eHealth Strategy 2014-2017
The eHealth Strategy 2014 – 2017 sets a national direction through a common vision and set of key aims. The Strategy maintains a significant focus on healthcare and the needs of NHSScotland, but has been redeveloped to recognise the rapidly evolving environment of integrated health & social care and the need to address not only NHSScotland requirements, but also the expectations and requirements of partnership organisations, and citizens for electronic information and digital services.
6 Governance and Delivery
6.1 Governance Arrangements and Principles
National strategic oversight of eHealth is provided by the eHealth Strategy Board, whilst governance oversight of the delivery of Scottish Government funded 'pillar' programmes and projects is provided by the eHealth Programme Board. They are both supported by an infrastructure of other bodies as shown below, which includes local consortium or internal NHS Board governance groups for local delivery projects.
eHealth Governance Arrangements in Scotland
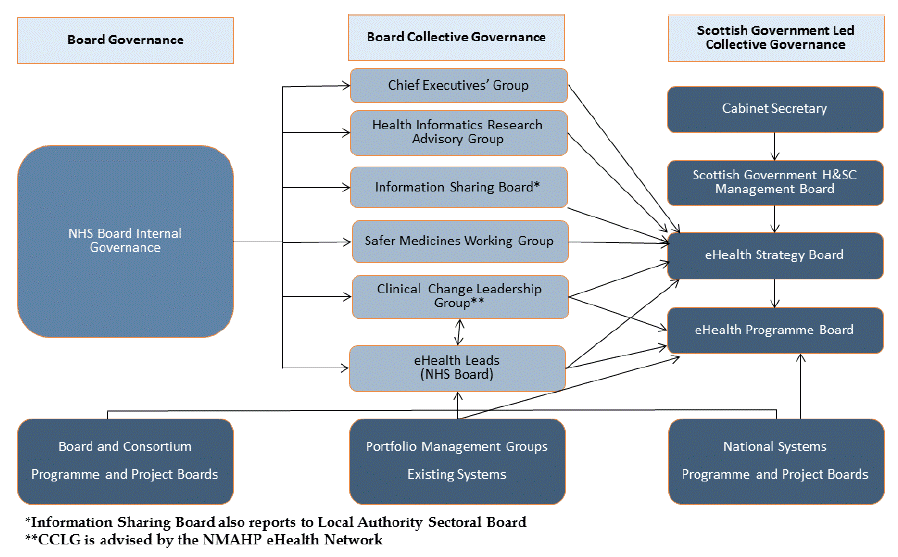
This overall structure will continue with membership of the various bodies reviewed and amended to recognise the increasingly closer links with social care.
In addition a number of national bodies will play key roles including:
- NHS Education for Scotland in relation to education and training in the use of eHealth systems, including their application to develop new models of care;
- Healthcare Improvement Scotland which is the lead improvement agency in healthcare in Scotland and views eHealth as a key enabler for driving improvements in health and social care. It is also the key organisation, together with processes undertaken by NICE, in the assurance and accreditation of clinical advice, guidelines and decision support capability, and support material and systems;
- NHS National Services Scotland in relation to a wide range of technology services and advisory functions. These include the operation of the national managed technical services contract and a number of other national contracts and services, assembly, custody and management of the national data resources, the provision of information analytical services, and acting as the centre of excellence for procurement and legal advice;
- NHS24, the Scottish Ambulance Service and the Scottish Centre for Telehealth and Telecare which lead on a range of functions including triage, information for patients, and aspects of out-of-hours services.
NHS Board eHealth Delivery Plans with stage point milestones will continue to be the main vehicle for planning, delivering and evaluating progress on delivery of eHealth, including use of the developing set of eHealth common measures. Plans will be signed-off by the local NHS Senior Management Board and progress will be reported annually to the Scottish Government. The Scottish Government will report annually to the Scottish Parliament.
In addition eHealth governance will continue to be guided by a number of key delivery principles, including:
- a focus on benefits and outcomes that really make a difference to citizens, patients and health and social care staff;
- the confidentiality, availability and quality and integrity of data, information and information services will remain paramount;
- development work will be done once on behalf of NHSScotland with subsequent sharing of the solution. This will apply to development for existing and new applications, for example designing electronic clinical documentation, generating business intelligence solutions, and undertaking core system detailed design and configuration;
- to achieve maximum benefit for patients and staff there must be the level of change management and benefits realisation required to support clinical reorganisation and redesign where eHealth supports new care models and clinical processes;
- an incremental and pragmatic approach will continue to be adopted, integration will be pursued rather than the creation of new solutions, and the core delivery approach will continue to be to ultimately provide a comprehensive Electronic Patient Record assembled from multiple operational system sources;
- a collaborative NHSScotland wide approach will be pursued, with the avoidance of duplication in all areas, and eHealth convergence over an appropriate time period that takes account of local circumstances and existing investment;
- the acquisition of eHealth solutions will be based on re-use of existing systems before buying new technology and a preference for buying existing solutions over building new applications.
6.2 Leadership
Both Scottish and wider global experience have demonstrated the importance of committed and effective senior organisational and clinical leadership to encourage the adoption of new technology and acceptance of associated change, and to maximise the timely realisation of benefits for patients and staff. NHSScotland will continue the practice of identifying senior leaders to take the SRO role for major programmes and will continue to emphasise and ensure the requirement for senior clinical engagement.
In Scotland the NHS Boards have historically had significant freedom to pursue their own priorities and agenda in relation to eHealth, hence the current varied position in terms of progress and systems. Scotland needs to strike the right balance to achieve progress at a speed that can be absorbed by NHSScotland, and maintain local ownership and innovation, whilst aiming for an increasingly consistent and integrated set of eHealth systems. This is a leadership challenge for management and clinicians, and is likely to prove most challenging in the area of ensuring collaborative approaches and increased rationalisation of eHealth infrastructures. eHealth Leads have promoted regional collaboration and working, and experience over recent years with GP systems, PMS and Clinical Portals demonstrates that this is achievable and that the best approach involves both top-down governance and bottom-up change management and clear communication.
eHealth needs primarily to reflect and respond to clinical requirements and clinical change, which places a particular responsibility on clinical leaders to set direction and persuade their colleagues of the benefits of eHealth and the necessity of change in working arrangements and processes. Scotland has been well served by the Clinical Change Leadership Group and the NMAHP eHealth network, and the clinical eHealth advisers at national and local levels. Further action has been taken with the introduction of the NMAHP eHealth Leadership Programme, which is now on its third cohort of staff, and leadership programmes for eHealth staff and middle managers, and consideration is being given to additional eHealth content in the medical postgraduate programmes.
A proposal has been put forward that the importance of eHealth to service delivery and the 2020 Vision, and the critical role of clinical leadership, should be recognised in the creation of more formal clinical information leadership posts within the existing management structures at national and local levels. This would provide an enhanced focus for eHealth development, as well as a cohort of clinical leaders to support the development of this economic sector in Scotland. This will be considered during the course of 2015 and proposals will be brought forward to strengthen senior clinical leadership in eHealth. In addition, there is a need to recognise that clinical leadership is required at all levels of NHSScotland to lead change in clinical care and processes associated with eHealth. Investment will be required in supporting clinicians who understand eHealth and are willing to lead change in individual clinical services and departments.
In addition to its own internal clinical leadership arrangements, NHSScotland will continue to ensure wide engagement with the clinical professions through the Royal Colleges and other representative bodies to ensure alignment with professional developments and guidelines and to ensure a collaborative approach to the development of eHealth.
6.3 Standards, Collaboration and Programme Delivery
Incompatible standards and data structures, and differing implementation approaches and decisions, have historically led to issues across NHSScotland with system integration and data sharing. As this is a capability that lies at the heart of enabling the types of care envisaged in the 2020 Vision, it must have the prominence and priority that it deserves. It will be addressed through a variety of measures including common applications, but also consistent data and messaging standards which will need to be adopted rigorously by NHSScotland and its suppliers.
The technical portfolio management groups (National Infrastructure Management Group and the National Applications Group), and in future the National Information Leads Group in relation to data standards, rightfully have ownership of this area on behalf of NHSScotland, and an increased emphasis will be placed on their review of the standards and integration aspects of significant developments and approval of proposed solutions. In addition, Scotland will continue its commitment to the Professional Records Standards Body for Health and Social Care.
Fundamental to the advancement of eHealth across NHSScotland will be collaboration and stronger programme delivery. Indeed, given the financial constraints on investment and the increasing complexity of care delivery, eHealth will struggle if these areas are not given the highest priority. NHS Boards will need to continue to adopt common approaches and solutions, and pool resources and expertise if they are to progress at the necessary speed. This is a leadership challenge for the eHealth Leads who sit at the centre of balancing local, regional and national priorities, and are faced with managing the local impact of collaborative decisions that may not reflect the immediately best or easiest solution for local NHS Board circumstances and pressures.
This has recently been recognised in the appointment of regional programme managers to support the Regional Planning Groups and this is likely to be an increased resourcing requirement, including at national level, to support collaborative approaches and developments. eHealth Division will work closely with the eHealth Leads Group to monitor this requirement to support collaborative programme delivery and, in particular, to ensure common standards and datasets for key developments such as:
- the information content of patient record summaries, for example of GP records or community records, that are viewed through the clinical portal;
- the content and format of a medications summary record, and associated reconciliation processes;
- the content and information that can be viewed through a patient portal that comprise a Personal Health Record;
- the content of shared health and social care developments.
6.4 Information Assurance
Effective information assurance is a foundational requirement for the successful exploitation of eHealth covering governance, confidentiality, security and availability, and integrity and quality of data, information and records. NHSScotland has a strong track record and has retained the confidence of the public, politicians and clinicians through the course of significant developments such as the Emergency Care Summary. The recent review chaired by Dame Fiona Caldicott[30] has signposted the way to acceptable further information sharing and has been adopted by the Scottish Government.
Scotland's information assurance framework will need to advance and keep up with eHealth developments such as the clinical and patient portals, health and social care integration, and the use of information for management and research, whilst retaining public confidence. In particular, there will be increased access from outwith the NHSScotland environment from public service partners and third sector organisations. eHealth Division has been reviewing existing documentation and its interpretation of data protection legislation, with a view to improving the clarity of guidance to health and social care workers across a number of areas. The review is taking account of the fact that eHealth systems and the information they hold will become increasingly vital to the provision of health and care services, and access to information will be from many more sources and a far greater range of devices.
During 2015 eHealth Division will review its existing programme. There will be particular focus on:
- embedding the Caldicott principles and guidance into NHSScotland and local government, including the Health and Social Care Partnerships;
- strengthening access monitoring and the incident reporting procedures;
- increasing capacity to undertake risk assessments and manage situations where the information governance risk from sharing information and the clinical risk from not sharing information can give rise to challenging decisions for eHealth and clinical professionals;
- policy development to better support information assurance for the emerging person-centred services and patient portals;
- policy, risk assessment and assurance for citizen identification when accessing NHS systems and services;
- continued reviews of ICT resilience and data integrity as NHS Boards increase their dependence on systems and move towards seven day working for some services;
- a continued programme of standards and guidance development, and delivery of training and support for local organisations and partner organisations.
The approach will continue to reflect past success through clear communication, consultation and openness with stakeholders.
6.5 Investment Appraisal, Benefits Realisation and Evaluation
There is a clear and established process to take eHealth concepts through appraisal to implementation and subsequent evaluation. It is not envisaged that this will change and conceptually it will continue to be an outcomes based approach - what will be the benefits for patients, staff, NHSScotland and the wider public sector? Given the financial pressures on NHSScotland it is only realistic that this process will continue to place an emphasis on operational efficiencies and opportunities to help address the demands on clinical services. Individual projects and programmes will be expected to demonstrate that consideration has been given to the process changes and training required to exploit new eHealth capabilities and realise benefits, and that an assessment has been made of the requirement for change management resources and skills. Suppliers will be expected to be cognisant of this, and, whilst it is difficult, a focus will remain on seeking to link supplier contractual commitments to outcomes and benefits.
However, given the complexity of the possible impacts of eHealth systems, and the breadth of outcomes in terms of behaviour, morbidity and mortality, consideration will be given to more extensive monitoring and evaluation of the most significant programmes, including academic and health economics approaches, to ensure rigour and sound evidence for further investment and development. This will include continuing to monitor worldwide developments in eHealth, drawing on the experience of the academic sector and bodies such as the Digital Health Institute, and engaging with industry and innovators. The focus will be on the identification and realisation of tangible benefits from eHealth investments in the form of improved safety, measurable improvements in service quality, financial savings, and increases in capacity and productivity.
With respect to monitoring progress by the NHS Boards, a set of Common Progress Measures were developed from analysis of NHS Board eHealth Plans, where a number of Boards had identified a similar approach to measurement of progress. These were developed into a set of measures which all Boards agreed to adopt. The measures came into use from April 2013 and are reported quarterly. They have been refined over time with Board input to ensure that they are meaningful and that the effort-to-value ratio is balanced. They will continue to be used to monitor progress and will form the basis of the evaluation framework for annual reviews and reporting, together with key pillar programme milestones and progress towards key deliverable targets.
6.6 Workforce Development
eHealth is about helping staff to do their jobs better and more efficiently, and inevitably it has a significant impact on their working lives. Success will only come from ensuring that not only is the technology appropriate but that staff are in the best possible position to exploit it for the benefit of patients and NHSScotland.
The focus of workforce development has shifted over recent years away from the more basic IT skills and system training. However, these remain important and a key component of undergraduate education, induction and new system implementation, but the burden across Scotland should reduce as eHealth systems become increasingly common and consistent. Going forward there will need to be an increased focus on ensuring that the clinical workforce is better educated and trained in the use of applied health informatics and exploiting eHealth systems to maximum benefit.
Recent work by NHS Education for Scotland has focused on the development of learning and training opportunities in the use of technology to deliver new models of care, with a focus on person-centred care in community and home settings, and the development of technology enabled learning. With the publication of the Everyone Matters: 2020 Workforce Vision[31] for the health and social care workforce, there is a much greater emphasis on how technology is used to support workforce development, which will be particularly crucial with the move to seven day services.
To achieve success in this area there is a need to ensure that:
- staff working in health and social care are confident, and enabled to use technology to access learning as part of their everyday activity;
- high quality digital learning resources are available on an anywhere, anytime basis, and are easily accessible to all those who can benefit from them;
- organisations in both health and social care settings are encouraged to ensure that the infrastructure that they provide is optimised to ensure that their workforce can access the learning resources that they need.
During 2015, NHS Education for Scotland will work in collaboration with the Scottish Social Services Council (SSSC) and other stakeholders to develop an action plan based around the vision that "People throughout Scotland's health and social care are empowered and enabled to use technology to learn, improve and transform services." This work will involve strengthening the health links into the Digital Public Services workforce streams focussed on workforce development across public services and supporting the health and social care workforce to make best use of technology in their learning and in their day to day work.
NHS Boards and other employers in the health and social care sectors will also have a vital role to play in ensuring that their workforce are able to access digital learning resources whilst at work, utilising their employer's infrastructure, and are equipped to recognise the need to make appropriate changes in the organisation and delivery of care in order to fully exploit eHealth capability.
6.7 Supplier Relationships and Procurement
At present, NHSScotland has a number of strategic relationships with suppliers that provide key systems and services. NHSScotland's strategy is to integrate systems from multiple suppliers, an approach that reflects historic approaches and investment, and a current absence of proven, enterprise-wide solutions appropriate to the NHS environment. As a result, NHSScotland needs suppliers to co-operate in bringing forward developments and supporting integration that was not entirely predictable or foreseeable at the time of procurement.
These relationships with suppliers are commercial and clearly NHSScotland needs to look to its own interests, in particular to ensure its needs for interoperability and consistency of standards take priority, and that suppliers deliver their full contractual commitments in terms of system functionality, integration and performance. Nevertheless, historic performance and approaches in this area will be a key future consideration when NHSScotland is placing contracts for products and services, and NHS National Services Scotland is taking the lead in protecting NHSScotland's interests in respect of eHealth, and ensuring a robust commercial approach with suppliers in collaboration with the NHS Boards.
The objective in procurement processes will continue to be the establishment of relationships that protect NHSScotland, are efficient and cost effective (development done once for Scotland), and can be mutually beneficial over the long term as eHealth and NHSScotland requirements inevitably change. This will include options to include performance and gain share based contracts and to encourage investment by commercial partners or joint venturing to benefit both parties.
6.8 Planning and Managing Delivery
This Strategy sets a Vision and Aims for eHealth and identifies the developments that are anticipated over the period to 2017 and then the period to 2020. Delivery of the Strategy will be a substantial challenge in which many organisations will have a role, including the Scottish Government, NHSScotland, various other public bodies and suppliers.
The Strategy is supported by a number of other documents, in particular:
- a Business Plan which sets out the major delivery programmes, including their context, organisational arrangements, key objectives and anticipated milestones;
- a Finance Strategy which identifies the level of financial resources that are likely to be available for local, regional and national initiatives and the associated management arrangements;
- a revised Technical Strategy addressing both infrastructure and applications.
Ongoing work will be required to develop and implement the delivery programmes and decisions will inevitably be required, during the course of investment appraisal, on relative priorities and the use of scarce investment resources. The eHealth Division of the Scottish Government will manage this process, working collaboratively with the NHS Boards through the various national eHealth management bodies. The focus will be on enabling an NHS-wide effort to collaborate, share experience and expertise, and, where appropriate, converge eHealth solutions, in order to deliver this eHealth Strategy and the associated benefits for patients, citizens and NHSScotland staff.
Contact
Email: Alan Milbourne
There is a problem
Thanks for your feedback