Scottish Health Survey 2016 - volume 1: main report
Statistics relating to the health of people living in Scotland.
This document is part of a collection
6 Multpile Risks
Anna Terje
Summary
- In 2016, 40% of adults had one risk factor and 31% had multiple risk factors (two or more) with just 1% of these exhibiting all four risk factors measured (smoking, harmful drinking, low physical activity and obesity).
- The number of adults with multiple risks (two or more) increased with age from those aged 16-24 (20%) to those aged 55-64 (39%) before declining to 33% of those aged 75 or over.
- The mean number of risks for all adults was 1.10 risks with higher mean risks for men (1.14) than for women (1.05).
- Among those with only one of the risk factors, the most common for men was drinking over the recommended limit (15% of men reporting this as their only risk) and for women the most common single risk was failing to meet the physical activity recommendation (16% of women).
- For those reporting two risk factors, failing to meet physical activity recommendations and obesity was the most common combination. Women were significantly more likely to have this combination than men (11% of all women compared to 6% of men).
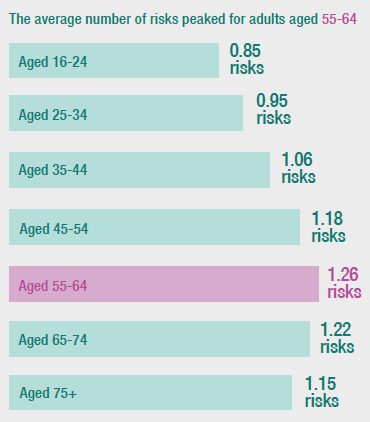
- The proportion of all adults assessed to be failing to meet physical activity recommendations and obese only increased with age, from 3% of those aged 16-24 to 18% of those aged 75 and over. A similar age-related pattern is seen for adults who both smoked and failed to meet physical activity recommendations: just 2% of those aged 16-24 exhibited these risks, rising to 5-6% of those aged 55 and over.
- Adults living in the most deprived areas were twice as likely to have two or more risk factors (41%) as those living in the least deprived areas (20%).
- Adults who reported having two or more age-standardised risk factors (smoking, alcohol consumption, obesity, or low exercise levels) were more likely to have a longterm condition (54%) than adults with one risk factor (44%) or no risk factor (37%).

6.1 Introduction
As a modern, developed society, Scotland faces substantial challenges to public health as a result of lifestyle behaviours and social-cultural norms that counteract positive health choice making amongst the population. These social determinants therefore are key risks that impact on the health and wellbeing of individuals, families and communities. The impact of these socially determined health risks is evident across the whole life-span. The prevalence of multiple risk factors is a pervasive problem and one where adverse socio-economic gradients remain largely unchanged[1,2]. Improved understanding of where and how they occur is crucial to raising awareness and informing strategies to encourage and reinforce healthy lifestyles in Scotland.
The population health implications of multiple overlaying risks are challenging, given that many of the individual risks are themselves part of a complex web of causation (for example, obesity), and the policy interventions available are themselves multi-faceted. However, the development of more holistic interventions that address multiple risk behaviours is relatively rare. This is in part due to the complexity of delivery, an evidence base that is dominated by interventions that tackle specific risks such as smoking cessation[3], and the lack of evidence for the efficacy of holistic interventions, for example in reducing heart disease mortality[4]. The balance of evidence also favours universal population-level approaches, rather than those solely targeting individual behavioural risk factors, particularly when the aim is to improve health without widening health inequalities[5].
6.1.1 Policy background
In recognition of the challenge of the impact of multiple risks on the health of the Scottish population, the Scottish Government aims to set clear national public health priorities for Scotland as a whole in 2017 to be led by a new single national public health body which will be established by 2019. The background to this can be found within the Public Health Review which, published last February, made several recommendations about how public health should be strengthened. The Scottish Government’s Health and Social Care Delivery Plan translated these recommendations into three specific Government commitments:
- to work with SOLACE and COSLA to produce and publish a set of national public health priorities by the end of 2017;
- the establishment of a new, single, national body for public health in Scotland by 2019; and
- the establishment of local joint public health partnerships between local authorities, NHS Scotland and others to drive national public health priorities and adopt them to local contexts across the whole of Scotland by 2020.
The public health priorities will include targeting particular health behaviours, actions to reduce avoidable harm and ill health based on a population approach to prevention, early intervention and treatment that reaches across the life-span[6]. Key areas of public health risk are alcohol and/or tobacco use, diet and obesity, mental health and physical activity. The extent to which the new actions will incorporate a holistic approach to interventions addressing multiple risks is not yet clear.
6.1.2 Reporting on multiple risks in the Scottish Health Survey
In 2010 the prevalence of multiple risks for poor health among adults in Scotland was explored in the Scottish Health Survey (SHeS)[7]. The focus was on the following five risks: smoking, hazardous or harmful alcohol consumption, overweight and obesity, low fruit and vegetable consumption and low physical activity levels. These factors are known to impact negatively on individual and population health and feature among the ten risks that have been estimated to contribute most to disease across the globe[8]. This approach was extended in the 2013 SHeS annual report[9] to include a wider range of risk measures, spanning a larger number of health domains. This provided a more detailed account of the myriad of ways in which risks and vulnerabilities occur in the population, which most commonly co-exist and how they are distributed between men and women, across the life-span and by deprivation levels.
This chapter first reports on the prevalence of multiple risks by age and sex for 2016, using smoking, harmful drinking, low physical activity and obesity as risk categories to assign a multiple risk score to individuals of between 0 and 4 risks. This is followed by an analysis of the associations between these risks.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. Where appropriate, to ensure that comparisons are not confounded by different age profiles within categories, data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of SIMD, BMI and age-standardisation. Supplementary tables are also available on the Scottish Government SHeS website[10].
6.1.3 Methods and definitions
There is detailed discussion of the individual risk factors used here, that is, alcohol, smoking, physical activity and overweight and obesity in chapters 1, 2, 3 and 5 respectively. For the purposes of this chapter risk factors are defined as being a current cigarette smoker, drinking more than the UK recommended weekly guidelines, WHO Body Mass Index (BMI) classifications of adult obesity and those not meeting the UK physical activity guidelines for adults.
For detailed methodology and definitions for:
- Alcohol consumption guidelines see Chapter 1, Section 1.2.
- BMI see Chapter 5, Section 5.2.
- Physical activity guidelines see Chapter 3, Section 3.
- Smoking status see Chapter 2, section 2.2.
- Self-reported long-term conditions see Chapter 7, section 7.2.
6.2 Numbers Of Risks By Age And Sex For 2013-2016 Combined
This section looks at the numbers of risks exhibited by adults (aged 16 and over), providing the percentages with one, two, three, four and none of the following risk types: smoking, hazardous or harmful alcohol consumption, overweight and obesity, and low physical activity levels.
Adults were most commonly assessed to have one risk factor (40%), 31% of adults had multiple risk factors (two or more) with just 1% of these exhibiting all four risk factors measured. Just under a third (29%) of all adults identified as having none of the risk factors. Overall, the mean number of risks among all adults was 1.1 risks.
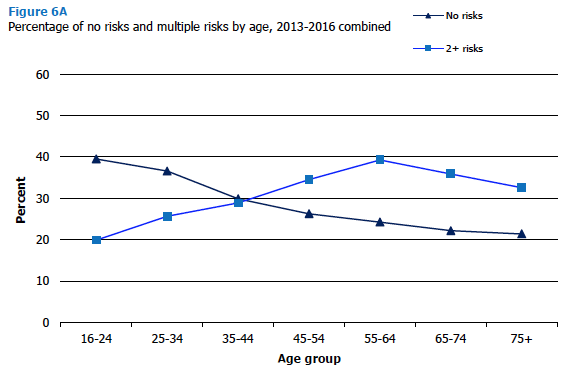
There was a significant association between age and the number of risks reported, as shown in Figure 6A and Table 6.1. The percentage of adults with none of the risk factors was higher at younger ages (39% among those aged 16-24 compared with 21% among those aged 75 and over). The number of adults exhibiting multiple risks (two or more) increased with age from 20% of those aged 16-24 to 39% of those ages 55-64 before declining to 33% of those aged 75 or over. These patterns were observed for both men and women. The prevalence of having all four risks was low for all ages, with percentages between 0% and 1% for all age / sex combination groups except men aged 55-64 (2%).
The mean number of risks was also significantly associated with age, increasing from 0.85 risks for those aged 16-24 to a peak of 1.26 risks for those aged 55-64 before reducing to 1.15 for those aged 75 and over).
The mean number of risk factors for all ages combined was 1.10 for all adults. There were significant differences between the mean risk for men and women (1.14 for men compared with 1.05 for women). This was largely due to differences in mean risk between the sexes among those aged 45-74, where men had higher mean risks than women (1.25-1.37 compared with 1.12-1.16). The age-related patterns of the mean number of risks were also significantly different for men and women. The number of mean risks rose steadily for women with age, from 0.88 among those aged 16-24 to 1.19 for those aged 75 and over. The mean number of risks for men increased with age from 0.82 for those aged 16-24 to 1.37 for those aged 55-64 but were lower thereafter (1.29 for those aged 65-74 and 1.08 for those aged 75 and over).
Figure 6A, Table 6.1
6.3 Prevalence Of Risk Types By Age And Sex For 2013-2016 Combined
This section describes the different combinations of risk types.
For all ages over 16 combined, 40% of men and women were assessed to have one risk only. Among the single risks, the most prevalent for men was drinking over the recommended limit (15%), while the most common risk for women was failing to meet the physical activity recommendation (16%).
Overall, 25% of men and 24% of women exhibited two risks. The most common combination of two risks was failing to meet the physical activity recommendations and obesity; 9% of all adults exhibited these two risks, with women significantly more likely than men to do so (11% compared with 6%). Just 7% of men and 5% of women exhibited three of the four risks, with combinations featuring failing to meet physical activity recommendations being the most prevalent among both men and women (1-2%).
There were some sex differences in combinations of risk. For example, the risk combination of smoking and drinking over the recommended limit was significantly more prevalent among men (6%) than women (2%). Furthermore, men were significantly more likely to be drinking over the recommended limit and also be assessed to be obese than women (5% and 2% respectively).
Prevalence of the various combinations of types of risks reported were significantly associated with age. For example, the percentage of all adults assessed to be both failing to meet physical activity recommendations and obese increased with age, rising from just 3% among those aged 16-24 to 18% of those aged 75 and over. A similar age-related pattern could be observed for adults who both smoked and failed to meet physical activity recommendations: just 2% of those aged 16-24 exhibited these risks, rising to 5-6% of those aged 55 and over.
The combined risks of drinking over the recommended limit and failing to meet physical activity recommendations also showed an increase with age, with just 2% of those aged 16-44 in this category, compared with 5% of those aged 75 and over. The reverse pattern was true for the combined risks of smoking and drinking over the recommended limit which fell with age from 6% of those aged 16-24 to 0% of those aged 75 and over.
Furthermore, the age group most likely to both drink and be obese was those aged 45-64, with prevalence estimates of 5-6% compared with 1-4% at younger and older ages. These age-related patterns were observed for both men and women.
Men aged 45-74 were most likely to have three risks (9-12% compared to 3-5% for other age-groups). For women there was no clear age related pattern.
6.4 Prevalence Of Long-Term Conditions In 2016, By Multiple Risks
Table 6.3 shows age-standardised prevalence estimates for long-term conditions by multiple risks and sex. Long-term condition was defined as any physical or mental health condition or illness lasting – or likely to last – for 12 months or more and then further defined as limiting daily activities or not. To ensure that the comparisons presented are not confounded by the different age profiles of the different categories, the data have been age-standardised.
In 2016, prevalence of long-term conditions was significantly associated with multiple risks. Men who reported having two or more risk factors were more likely to have a long-term condition (49%) than men with one risk factor (42%) or no risk factor (33%); the corresponding figures for women were 60%, 46% and 41%, respectively.
Prevalence of limiting long-term conditions was almost double for those who reported having two or more lifestyle risk factors (age-standardised prevalence of 35% among men and 45% among women) compared with no risk lifestyle risk factors (17% among men and 25% among women). There was no significant association between number of risks and non-limiting long-term conditions.
6.5 Multpile Risks In 2016, By Area Deprivation
There were significant associations between age-standardised number of risks and area deprivation.
As shown in Figure 6B, the age-standardised prevalence of multiple risks (two or more) among all adults increased with area deprivation; 20% of adults in the least deprived area quintile were assessed to have multiple risks, compared with 41% of those in the most deprived quintile. A similar pattern was found among both men and women.
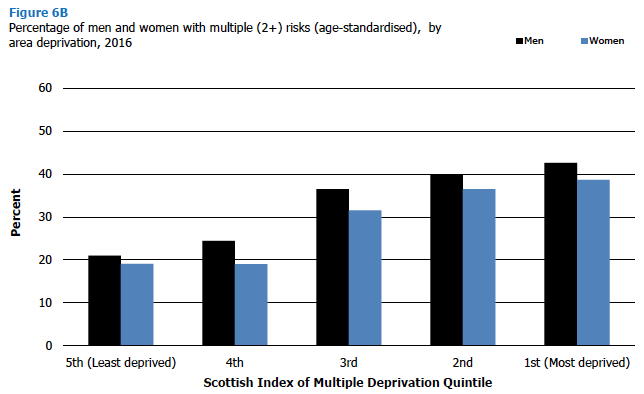
Conversely, the pattern was reversed for the age-standardised percentage of adults with no risks; 40% of adults in the least deprived quintile exhibited no risks, compared with 21% in the two most deprived quintiles. Again this pattern was similar for both men and women.
The pattern for adults assessed to have one risk was less clear with no significant association between prevalence of one risk and deprivation.
Contact
Email: Julie Landsberg, Julie Landsberg
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG
There is a problem
Thanks for your feedback
