The Scottish Health Survey 2008
The Scottish Health Survey 2008
1 GENERAL HEALTH AND MENTAL WELLBEING
Lisa Given
SUMMARY
- Three-quarters of adults rated their health in general to be 'very good' or 'good' and 7% rated it as 'bad' or 'very bad'. Perceptions of health varied significantly with age; 88% of men and 86% of women aged 16-24 said their health was 'good' or 'very good' compared with 55% of men and 51% of women aged 75 and over.
- 38% of men and 42% of women had a long-term condition or disability, with 28% of men and 23% of women having a limiting long-term condition. The prevalence of long-term conditions increased with age: fewer than two in ten of those aged 16-24 had a long-term condition compared with around seven in ten of those aged 75 and over.
- Conditions of the musculoskeletal system were the most commonly reported long-term conditions among both men and women (143 per 1000 and 178 per 1000 respectively) followed by conditions of the heart and circulatory system (107 per 1000 for both men and women).
- Multivariate analysis was used to explore the relationship between a range of factors and the odds of having poor self-assessed health. The odds of having poor self-assessed health increased with age, and also rose as income declined and area deprivation increased. Smokers had higher odds than non-smokers of having poor self-assessed health while those who drank over the recommended weekly limits for their sex had lower odds.
- Women were more likely than men to have a high GHQ12 score, which indicates a possible psychiatric disorder (17% versus 12%).
- The proportion of adults aged 16 to 64 with a high GHQ12 score has not changed since 1995.
- The Warwick-Edinburgh Mental Wellbeing Scale ( WEMWBS) measures mental wellbeing. Higher scores indicate higher levels of wellbeing. Men in 2008 had a slighter higher mean score than women (50.2 and 49.7 respectively).
- Mean WEMWBS scores were lowest amongst those in semi-routine and routine households, the lowest income quintile households, and the most deprived area quintile.
- Multivariate analysis showed that the odds of having a lower than average WEMWBS score were higher among adults who were not in employment, and for those in the 4 th and 5 th income quintiles. For women the odds of a lower than average WEMWBS score increased as area deprivation increased, and were higher among single, divorced and widowed women compared with married women.
1.1 INTRODUCTION
This chapter covers self-assessed general health, long-term conditions and mental health.
The Scottish Government's National Performance Framework, 1 launched in October 2007, is at the heart of a new outcomes focussed approach to policy formulation in Scotland. The following overarching purpose guides all aspects of the Framework:
To focus government and public services on creating a more successful country, with opportunities for all of Scotland to flourish, through increasing economic sustainable growth
A number of high level targets support the pursuit of this purpose, one of which acts as the main driver of health policy in Scotland:
To match average European ( EU15) population growth over the period from 2007 to 2017, supported by increased healthy life expectancy in Scotland over this period
The commitment to increase healthy life expectancy is reflected in one of the five strategic objectives that support the high level targets. The objective below, which focuses on Scotland's considerable need for health improvement and reduction of inequalities, is of central importance to the Scottish Health Survey and this report:
Healthier: Help people to sustain and improve their health, especially in disadvantaged communities, ensuring better, local and faster access to health care
Allied to the five strategic objectives are 15 national outcomes that describe what the Government is aiming to achieve and 45 national indicators that track progress towards these outcomes. The outcome "we live longer, healthier lives" is clearly of most direct relevance in terms of achieving the "healthier" objective. The persistence and pervasiveness of health inequalities in Scotland means that the outcome "we have tackled the significant inequalities in Scottish society" is also pertinent.
As a study of public health, the Scottish Health Survey has an important role in assessing health outcomes and the extent of inequalities in Scotland over time. Each of the chapters in this report addresses an aspect of health that relates either directly or indirectly to the Government's objective of improving health in Scotland. As well as addressing general health and long-term conditions, both critical measures of the population's overall health status and key markers of health inequalities, 2 this chapter presents the data on mental wellbeing used to measure progress for the following national indicator:
Increase the average score of adults on the Warwick-Edinburgh Mental Wellbeing scale by 2011
The 2008 report of the Ministerial Taskforce on Health Inequalities Equally Well highlighted the significant inequalities associated with self-reported general and mental health and stated that "enhancing mental health, wellbeing and resilience" was one of its key priorities. 3 Public health policy in Scotland has, of course, been informed by numerous other White Papers, strategy documents and action plans, both before and after the publication of the 2007 performance framework and Equally Well. For example, the 2003 strategy document Improving Health in Scotland: the Challenge acknowledged that self-reported general and mental health were key markers of health inequalities at that time. 4
A number of policy documents with particular significance for mental health and wellbeing in Scotland were published in the period 2006-2009. The previous Scottish Executive's action plan, Delivering for Mental Health, was published in 2006 and contained a series of targets relating to the care and treatment of people with mental ill-health. 5 Mental health and wellbeing were integral to the 2007 Better Health, Better Care6 action plan for improving health and health care in Scotland; this also contained a commitment to implementing the 2006 Delivering for Mental Health plan.
Building on Scotland's National Programme for Improving Mental Health and Well-Being 7 (the National Programme) launched in 2003, a new policy and action plan for mental health improvement in Scotland was launched on 7th May 2009: Towards a Mentally Flourishing Scotland ( TAMFS). 8 This policy and action plan outlines six strategic priorities aimed at: promoting good mental wellbeing; reducing the prevalence of common mental heath problems, suicide and self harm; and improving the quality of life of those experiencing mental health problems and mental illness. The six strategic priorities are:
- Mentally healthy infants, children and young people
- Mentally healthy later life
- Mentally healthy communities
- Mentally healthy employment and working life
- Reducing the prevalence of suicide, self-harm and common mental health problems
- Improving the quality of life of those experiencing mental health problems and mental illness.
In 2006 the National Programme commissioned NHS Health Scotland to devise a set of national mental health indicators for adults to enable the monitoring of various linked activities. 9 A broad approach was taken that encompassed positive wellbeing as well as traditional measures of mental ill-health. Twenty of the final 55 measures in the set are based on questions in the Scottish Health Survey, some of which have been asked in each round of the study and some which were newly introduced in 2008 for the purpose of providing monitoring data. All the topics reported in this chapter are included in the mental health national indicators. The development process for the national mental health indicators revealed a measurement gap in relation to positive mental wellbeing. This gap was filled by adapting and shortening a 40 item scale originally developed in New Zealand, the Affectometer 2, 10 for use in the Scottish Health Survey from 2008. The resulting new scale, the Warwick Edinburgh Mental Wellbeing Scale ( WEMWBS), has 14 items designed to assess positive affect (optimism, cheerfulness, relaxation); and satisfying interpersonal relationships and positive functioning (energy, clear thinking, self-acceptance, personal development, mastery and autonomy). 11 The Scottish Health Survey has also included the General Health Questionnaire ( GHQ12) 12 since 1995. This is a widely used standard measure of mental distress and psychological ill-health, consisting of 12 questions on concentration abilities, sleeping patterns, self-esteem, stress, despair, depression, and confidence in the previous few weeks. The development phase of WEMWBS established that the new scale did not simply detect the absence of distress or psychological ill-health, as measured by GHQ12, but also captured a different dimension of mental wellbeing. This chapter reports both these measures and can, arguably, paint a more comprehensive picture of mental health and wellbeing than has been the case until now.
This chapter is in two parts. The first section looks at self-assessed general health and long-term conditions. The second presents the two measures of psychological ill-health and wellbeing outlined above.
1.2 SELF-ASSESSED GENERAL HEALTH AND LONG-TERM CONDITIONS
1.2.1 Introduction
This section reports self-assessed general health and long-term conditions. Every participant was asked to rate their health in general, and whether they had any long-term condition or disability. Responses are based on participants' recall and as such are subject to distortion due to variations in individual perceptions. Each of the two aspects is first presented in detail.
1.2.2 Self-assessed general health
All participants were asked to asses their health in general as either 'very good', 'good', 'fair', 'bad' or 'very bad'. Self-assessed health is a useful measure of how an individual regards their own condition generally and is known to be related to the incidence of chronic and acute disease, as well as being a good predictor of hospital admission and mortality. 13, 14
Self-reported general health was similar for both sexes. Three quarters of men (76%) and women (75%) described their health in general as 'good' or 'very good'. 16% of men and 19% of women assessed their health as 'fair' and 7% of adults described it as 'bad' or 'very bad'.
For both men and women, the prevalence of 'good' or 'very good' general health decreased with age. 88% of men and 86% of women aged 16-24 assessed their health as 'good' or 'very good' compared with 55% of men and 51% of women aged 75 and over. Just one percent of men aged 16-24 reported their general health as 'bad' or 'very bad' compared with 17% of men in the oldest age group (aged 75 and over). The corresponding figures for women were similar (2% and 13% respectively). Table 1.1
1.2.3 Long-term conditions
All participants were asked about physical or mental conditions, or disabilities, that had affected, or were likely to affect them for at least a year. The name and nature of all long-term conditions or disabilities reported were recorded verbatim. Participants were also asked to say whether their condition or conditions limited their daily activities in any way so that conditions could be further classified as limiting or non-limiting.
In 2008 the wording of the question about long-term conditions was changed in line with moves to harmonise questions across all Scottish Government surveys and to bring it into line with the definition of disability used in the Disability Discrimination Act. The wording used in 1995, 1998 and 2003 was:
Do you have any long-standing illness, disability or infirmity? By long-standing I mean anything that has troubled you over a period of time, or that is likely to affect you over a period of time?
The new question being used from 2008 onwards is worded as follows:
Do you have any long-standing physical or mental condition or disability that has troubled you for at least 12 months, or that is likely to affect you for at least 12 months?
For this reason trends in the prevalence of long-term illness or conditions must be interpreted with caution and are not reported here.
Prevalence of long-term conditions
Around 4 in 10 adults (38% of men and 42% of women) had a long-term condition or disability. The same proportion of men and women (15%) had conditions which they described as non-limiting, while the proportion with limiting long-term conditions was higher among women than men (28% compared with 23%).
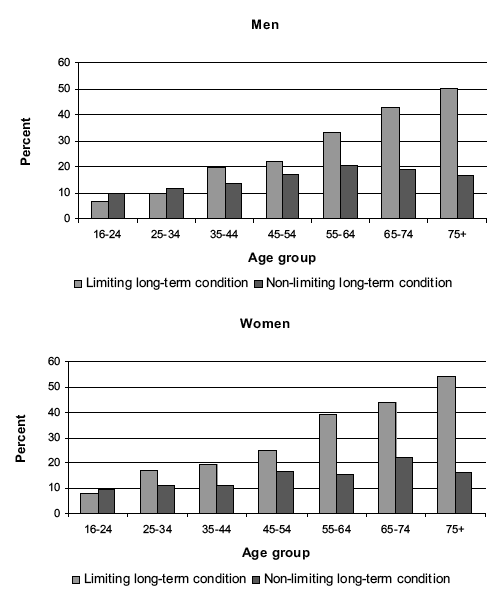
The prevalence of long-term conditions increased significantly with age for both men and women. Fewer than two in ten of those aged 16-24 (16% of men and 18% of women) had a long-term condition compared with around seven in ten of those aged 75 and over (67% of men and 71% of women). A majority of men and women aged 55 and above had a long-term condition. As Figure 1A shows, the association with age was more pronounced for limiting than for non-limiting conditions. Prevalence of a limiting long-term condition was around 7 times higher for those aged 75 and over than for those aged 16-24. Half of those aged 75 and over (50% of men and 54% of women) reported having a limiting condition compared with 7% of men and 8% women aged 16-24. Table 1.2, Figure 1A
Figure 1A Prevalence of long-term conditions by age and sex
Number of long-term conditions
The number of long-term conditions reported was similar for both sexes. A quarter (23% of men and 25% of women) reported having one condition and one in six (15% of men and 17%) had two or more. Of those with a long-term condition, the mean number of conditions was 1.6 for both men and women.
There was a strong association between the number of long-term conditions reported and age. Just 3% of men and women aged 16-24 had two or more long-term conditions compared with more than a third (35% of men and 39% of women) of those aged 75 and over. Table 1.3
Type of long-term condition
Long-term conditions were classified using the International Classification of Diseases ( ICD-10) coding schema. These conditions were first coded by broad category and then aggregated into groups based on ICD-10. The classification of conditions was based solely on participants' definitions and self-reported symptoms. As a result the classification might not always correspond with a doctor's diagnosis.
Conditions of the musculoskeletal system were the most commonly reported long-term conditions among both men and women (143 per 1000 and 178 per 1000 respectively) followed by conditions of the heart and circulatory system (107 per 1000 for both men and women). These were followed by respiratory conditions for men (66 per 1000) and conditions of the endocrine and metabolic system for women (78 per 1000).
In general, rates increased with age with a few notable exceptions. Rates of infectious diseases and skin complaints were similar across all age groups for both men and women. Rates of mental disorders were highest among those aged under 65. Among men, the rates per 1000 adults were 53 for the 16 to 44 age group and 56 for those aged 45 to 64, compared with 21 and 23 for those aged 65-74 and 75 and over respectively. The corresponding figures for women were 69, 74, 48 and 33. Mental disorder rates were also higher for women than for men (64 per 1000 and 48 per 1000 respectively). It is worth noting that it is likely that many older people with mental disorders will live in residential settings so this household based measure could potentially under-report the prevalence of such conditions among older people. Table 1.4
1.2.4 Factors associated with poor self-assessed health
Multivariate logistic regression was used to examine the factors associated with poor self-assessed health. Poor self-assessed health was defined as reporting health in general to be either 'bad' or 'very bad'. Separate regression models were run for men and women and the factors found to be significant for both sexes were: age, equivalised household income, area deprivation quintile, smoking status and alcohol consumption. Household and parental socio-economic classification (classified according to the highest occupation recorded for participants' parents when the participant was aged 14), were also explored but were not found to be significant. The income, area deprivation and socio-economic classification measures are all fully described in the Glossary. Logistic regression compares the odds of a reference category (shown in the table with a value of 1) with that of the other categories. In this example, an odds ratio of greater than one indicates that the group in question is more likely to have poor self-assessed health than the chosen reference category; an odds ratio of less than 1 means they are less likely. For more information about logistic regression models and how to interpret their results see the Glossary at the end of this volume.
Age was significantly associated with poor self-assessed health. As the prevalence of poor self-assessed health was very low among the younger age groups age was treated as a continuous rather than a categorical variable in this analysis, so odds ratios are not available for specific age groups. Instead, the odds ratio shows how much the odds of reporting poor health change as age increases by one year (from 16 onwards). The odds of reporting poor self-assessed health increased by 1.04 for each additional year for men and by 1.03 for each additional year for women.
Household income was significantly associated with poor self-assessed health for both men and women. When compared with the highest household income quintile, the odds of reporting poor health were significantly higher among men in the 3 rd, 4 th and 5 th income quintiles, and among women in the 4 th and 5 th. The odds of those in the lowest quintile having poor self-assessed health were 8.03 times higher for men and 2.50 times higher for women.
For both sexes there was a significant association between SIMD quintile and poor self-assessed health. Among men, those in the most deprived quintile had significantly higher odds of reporting poor health than those in the least deprived quintile (odds ratio of 2.51). The odds of women living in the 4 th, 2 nd and 1 st (most) deprived deprivation quintiles were significantly higher than those in the least deprived (for example, the odds ratios for those in the 2 nd and 1 st most deprived quintiles were 1.98 and 2.79, respectively).
The odds of ex-regular smokers and current cigarette smokers describing their health as 'bad' or 'very bad' were higher than those of men and women who had never smoked. For example, for men the odds of smokers having poor self-assessed health were 3.16 times higher while the equivalent odds ratio for women was 2.22.
Alcohol consumption in excess of the recommended weekly limit guidance was significantly associated with poor self-assessed health. The odds of men who drank over 21 units reporting 'bad' or 'very bad' health were lower than for those drinking within recommended weekly levels (0.64). The same was true for women who drank over the recommended weekly level of 14 units (0.57). This finding is in line with the equivalent regression analysis of poor self-assessed health carried out in the last report. 15 This analysis does not reveal anything about the direction of causation between two factors so it cannot be inferred that drinking above the weekly recommended limits protects against poor reported health. Rather, this finding is likely to be accounted for by the fact that non-drinkers have been included in the reference group and people in poor health are more likely to be non-drinkers. Table 1.5
1.3 MENTAL HEALTH AND WELLBEING
1.3.1 Introduction
This section concerns mental wellbeing and mental health problems. As noted in the introduction, it presents results from two measures: the General Health Questionnaire ( GHQ12) and the Warwick-Edinburgh Mental Wellbeing Scale ( WEMWBS). Due to the sensitivity of the questions both scales were asked in the self-completion booklet.
The GHQ12 measures deviations from people's usual functioning in the previous few weeks. It cannot, therefore, be used to detect chronic conditions. Furthermore, estimates cannot be made of the duration of any incidence of recent psychological ill-health and as such it is simply a measure of ill-health at a particular point in time. However, the strength of the GHQ12 is that it enables comparisons between sub-groups and trends over time to be investigated.
Responses to the GHQ12 items were scored, with one point given each time a particular feeling or type of behaviour was reported to have been experienced 'more than usual' or 'much more than usual' over the past few weeks. These scores are combined to create an overall score of between zero and twelve. A score of four or more (referred to as a 'high' GHQ12 score) has been used here to indicate the presence of a possible psychiatric disorder. A score of zero on the GHQ12 questionnaire can, in contrast, be considered to be an indicator of psychological wellbeing.
The WEMWBS scale comprises 14 positively worded statements with a five item scale ranging from '1 - None of the time' to '5 - All of the time'. The lowest score possible is therefore 14 and the highest is 70; the tables present mean scores. Unlike the GHQ12, WEMWBS is not designed to identify individuals with exceptionally high or low levels of positive mental health so cut off points have not been developed. 16
Differences in GHQ12 and WEMWBS scores are presented by age and sex; trends in GHQ12 scores are also presented. Further analysis of differences in WEMWBS scores are also presented by socio-demographic characteristics.
1.3.2 GHQ12 scores
Table 1.6 presents the GHQ12 scores for men and women by age group for all adults aged 16 and over in 2003 and 2008. In addition, it presents the figures for adults aged 16 to 64 in each of the four survey years (1995, 1998, 2003 and 2008). Changes to the sample composition over the years mean that trends back to 1995 can only be based on those aged 16 to 64.
In line with previous years, more women than men aged 16 and over had a high GHQ12 score indicating a possible psychiatric disorder (17% and 12% respectively). The only age group for whom this was not the case was 65-74 where the proportion of men and women with a high GHQ12 score was the same (11%). GHQ12 score did vary by age but with no clear overall pattern for men or women. For both sexes, a high GHQ12 score was most prevalent among the 45-54 year old age group (15% for men and 21% for women).
Looking now at the trends for the 16 to 64 age group, the proportion of men with a high GHQ12 score has been the same every year (13%) and very little change occurred among women in the same period. Table 1.6
1.3.3 WEMWBS mean score
As WEMWBS is a relatively new scale only provisional population norms had been established prior to its inclusion in the 2008 SHeS. 16 The baseline against which the National Indicator will be measured is the 2006 Well? What do you think? Survey. The mean score in that study was 51.1 (51.2 for men and 50.9 for women). 17SHeS 2008 showed a similar pattern by gender with men having a slightly higher mean score than women (50.2 and 49.7 respectively), although the overall mean scores for men and women are slightly lower. It is difficult to assess whether the mean WEMWBS score has changed significantly between 2006 and 2008 as the results are from two different surveys (and the sample in the Well? survey was much smaller than SHeS). SHeS data from future years' surveys will provide a more robust measure of changes in WEMWBS over time.
The variation in the mean score across age groups was significant among women but with no obvious pattern; it was highest among those aged 65-74 (51.2) and similar for the other age groups (with scores ranging between 49.0 and 49.8). There was no significant association between age and mean scores among men. Table 1.7
1.3.4 WEMWBS by socio-demographic characteristics
Tables 1.8 to 1.10, present the mean WEMWBS scores by socio-economic classification ( NS-SEC of the household reference person), equivalised household income and the Scottish Index of Multiple Deprivation (descriptions of each of these measures are available in the Glossary at the end of this volume).
To ensure that the comparisons presented in this section are not confounded by the different age profiles of the sub-groups, the data have been age-standardised (for a description of age-standardisation please refer to the Glossary). On the whole the differences between observed and age-standardised percentages are small. Therefore, the percentages and means presented in the text below are standardised. The tables report both the observed and the age-standardised figures.
Socio-economic classification ( NS-SEC)
There was a significant association between mean WEMWBS score and NS-SEC for both men and women. Adults living in managerial and professional households had the highest mean scores (51.5 for men and 51.0 for women) while those in semi-routine and routine households had the lowest scores (48.4 for men and 47.9 for women). Table 1.8
Equivalised household income
The relationship between equivalised household income and mean WEMWBS score was also significant, and was more pronounced than for socio-economic classification. The association was linear with the age-standardised mean WEMWBS score decreasing as annual household income decreased. This was true for both men and women. The mean scores for those living in the highest income quintile households were 51.6 for men and 52.1 for women. The corresponding figures for those living in the lowest income quintile households were 45.9 and 45.7, respectively. Table 1.9
Scottish Index of Multiple Deprivation
Two measures of SIMD are being used throughout this report. The first, which uses quintiles, enables comparisons to be drawn between the most and least deprived 20% of areas and the intermediate quintiles and helps to assess the extent of any inequalities in behaviours or outcomes. The second contrasts the most deprived 15% of areas with the rest of Scotland (described in the tables as the "85% least deprived areas"). The most deprived 15% of areas have been identified as of particular concern by Scottish Government and are the subject of a number of policy initiatives. The Scottish Health Survey is designed to provide a large enough sample in the SIMD 15% areas after four years to enable robust detailed analysis at this level.
Age-standardised mean WEMWBS scores were highest for men and women living in the least deprived quintile (51.7 for both sexes) and lowest for those living in the most deprived quintile (48.0 for men and 47.1 for women); these differences were significant. This association is confirmed when the scores of adults living in the 15% most deprived areas in Scotland are compared with those living in the rest of Scotland. The gap is greater for women (46.8 and 50.2, respectively) than for men (48.0 and 50.6). Table 1.10
1.3.5 Factors associated with 'below average' WEMWBS mean score
Logistic regression analysis was carried out to establish which factors were associated with a 'below average' mental wellbeing score (defined as being more than one standard deviation below the mean). 18 Separate models were run for men and women. Employment status was significantly associated with a below average WEMWBS score for both sexes. Equivalised household income was significant for men and just marginally non-significant for women. SIMD and marital status were also significant factors for women but not men. Age, household and parental NS-SEC (classified according to the highest occupation recorded for participants' parents when the participant was aged 14), and educational attainment were also explored but were not found to be significant.
For men, the odds of having a below average WEMWBS score were significantly higher in the 4 th and 5 th lowest household income quintiles than in the highest quintile (odds ratios of 2.26 and 2.29 respectively). Among women, the overall association between income and below average wellbeing was just on the margin of being significant; as with men, those in the lowest quintiles had higher odds than those in the highest.
Men and women permanently unable to work because of ill health had higher odds of having below average mental wellbeing than those who were in paid employment, self-employed or on a Government training programme (odds ratios of 5.96 for men and 4.30 for women). Men and women who were either looking for, or intending to look for, paid work also had higher odds of having below average mental wellbeing than those in work or training (odds ratios of 2.23 and 2.82, respectively; though note that the sample size for women in this group is relatively small). Women who were looking after the home or family also had significantly higher odds (1.46) of having below average mental wellbeing.
For women the odds of having below average mental wellbeing were significantly higher in each SIMD quintile compared with the least deprived quintile, and were highest among those in the most deprived quintile (1.93).
Marital status was a significant factor for women but not for men. Compared with women who were either married or in a civil partnership, single, divorced and widowed women all had higher odds of having a lower than average WEMWBS score. The greatest odds ratio was for women who were either widowed or a surviving civil partner (2.77). Table 1.11
There is a problem
Thanks for your feedback