
Our initial improvement interventions will be:
- Accelerate roll out of the Scottish Patient Safety Programme in acute care, reducing hospital mortality and harm;
- Implement patient safety programmes for primary care and mental health;
- Accelerate medicines reconciliation across all transitions of care;
- Ensure synergy with the work of the HAI taskforce to secure further reductions in infection; and
- Extend the Electronic Care Summary and make widely available.
Making It Real - Anaesthesia and intensive care, Glasgow Royal Infirmary |
|---|
Before Patients and public - All adverse events in Intensive Care Unit ( ICU) increase duration of ICU stay. Actions Implementation of Scottish Intensive Care Society Ventilator Associated Pneumonia Prevention Bundle using real time data to measure improvement, and improvement in delivering interventions that are known to be effective. After Patients and public - reduction in ventilator associated pneumonia and other infections, a reduction in average length of stay in intensive care by a day and a half. System - more efficient use of highly specialised intensive care facilities and improved reliability at delivery of effective interventions and reduced variation. |
Effective
We will continue to focus on primary prevention of health problems, shifting the balance of care to prevention and early intervention. We will identify and reduce inappropriate variation in clinical practice, and in provision of care packages and treatments across all healthcare pathways so that the best care is consistently provided by the right person in the appropriate place at the right time. We will also implement our proposals to improve standards of care for long-term conditions and acute care in hospital, in the community and through supported self-management. Through these measures we will ensure that clear and challenging quality outcomes and success indicators are established for services for older people, and people with long-term conditions, and that there is leadership and capacity to support improvement. Much of the work required to improve quality and ensure sustainability of services for people with long-term conditions will involve primary and community care services, and supporting the drive to shift the balance of care away from hospital services towards the community.
Shifting the balance of care and enhancing prevention and anticipatory approaches has the potential to make services more efficient and sustainable by avoiding the development of disease and unnecessary hospital admissions, reducing avoidable days in hospital and improving patient experience. However, where hospital admission is required, we will ensure that patients receive high quality, evidence-based healthcare from well trained and empowered staff. We will support those with the most complex needs by ensuring that each of them has an integrated and shared Anticipatory Care Plan in place. Making this aspiration a reality will require a firm commitment to excellent cooperation and communication throughout the different stages in the care journey.
'...enhancing prevention and anticipatory approaches
has the potential to make services more efficient and sustainable by
avoiding the development of disease and unnecessary hospital admissions...'
We will continue to deliver our policy of reshaping the medical workforce so that the medical contribution is delivered predominantly by trained doctors, rather than doctors in training, and in collaboration with the extended multi-professional clinical team with the appropriate skill mix and capability.
We will also ensure that NHSScotland staff are properly supported, through new development packages where necessary, to provide anticipatory health and healthcare advice and support to people and their carers, tailored to the social, psychological and economic circumstances of their lives.
We will support a step change in health literacy across the whole population, taking full advantage of existing and new approaches to communications, technology and resources to ensure that everybody has access to the information and advice they need, when they need it, to support them to maintain their health and
wellbeing, manage ill-health and have the confidence to participate fully in shared decision-making.
'...a step change in health literacy across the whole population... '
With NHSScotland assets currently valued at approximately £5bn it is important that these assets are effectively managed to ensure the availability of appropriate, clean and safe healthcare environments which are central to the delivery of high quality healthcare. We will ensure that the NHSScotland Property and Asset Management Policy establishes an aligned approach to arrangements required by Boards for the safe and effective operation of their assets including premises, medical equipment vehicles and IT.
Our initial improvement interventions will be:
- Preventative and anticipatory approaches, building on and extending initiatives such as Keep Well/Well North, alcohol brief interventions and smoking cessation;
- Implement the Long-term Conditions Action Plan;
- Initiating a process of refreshing the suite of care pathways in close collaboration between secondary and primary care with clear prioritisation;
- Introduce and share Anticipatory Care Plans for 5 per cent of the population most at risk of hospital admission;
- Implement the major national strategies; Better Cancer Care, Mental Health Primary Care, Heart Disease and Stroke, Dementia and Living and Dying Well;
- Establish the appropriate healthcare skills and roles required to deliver high quality healthcare, and, through the use of the NHSScotland Career Framework and local/national workforce planning, establish plans to reshape the workforce accordingly;
- Ensure all our GP enhanced services are fit for the purposes of this strategy;
- Implement the Strategic Options framework for emergency response in remote and rural areas;
- Leading Better Care implemented across all Boards by December 2010;
- Implement the Releasing Time to Care approach across acute and community teams in all Boards; and
- Ensure high impact Efficiency and Productivity approaches are implemented reliably - (e.g. disinvestment, reduce harmful and wasteful variation ( GP referrals, hospital length of stay, prescribing etc)).
Making It Real - Clinical Quality Indicators |
|---|
Before Patients and public - variation in experience, care and outcomes around nutrition, pressure areas and falls. Staff - no reliable local or national measure of the impact of nursing and midwifery care on quality. Actions A core set of evidence-based Clinical Quality Indicators ( CQIs) were developed for nursing to support the measurement of the quality, safety and reliability of care. The initial focus was on CQIs applicable to inpatients, in a variety of specialties, on: food, fluid and nutrition; falls; and pressure area care. After Patients and public - evidence, for example in one NHS Board, that food, fluid and nutrition compliance is up from 50 per cent to 95 per cent, pressure area care from 60 per cent to 80 per cent, and falls compliance from 64 per cent to 66 per cent, and average compliance for all three CQIs has risen from 70 per cent to 90 per cent - real improvements for patients. Staff - Better evidence, owned and used by ward staff to identify and support improvement actions, leading to better job satisfaction. |
Quality Infrastructure
'...identify and remove any hurdles and barriers...'
A key requirement to realise our Quality Ambitions is for our systems and actions to be integrated and aligned across the whole NHS system. We need to identify and remove any hurdles and barriers presented by the current approaches to policy development and delivery across Scottish Government and NHSScotland. Responsibility for taking this action lies ultimately with NHSScotland Senior Management and with Scottish Government Ministers and senior officials.
'...Quality Alliance to involve all key stakeholders and
oversee the implementation of the Quality Strategy... '
We will establish a new Quality Alliance to involve all key stakeholders and oversee the implementation of the Quality Strategy, and to ensure whole-system integration and alignment. The initial actions required include a simplification of the policy and delivery landscape with the introduction of a new approach to ensure that existing and new initiatives are appropriately aligned with the Quality Strategy Ambitions, and that their impact on these ambitions is transparently communicated and properly measured and monitored. There will be a more robust review of HEAT, ensuring that we have a set of national targets which is clearly aligned and evidence-based in support of the Quality Ambitions.
We propose that the new Quality Strategy will extend to cover the activities of NHSScotland which are primarily focused on preventative and anticipatory care and are in pursuit of reducing health inequalities and in improving health. It will form the basis for our relationship with independent contractors.
We further propose that the Quality Strategy provides a basis for NHSScotland to work with community planning partners and the third sector in securing progress towards the Quality Ambitions and the outcomes agreed locally and nationally through the Single Outcome Agreements and the National Performance Framework.
'...ambitious leadership and strong professional values... '
The central purpose of the NHSScotland Quality Strategy is to create high quality, person-centred, clinically effective and safe healthcare services. Delivering this purpose requires ambitious leadership and strong professional values, supported by a robust and effective governance framework.
Strong and well developed governance arrangements will provide a framework of leadership, assurance and measurement in order to ensure transparency. This will mean NHS Boards need to ensure that governance activity at corporate level (including staff, financial and clinical governance) provides assurance that the organisation has a focus on quality; and that frontline staff, through a care governance approach, deliver care which aligns with our ambitions.
'... NHS Boards need to ensure that governance activity...
provides assurance that the organisation has a focus on quality...'
Professional leadership, clinical engagement and the collective energy of all staff will be vital to Care Governance. Together we can cement the connection between improving our performance in all dimensions of quality with, and through, the clinical practice and individual contribution of every health professional in NHSScotland. Care Governance will explore how this dynamic process can be strengthened and provide mechanisms for robust assurance on healthcare quality from 'point of care' to Board.
Our initial improvement interventions will be:
- Establish Quality Ambitions by May 2010;
- 2011/12 HEAT targets aligned with Quality Strategy by October 2010;
- Quality Measurement Framework underpinning Quality Ambitions with related high-level outcome indicators agreed by October 2010 - including 'early alert' Quality Scorecard;
- Establish governance responsibilities and procedures to support quality, and minimise risks;
- Ensure that national and local audit programmes support the development of appropriate indicators of quality, rigorous peer review and local action to address inappropriate variations in care;
- Develop, support and make best use of the skills, knowledge accountability and professional leadership of our staff to provide assurance of care quality at all levels; and
- Develop the Quality Improvement Hub, reflecting a new partnership for improvement between NHS National Services Scotland ( NSS), NHS Quality improvement Scotland ( QIS), NHS Heath Scotland, NHS National Education for Scotland ( NES), and the Scottish Government Health Directorates Improvement and Support Team ( IST).
The Quality Measurement Framework
'Measurement is an important tool for driving large-scale improvement.'
Measurement is an important tool for driving large-scale improvement. This requires the use of appropriate measures for various purposes (e.g. improvement activity, performance management and tracking progress on outcomes). We are committed, through the Quality Strategy, to simplify and streamline the range of measures we use across NHSScotland to ensure that we achieve maximum value from our investment in data collection and measurement. Ensuring that there is a shared understanding of the types of measures involved, and how they relate to the achievement of the Quality Strategy's Ambitions, is critical.
We therefore propose to develop a Quality Measurement Framework that supports our shared vision of healthcare quality as described by the three healthcare Quality Ambitions. These clearly underpin the Scottish Government's Purpose and National Outcomes.
'...simplify and streamline the range of measures we use across
NHSScotland to ensure that we achieve maximum value from our investment
in data collection and measurement.'
It is proposed that progress towards the three Quality Ambitions will be assessed nationally by reference to 12 Quality Outcome Measures. These measures will be based on a combination of patient and staff reported experiences and outcomes as well as measures of patient safety and clinical effectiveness. The detail of the measures is yet to be developed and agreed, but table 1 provides some examples of measures that will be considered. The Quality Outcome Measures will also contribute to the Quality Scorecard, a key tool for the NHS Boards to use to assess quality of care, and to provide an early warning of any potential quality issues.
The national targets for NHSScotland ( HEAT targets) will be aligned to the Quality Ambitions, and will set out our agreed areas for specific accelerated improvement each year.
The Quality Measurement Framework also allows for supplementary local and national indicators that will underpin progress towards our Quality Ambitions, for example, the measures contained in the patient safety extranet.
By setting out the Quality Measurement Framework and ensuring a common understanding of healthcare quality we will be able to make sure that all of our measurement, performance and reporting systems converge and align. It is intended that this will include the National Performance Framework, Single Outcome Agreements, HEAT and national data systems (held by ISD), as well as systems which Boards use in their own local areas (e.g. local governance, improvement and performance indicators).
Proposed Quality Measurement Framework
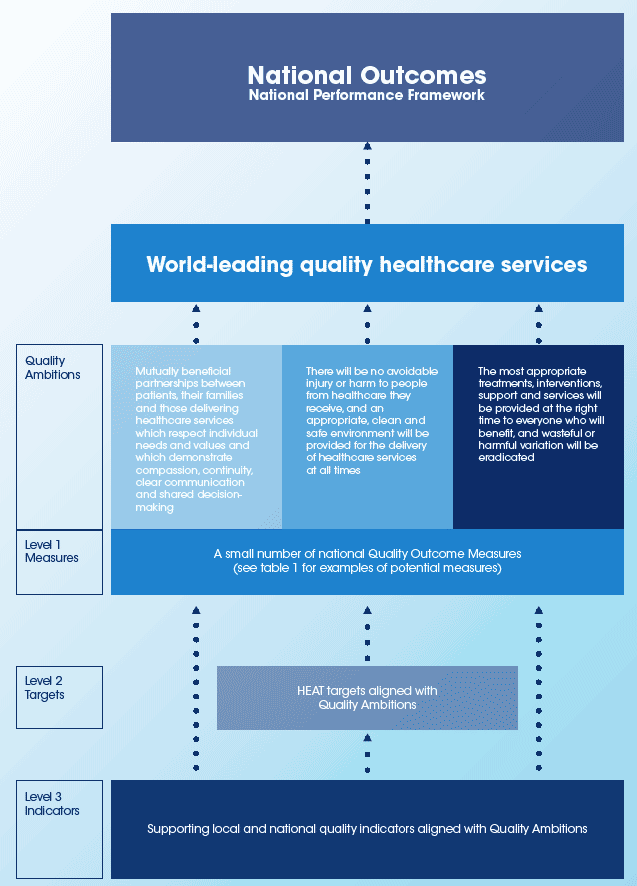
Quality Outcome Measures
The Quality Outcome Measures:
- will reflect national progress towards the three Quality Ambitions, but will not be subject to specific targets;
- include a combination of patient-based, staff-based and system-based measures to cover the three main levers for change;
- are being derived in close collaboration with colleagues across NHSScotland; and
- provide a line of sight to the National Outcomes and the National Performance Framework.
Table 1 introduces the 12 potential national Quality Outcome Measures. Further analysis and consultation will take place with a view to agreeing them by October 2010 for implementation alongside the related set of HEAT targets for 2011/12. Some measures are likely to require development over the longer term.
Table 1: Potential National Quality Outcome Measures
Potential measure |
Rationale |
Patient/ staff/ system measure |
|---|---|---|
Healthcare experience |
People's experience of our services is important. This is also an indicator in the National Performance Framework for which methodology has still to be developed. Ideally, this measure would include feedback from both patients and carers. Patient experience of various aspects of quality can be assessed from current surveys. Further consideration around how to capture the experience of carers will be required and existing information sources will be explored. |
Patient |
Staff experience |
Staff survey results provide another angle on the person-centredness of the NHS. Survey questions relate to several of the quality dimensions. Again, these could be separate measures or combined into one measure. |
Staff |
Staff attendance |
This indicator supports several dimensions, including efficiency and person-centredness. In addition, a reduction of staff absence could be expected to contribute to improved safety, timeliness and effectiveness. |
System |
Healthcare Associated Infections |
Key priority within the strategy. Indicates a cleaner environment and reduction in avoidable harm. Infections can result in longer stays in hospital, reducing clinical effectiveness, efficiency and affecting timeliness. |
System |
Emergency admissions |
This outcome indicator should represent a shift in the balance of care. It could demonstrate effectiveness of anticipatory and planned care. Patients are supported to remain at home where safe and appropriate. This measure should, therefore, reflect improved partnership working with social care, carers and the voluntary sector. |
System |
Adverse events |
This directly contributes towards the aim of no avoidable injury or harm. Adverse events result in poorer clinical outcomes and less effective use of resources. Therefore, this measure supports effectiveness and efficiency as well as safety. |
Staff |
Hospital Standarised Mortality Rate ( HSMR) |
National reduction in HSMR should reflect work in individual hospitals to review mortality under the Scottish Patient Safety Programme and reflect reduction in serious adverse events and infections |
System |
Proportion of people who live beyond 75 years |
This outcome is intended to reflect the range of improvements right through the healthcare system from prevention to treatment. |
System |
Patient Reported Outcomes |
Indicates whether interventions have been effective from the point of view of patients. It is proposed that there is potential for, through time, an aggregated measure of PROMS based on local feedback to be developed. A project is being initiated by NHSQIS, working in partnership with the Universities of Stirling and Dundee & The Alliance of Self Care, to develop a national toolkit for this. As part of this project, the potential for this type of measure will be investigated. This is therefore a longer-term aim. |
Patient |
Patient experience of access |
Shows the patient point of view as to whether they have been able to access the care they needed, when they needed it. |
Patient |
Self Assessed General Health |
Self-assessed health will be a longer-term measure that will allow us to assess the effectiveness of a wide range of initiatives. Will reflect all quality outcomes including person-centred, timeliness, efficient, clinical effectiveness and safe. |
Person |
Percentage of last 12 months of life spent in preferred place of care |
Captures the outcomes of Living and Dying Well (a national action plan for palliative and end of life care in Scotland) i.e. use of tools to identify and assess people with palliative and end of life care needs; delivery and coordination of care across care settings to address those needs by consistent access to, and review of, anticipatory care plans (including palliative care summary and Do Not Attempt Cardio-pulmonary Resuscitation ( DNACPR). |
System |
There is a problem
Thanks for your feedback