Leading Better Care: Report of the Senior Charge Nurse Review and Clinical Quality Indicators Project
Results of the Senior Charge Nurse Review and Clinical Quality Indicators Project conducted by the Scottish Government and professional advisers.
Section 3
Clinical Quality Indicators Project
Background
The background to this project is the Audit Scotland report Planning Ward Nursing - Legacy or Design? (Audit Scotland, 2002). This report emphasised that despite high numbers of nursing and midwifery staff in the NHS workforce, there was limited information available to compare nursing numbers, costs and impact on quality. Among its recommendations were:
- NHSScotland should develop and agree clinical quality measures that focus on continuous improvement
- NHS boards should review the quality indicators regularly and take action when problems arise.
This led to a pilot project commissioned by the Chief Nursing Officer Directorate and hosted by NHS Quality Improvement Scotland ( NHSQIS). This project tested the feasibility of developing clinical indicators for nursing and midwifery and the outcomes were published in The Impact of Nursing on Patient Clinical Outcomes ( NHSQIS, 2005).
When Audit Scotland published a follow-up report in 2007 (Audit Scotland, 2007) they recognised the progress that had been made in developing quality indicators but noted that:
"Boards are still measuring quality in a variety of ways and challenges [remain] in working towards a national system of quality indicators."
The recommendations of the Impact of Nursing on Patient Clinical Outcomes report have been progressed through the Clinical Quality Indicators Project, which has developed a core set of clinical quality indicators ( CQIs) in collaboration with NHSQIS, ISD and NES.
Objectives of CQI Project
The objectives achieved by the project were:
- develop robust quality indicators that demonstrate the nursing and midwifery contribution to care
- develop an electronic data-capture and analysis system to enable monitoring of CQIs in NHS board areas to inform continuous quality improvement
- use the agreed indicator set in the development phase of the Review of the SCN Role
- develop a model to ensure continuous review and development of the CQIs.
This project was carried out in collaboration with five NHS boards _ NHS Fife, NHS Forth Valley, NHS Grampian, NHS Greater Glasgow and Clyde and NHS Lanarkshire. The aim was to test and refine the CQI set in conjunction with the Framework for the SCN Role.
All remaining NHS boards were involved in the development phase through releasing a clinical facilitator to work two days per week on the projects. A national network of clinical facilitators was established to ensure shared learning and strengthen the outcome of both projects.
Challenges of CQI Project
The Impact of Nursing on Patient Clinical Outcomes report highlighted the substantial challenges posed to practitioners by the lack of a national approach to measuring and improving quality in nursing and midwifery services. This has led to a situation in which nationally there are:
- no comparative data with which to measure the impact of nursing numbers on costs and quality
- no agreed quality measures that focus on continuous quality improvement
- no measure of impact of available evidence on practice and outcomes.
Audit Scotland acknowledged that, as summarised in the NHSQIS report:
"this is a complex area and many confounding factors exist that make it difficult to isolate and clearly identify the impact made by nurses."
In this challenging context, the CQI Project has made significant progress in establishing CQIs for nurses and adopting a model for progressing CQIs in other areas of nursing and midwifery.
Developing robust quality indicators
The literature reviews conducted to inform the NHSQIS report and Measuring and Reporting the Quality of Health Care: Issues and Evidence from the International Research Literature review (Davies, 2006) were used to inform the development of CQIs for nursing and midwifery. This process determined that the CQIs would focus on continuous improvement rather than performance management.
Their development has also been informed by activities carried out as part of the projects' stakeholder engagement ( see Figure 1). This reinforced the requirement to develop CQIs across the six dimensions of quality defined in Better Health, Better Care (Scottish Government 2007): safe, effective, efficient, patient-centred, timely and equitable health care. Stakeholders also identified priorities for indicator development.
The literature searches and stakeholder engagement informed the next stage of the project. The three key outcomes were that CQIs should:
- focus on continuous quality improvement rather than performance management
- include process indicators which measure aspects of nursing care such as assessment and interventions
- include nursing-sensitive patient outcome measures, which improve in the context of the quality of nursing care.
Developing quality indicators is complex and stakeholder consensus decreed that the initial focus would be on four CQIs that would be applicable to in-patients in a variety of specialities, including acute hospitals, old-age psychiatry, rehabilitation areas and community hospitals. They were:
- food, fluid and nutrition
- falls
- pressure ulcer prevention
- monitoring and observation.
The indicator development also included collecting data on the profile of staffing in the ward to reflect not only the process and outcomes of care in the CQIs above, but also the structure of care as indicated by the supply and skill level of nursing staff.
The dataset for the ward profile was developed in collaboration with the Nursing and Midwifery Workload and Workforce Planning Programme commissioned by the Chief Nursing Officer Directorate. The profile provides information about effective rostering, sickness/absence data and information on use of additional staffing.
Any systematic approach to improving quality should include plans to monitor, evaluate, maintain and embed change into practice. The eQIPS system has been designed around a simple model that will support clinical teams to develop, test, implement and evaluate change.
Progress on electronic data-capture to support improvement
One of the objectives of the project was to develop an electronic data-capture and analysis system to support senior charge nurses in continually monitoring and improving practice. Following consideration of the options, it was agreed that the Chief Nursing Officer Directorate would work with the Information and Statistics Division ( ISD) to develop a national data-capture and reporting system. This would be underpinned by the eHealth-aligned clinical information standards, as developed by the National Clinical Dataset Development Programme ( NCDDP) (see: http://www.isdscotland.org/isd/4998.html) . This has resulted in a unique national electronic Quality Improvement Programme for NHSScotland ( eQIPS).
The indicator sets have been developed from the best evidence available and the system is based on the Model for Improvement (Langley et al. 1996), a simple but powerful tool for accelerating improvement that has been used very successfully by hundreds of health care organisations in many countries. It is also the methodology used by many of NHSScotland's national programmes.
Two parts of the Model for Improvement are incorporated into eQIPS:
- three fundamental questions: what are we trying to accomplish; how will we know that a change is an improvement; and what changes can we make that will result in improvement; (these can be addressed in any order).
- the Plan-Do-Study-Act ( PDSA) cycle to test and implement changes in real work settings, which guides the test of a change to determine if the change is an improvement.
Development of agreed indicator set in the development phase of the Review of the SCN Role
It was identified that the act of measuring had a positive impact on what was being measured. This is demonstrated in the case study below from one of the development sites, which also highlights the synergy between the SCN Review and the CQI Project.
Case Study
At the start of the development phase of the project, one of the senior charge nurses involved was uncertain how this would impact on clinical practice and how she would manage to undertake the work within her clinical area, with the existing work pressures she experienced. At the time the ward area was about to expand and open a further four beds for high dependency patients and there were staff vacancies. This all contributed to additional pressures within the clinical area.
The initial baseline data collection of the CQIs highlighted to the senior charge nurse areas for improvement. This confirmed what she, as the clinical lead for the area, had already suspected but had had little evidence to support.
Following the initial data collection, the results were discussed with the ward team and Plan-Do-Study-Act ( PDSA) change cycles were developed to improve compliance. These included communication reminders regarding timing of documentation, through documentation completion, with staff members being given the responsibility to ensure that the identified actions were completed. The senior charge nurse also noted that although an elective ward, over 70% of the patients were transferred to her clinical area rather than direct admission. This had implications with regards to compliance with CQIs out with her sphere of responsibility.
The senior charge nurse re-audited the clinical area against the CQIs to ensure that improvements were being embedded into the clinical area. During this time the four HDU beds opened, staff vacancies were filled with regular bank staff but the senior charge nurse continued to practice in the role she had always practiced within, rather than being able to adopt the refocused role framework. Over this period, approximately 15 hours per week of the senior charge nurse's time was lost to providing hospital cover duties.
In the fifth month of the development period, there was a concerted effort to change the role of the SCN to be more aligned to the role framework. During this period, hospital cover was removed from her role, she became non caseload holding and consequently was more visible and accessible for staff and patients. Her role in coaching, supporting and providing expert clinical opinion for clinical staff was used to assist in monitoring and improving clinical quality. Time to educate and implement new documentation (falls risk assessment tool and nutritional screening) was available, assisting in improving the compliance to CQI. This is demonstrated in the graph.
Improved compliance with CQI following introduction of revised SCN role
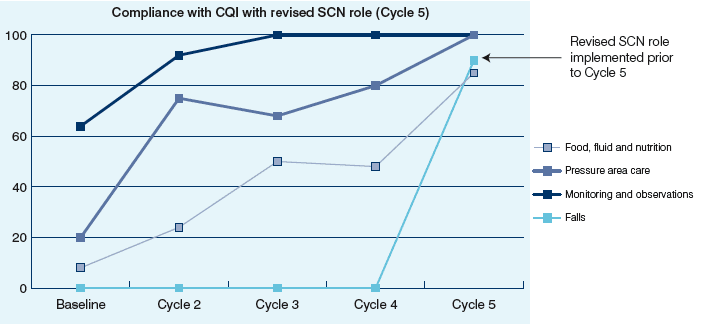
As the senior charge nurse and her team became more focused upon improving quality and implementing continuous quality improvements, compliance with the CQIs improved. (It is important to note that compliance was measured as having documented evidence, and the increased compliance indicates a marked improvement in record keeping in these areas.)
This case study demonstrates the synergy between these two projects and highlights that focus and improvement in quality of care and experience correlates with the introduction of the revised SCN role.
Develop a model to ensure continuous review and development of the CQIs
One of the recommendations of The Impact of Nursing on Patient Clinical Outcomes was to consider the development of "Centres of Responsibility" for the development of Clinical Quality Indicators.
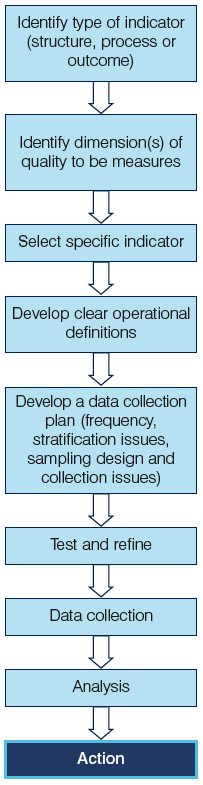
With the concept of "Centres of Responsibility", NHS boards would be responsible for developing CQIs. This would require an element of national coordination and support to ensure that the CQIs developed are prioritised, appropriately tested and valid for use in other NHS boards. A model for indicator development has been adopted and adapted for this purpose (adapted from Lloyd, 2004) (Figure 3). It is noted that there is a potential synergy with the NHSQIS Joanna Briggs Institute ( JBI) project ( http://www.joannabriggs.edu.au/about/home.php) . It is anticipated that access to the JBI system will support the development of further CQIs.
Figure 3. Model for the Development of Quality Indicators (adapted from Lloyd, 2004)
Summary of CQI Project
The development of CQIs for nursing has a long history. There are now four generic indicators that are applicable across a wide variety of in-patient settings. The model of Centres of Responsibility has been developed to ensure that other indicators in progress for midwives and paediatric, mental health and learning disability nurses will continue to be developed.
The focus of these indicators is to support nurses and midwives in delivering improvements in the quality of processes and outcomes of care in their areas. This will be further supported by eQIPS, which will be ready to be rolled out across Scotland by September 2008. This will provide nurses, when they are completing their CQIs compliance, with real-time reports and data to support where they are doing well, and highlight areas that require further work. In the implementation framework set out in the next chapter, CQIs are an important tool for senior charge nurses to establish a continuous quality improvement culture in their areas.
There is a problem
Thanks for your feedback