Organ Donation Teaching Resource Pack
Teaching Pack for use in High Schools
Organ Donation
Teaching Resource Pack
Donor/Recipient Stories
Story 1
Peggy Murray is the wife of a liver transplant patient. She has written this story, recording her thoughts, fears and joy. Read the story.
Call at midnight: Our experience of transplant - Peggy Murray
"I remember that Sunday in January as an awful day. I stood at the bedroom window looking at the trees blowing and creaking, a dirty long streak of loose polythene entwined itself round the telegraph wires in a mad dance. The sky was almost black. It all just seemed to sum up misery. He was silent in bed in the room behind me and far from well. All he ever said was 'I'm fine'. He had had another fall and there was a purple bruise down the side of his face. It had been a struggle to lift him back up and we managed only with a chair placed against the table and a series of slow hauls and pushes. Later, as the heavens opened and rain poured down on the dispiriting scene outside, I remember thinking this is just the end. Pathetic fallacy it is called, in plays like 'King Lear' and it seemed very apposite to me. I did not think he would survive until the operation.
He had by now been on the waiting list for a liver transplant for only 4 days. First, there had been months of tests and assessments, in and out of hospital. On the last Wednesday he had at last been put on the waiting list officially and given a bleeper so that he could be alerted at any time of the possibility of an operation. At his interview as I sat beside him, the lady co-ordinator laid out very clearly the pros and cons and conditions. I knew he had no real option - it was the operation or nothing. Nothing meant just the continuation of the slow and awful decline of the past months. At the interview he was in such a state of confusion and toxicity that I fear very little of what was said stayed with him. Only someone who knew him well might be aware of that. His responses as usual were highly socially appropriate, though shorter than they would have been once. That day we left with instructions to have the bleeper with us at all times. He was to avoid infection and report any that occurred, to drink lots of water and exercise daily.
And now it was Sunday and his yellow face looked up blankly from the bed as he responded once again that he was fine and feeling better. He had kept (or been kept) rigidly to his regime of pills but they were clearly not going to be enough. As well as falling and being increasingly unsteady, his memory had got so much worse. This made life one of continual vigilance. Determined as ever to help, he would go to the freezer to get some item out for tea time and later I would find many other melting packets left on the adjoining shelf or on the floor. His ability to write deteriorated and I would find him trying to practise his signature, although he no longer wrote anything. Phone calls had to be monitored in case important messages were forgotten. Cooker and water taps had to be checked, and when he was fit to walk, he had to be kept within sight if we were out, because if he turned a corner he might get lost.
The awful Sunday passed and Monday dawned - another blustery day. He got up late and wanted to read his papers and have his breakfast, but he soon was tired and went back to bed. A friend called to see him, but he was then sound asleep and there seemed little point in waking him to tax him with trying to chat. The friend left with a very grave face.
He got up later briefly, but nearly fell over again, and it was a relief when he wanted to go back to bed to rest. 'Fine, but a little tired' he said. No complaints, very little speech.
It was 10 minutes to midnight and I was completing the nightly rituals of letting the dog out and locking up when the phone rang. Strangely I answered it with no thought other than that it was one of the many relatives who kindly kept in touch and rang at all hours to enquire. A warm and calm voice, but an unfamiliar one, told me that there was a possibility that they had a liver match for him, and could I get him in to hospital to be ready for an operation in the morning? He was to have nothing more to eat or drink in the meantime.
I wakened him and got him in to his dressing gown, still full of sleep, but pleased enough to do as he was asked. Soon the ambulance was there, although I had been warned that as a 'non-urgent' case we might have two hours to wait. The run-up through the sleeping streets of Edinburgh and the park was another chance to appreciate the care and professionalism of the ambulance attendants, one driving while the other kept patient and passenger relaxed and comfortable. They wheeled him through the darkened hospital corridors and up in the lift to the Unit, leaving us only when a waiting nurse and doctor there took over. Over the next 2 hours the nurse and doctor went through all the preliminaries with great thoroughness as I sat by him and replied for him in some measure, occasionally having to correct his recollections or information, although in some strange way the occasion appeared to have jolted a rather better level of functioning than he had recently shown. Heart, blood pressure, blood tests were all systematically taken as the clock moved on through the witching hours and the rest of the Unit - and the city - slept.
About 3 o'clock all was in readiness and he was wheeled away to a bed in the ward. I was free to leave or take the kind offer of a bed for the night in the relatives' room. Mindful of my canine housemate, and feeling that it was probably easier to face the next day at home, I made my way through the dark and silent corridors once more, out of the A & E exit and to the taxi rank across the road.
Next morning I learned that the operation was indeed to go ahead and from 10.30am he would be in the theatre. Phone calls to alert the rest of the family and close friends took up part of the day, and it passed, as even the slowest of days do, until at 6.30pm there was a call from the surgeon in charge to say it had all gone well. He had been 'healthy' all through and he was now in Intensive Care.
When his offspring and I saw him next day in Intensive Care the first thing we noticed was the change to a pinkish tinge in his skin colour. A lovely Canadian nurse - Maggie - was looking after him and he had, she said, been singing a Hebridean song to her. He had no recollection of an operation and thought it might still be to come. The change in his looks was dramatic and already he was taking a bit of interest in the world around.
The next few weeks were a bit rocky, with complications from infection and a rather embarrassing couple of days of confusion and agitation. In public he would have committed a breach of the peace. In his delirium he was back at work and laying down the law - in every sense - to the ward staff and patients. They must have found it, in every sense, a sore trial! But that passed and slowly but surely physical recovery began. The work of the physiotherapists and occupational therapists helped this along and even when the added diagnosis of diabetes had to be faced things never looked so bleak again.
The grey and faltering figure who was helped home after 7 weeks was, however, only beginning on the long road to fitness. My sister came from half-way around the world to help in the first crucial weeks and the hospital back-up with advice and equipment made it feel that we were not facing this alone. The continuing daily care and counsel of the district nurses helped incalculably.
Six months along the line, with clinic check-ups becoming encouragingly fewer and levels of medication lessening, progress has become steadier and faster. Walking has improved and his self-help skills are completely restored. All the aids so thoughtfully supplied are no longer needed and he took great delight in storing them personally in the garage for collection as soon as that was possible. Most cheering progress is exemplified by the return of his writing ability. He will now write a perfectly legible note - with spelling intact and grammar correct. He added a few notes to this account which I have included. He remembers almost everything. He can cook and mow the lawn - and he knows what we have to put on the grocery list. He tells the most awful jokes once again. While these may seem trivial, they are not to us - or anyone who has had to deal with the enveloping fog caused by this type of liver disease. He has been able to enjoy two brief breaks away from home among familiar and delighted relatives.
He has, truly, a new lease of life. He is restored to being the cheery fellow we used to know, able to enjoy the pleasures of home and neighbourhood and especially the delights of the growing grandchildren of whom he was scarcely aware last year. And if he has a life back, that makes two of us.
We have much to thank everyone for - the surgical, medical and nursing staffs and all relatives and friends, our church members, and all of the many faiths who remembered him in prayer groups and individually, our National Health Service, within which we indeed got signal advice.
There is - there was - someone who has to be thanked and that person is one I have not yet mentioned throughout this account of a marathon sojourn. I do not know this person's name or even if he is male or she is female, although I suppose the former. I only know the person's blood group and that his liver was of a suitable size. I also know that without his donation, without his thought for another, I would not be writing this story of a life leased back. So, thank you from all of us Mr Unknown Donor, and thanks to your family who at the saddest of times thought of others and ensured a second chance for a stranger.'
Discussion points
|
Story 2 - Euan Abel (8 years old)
Euan was 8 years old when he died after suffering severe head injuries in an accident. Read over his story.
An 8-year-old Scottish boy has died after falling down a lift shaft in a hotel in a French ski resort.
The screams of Euan Abel, were heard by his sister Heather, 14. Dr Graeme Abel, the boy's father, spoke of his family's grief and said he hoped his son's organs would help save other children. The family was with a party of 26 friends, including 14 children, all from Scotland, for a skiing holiday in a popular resort.
Dr Abel said: "The one positive thing that has come from this is that because Euan was able to get to hospital, he was able to donate his heart, both kidneys, his pancreas and both lobes of his liver for others. That will probably have helped six children who might otherwise have died". His son's organs were donated through the European transplant network. "We have lots of anger yet to come, but hopefully his heart is still beating somewhere in some other child who has been severely ill. Euan was always a very generous boy. This was something else he was able to give."
Dr Abel said: "Euan and his sister Heather had got up early to see off some friends who were going home on an earlier flight. They took the lift up to the next floor, and when they got out into the lobby it was in darkness because the lights were on saver-switches. Heather went across to push the time-switch and Euan turned right into what he thought was a corridor. It was another lift shaft. The lift had got stuck between floors in the night, and the fire brigade had rescued the occupants. For some reason the lift doors had been left open. Euan just went straight down."
Heather ran to get her parents. Graeme Abel ran to the ground floor and, with the help of a friend, was able to force the lift doors and climb into the shaft. He said: "I carried Euan out. He was unconscious and dying. He had emergency surgery for a ruptured spleen, but we knew he had very severe head injuries, and over the next 48 hours it became obvious he wasn't going to survive them."
Discussion points
|
Story 3 - 'Heart Operation Athlete's Tribute to Family of Saviour'
Reg Chisholm had a heart transplant in 1999. Read his story which was printed in a Scottish newspaper.
"A top athlete who had a heart transplant has dedicated his medal haul to the man who saved his life. Reg Chisholm returned from the European Heart and Lung Transplant Games as Scotland's number one. And he has given thanks to the family of the man who allowed him to live again.
He said 'I know nothing about him, but I will forever be grateful they allowed me to have his heart.' Looking at the 2 golds, silver and a bronze he brought back from the Games in Austria, he admitted the donor was in his thoughts.
He said 'He was always in the back of my mind, whoever he was. These medals are my tribute to him.' Reg, 48, had a massive heart attack when he was 45. He was told he needed a transplant or he would die, and days later a donor was found. In December 1999 the dad of three was under the knife at Glasgow Royal Infirmary. It was the start of a new life for the Dunbar-based ScottishPower worker.
He said 'I thought, this man didn't have the chance to live on, so I should try to keep his heart in top condition'. The former Dunbar Rugby Club forward won the 21km veterans' cycle race, then gold in the biathlon, silver in the 1,500 metres and bronze helping the Spanish team in the 4 x 100 metres relay.
He added 'It's a dream come true. I can hardly believe it. I wanted to do it for myself, my wife Norma, and my sons and grandkids. But above all I wanted to do it for that man who didn't have the chance. I also wanted to thank his family'."
Discussion points Reg said of the donor: "I know nothing about him, but I will be forever grateful they allowed me to have his heart."
|
Story 4 - Donor Family
Rebecca Nix, 21, died in a car crash in America. Yet as her mother Jane explains in this emotional letter, her only daughter's childhood pledge has given dozens of other people renewed hope.
"Dear Rebecca,
You were a gentle, caring child, always putting others first. So it came as no surprise when you announced you wanted to be an organ donor. You were only 7, and I can remember how serious you looked pushing the consent form into my hand. There'd been a talk at school, and your mind was made up. I talked it through with your dad, both of us touched by your determination. It was such a strange request for a child, but so like you. We signed the form.
As you grew up your donor card stayed in your purse getting tattier as the years passed. You even had to update it. I never gave it another thought, to be honest. Not until that fateful November night in 1996. You'd been working as an au pair in America for 8 months, looking after 3 small boys. I was wrapping presents when the phone rang. I answered it, imagining your chirpy voice. But it was your friend Donna. She sounded tearful, struggled to get the words out. 'There's been a car crash,' she said 'Becky's dead'. I dropped the phone, screaming. After 10 minutes of sobbing, I rang your dad on his mobile. 'Rebecca's dead,'I blurted. 'Please drive home safely.'
Sitting alone, my mind played back our last conversation. You told me all about the new grey sweatshirt you'd bought. Before you rang off you said, 'I love you mum.' Now I'd never hear those words again. I hugged your dad when he arrived home, ashen-faced and speechless. We were too choked to speak.
The night wore on. A call from a doctor at the Hartford Hospital in Connecticut filled in the gaps about the accident. You were driving to meet the school bus and crashed head-on into another car. You'd died instantly, he said. You hadn't suffered. That was a comfort.
We couldn't sleep, lost in grief. Then a strange thing happened. An image of your red-and-black donor card sprang into my mind. I jumped up, my thoughts racing. Did she have it on her? Do the doctors know about it? It was like you were propelling me forwards. Your dad dialled the hospital. He didn't mince his words. 'Take whatever you can from Rebecca,' he said. We were told your heart, lungs and liver couldn't be used because they'd been starved of oxygen. But there was hope other parts could be transplanted. The nurse thanked us and promised she'd be in touch. A wave of relief flooded over me. The next day we learnt surgeons had removed your eyes, heart valves, sections of your skin and bones. At least you were coming home to us.
Three days later I went to see you in the chapel of rest near our Birmingham home. You were wearing the American sweatshirt you'd told me about, you looked as if you were sleeping. I slipped your favourite brown lipstick in beside you, together with your Winnie The Pooh gloves. 'You're still my little girl,' I whispered. 'You always will be.'
A month after your death the first letter came. Your corneas had restored the sight of a 24-year- old man and a 41-year-old woman. We cried. Your skin had been grafted onto children suffering severe burns. Your heart valves were given to two men, while your bones were used to replace diseased tissue in dozens of patients.
A total of 74 people were helped by you. So even in death you reached out to others. Our grief is still raw, and it would be too painful to contact any of them, but the hospital has told us every single one wanted to pass on their thanks for your special gift. I think every bereaved parent has an overwhelming fear their child will be forgotten. But we know that will never happen to you, Rebecca. It's such a comfort to know you've given so many people a better life. I'm so proud of you in death as I was during your all-too-short lifetime.
Your mum,Jane Nix"
Story 5 - A Decision not to Proceed
The Transplant Co-ordinator was called to the Intensive Care Unit (ITU) to speak to the parents of a 17-year-old male who had been declared dead following brain stem tests as a result of a road traffic accident. He had just passed his driving test and his parents had helped him buy the car. He was brought into the Accident and Emergency and later was transferred to the ITU where he was in a coma, attached to a life support machine in a critical condition with little hope of survival. When it became apparent that nothing further could be done for this patient the family were informed and the doctors explained that they were going to perform brain stem death tests. The doctors went on to test the patient's brain stem function and along with the scan of his brain found that he had suffered irreversible damage to his brain stem. When two sets of brain stem tests were completed and confirmed that the patient was dead this was then explained to the parents and then they were asked if they would like to discuss the option of organ donation as their son had carried an organ donor card. When the transplant co-ordinator spoke to the parents they were aware that their son had carried a donor card but felt unable to agree.
Discussion points
|
Living Donation
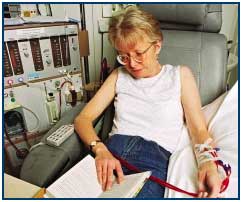
Story 6 - The Story by Joyce
"In June 1999 I had a kidney removed due to polycystic kidneys and began haemodialysis. Both sisters offered me a kidney and a meeting was arranged with the transplant surgeon and the co-ordinator. Information about the procedure was given honestly, making it clear that the donor underwent a more painful operation than the recipient and all the risks involved. Having discussed the benefits for me within the whole family, it was decided to go ahead to see if Elizabeth was compatible.
Life on dialysis was limiting but I was lucky and kept well, managing to hold down a part-time job as a teacher. My family were very supportive and took on many new roles than they had previously, as I attended haemodialysis three times weekly.
When Elizabeth came up for the 2 days of pre-transplant tests, I was swaying from being very positive and keen, to being worried and upset. Elizabeth was planning to undergo major surgery for me with no benefit to herself, other than hopefully seeing me enjoy a normal life again. This was brought out in the open and she reassured me that she did not feel pressurised or obliged to go ahead. When the results came through we were given a date for July and planning began in earnest. Children and pets had to be taken care of and it was important that arrangements were flexible.
I was admitted 2 days before the operation and underwent routine checks. Elizabeth was admitted the next day. I had my final dialysis that evening and returned to the unit to find both families and our dad there. It was a tense evening and after the visitors went away, Elizabeth and I did a jigsaw in the day room until 12.30am, putting off the moment of going to bed and being left with our thoughts.
On the morning of the operation we were both up early, showered and Elizabeth went to the operating theatre about half an hour before me. The next thing I knew was waking up and my husband being by my bed and it was all over. Elizabeth was opposite me in the High Dependency Unit and once we were both awake and had reassured each other we felt 'great', there was amazing relief and hilarity that the operation was behind us.
The next day I got up with the help of the physio and really felt great, but was concerned that Elizabeth was obviously in discomfort and sleeping a lot. The staff were fabulous and assured me that this was the normal pattern, the donor initially taking longer to recover. It took another 3 days for Elizabeth to return to her usual self and after that there was no stopping her.
I was also discharged after a week and initially attended hospital every few days for blood tests.
Life is so different for me!!
I have a new found energy, can eat a much larger variety of foods, can drink lots of fluids, have much more time to myself - and really am a new person. All thanks go to my sister Elizabeth and the team of people in the Transplant Unit."
Story 7 - The Story by Elizabeth
"When my sister Joyce was told she had kidney failure, I cannot remember actually making the decision about asking to be considered as a donor, I just knew it was what I wanted to do. My husband and children were completely supportive. I think that this is vital to the whole process, because it inevitably involves you all.
My younger sister was also keen to be considered. So we told Joyce, and a meeting was arranged with the transplant surgeon and transplant co-ordinator.
One of my main impressions of this time was that much of the information given seemed to be pointing towards the more negative aspects of what might happen, despite the superb success rates. This was to ensure that the donor was as clear as possible about what was involved and that the offer was made with no pressure from any quarter. When it became clear that I was compatible and my general health was good, a 2-day admission to hospital was arranged for a series of more specific tests. This was my first visit to hospital, excluding the birth of our children, but any apprehension was soon dispelled by the supportive attitude of all staff. The tests consisted of blood tests, blood pressure, a chest X-ray, an ultrasound scan and a renal angiogram. I actually quite enjoyed the experience!
This was also a very important point in the whole process. It was during this time that I realised how complex Joyce's feelings were about what was happening to us all. It was a very emotional time for her. As far as she was concerned, it was because of her that I was in hospital - despite the fact that the tests themselves were straightforward and far from dreadful. It highlights the fact that this is something the recipient cannot repay and how difficult it can be to accept this. Personally, I think it is probably easier to be a donor. The good part of this was that it provided an opportunity to reaffirm our feelings and remain very positive about continuing.
Much to our delight, the results showed that my general health was good and I had 2 well functioning kidneys. Reality strikes! Dates were put into place and arrangements made. As a teacher, I am fortunate to have a long break in the summer and it was arranged that this was when the operations would take place. This was at our request, and another example of how well we were looked after.
The day before the transplant was scheduled, I was admitted into the Transplant Unit. 'Unit' is an excellent description of the place. Every person, without exception, works as part of the team to provide a service second to none. The atmosphere is so positive and caring that it helps to dispel the inevitable apprehensions. The night before the transplant was most peculiar. It is very comforting to be in hospital with someone you know so well and this helped me in many ways. Our families visited and it was a time of mixed emotions. Everyone is affected by what is happening. It is not just the donor and recipient. When Joyce and I did eventually go to bed, it was with hope and expectation.
Early the next morning I was prepared to go to theatre first, and Joyce soon after. The operations take place in a specially designed twin theatre. The faces I saw on the ward, on the way to theatre and in the anaesthetic room were familiar. All had introduced themselves previously, which is so helpful when the surroundings are unfamiliar. The operations are carefully planned with consultant transplant surgeons leading the two teams. After the kidney is removed, it is transferred to the adjoining theatre to be transplanted.
When I woke up on the High Dependency Ward Joyce was opposite and we seemed to come round about the same time. We both reassured each other that all was well. What a wonderful feeling! Everyone on the ward helped to make sure that everything was done to make us as comfortable as possible. When our families visited later in the day there was so much joy and laughter. Now we had to hope that the kidney would do its job and make Joyce feel better than she had been in a long time.
The next few days were filled with a variety of checks such as blood tests, urine counts and fluid intake. The physiotherapist was on hand to make sure mobility returned as quickly as possible. My recovery was made so much easier by the signs that the kidney was doing its job. Joyce was feeling good! I will never forget her euphoria on the morning of the second day when she noticed that the whites of her eyes were no longer yellow, but clear white - a very positive sign.
Things continued to go well and after a week in the Unit I was allowed home. A follow-up, 6 weeks after the operation, ensures that blood and urine tests have returned to normal. It is also made very clear that if anything crops up at home which causes concern, there is always someone available at the Transplant Unit to answer questions and provide support.
Being a kidney donor is a unique experience that not everyone who wishes to has the opportunity to take. I was fortunate to be able to do this and would encourage others to do so as well. Personally I feel richer as a result of the whole experience and through meeting so many special people."
Discussion points
|
There is a problem
Thanks for your feedback