eHealth Strategy 2014-2017
The eHealth Strategy 2014 – 2017 sets a national direction through a common vision and set of key aims. The Strategy maintains a significant focus on healthcare and the needs of NHSScotland, but has been redeveloped to recognise the rapidly evolving environment of integrated health & social care and the need to address not only NHSScotland requirements, but also the expectations and requirements of partnership organisations, and citizens for electronic information and digital services.
5 eHealth Strategic Programme
The Vision and Aims set direction, however it is equally important that this eHealth Strategy focuses the attention of all parties around a common strategic programme to enable effective delivery. This section sets out that programme describing in more detail the vision for 2020, consistent with NHSScotland's overriding strategic narrative, and identifying priority developments in the period to 2017. Its structure is based on the seven strategic eHealth aims (note that specific deliverables are highlighted in bold text, those carried over from the original 2011 strategy are identified by an asterisk, and timing references are to the end of the calendar year).
5.1 To enhance the availability of appropriate information for healthcare workers and the tools to use and communicate that information effectively to improve quality
5.1.1 Current Status
Overall, NHS Boards have made significant progress since 2011, with clinical portals becoming a core strategic capability and making a significant impact on the availability of the nationally agreed 14 priority clinical information items. However, there are remaining gaps in clinical information system portfolios and areas where substantial upgrades or system replacements are required. This applies for some NHS Boards to community and mental health systems, and also to the Patient Management System where a number of forthcoming implementations are planned by NHS Boards. Additionally, there remain a range of functionality and ergonomic issues, and many staff do not at present have easy access to electronic systems.
5.1.2 Vision and Priorities
This aim goes to the heart of the views expressed by clinicians that they want access to summaries of the patient records of their colleagues and that eHealth systems should support them in quickly and effectively undertaking their day-to-day patient care tasks.
The vision for 2020 is that NHS Boards will build on the existing infrastructure of electronic clinical systems, integration hubs, and the adoption of portal technologies so that:
- all appropriate staff have access in all locations where they work to an effective and resilient electronic clinical system that supports them in their daily work caring for patients, including accessing and recording patient information, accessing clinical advice and decision support guidance, and initiating and managing care processes by themselves and colleagues;
- all appropriate staff have access to a view of each patient's comprehensive Electronic Patient Record which will provide them with an overview of the key information recorded by any colleagues in health and social care, and, where applicable, by the patient or their carer(s). This will comprise of a view of summary information from the major clinical systems, including general practice, community care, secondary care and others, and, ideally, will provide the capability to 'drill down' to an appropriate degree of further detail;
- patient care processes will be supported as these systems will enable staff to refer to colleagues, triage referrals, request investigations and receive results, generate clinical correspondence, and track care and receive prompts and alerts;
- information can follow patients irrespective of departmental and organisational boundaries, facilitating the work of the clinician, including mobile access where required.
5.1.3 Strategy and Deliverables
During the new Strategy period:
- NHS Boards will, over the period to 2020, provide staff across health and social care with appropriate electronic access to an increasingly broad view of patient information as it is digitised to create a comprehensive Electronic Patient Record. For most NHS Boards this is expected to be through their clinical portal infrastructure and to include access to summaries from all major clinical systems, including general practice and community and secondary care. A key feature will be retention of the patient-centred context, ease of navigation between datasets, and management of appropriate privacy and confidentiality controls. It will also include removing blockages arising from NHS Board boundaries through greater interoperability of systems to allow sharing of information. This will also help to future proof systems in the event of changes to organisational structures;
- By 2017 NHS Boards will complete making the nationally agreed 14 priority clinical information items available electronically. NHS Boards will continue the process of widening access to their electronic patient clinical information to support patient flows and clinical need, including across NHS Board boundaries. This is already occurring through providing wider access to individual NHS Board's clinical portals. These developments will see the functionality of portals being enhanced beyond a viewing space to one that includes a simple, intuitive and fast interface for the use of clinicians that enables them to fully manage their work and support safe care. Further work will be undertaken to consider the requirements for patient information in varied clinical circumstances, and whether there should be an expansion of the national set of 14 patient information items;
- By 2017 NHS Boards will complete the introduction of appropriate single sign-on for healthcare workers. This has been widely introduced in secondary care but requires completion of roll-out and extension to primary care;
- By 2017 NHS Boards will complete the roll-out of privacy breach detection tools;
- NHS Boards will continue to broaden access to the dataset that is co-created with the patient and is currently held in the Key Information Summary system. This will extend access to all health staff, and with appropriate consent arrangements social care staff, who require this information as part of their role;
- By 2016 eHealth Division, working with key partners such as Healthcare Improvement Scotland, will sponsor development of a clear strategy and organisational arrangements for the future creation, adoption and management of clinical decision support information and tools, and the intelligent use of patient electronic information to enhance safety, care quality, and clinical knowledge and learning. This will need to recognise that a considerable volume of clinical decision support material already exists and is in use across NHSScotland, including the SIGN guidelines and a wealth of clinical assessment, procedural and other guidance. At this stage, it is expected that this area will continue to be led by the national Clinical Decision Support Steering Group working closely with the CCLG and Healthcare Improvement Scotland;
- NHS Boards will continue the process of acquiring, improving and widening the scope of their major clinical information systems portfolio. This includes for several NHS Boards replacement / rollout completion of their community systems and mental health systems, and for some replacement of their patient management system (HEPMA is discussed separately below);
- By 2017 the process to put in place a contractual environment to support the future provision of GP systems and associated community system requirements will be completed. This will need to address a range of issues, including web-based server solutions, integration with community systems, both existing and new, future provision of the functionality of the current ECS/KIS/PCS solutions, and support for clinical portal and patient portal developments related to the Electronic Patient Record and the Personal Health Record in the form of enabling appropriate summary views of GP patient information. This will need to be accompanied by the necessary governance and access protection for such summary patient views, which may be facilitated by agreeing at national level a definition of content and associated processes for use;
- Over the period to 2017 and beyond NHS Boards will further progress making patient information available to health and social care staff in all appropriate care locations. This will be facilitated by the Scottish Wide Area Network (SWAN) contract and the Next Generation Broadband developments which will help to provide network access from community locations, care homes and patient homes. However, it will require a significant expansion of access devices in hospitals and in the community, including, in particular, mobile devices. It will also require a focus on screen design and ergonomics given the amount of patient information, and the need to present it in a way that facilitates efficient and safe working practices. Given the growth in number of devices that this will involve and their importance in allowing staff to do their work, consideration will be required as to how best to manage this in the most economic fashion across Scotland, and the revenue consequences associated with funding timely support and a realistic replacement cycle in order to ensure reliability.
5.2 To support people to communicate with NHSScotland, manage their own health and wellbeing, and to become more active participants in the care and services they receive
5.2.1 Current Status
Considerable progress has been made in the provision of online information to help people to manage their wellbeing and conditions and to organise their healthcare, for example through NHS Inform[23], together with wider wellbeing initiatives such as 'Living It Up'. This is already contributing to supporting patients to manage their own health. In other area progress is more limited and experimental but is significant, including:
- some general practices that have adopted electronic repeat prescribing and online appointment booking;
- the use of teleconferencing to enable patient consultations, for example to remote locations and to care homes, as well as to support minor treatment centres;
- a current initiative to provide patients with the option to receive their health correspondence by email;
- the work with My Diabetes My Way and Patient View which enable co-created records, access to results, and secure messaging for these specific groups of patients;
- work being undertaken through Patient View to assess patient access to their ECS record and the impact and effect of providing test results online.
In addition, a Proof of Concept scheme for a patient portal is currently being developed. The challenge moving forward is to broaden the support that can be provided, design and implement patient access to their own records, and incorporate these models into routine care at scale.
5.2.2 Vision and Priorities
The vision for 2020 is that citizens and patients will be able to use a patient portal to access their own Personal Health Record (in essence Electronic Patient Record data enhanced and presented as required to make it accessible, informative and useful for patients and their carers), and make their own contributions to the record. They will also be able to access structured information about managing their health, prevention and self-management of conditions. In addition, they will use secure two way electronic communication with their health and social care providers to book and manage appointments, order repeat prescriptions and, where appropriate, use eConsultation facilities, resulting in convenience for patients and reduced transaction and administration costs for NHSScotland. These services will be designed and built based around the preferences of citizens and patients.
It is also expected that patients will be able to download their data for personal use in their own applications and devices. Again this will be intended to support health maintenance, prevention and self-management. The result will be more empowered, educated and supported citizens, patients, carers and families, who can play a much greater role in orchestrating their own care and taking informed decisions about their health, its monitoring and treatment.
Person-Centred Support and Communications
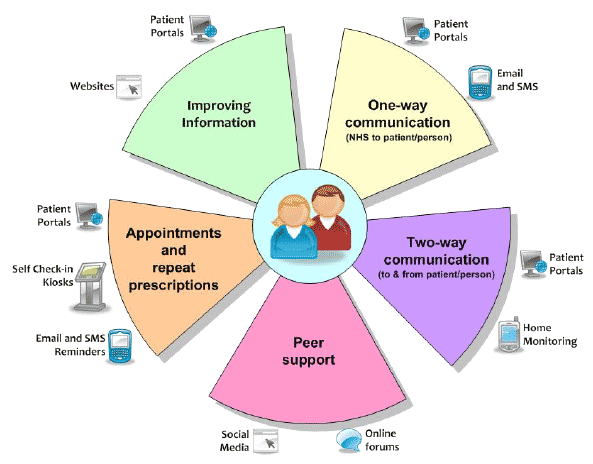
5.2.3 Strategy and Deliverables
During the new Strategy period:
- NHSScotland will continue to adopt the products and infrastructure available as part of the public sector Digital Services Strategy. Specifically, the Citizen Account system (myaccount[24]) will be the service through which patients will authenticate their identity and register for online transactional services. The service will be developed to allow registered users to link to their CHI number which will be the key to retrieving their personal information and data;
- By 2015 eHealth Division will sponsor the definition of a national approach to a patient portal that will provide a single point of access for patients and the public to their information and digital services, together with a development and implementation approach and an associated business case. This will address the need for integration with authentication services and the requirement for a simple and intuitive interface for citizens with access to appropriate support services. The work will need to define those services that will be offered through the portal. There will need to be further consultation with patients regarding their priorities and learning and evidence from the Proof of Concept initiative on what works well, and input from industry in respect of the tools and capabilities that they may provide to patients that may seek to interact through the portal and associated services;
- All GP practices will be encouraged to provide online repeat prescribing and online appointment booking as online services, with a view to at least 90% of practices offering this service by 2017. This will provide benefits for patients and administration time savings for practices as well as important experience of the impact of these options which will inform wider developments;
- By 2017 NHS Boards will have implemented electronic communications by which correspondence with patients, such as appointment letters, clinical instructions and clinic letters, can, optionally, be done online. This development will provide all patients with the option to receive their health correspondence from NHSScotland by email or SMS and reply in similar fashion. As well as being quicker and more organised and convenient for patients this will have substantial financial savings for NHS Boards through reduced transaction and administration costs;
- The portal development with sequential incorporation of services as defined in the business plan and development approach to provide a Personal Health Record will be undertaken over the period 2016 - 2020, alongside the associated technology enabled care developments described under Aim 3 below.
5.3 To contribute to care integration and to support people with long term conditions
5.3.1 Current Status
SCI-Diabetes is an excellent example of system support for long term conditions. The single instance system is used by all diabetes services across Scotland and many general practices. It provides highly specialised functionality for the care of this specific condition, and is integrated into the wider eHealth infrastructure for information exchange. The My Diabetes My Way portal extends access to patients who sign in via myaccount, and a clinical decision support rules system is integrated to provide additional intelligence.
The renal system (lc) is another example of where long term condition support exists. In the west of Scotland a single instance operates across several NHS Boards allowing shared electronic patient records across care and treatment locations. Again the system includes significant professional guidance, and the Patient View portal is providing access for patients which has had very positive feedback.
Work remains, as described in relation to the other strategic aims, to provide wider and easier access to health and social care information for clinical professionals in the form of an Electronic Patient Record. This will have a major impact on the care of this group of patients with long term conditions who often have significant clinical information spread across locations and systems. In addition, completing the digitisation of patient information will provide a basis for the delivery of a Personal Health Record.
NHS Boards are working currently with their local authority, and third and independent, partners on the sharing of patient / client information, in particular through the Health and Social Care Partnerships. This has included not only adult care but also consideration of Getting It Right For Every Child which has been set in statute through the Children and Young People (Scotland) Act 2014. The National Information Sharing Board, coordinated by eHealth but with cross-public sector and third sector representation, has played a key role in setting out guidance and standards. Two key guidance documents have been developed that will support information sharing. Firstly, there is the Information Strategic Sharing Framework[25] which sets out the landscape in which partnerships will be expected to work and share information. The second is more technical in nature and is an Information Architecture Vision which can be used by partnerships to guide their ICT implementations and ensure conformance to standards that will enable sharing beyond partnership boundaries. A number of approaches have been adopted to facilitate information sharing according to local circumstances, including portal developments and Multi-Agency Stores. Further development will need to follow to provide workflow support for the co-ordination of care, including supporting cross-border patient flows.
Scotland has significant experience of Technology-Enabled Care and is now in the process of refining approaches that will work at scale based on evidence of what works in a cost-effective and impactful way. The approach to, and investment in, this area has recently been extended through the announcement of £10m to support the Technology-Enabled Care Programme. This programme will be key to setting the direction and development of this area in Scotland by clarifying the evidence on the best technology and organisational models. There are five priority areas:
- Expansion of home health monitoring as part of integrated care plans to move beyond the small/medium scale initiatives that have been introduced in a small number of areas to substantial programmes across Scotland;
- Expanding the use of video conferencing through using the experience of the NHS video conferencing systems to enable partner organisations across all health and social care sectors to participate and benefit, as well as growing its use for clinical/practitioner consultations;
- Creating a national digital platform framework, learning from, and potentially building on, national initiatives such as Living it Up and ALISS to expand supported self-management information, products and services for Scottish citizens;
- Expanding the take up of Telecare, with a particular focus on upstream prevention, support for people at transition points of care and people with dementia and their carers;
- Exploring the scope and benefits of switching current provision of Telecare from analogue to digital Telecare, scoping a move for Telecare from the current analogue systems to digital in order to facilitate integration with Telehealth.
These developments will, in due course, make a major contribution to the care of patients with long term conditions, in particular enabling and supporting their self-management, as well as helping those in remote and rural locations.
5.3.2 Vision and Priorities
The agenda in this area is set by All About Me[26], the action plan to improve care and support for people with multiple morbidities, the Home First[27] actions to transform discharge, and the work of the Joint Improvement Team as set out in their Strategic Plan 2013 - 2016. Clearly, it is also a major area that is intended to be addressed through the creation of the Health and Social Care Partnerships.
The vision for 2020 is that the integrated health and social care teams that support people with long term conditions and multi-morbidities will easily process information and communicate electronically to co-ordinate their activities to ensure seamless, more effective and higher quality care for patients. This will include supporting current and emerging forms of care delivery including single point of care community hubs, hospital at home, and community wards that are all aiming to provide supported discharge and alternatives to acute care and admission.
Additionally, standardised models of technology enabled care, such as home health monitoring, will become available directed at enabling patients to remain at home or in the community. eHealth services will be developed to ensure that these developments in patient care are accommodated within the eHealth architecture.
All of this will be directed at providing patients with the reassurance and confidence to manage their own condition(s) and care, and to seek and receive more timely help and support, enabling them to remain at home or in the community for longer. In effect it will help to include the patient and / or their carer as appropriate as an active member of the care team, and increasingly allow them to decide on the support they seek from health and social care professionals.
5.3.3 Strategy and Deliverables
During the new Strategy period:
- NHS Boards will continue to work with the Health and Social Care Partnerships to fully define their information management requirements and develop appropriate solutions, building on the work of the Health and Social Care Information Sharing Strategic Framework;
- The current deployment of initial capability to enable sharing of information between health and social care will continue;
- By 2016 NHS Boards will have improved capability to stratify their patients to identify those with multiple morbidities and long term conditions;
- By 2015 eHealth Division will sponsor work to establish the future approach to systems that support the management of long term conditions. The SCI-Diabetes and Renal developments have shown the potential of specialist systems that bridge patients and clinicians, and primary and secondary care, however there are a range of other specialties and long term conditions that do not have such support;
- Over the period to 2017 and beyond to 2020, NHS Boards will support the improvement work to develop intermediate care options for people with long term conditions and multiple morbidities. This will be through taking advantage of developments under other eHealth strategic aims that will address improvements in patient information access, communication and workflow between teams of health and social care staff, and support for patients to manage their own health;
- Over the period to 2017 and beyond, as technology enabled platforms and solutions become proven at scale, they will be adopted by NHSScotland clinicians as appropriate to individual patient's conditions and circumstances. The key consideration will be that solutions have clear evidence that they are beneficial for patients, cost effective, and are at least as good as current services. NHS Boards will also develop their information systems to ensure that they support individual patients with multiple morbidities and long term conditions. eHealth will have a role to ensure that emerging technology based solutions are supported within these information systems.
5.4 To improve the safety of people taking medicines and their effective use
5.4.1 Current Status
Electronic prescribing in general practice is universal and is linked into the ePharmacy systems that support dispensing, with community pharmacists also having access to the Chronic Medications Service system to manage patients' repeat prescriptions and reduce the burden on GPs. There are still gains to be had, however, from widespread utilisation of patient access to GP systems, as opposed to email messaging, to order repeat prescriptions. The Emergency Care Summary provides the current capability to share medications information between healthcare sectors, and the range of staff able to access this has been widened, with professional and public consent, to include scheduled care.
However, acute hospital prescribing and recording of medicines administration remains predominantly paper based reflecting that it is considerably more complex. The exception to this is NHS Ayrshire and Arran which has successfully undertaken a long and complex implementation and, consequently, has gained substantial experience of the specific challenges of implementing HEPMA.
HEPMA is commonly viewed as a vital missing-piece of the digital medications jigsaw. A national outline business case has been completed and approved for HEPMA systems, and the Closing the Loop clinical blueprint work has defined the requirements in relation to medicines reconciliation at transitions of care. In addition, a current project is working to define a 'dose syntax' that will enable translation between the different prescribing formats utilised in primary and secondary care.
However, there remains considerable work to implement HEPMA and medicines reconciliation in a safe and sustainable format that takes account of existing investment at NHS Board level and meets both local and national requirements. Development in this area is widely regarded as a particularly high priority, however it is recognised that the requirements are complex, will result in considerable change to working practices, and can impact safety if not implemented carefully.
5.4.2 Vision and Priorities
The safer use of medicines is key to patient safety and the quality of care as it sits at the centre of the therapeutic process in the vast majority of patient care events. There are also crucial requirements for local and national monitoring and research regarding the use and administration of drugs. In the period to 2017 and on to 2020:
- significant progress will be made in enabling hospitals to adopt electronic prescribing and medicines administration (HEPMA) systems. These systems will enable digitisation of a key component of the patient's care and information such that the drug record is available within the Electronic Patient Record. In addition, with appropriate built-in clinical decision support, full recording of the reasons underlying prescribing decisions, and other intelligence such as support for polypharmacy reviews, these systems have enormous potential to reduce risk and improve the quality of patient care and provide important national clinical intelligence on prescribing practices, outcomes and adverse events;
- in addition, as an associated development, NHSScotland will develop electronic capability to support the reconciliation of patient medications across all transitions of care, in particular between primary and secondary care at admission and discharge (Closing the Loop). This will also target providing access to a full summary of patient medications, including those prescribed by community staff, specialist clinics and community pharmacists, and including information on prescription dispensing. This will allow more effective medicines reconciliation, safer transitions and reduced risk for the patient, and the elimination of all re-keying of prescription data.
Achievement of the above, together with developments under the other strategic aims, will enable all appropriate health and social care workers to have access to a comprehensive view of a patient's medications summary and to record any updates or changes, which will make a major contribution to patient care and safety. A longer term aim will be the electronic interaction of patients with their own medication records, for example to record aspects such as side effects they have experienced and non-prescription drugs that they have taken.
However, it remains the case that implementation of these solutions will be particularly complex as they impact a critical area of care where mistakes can have serious consequences, and they will have a significant effect on current working practices. Experience suggests that whilst eliminating some risks to patients, they can introduce new problems, and, therefore, they require particularly careful design and implementation. As a result, this area is not subject at present to specific target dates for completion, although the benefit from early implementation of these systems is clearly recognised.
5.4.3 Strategy and Deliverables
During the new Strategy period:
- By 2015 eHealth Division will sponsor work to be undertaken collaboratively to confirm and agree a way forward for Scotland. This will involve:
− reviewing the existing specification for HEPMA solutions and ensuring it is appropriate for current needs in the context of the overall vision for medications information management across NHSScotland. This will take account of experience gained in Scotland in the use of this type of system, with a particular focus on safety, but also including more extensive functionality and requirements for clinical decision support, and the need to provide flexibility to support varying clinical processes between specialties and hospitals;
− completing the 'dose syntax' work and considering the impact of the 'Closing the Loop' requirements, and defining how these will be addressed and the impact on HEPMA solutions, existing GP systems and ePharmacy systems. This may require approaches involving a separate patient medications summary record, but this remains to be determined;
− reviewing the key integration between pharmacy management solutions and HEPMA and patient management systems and HEPMA, and system operation at an enterprise level;
− considering the market solutions and procurement options available to NHSScotland, and the relative advantages of a single common solution as opposed to a framework for NHS Boards to choose from given relative solution quality and cost, and the possible impact on existing investment;
− confirming and agreeing a way forward for NHSScotland and the NHS Boards that will deliver the medications information management vision, and maximise effective working for staff, and safety and quality for patients. This will confirm procurement and implementation approaches, including the initial scope of solutions, and address how data and messaging standards in this critical area, and ideally the user interface, will be consistent across Scotland, for example through the work being undertaken by the Professional Records Standards Board on medication messaging standards; - NHS Boards will implement the agreed way forward, collaborating on all aspects where there may be advantage to NHSScotland and patients, such as common datasets, system design and infrastructure, and shared maintenance and support. Some NHS Boards will progress HEPMA and medicines reconciliation solutions as an earlier development than others, depending on local priorities and business cases, availability of resources and implementation capacity. It is expected that most NHS Boards will have some elements of HEPMA operational by 2020.
5.5 To provide clinical and other managers across the health and social care spectrum with the timely management information they need to inform their decisions on service quality, performance and delivery
5.5.1 Current Status
Scotland has historically performed well in the collection and analysis of health data, including clinical datasets to support audit. Much is already undertaken through local data warehouse capabilities and analysis tools, and the national datasets managed by NHS National Services Scotland. Additionally, substantial research capability exists in Scotland's universities, for example the Farr Institute for health informatics at Dundee and Edinburgh Universities, to work with complex, unstructured data. The challenge will be to meet the needs of local clinicians whilst also ensuring continued effective and efficient capture and integration of increasing amounts of data from operational to national levels. This will require definition and stricter adherence to agreed national data sets and standards, access to the tools, and continued development of the capabilities and skills that will support measurement of performance and quality across the health and social care spectrum. It will also require education and training for staff to ensure they understand and can respond to the requirement to record structured, consistent data if it is to be useful for these purposes.
The area as a whole is subject to demand growth as a result of the pressure on services and the degree of scrutiny, increasing complexity, including the integration of health and social care, and the need to keep up with new tools and technologies. The need for effectively planned and integrated infrastructure and data collection and collation mechanisms, together with the capacity and skills to manipulate, analyse and interpret that data, has never been greater.
Recognising the above, a new National Information Leads Group (NILG) has been established to take the lead for NHSScotland on all aspects of data definitions and recording, information analysis and reporting, and associated with this the development of skills and capacity. In particular, it is well placed to ensure that across the range of stakeholders from the operational frontline to research and public uses of health information, there is a co-ordinated process to ensure information is managed appropriately and effectively.
In addition NHS National Services Scotland which manages the national datasets has initiated an Information Redesign Programme to consider how the collection and analysis of health and social care data across Scotland should be developed to enhance effectiveness and efficiency, including reducing the burden on NHS Boards, enhancing the services that can be provided in complex areas such as predictive analytics, and contributing to the Scottish Government's goal of increased publishing of Open Data.
5.5.2 Vision and Priorities
The vision for 2020 recognises that frontline operational activities and eHealth systems provide the data that can be collated and analysed at local, regional and national levels. This can then generate information that can be utilised for a range of purposes:
- clinicians may utilise datasets to enable examination of their own clinical practice, to carry out personal, team and hospital / practice clinical audit for quality assessment and improvement purposes, and to work with their colleagues locally, regionally, nationally and internationally to improve outcomes;
- immediate, essentially real-time, local operational decision taking, and associated planning monitoring and evaluation of activity levels to maximise capacity and use of resources;
- local and national evaluation of service delivery in terms of its timeliness, safety, quality and outcomes;
- national and international research and innovation using multiple data sets, unstructured data, and data linkage, to answer complex questions which generates new knowledge and intelligence that provides a basis for revised policy and practice.
All of this contributes to generating a cycle of continual improvement in the health and social care delivered in Scotland and also supports reporting to the public and Government.
Record Once, Use Many Times and the Cycle of Improvement
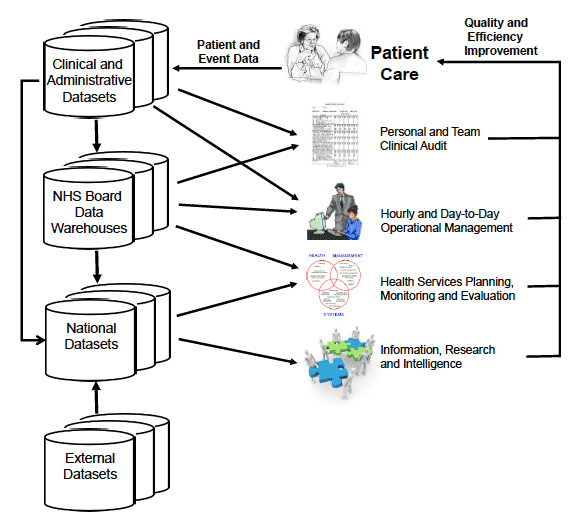
It can be expected that significant additional value can be generated in future. For example, as systems such as HEPMA are rolled out, which can provide data on prescribing practices, it should be possible to better support work in areas such as polypharmacy, antibiotic resistance and hospital acquired infections, whilst greater electronic overage and use of eForms and structured data will support linkage across care pathways and improved understanding of resource use and outcomes.
Scotland requires to continue progress and developing capabilities towards:
- integrated and person-centred information and intelligence to support integrated and person-centred care;
- increased capacity to analyse, interpret, and use data, information and intelligence;
- having the infrastructure to support information and intelligence and knowledge creation[28].
There will also need to be parallel and ongoing development of information governance arrangements and patient consent models to retain the public's confidence, and to ensure it keeps pace with developments, including the continued use and development of Safe Havens for information management.
In addition to supporting NHS related research, this infrastructure will also impact positively on the wider field of informatics for health and biomedical research and innovation as set out in the recent draft strategy[29] for this area.
5.5.3 Strategy and Deliverables
During the new Strategy period:
- By 2015 eHealth Division will review the process for development, maintenance and use of clinical content and messaging standards and datasets in Scotland, reflecting both UK and wider international developments. This will include resource requirements and a plan for the adoption and maintenance of standards, including the need for education and training programmes, and data quality improvement, and arrangements for ongoing engagement with suppliers in relation to this key requirement. This will need to build on existing standards in Scotland and be a clinically-led process that is dynamic and informed by national, international and industry developments and standards, and can inform future system development and procurement. It should provide a basis for common and compatible clinical information across Scotland, and enable clinical audit and quality improvement as well as systems integration. A key component will be Scotland's continued participation in the Professional Records Standards Body for Health and Social Care;
- A focus will be maintained on the need for immediate monitoring and reporting information, including track and trigger capability, that is focused on patient safety, care quality, and clinical audit;
- By 2015 NHS Boards will assess the requirements and approach to the future use of SNOMED CT within NHSScotland eHealth systems. This will result in eventual replacement of the current use of READ codes and a standard approach across Scotland. Training and support will be required to enable staff to make the best use of a new coding structure where accuracy and completeness will be an important part of getting maximum value from eHealth systems;
- By 2015 eHealth Division will embed a process to ensure that all aspects of information management are fully considered from the outset of considering new operational systems, including use of national standards and data sets, and the availability and use of collated data to support analysis and research. This will involve close working with various bodies including Clinicians, NHS Research Scotland, the Health Informatics Research Advisory Group (HIRAG), the Farr Institute and a multitude of other interested parties;
- By 2016 eHealth Division will sponsor work to review with key parties, including the NHS Boards, the National Information Leads Group, NHS National Services Scotland and Health Analytical Services Division, as well as other research and industry organisations, the requirements to ensure alignment between information system developments at local level and business intelligence activities at NHS Board, regional and national levels. This will include the generation and maintenance of local and national data sets, and the best approach to ensuring a co-ordinated and effective information architecture, infrastructure and governance. It is expected that this will take the form of an Information Strategy for NHSScotland which will address these issues;
- Work will be undertaken in the periods to 2017 and to 2020 to improve this alignment based on the Information Strategy, NSS' Information Redesign Programme, the National Information and Intelligence Framework, and the Health and Biomedical Informatics Research Strategy.
5.6 To maximise efficient working practices, minimise wasteful variation, bring about measurable savings and ensure value for money
5.6.1 Current Status
Paper-lite environments and reduced travel are increasingly common within NHSScotland as a result of digital dictation, voice recognition, scanning, videoconferencing and electronic requesting and reporting. Work is ongoing to broaden and extend this use which was an original aim for 2014 and will continue in the period to 2017. However, much opportunity still remains to streamline, workflow and automate many elements of care processes. Whilst paper-lite operations are indicative of progress, the real goal is to relieve clinical staff of as much documentation and administrative burden as possible and enable them to focus on care delivery within a highly planned and co-ordinated healthcare environment following standardised processes and protocols.
5.6.2 Vision and Priorities
eHealth developments under the other strategic aims should make a substantial contribution to improving efficiency through making staff activity more effective, and enabling better informed and more timely decisions about patient care which inherently will generate greater value and avoid mistakes and duplication. Additionally, clinical decision support and workflow will standardise care processes and reduce variation whilst at the same time allowing enough flexibility to adapt to individual patients and local situations. The net effect will be an upward drive to care quality, a reduction in delays and faster treatment times, and an associated increase in efficiency. The focus on enabling self-management includes a clear objective to release NHSScotland capacity, whilst clinical decision support should also enable staff to increase their knowledge and capability to care for a broader range of patients.
However, all of these developments will require recognition of the need for a full change management process of investment appraisal and benefits realisation, including effective consultation with staff, process definition, and appropriate levels of user training and support.
There are also opportunities from the ongoing convergence process across Scotland in terms of both operating practices and the infrastructure and support of eHealth systems. NHS Boards already share a number of eHealth services and further sharing options will be pursued on a regional and national basis. Delivery will be dependent on strong eHealth and clinical leadership to meet the challenge of effecting, in some cases, disruptive change to established ways of working.
Corporate business systems, specifically finance, payroll and human resources play a key role in enabling efficient management of NHSScotland. Common finance systems across the NHS Boards are already in place and the roll-out of the new Electronic Employee Support System (eeSS) is currently underway. The future of the payroll system in the context of the anticipated retirement of the current mainframe infrastructure is currently under consideration. The convergence of these systems will provide a platform for any future development of shared services in these areas within NHSScotland.
The vision for 2020 is that this will be reflected in a largely paperless environment where communication will be electronic with reduced transaction costs and time. Staff and physical assets will be utilised in the most effective and efficient way, including seven day services where appropriate, as a result of increased capacity to organise, manage and control the healthcare delivery environment. Consequently, patients will receive care quickly and efficiently, confident that they are receiving the best available quality. Additionally, where possible care will be in the patient's home or community, with travel for patients and staff reduced through electronic communication, including videoconferencing, and supported self-care.
It is acknowledged, however, that eHealth can result in some tasks taking longer, albeit with better information recording and management as a result, which has longer term benefits for patient care. Additionally, purchasing and maintaining an electronic infrastructure has significant costs, in particular given the requirements for a regular schedule of technical refresh. This needs to be accounted for in assessing investments and making financial provision.
5.6.3 Strategy and Deliverables
During the new Strategy period:
- *NHS Boards will focus on taking advantage of the economies of scale available from eHealth convergence and common infrastructure, both hardware and software, shared services, and associated benefits of overall simplification of the eHealth systems architecture and support. This applies to system procurement, operations and ongoing support, and also provides an opportunity to improve resilience. SWAN reflects this direction, and it is expected to be a continuing trend in the period to 2017 with more dramatic progress in the period to 2020 and beyond as key systems and contracts are replaced. Examples include greater shared system hosting and development, common desktop and mobile hardware and software, more Category A (mandatory) and Category B (preferred new replacement) applications and fewer instances of systems, with shared helpdesk and other support arrangements. NHS Boards will be expected to include within their local delivery plans, and report at their annual reviews, their assessment of opportunities and progress with convergence with NHS Partners and on a regional public sector basis;
- Advantage will be taken of the annual IM&T Survey to collect information on eHealth convergence that will allow NHS Boards to compare progress and share learning. This will also be linked into the reporting work on common measures with the aim of enabling robust annual eHealth reviews;
- Implementations will focus on identifying, defining and supporting real change to care models and processes. This is undoubtedly challenging and disruptive. However, for eHealth technology solutions to enable self-management and to impact efficiency, significant effort will be required to ensure they complement or replace existing care activities and are not just an add-on to current practices. This will require close relationships and joint working with the Joint Improvement Team at national level, and clinical redesign teams and the Health and Social Care Partnerships at local level;
- By 2016 eHealth Division will sponsor a study to consider the opportunities available from enhancing the systems support for exploiting NHSScotland's property and facilities. This eHealth Strategy envisages extensive development in supporting NHS staff and the management of medications, two of the largest areas of cost. This aim recognises the substantial investment and spend in the area of estates and the need to maximise the value and quality from the healthcare environment, and the opportunities available from flexible use of space enabled by mobile access to systems, space booking systems, and conferencing and collaborative working support. Some work has already been undertaken in this area, and these developments will enable any future developments around shared services related to the maintenance and use of property and facilities.
5.7 To contribute to innovation occurring through the Health Innovation Partnerships, the research community and suppliers, including the small and medium enterprise (SME) sector.
5.7.1 Current Status
The digital health sector is recognised globally as a very significant economic opportunity. Key initiatives to encourage innovation in healthcare have been established in Scotland over recent years including the Innovation Partnership Board, the Health Innovation Partnerships and the Digital Health Institute (DHI), whilst NHS Boards work directly with a number of SME partners on various eHealth developments.
Scotland's reputation for health innovation within Europe is strong based on significant success. Within the European Commission's flagship programme - the European Innovation Partnership for Active & Healthy Ageing - the Joint Improvement Team's Telecare Development Programme was recognised as one of the top ICT enabled programmes in Europe. With SPARRA (Scottish Patients at Risk of Readmission and Admission) and the National Falls Programme also recognised, this put Scotland within the top three regions in Europe for the use of technology enabled care in support of the older population in their own homes, with Scotland now one of the few formal 'Reference Sites' within Europe.
A key development has been the creation of the Digital Health Institute (DHI) in Scotland. This is an innovation centre established by NHS24, the University of Edinburgh and Glasgow School of Art, with funding from the Scottish Funding Council specifically to consider the role that digital technologies can play in addressing major health and social care challenges. It works with the public sector, the research community and the private sector with the objective of stimulating economic development in this area in Scotland, including inward investment. The DHI has significant funding and can progress proposals arising from all sources, and is able to facilitate areas such as procurement, commercial arrangements and intellectual property rights. Currently, there is a significant range of live projects, with substantial involvement from NHS Boards and Local Authorities.
5.7.2 Vision and Priorities
This aim recognises that a prime purpose of Scottish Government is the development of the Scottish economy. NHSScotland has an important role to work closely with its suppliers to innovate and develop existing deployed systems and tools. However, given its scale and footprint it is also in a position to co-develop innovative solutions and services with the wider industry which contribute towards the 2020 objectives and the economic development of the health technology industry in Scotland. This will include the co-operation of current and future strategic suppliers to enable this objective through open data standards and supporting access to their APIs to allow interoperability. This could, for example, be considered for inclusion as a contractual requirement in future procurements.
The vision for 2017 is that NHSScotland will be working in an effective partnership with the Scottish Government, the academic sector and industry, including SMEs, to promote Scotland as an attractive location for organisations active in the area of eHealth research, development and innovation. This applies to NHSScotland's existing suppliers of eHealth systems and tools, from which continuous innovation is expected, as well as other potential suppliers.
NHSScotland will continue to expect any new eHealth products, developments or upgrades to be affordable, effective and resilient, and to offer significant benefits not currently available to NHSScotland and its staff and patients. The best way to achieve this will be to involve users in the researching, planning, development and trialling of new systems and tools from the outset. It is expected that key relationships will continue to be established at international, national and local levels, with the ultimate aim of seeking additional research and innovation investment opportunities, and the momentum that can arise from a concentration of expertise within a Scottish cluster. Such opportunities will include NHSScotland involvement in consortia bidding for European Union, Medical Research Council and Innovation UK Funding.
5.7.3 Strategy and Deliverables
During the new Strategy period:
- NHSScotland will participate with academia, the Digital Health Institute, Scottish Government, the Enterprise Network and industry partners in the definition of a strategy for research and innovation in eHealth in Scotland, including identification of the key opportunities with potential for development at scale;
- NHSScotland will undertake to engage in a structured programme of periodic meetings with the industry and its representative bodies to share information on developments, key areas of interest and critical challenges. This will include participation in initiatives to promote Scottish eHealth science and technology internationally;
- NHS National Services Scotland will co-ordinate the activities of NHS Boards on leading growth in the publication of Open Data for external use and analysis to better facilitate research and innovation;
- NHSScotland will continue to pursue the widespread adoption of standard clinical datasets and messaging standards, and will encourage, including through possible contractual obligations, the opening up of APIs on eHealth systems to allow other suppliers to provide complementary innovations. This will include recognising that patients will, over time, expect to both download their own data for personal use in applications and devices, and record data that they have generated through their own personal health monitoring and assessment activities;
- NHSScotland will continue to work through the DHI, the Health Innovation Partnerships and other consortia to collaborate with commercial organisations including SMEs, as well as continuing to work directly with local partners and networks;
- The DHI and NHS national procurement will continue to act as advisers in relation to appropriate procurement arrangements and options for IP and suitable contractual terms and conditions.
Contact
Email: Alan Milbourne
There is a problem
Thanks for your feedback